Abstract
Background:
The purpose of this study was to compare indirect calorimetry to use of a body weight equation to determine nutrition needs of critically ill patients and whether one method leads to better outcomes. A secondary purpose was to determine what percent of the prescribed nutrition critical care subjects receive.
Methods:
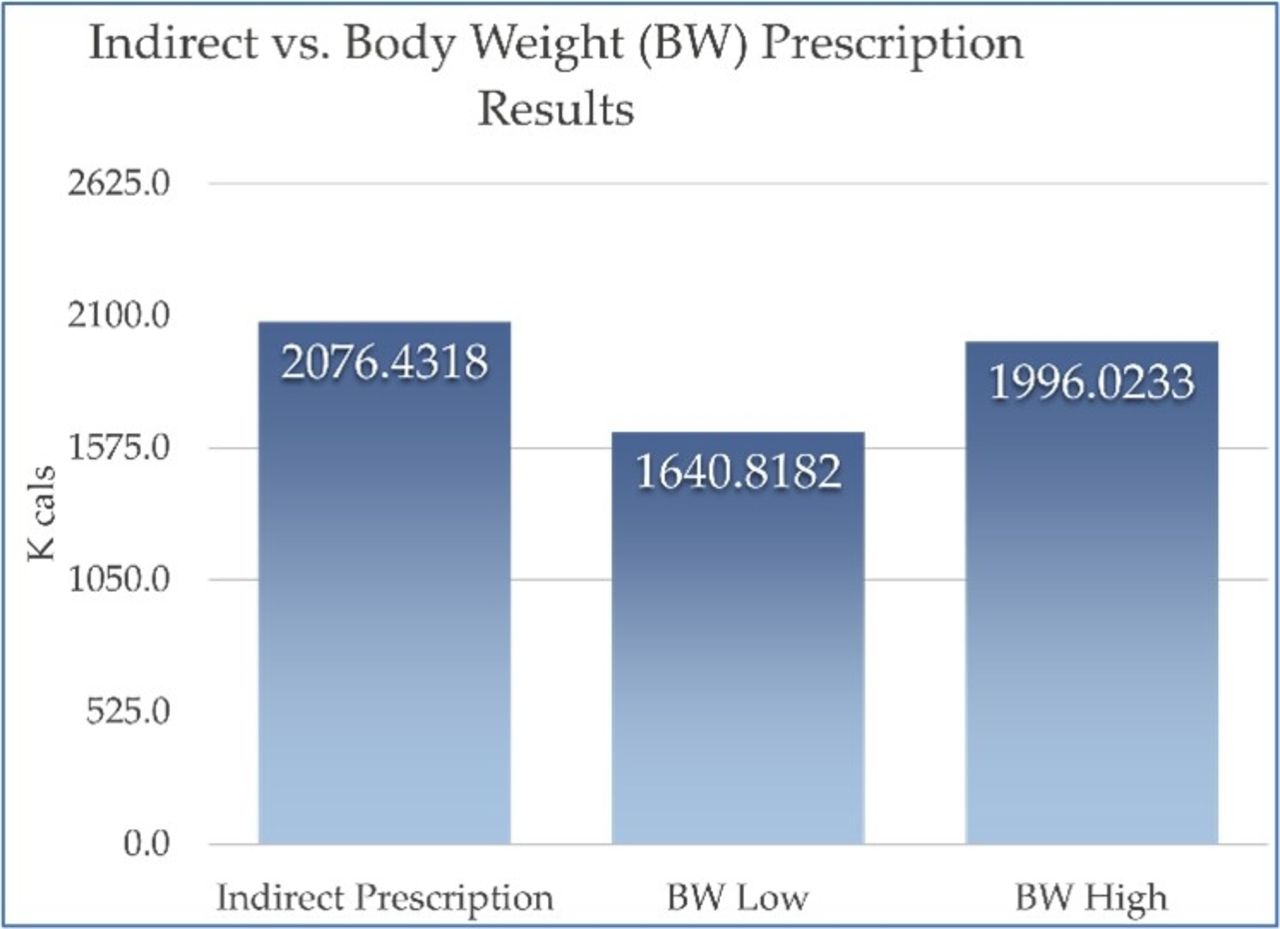
Approval from the Honor Health IRB was obtained. A quantitative design was used. Length of stay and ventilator days were compared between the groups who had indirect calorimetry used to calculate nutrition needs vs those who had nutrition needs determined by the standard body weight equation. In addition, the intervention group had both a body weight equation and indirect calorimetry to compare how close the two prescriptions were. The percentage of prescribed nutrition that a patient received was calculated by comparing total nutrition ordered to total nutrition received.
Results:
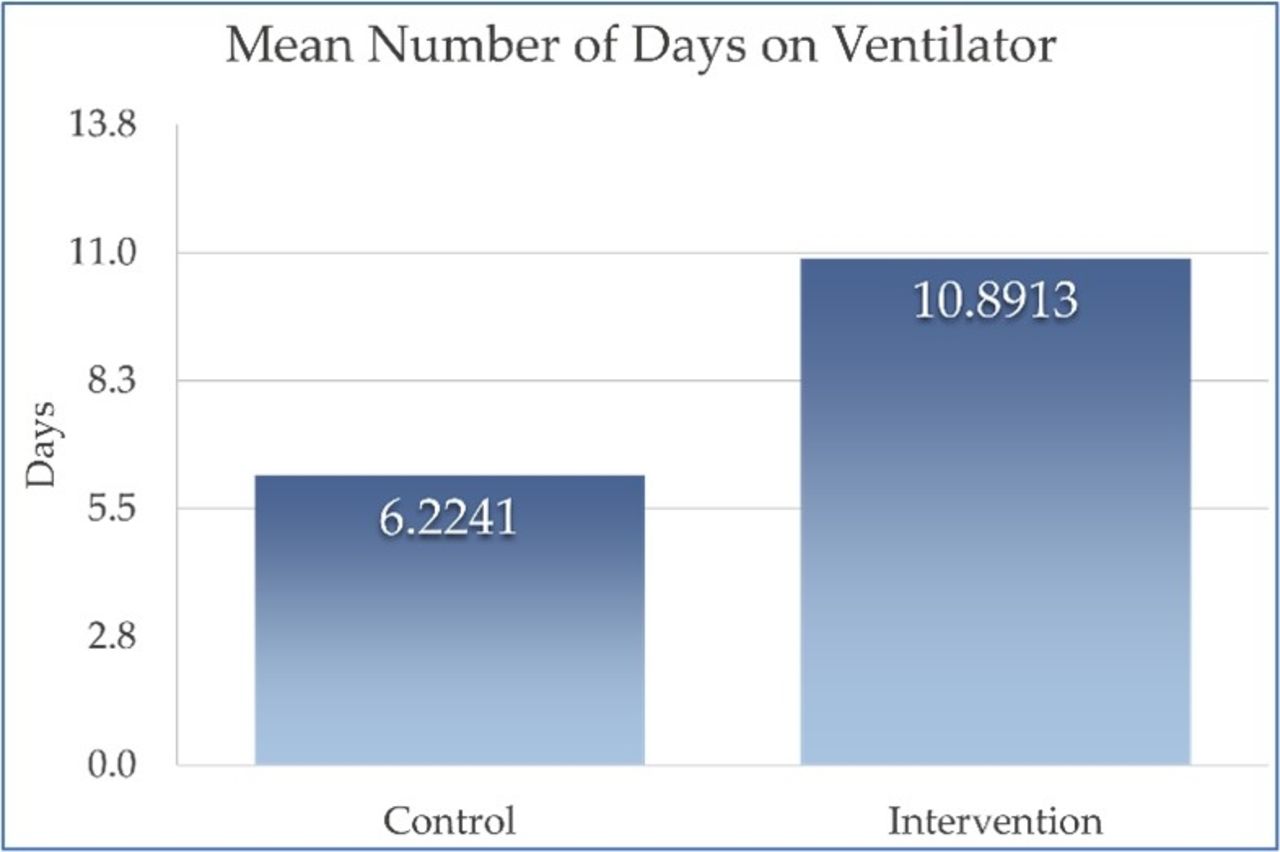
The intervention group and the control group were well matched by demographics and did not differ statistically on the key dependent variables: time on ventilator and length of stay in the ICU. The groups also did not differ on the percent of prescribed nutrition that they received, though in both groups it was only approximately 70% of what was prescribed. The COVID-19 pandemic may have contributed to the results. A shortage of rooms made it difficult to move ICU patients to a lower level of care and that may have contributed to the increased length of stay in the ICU. Staffing issues may have also impacted ventilator weaning because of the large number of ICU patients on ventilators
Conclusions:
Since both groups only received roughly 70% of their nutrition, more work must be done to improve the processes used to meet the nutritional needs of our patients. More studies need to be done to determine if length of stay and ventilator days do decrease when patients receive their full prescribed nutrition amount. If this study were to be repeated it would be important to study the groups concurrently to ensure that they are subject to the same external forces. In this case, patients in the intervention group were hospitalized during the COVID-19 pandemic. That resulted in an increased census, higher acuity patients, a lack of beds, and staffing shortages. Generalizability of the study findings is limited by the non-probability convenience sample of the participants and retrospective nature of the control group. The study sample size was also small. A larger sample would increase statistical power.
Get full access to this article
View all access options for this article.
