Abstract
Background:
Invasive mechanical ventilation is necessary for many infants in the neonatal intensive care unit (NICU). Although it is a lifesaving intervention, it has potential adverse effects, including UE. UE can lead to significant cardiovascular and respiratory compromise. In 2018, our UE rate was 1.724/100 ventilator days. Due to the UE rate, the NICU developed an interdisciplinary UE committee to assess potential gaps in practice.
Methods:
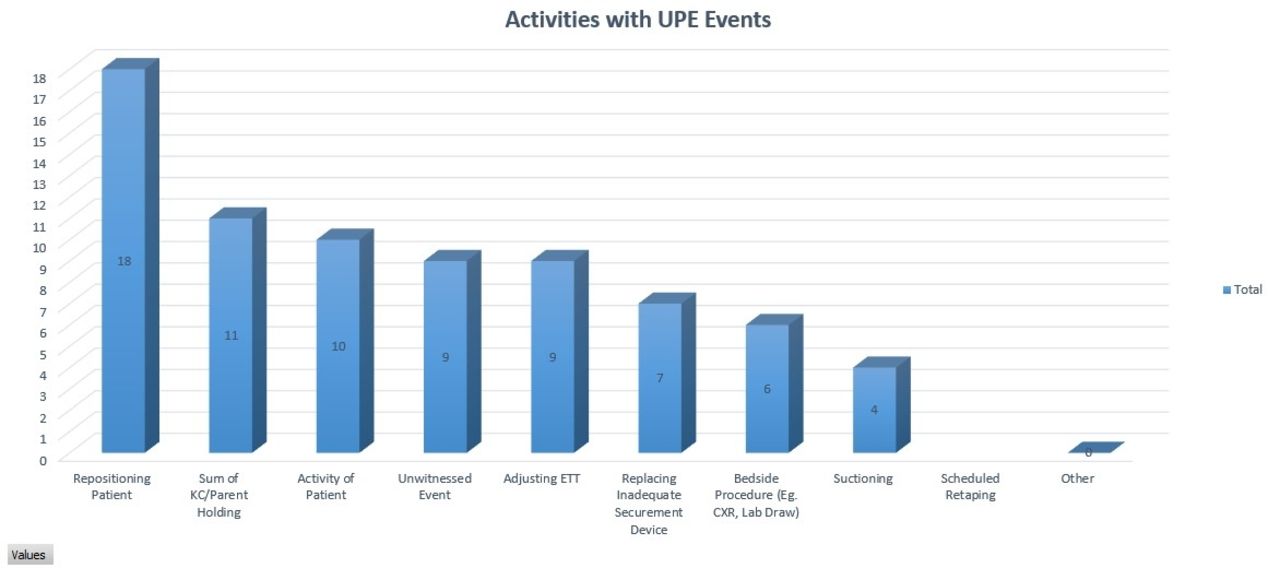
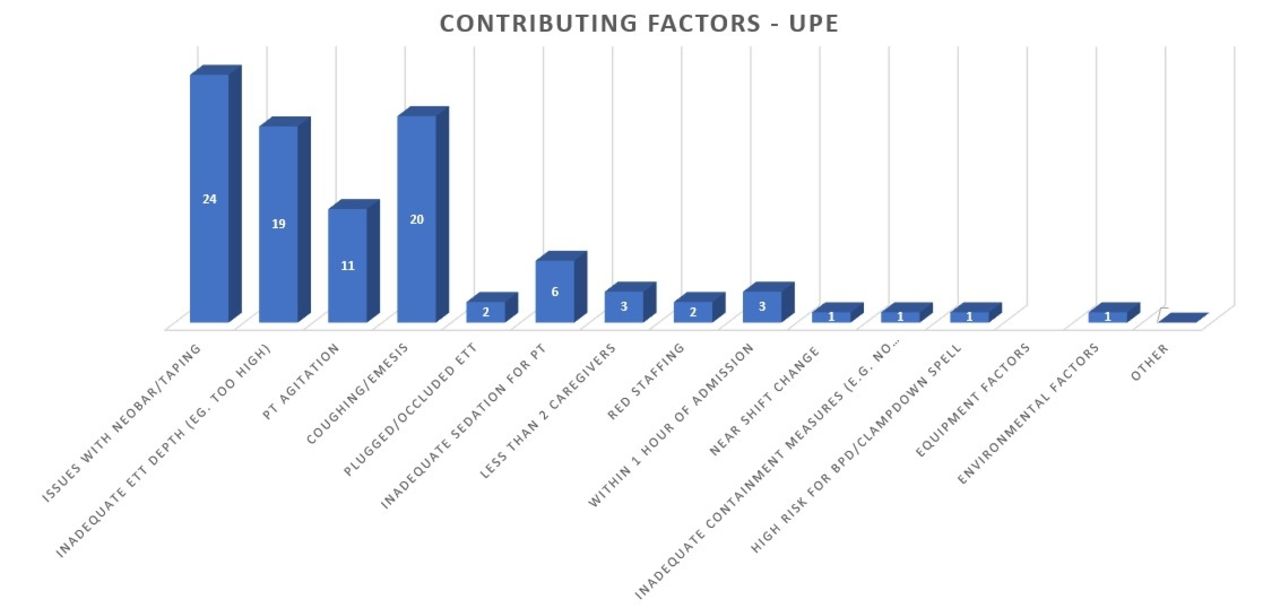
Our interdisciplinary UE committee meets monthly to complete an apparent cause analysis of each UE event. After the investigation is complete, the committee trends data on a dashboard and identifies countermeasures based on trends. The UE committee utilizes the IHI Model for Improvement and completes PDSA cycles. Our PDSA cycles include: 1. Developing standardized practices (ETT placement, 2-person positioning). 2. Increased situational awareness through an ETT card and order set. 3. Standardizing ETT securement method. 4. Developing an annual awareness month to promote bundle compliance and discuss new trends from ACAs. 5. Interdisciplinary UE debriefing led by a physician. 6. Chest radiograph standardization including optimal patient positioning and annotation of ETT position.
Results:
Our NICU had two centerline shifts: in June 2018 (decrease from 1.724 to 1.089) and in July 2021 (1.089 to 0.56). We increased compliance with UE debriefing from 45% to 53% of all events. We were to maintain 100% reliability to our UE prevention bundle (2 people for retaping, standardized landmark and standardized securement method). Our longest record between events is 72 days. We promoted intervention and data transparency through quarterly emails, nursing/respiratory updates, daily management system, and celebrations of milestones.
Conclusions:
Reducing UE remains a top priority for our NICU with an engaged committee and increased staff awareness. The culture of safety has shifted towards increased escalation of concerns and proactive discussions of high-risk patients. With the support of key stakeholders and sponsors, we were able to remove barriers and promote accountability of compliance of targeted interventions. Staff are empowered to escalate concerns through use of error prevention tools and a collaboration algorithm that proactively address securement concerns. We also identified that continuous assessment of previous interventions is necessary as they may cause unanticipated consequences.
Get full access to this article
View all access options for this article.
