Abstract
Background:
At our institution, in the outpatient primary care settings, orders for a written asthma action plan (AAP) with education and pulmonary function testing (PFT) are currently entered at the discretion of the licensed independent practitioner (LIP). A chart review revealed that AAPs and PFTs were not consistently ordered based on the recommendations from the Global Initiative for Asthma Management and the National Heart, Lung, and Blood Institute Expert Panel Report 3 asthma management guidelines. A respiratory therapist (RT)-driven protocol was developed as a quality improvement study aimed to increase frequency of PFTs and AAPs in primary care clinics. This protocol allows the RT to order PFTs and AAPs for children with asthma who meet specific criteria. The aim of this study was to evaluate provider acceptance of an RT-driven protocol and to assess barriers regarding protocol implementation.
Methods:
A survey was created and sent electronically to LIPs prior to implementation of the RT-driven protocol. Survey questions focused on RT availability, barriers to ordering PFTs and AAPs, comfort with utilizing PFT results, and importance of asthma education. The survey was repeated 6 months post protocol implementation with additional questions regarding LIP satisfaction with the RT-driven protocol. Responses were collected in REDCap.
Results:
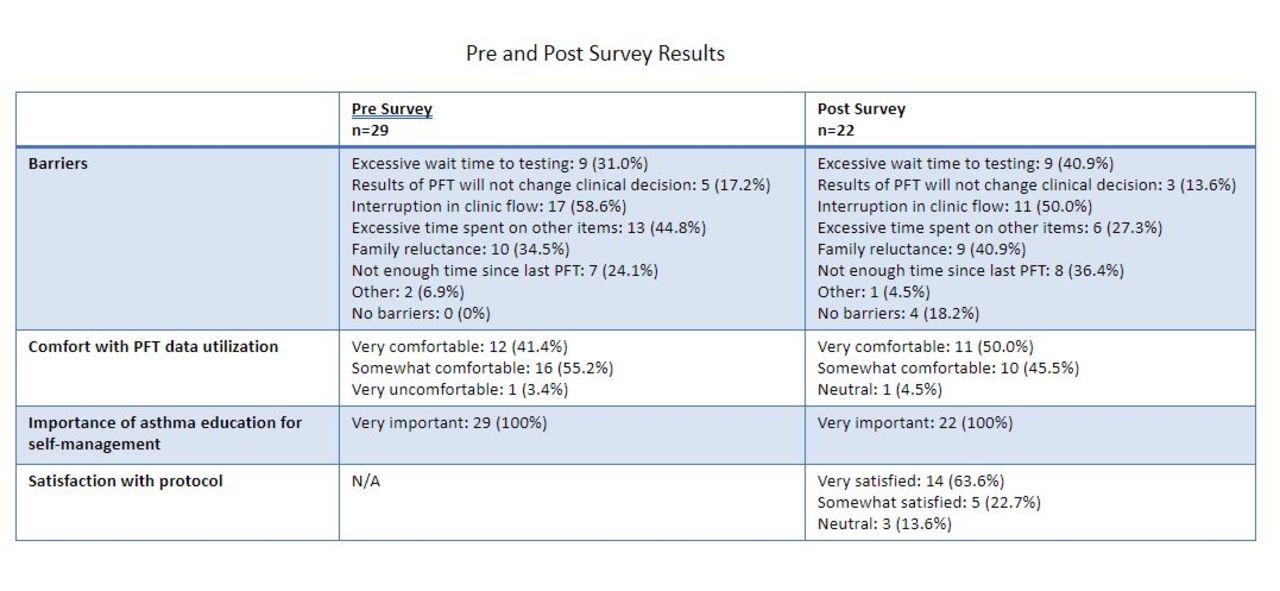
The survey was sent to 115 LIPs. The survey was completed by 29 (25%) and 22 (19%) LIPs pre and post protocol respectively. The pre protocol survey identified interruption to clinic flow as the main barrier to ordering PFTs (17, 58.6%). The majority (28, 96.6%) were comfortable utilizing PFT data for clinical decision-making. All respondents indicated asthma education is important for self-management of asthma. In the post protocol survey, half of all respondents identified interruption to clinic flow as a barrier to LIP ordering PFTs (11, 50%). Most (21, 95.5%) LIPs felt comfortable utilizing PFT data for clinical decision-making, and all continued to report asthma education is an important part of asthma self-management. The majority (19, 86%) were satisfied with the RT-driven protocol.
Conclusions:
Interruption to clinic flow was the main barrier identified by LIPs for ordering PFTs. All LIP respondents felt that asthma education is important for self-management. Providers were satisfied with an RT-driven protocol for ordering PFTs and AAPs in the primary care setting.
Get full access to this article
View all access options for this article.
