Abstract
Background:
Nishimura reported in his article regarding respiratory care in 2016 that high-flow nasal cannula (HFNC) was a reliable therapy device for respiratory failure patients with hypercapnia. However, we often experienced carbon dioxide narcosis in patients using Venturi-effect typed HFNC (HFNC/Venturi). PURPOSE We hypothesized that oxygen concentration was increased by back pressure in the circuit of HFNC/Venturi which was produced during breathing.
Methods:
FIO2 on HFNC/Ventrui was adjusted to 32%, which is the minimum concentration (MaxVenturi, Maxtec, US). Three volunteers using the Venturi-effect typed HFNC maintained stable breathing for 30 seconds. Then, the back pressure and the oxygen concentration in the circuit during their stable breathing were measured three times for each examinee. The experimental conditions used are shown as below. Total flow: 20 to 60 L/min. Breathing style: mouth and nose.
Results:
Back pressure in the mouth breathing when the total flow was 60 L/min reached a median of 14.2 cm H2O (interquartile range [25th to 75th percentile], 14.0 to 14.2), as compared with 1.65 cm H2O (IQR, 1.60 to 1.80) in that of the total flow 20 L/min (P < .001). In the nose breathing, back pressure of the total flow 60 L/min reached a median of 15.9 cm H2O (IQR, 15.4 to 16.3), as compared with 1.90 cm H2O (IQR, 1.63 to 2.18) in the total flow 20 L/min (P < .001). Similarly, the oxygen concentration in the circuit increased significantly in proportion to the increase of the total flow (figure).
Conclusions:
The results support the hypothesis that FIO2 in the circuit of the Venturi-effect typed HFNC would increase in proportion to the back pressure produced during breathing. Therefore, the use of the Venturi-effect typed HFNC in COPD is recommended to be avoided in clinical situations.
Oxygen concentration in the circuit of the Venturi-effect typed HFNC on the setting: FIO2 32%: It increased in proportion to total flow in both breathing styles. Especially, the measured oxygen concentration of nasal breathing was significantly higher than that of mouth breathing.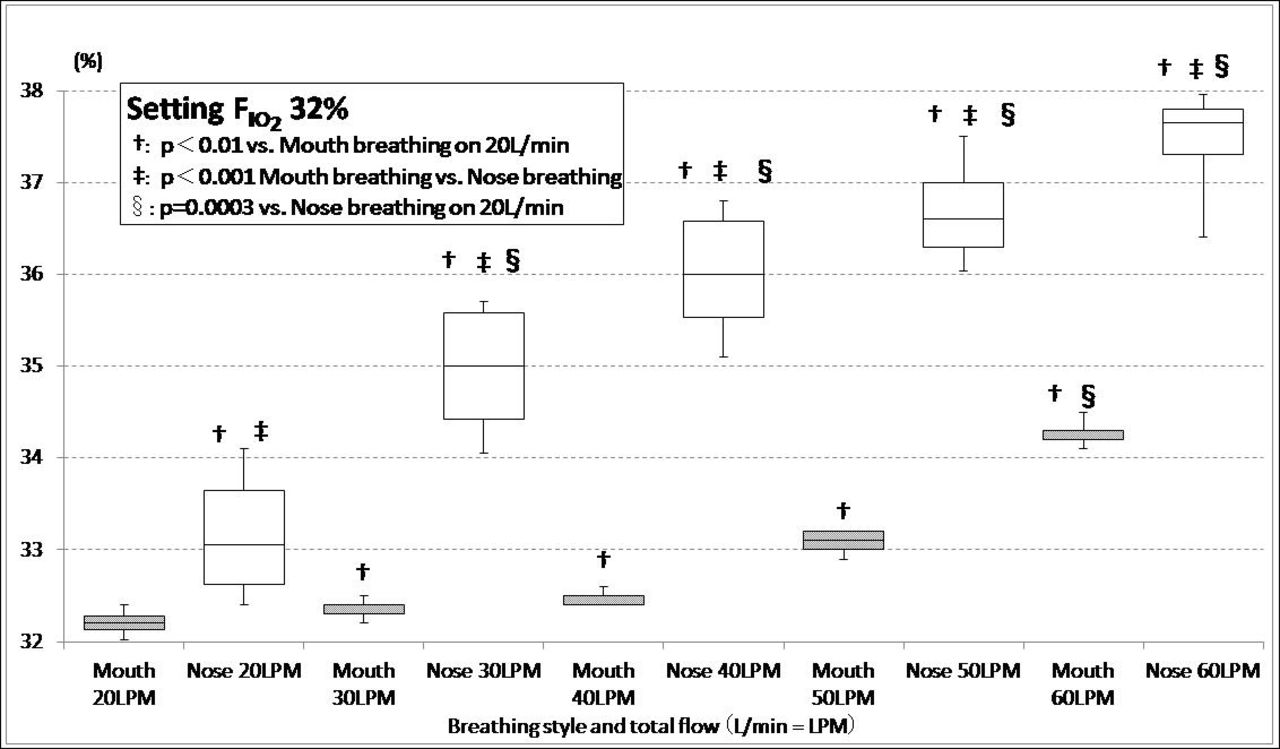
Get full access to this article
View all access options for this article.
