Abstract
Background:
Recent publications document less than 5% of patients with a qualifying lung disease are enrolled into a pulmonary rehab program. Limitations such as access, transportation, and financial concerns effect patients attending center-focused pulmonary rehab (CFPR). The COVID-19 pandemic created additional barriers for the care of patients, further limiting access to CFPR. In spring of 2020, the Centers for Medicare and Medicaid Services (CMS) temporarily expanded its coverage to include telehealth services. We assessed the effectiveness of remote rehab compared to CFPR during the pandemic.
Methods:
We developed a remote pulmonary rehab (RPR) program to safely monitor patients in their home while participating in remotely-guided pulmonary rehabilitation. From October 2020 through July 2021, 21 patients completed the program (11 RPR, 10 CFPR). Outcome measures in all patients on site included: Timed Up and Go (TUG), 6-min walk distance, Metabolic Equivalency Threshold (METS), and fragility measurement (grip strength) at baseline and upon program completion (9 to 12 weeks). RPR patients were provided Therabands, a pulse oximeter, video tablet, and educational booklet. Sixty-minute remote sessions including up to 4 patients were led by an exercise physiologist or respiratory therapist utilizing the Vidyo application. Like CFPR, RPR sessions included education, monitoring, and exercise, but only CFPR had access to aerobic exercise equipment.
Results:
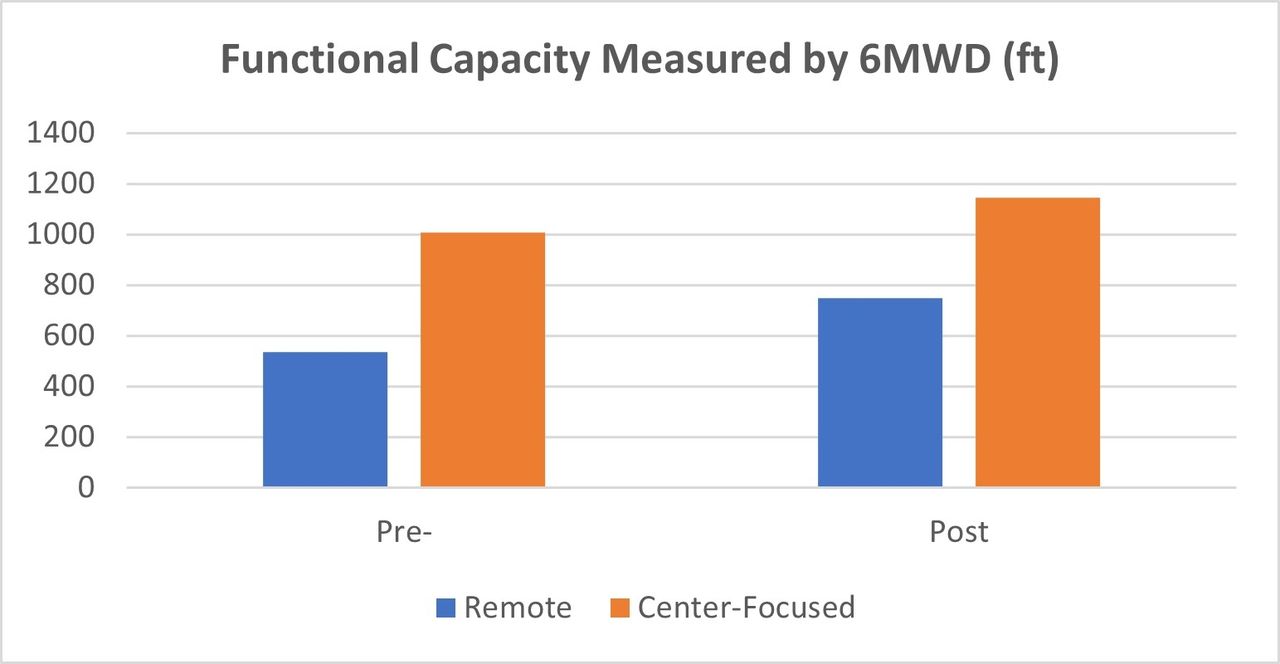
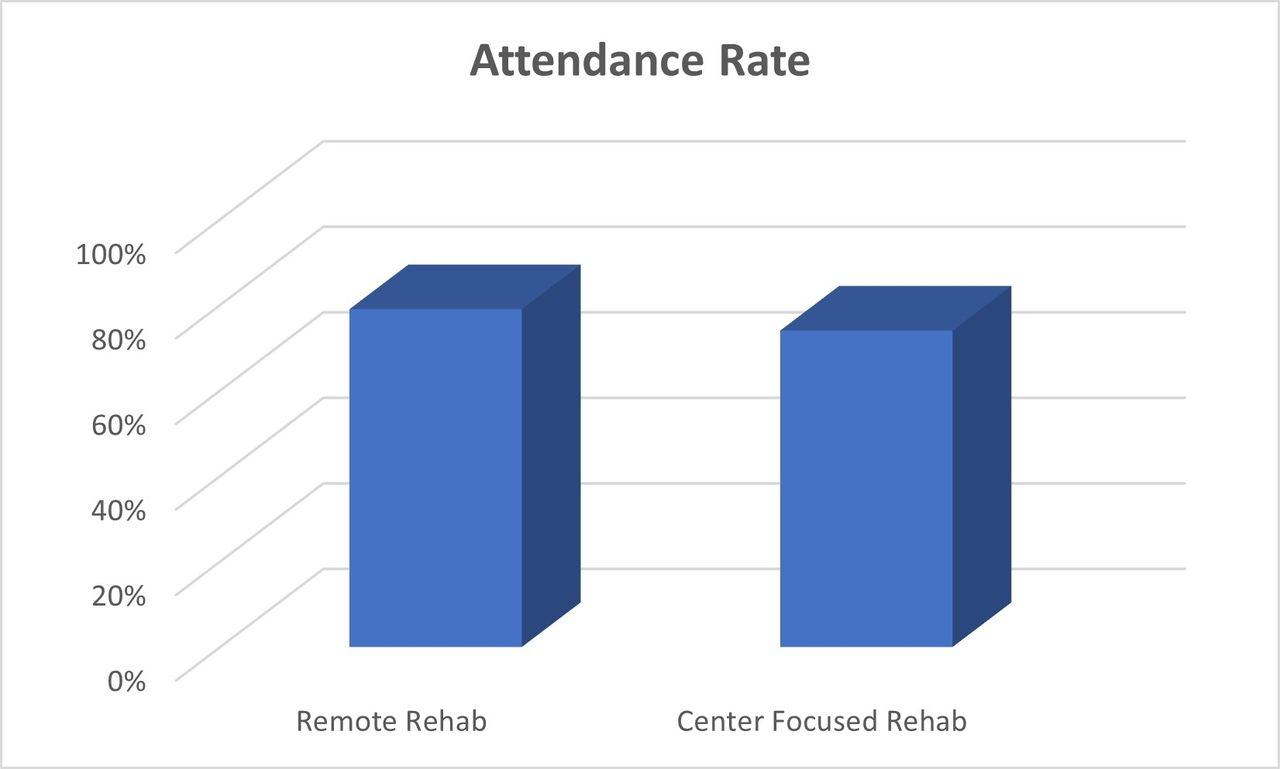
RPR patients had a 79% attendance rate versus a 74% attendance rate in center-focused rehab. 73% of patients attending RPR and 70% of patients completing CFPR met minimum clinically important differences for 6-min walk functional capacity (98 feet). TUG measurements improved in 64% of the remote population and 90% in the CFPR. Grip strength measurements improved in 73% of the RPR group and 90% in the CFPR group. METS obtained from a recumbent cycle improved in 45% of the remote population and 70% in CFPR.
Conclusions:
Telehealth allows accessibility for those needing pulmonary rehab, particularly during the pandemic. While objective testing demonstrated a greater proportion of improvers within the CFPR program, RPR patients exhibited improvements in objective outcomes justifying the continuation of telehealth service for pulmonary patients with limited accessibility.
Get full access to this article
View all access options for this article.
