Abstract
Background:
The Center for Disease Control (CDC) and National Health Safety Network (NHSN) have defined VAE as a deterioration in respiratory status following a period of stability-determined by PEEP or FIO2, evidence of inflammation or infection-determined by patient temperature and white blood cell count or lab evidence of a respiratory infection. VAE rate is defined as the number of events per 1000 ventilator days. The VAE rate had been higher than expected in our adult Surgical/Trauma and Neuro ICUs. We wanted to determine if a performance improvement process could reduce that rate. METHOD: This is a retrospective review of all ventilator patients in our Surgical/Trauma and Neuro ICUs during the baseline (January 2013 to September 2018) and pilot (September 2018 to present) periods. We employed a PDCA performance improvement process. The main performance improvement implementations that occurred were caregiver education on the VAE criteria and initiating a new standard baseline PEEP setting of 6 cm H2O for all ventilator patients instead of 8 cm H2O.
Results:
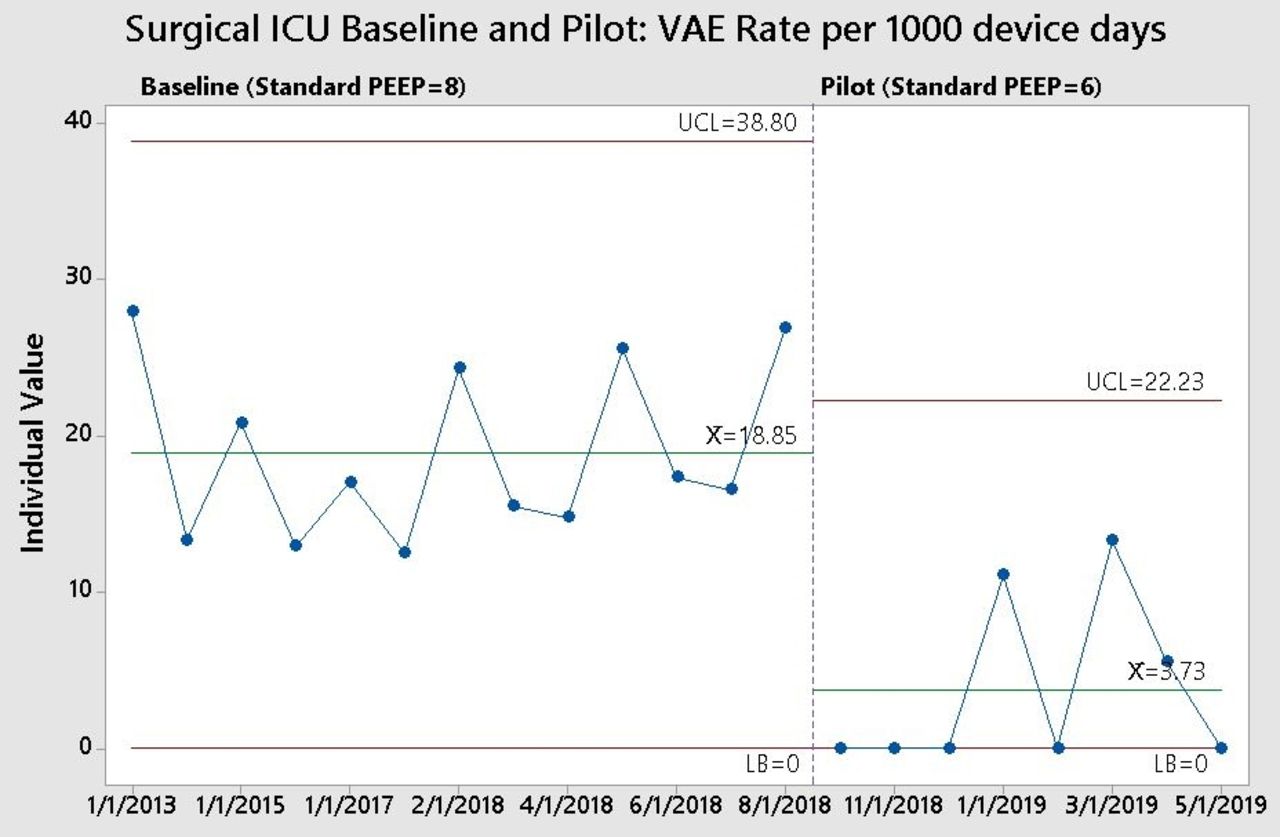
Mean VAE rates for the Surgical/Trauma and Neuro ICUs were 18.9 and 15.7, respectively, prior to project implementation. After implementation, VAE rates fell to 3.7 and 2.6, yielding an 80% and 83% reduction in the VAE rate. The reduction is statistically significant for both ICUs (P < .05). See image for control chart of VAE rate in the Surgical/Trauma ICU over time with baseline and pilot periods
Get full access to this article
View all access options for this article.
