Abstract
Background:
Pulsed oxygen sources rely on pressure triggering to detect inhalation: during inhalation, room air entrainment creates a small drop in pressure monitored through the cannula tubing, referred to herein as the signal pressure. When the signal pressure exceeds the triggering threshold of a pulsed-flow oxygen device, a pulse of oxygen is released. Patients may struggle to trigger oxygen delivery during sleep, oral breathing, or other circumstances characterized by low nasal inhalation flows. To address this issue, a new nasal interface that can provide higher and more consistent signal pressures is being developed.
Methods:
Eight volunteers ranging from 22-47 years old participated in the study. Each volunteer was asked to breathe at different flows through their nose while connected to an oxygen tank with a Philips SimplyGo Mini POC, an OxyGo Next POC via standard nasal cannula, or the new nasal interface. A Precision Medical Easy Pulse 5+6 oxygen conserving device was used with the tank. To monitor flows, a respiratory belt (Respiration Sensor, TTLP2HRVSYS, Bio-medical Instruments, MI) was strapped around each participant’s chest. The respiratory belt was calibrated using spirometer data (MicroLoop Spirometer, #ML3535-S, Micro Medical, ME). Tests were repeated while participants breathed through their mouths. Video recordings with a close-up view of the oxygen sources were used to detect pulse triggering. Each participant breath was retroactively matched with a pulse/no pulse response, and the number of pulses was divided by the number of breaths to calculate triggering success rates. A two-tailed t-test (P <.05) was conducted with triggering success rate as the dependent variable and cannula type as the independent variable. Ethics approval was granted by the NAIT Research Ethics Board.
Results:
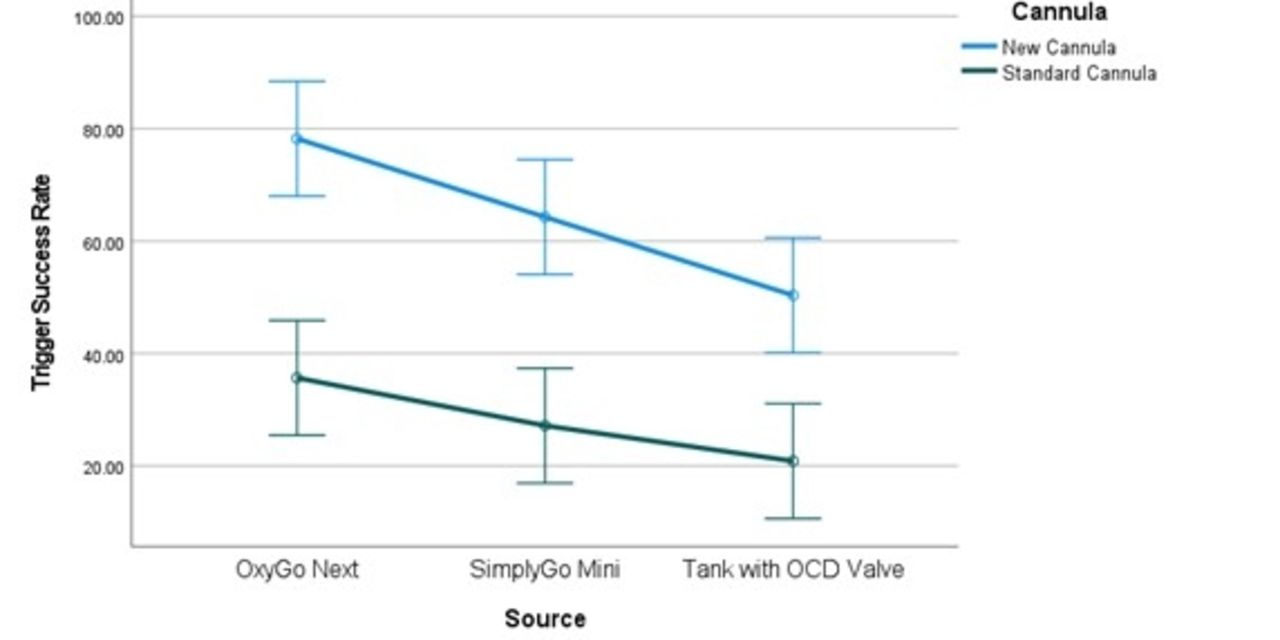
Pooled across all study conditions, triggering success rates were significantly higher (P = .03) when using the new nasal interface (78.9%) compared to the standard nasal cannula (65.2%). When using a standard nasal cannula during oral breathing, mean triggering success rates were below 40% for all oxygen sources. Using the new nasal interface approximately doubled oral breathing triggering success rates.
Conclusions:
Reliable breath detection is an issue when using pulsed-flow oxygen sources, especially during oral breathing. Significantly improved breath detection was observed when healthy participants used the new nasal interface versus a standard nasal cannula.
Figure 1: Average triggering success rates (%) when using a Standard Cannula and the New Nasal Interface. Error bars represent standard deviations. Data is pooled across all breathing patterns and oxygen sources. Figure 2: Triggering Success Rates during Oral Breathing sorted based on Cannula Type and Oxygen Source. Error bars represent standard errors.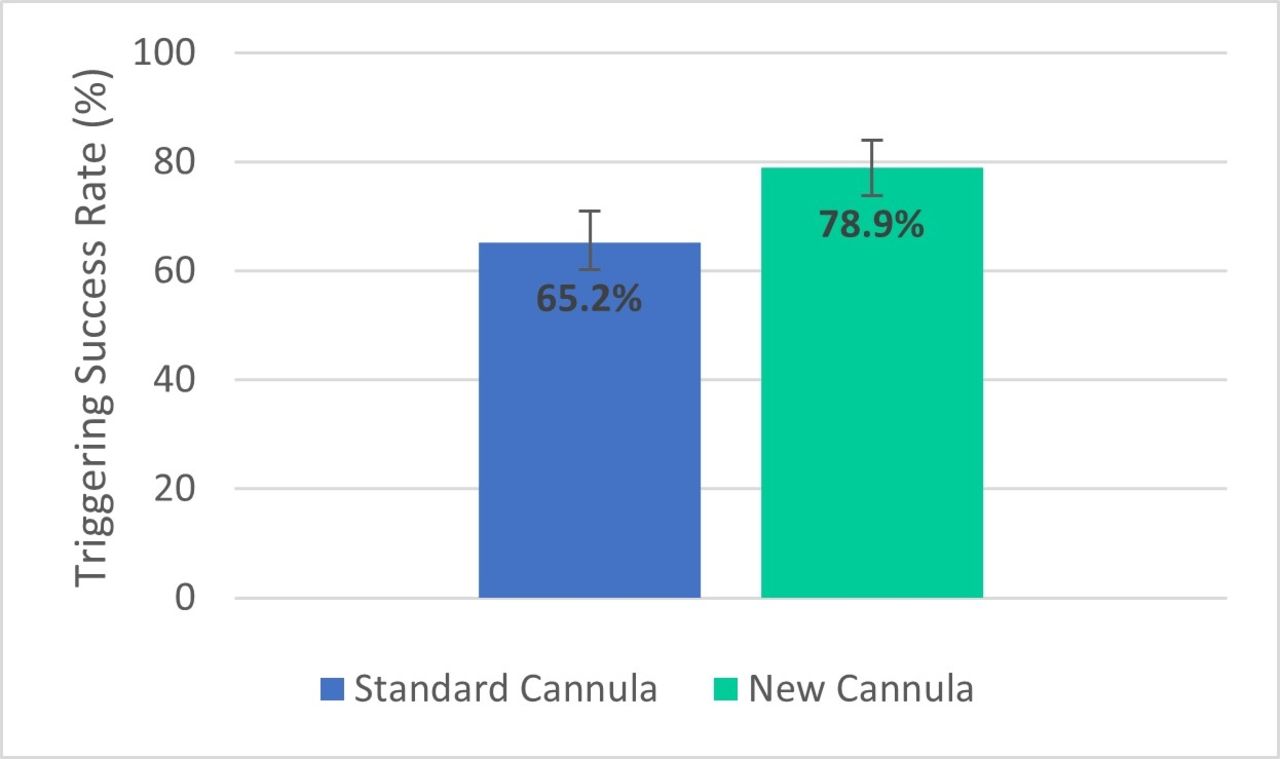
Get full access to this article
View all access options for this article.
