Abstract
Background:
Bronchospasm occurring during anesthesia is commonly treated with albuterol via a pressurized metered dose inhaler (pMDI). A laryngeal mask airway (LMA) during anesthesia is frequently used to maintain an open airway and provide support during anesthesia. The aim of this study was to evaluate delivery of albuterol administered through an LMA using a model of a spontaneously breathing infant and child.
Methods:
A ventilator (breathing frequency 30 breaths/min, tidal volume 50 or 100 mL, PEEP 5 cm H2O, FIO2 0.21) was connected in series to an unheated ventilator circuit, pMDI delivery device (valved holding chamber [VHC] or adapter), LMA (size 1, 1.5 or 2 modified to create a seal), filter, and test lung (Rp20, 5 mL/mbar). Tidal volume (VT) was measured with a flow analyzer placed between the LMA and filter prior to aerosol delivery. Four actuations of albuterol 90 µg were delivered during inspiration or expiration either as a single actuation, waiting at least 30 s (allowing 15 breaths) and shaking between actuations, or multiple actuations without waiting/shaking. Albuterol mass was measured via spectrophotometer. Each condition was repeated in triplicate. The dependent variable was delivery efficiency (mass captured in the filter expressed as percentage of nominal dose). General linear regression (LMA size, VT, device, single vs. multiple actuations, and timing of actuation) and descriptive statistics were performed. Comparison between otherwise similar variables but different device, different tidal volume, use of single and multiple actuations, timing of pMDI actuation, and LMA size were made with T-test.
Results:
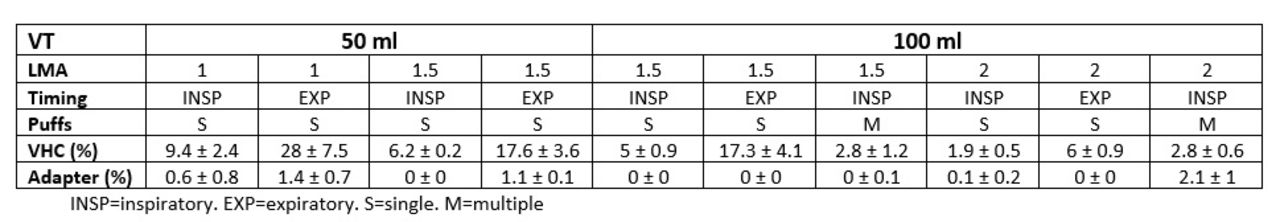
VHC had higher delivery efficiency than adapter (P < .05). Larger LMA size did not improve delivery efficiency except when for VHC/VT 100 mL/both actuation timing (P < .036). No differences were found between different tidal volumes or single vs. multiple actuations (P > .05). There was a 3-fold increase when actuation occurred during expiration while using VHC (P < .04). R2 was 0.623 with the type of device, timing of actuation, and tidal volume explaining 33%, 17% and 8% of the observed variation respectively.
Conclusions:
Delivery efficiency of albuterol pMDI through small size LMAs in a model of a spontaneously breathing infant and child increased with use of a VHC, actuation during expiration, and with small tidal volumes.
Get full access to this article
View all access options for this article.
