Abstract
Background:
Frequent flyer hospital visits account for a disproportionately large share of overall visits and costs. A 2011-2012 Intermountain Healthcare study investigated factors driving high hospitalization rates of COPD frequent flyers. We repeated this study on new subjects for 2019-2021 to detect changes in demographics, treatment, comorbidities, and non-compliance. Following the original study, initiatives were implemented to improve COPD patient care. Additionally, in 2017, the Pulmonary Disease Navigator (PDN) scope was expanded to include COPD.
Methods:
For 2019, 2020, and 2021, we extracted adult subjects assigned a COPD exacerbation diagnosis associated with ≥ 5 visits (ER or admission) per year at all Intermountain hospitals. We performed retrospective electronic medical record reviews on these subjects, including all variables from the original study. To assess differences between cohorts in age, ages were grouped into 30-60 and >60 due to limited data, then compared with a chi-square test. For cohort differences in comorbidities, each variable was compared with a z-test. Pearson correlation was used to identify relationships between comorbidities in the 2020-2021 cohort.
Results:
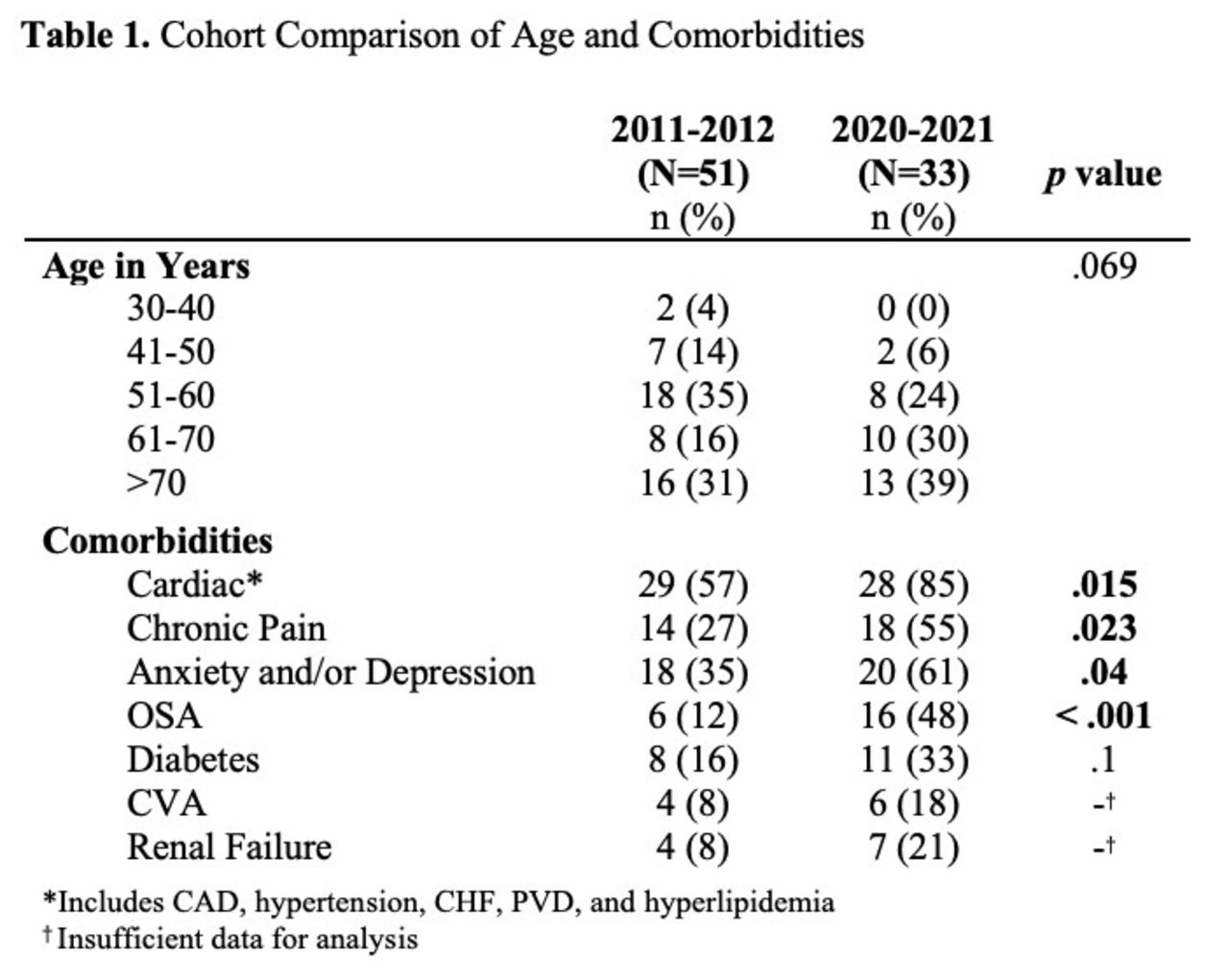
We identified 33 subjects with ≥ 5 visits per year during 2020-2021. There was a significant difference between cohorts in proportions of cardiac, chronic pain, anxiety and/or depression, and OSA comorbidities. For the 2020-2021 cohort, OSA and diabetes were significantly positively correlated (P = .05). 61% of the 33 subjects are followed by a PDN. Other results are reported in accompanying abstracts.
Conclusions:
Compared to the previous cohort, a larger proportion of subjects in the current cohort have cardiac, chronic pain, anxiety and/or depression, and OSA comorbidities. At the same time, we extracted fewer subjects, which may conclude that COPD patient care has improved, and remaining frequent flyers have more complex health conditions. The current cohort may also have a smaller proportion of young subjects and larger proportion of old subjects, contributing to comorbidities. Possibly influenced by a rising national BMI, OSA is the most significant change and will be addressed by the OSA navigator role being developed. This study was limited by a small sample size and no access to the original dataset. We conclude a reduction in COPD frequent flyers and that these subjects have increased comorbidities, possibly due to a concentration of medically complex subjects and a possible shift toward older age.
Get full access to this article
View all access options for this article.
