Abstract
Background:
Setting appropriate tidal volumes for mechanically ventilated patients is an important factor in improving patient outcomes. Tidal volume settings are typically calculated in mL/kg using ideal body weight based on patient height. We discovered that height information recorded in the EMR is gathered inconsistently and may be collected by an actual measurement, verbally from patient and/or family member, or by estimation. We also discovered that our therapists were often using the EMR data to calculate ventilator settings. One quality metric we evaluate in our organization is adherence to lung protective ventilation strategies comparing documented tidal volumes and recommend volumes based on documented height in the patient electronic medical record (EMR). A potential issue for accurately calculating and reporting this data is tidal volume is accurate height measurement and accurate documentation in EMR.
Methods:
Single center, retrospective review of mechanically ventilated patients at a community-based hospital. Patient height was measured at bedside by a staff respiratory therapist upon initial vent setup. The measured height was recorded on a paper form and submitted to the RT supervisor to complete a chart review and record documented EMR height.
Results:
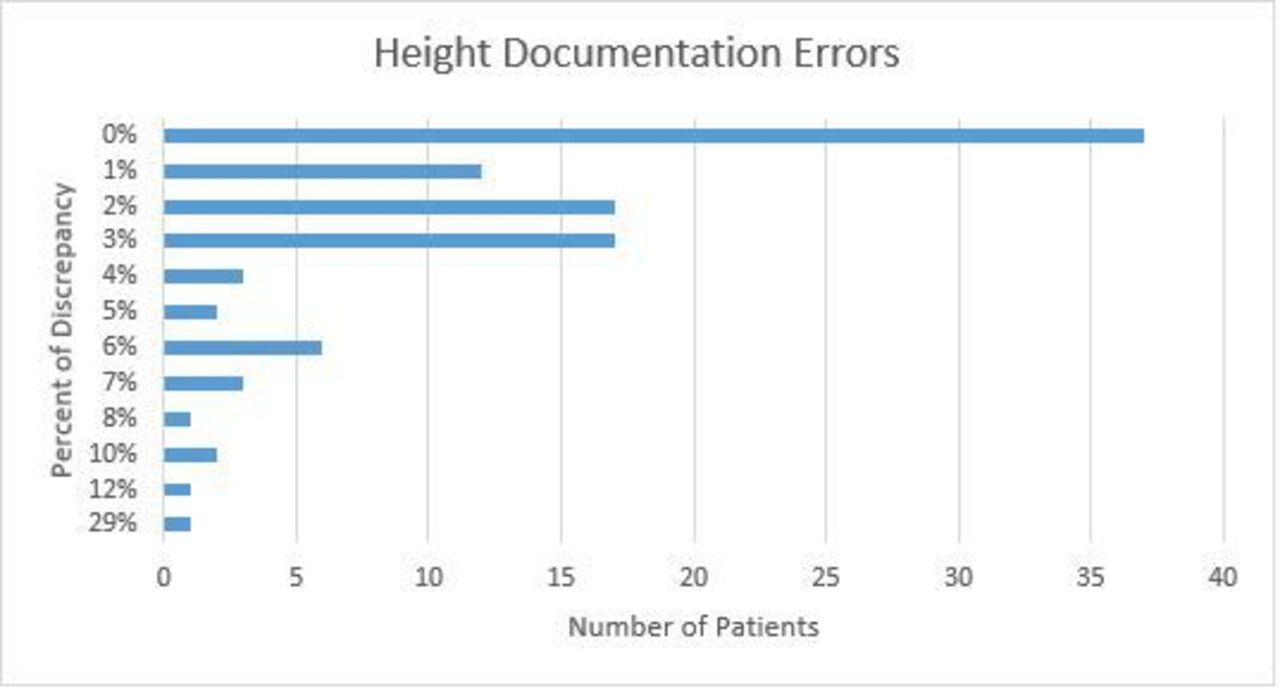
A total of 102 mechanically ventilated patients were reviewed, of these a total of 37 (36.28%) had a measured height that matched the documented height in EMR. Actual variances ranged from 1-16 inches, resulting in variances between 1-29%. 15 patients (14.71%) had a discrepancy between 1-3%, 46 (45.10%) had a discrepancy between 4-9%, and 4 (3.92%) had a discrepancy of 10% or higher. The largest discrepancy was bilateral amputee patient that had actual current length documented as height in EMR.
Conclusions:
Inconsistencies in height measurement practices, in addition to discrepancies in documented height in patient record can lead to inaccurate calculation of appropriate tidal volumes and/or inaccurate reporting and benchmarking of quality metrics. Further evaluation is needed to determine the impact on patient safety, however, there is an evident need to improve consistency in practices as well as documentation to ensure reliability of EMR data.
Get full access to this article
View all access options for this article.
