Abstract
Background:
Peak flow meters (PFM) are small portable devices that are used in the asthmatic population to measure how fast a patient can blow air out of their lungs with a forceful exhalation. Spirometry is a physiological test that measures how a patient inhales or exhales gas as a function of time and includes a measurement of the patient’s peak expiratory flow. Accuracy of PFM has been widely studied, but data on device is reliability and accuracy when compared to a patient’s actual spirometry peak flow (PF) has not been explored. At our institution, PFMs are used to measure asthma patient’s PF before and after allergy immunotherapy to monitor for adverse reactions, and occasionally those patients will perform spirometry to monitor their lung function and status of their asthma. We aimed to determine how the PFM measurement compared to the spirometry measured PF.
Methods:
In an IRB approved retrospective analysis, we compared PFs measured with a PFM versus spirometry PF for our pediatric asthma patients receiving allergy immunotherapy from Jan 2017- May 2022 (n = 150). Spirometry testing was performed immediately after the patient performed a PF maneuver with a PFM. We analyzed the PFM measurement with the spirometry and compared them to the predicted PF value for that patient at our outpatient allergy clinics.
Results:
In patients ages 6 to 20 (mean 12.9 years, n = 150), the PFM measured higher than the spirometry PF by a mean of 99.22 L/min (35.93% higher). When compared to the predicted PF, the PFM was higher by a mean of 104.70 L/min (17.85% higher). When comparing measured spirometry PF to the predicted, the spirometry was higher by a mean of 8.91 L/min (0.19% higher).
Conclusions:
When comparing spirometry PF measurement to predicted PF measurement on an individual patient basis, the PFM measured much higher by a significant amount (P < .001), displaying that this device is not as reliable as a spirometry PF measurement. While pre and post PF measurements regarding allergy immunotherapy side effects may be useful, this information can not be used to effectively or reliably determine an asthma patient’s actual PF. More research is needed to determine the cause of the discrepancy between the PFM and spirometry PF.
Graph 1 shows the difference in correlation between spirometry PEF (blue) and peak flow device measurement (orange) to the predicted peak flow for each patient.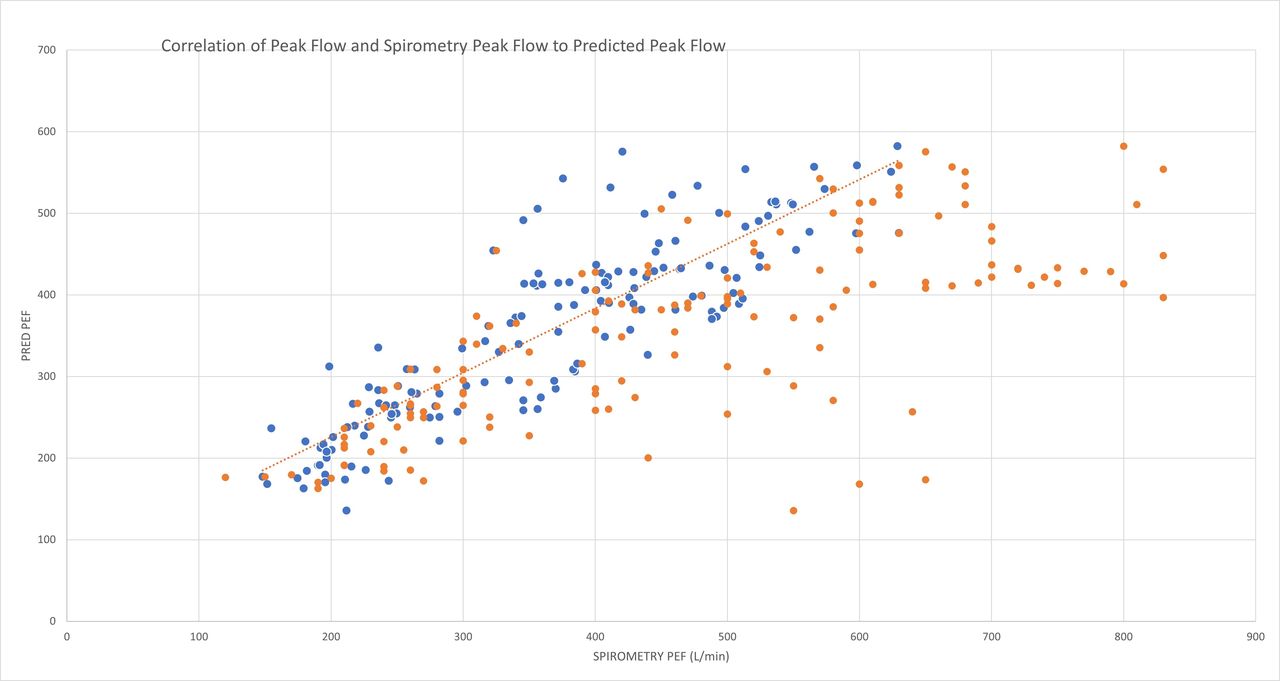
Get full access to this article
View all access options for this article.
