Abstract
Background:
Historically, the overall post-operative care (including, ventilator weaning) in the Cardiovascular ICU was the responsibility of the nursing staff. Respiratory therapy staff would assist with ventilator weaning on an as-needed basis. When transitioning to new ventilators, it was suggested that a dedicated Respiratory therapy team could wean the patients from mechanical ventilation in less time than a primary nurse-lead weaning approach.
Methods:
Data collected from patients' that underwent cardiac surgery from January 2017 through August 2017 was reviewed. An opportunity for improvement was noted in regards to streamlining the weaning and extubation process. A two person respiratory therapist based weaning team was put into place to focus on these patients upon arrival into the ICU. Additionally, a revised ventilator management protocol was utilized to manage these patients improving the weaning and extubation process.
Results:
Each medical discipline developed recommendations for improving patient care in their respective areas. The respiratory therapists implemented a weaning team that was focused solely on management of these post- operative patients. This allowed direct observation of respiratory patterns, selection of appropriate ventilator settings, blood gas management, and timely assessment for the readiness of CPAP. Recently, we revised the standard process to include administration of a paralytic reversal agent upon admission to the ICU. This further reduced the time for nursing staff to decrease sedation. Our standard process also included a standardized PEEP of +8 to help post-surgical alveolar recruitment and oxygenation. Finally, all staff completed Team STEPPS and Cultural Beliefs training which facilitated open communication between all team members regarding care management, patient extubation readiness, and options for oxygen devices post extubation
Conclusions:
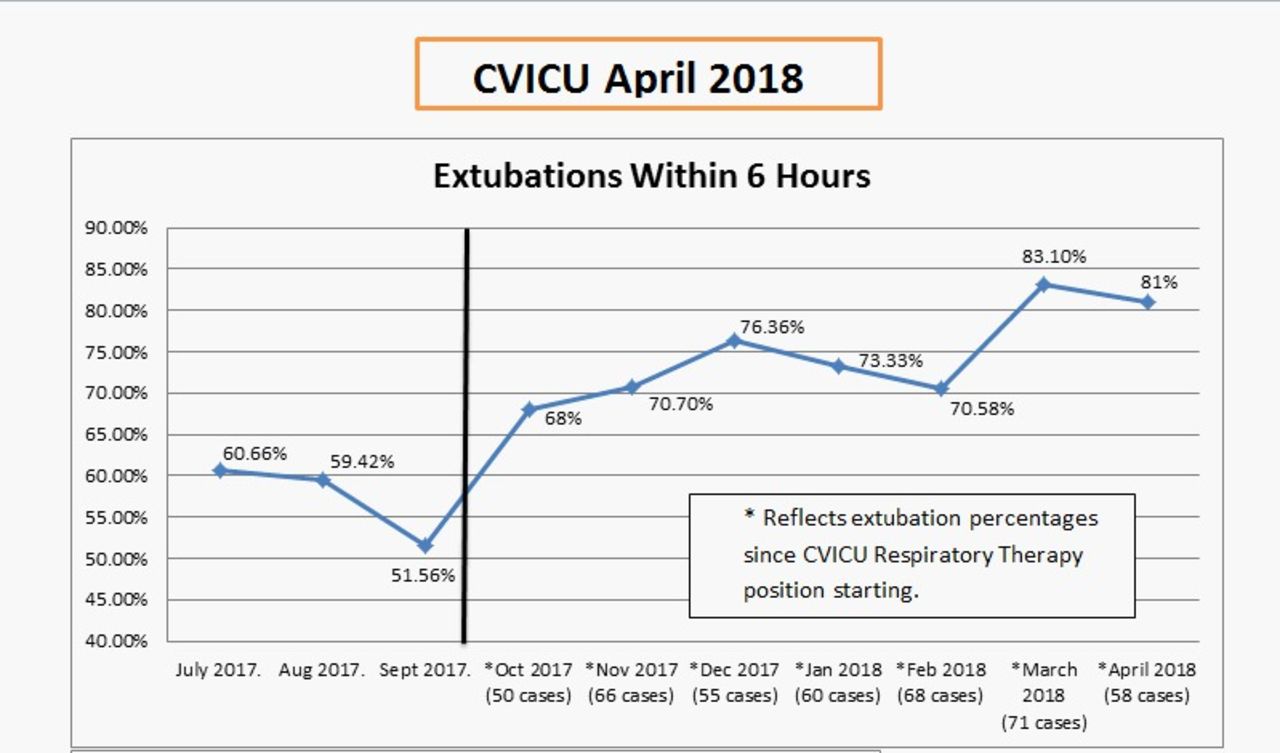
Data regarding outcomes for RT weaning of post-operative patients in the CVICU shows an increase of patients being extubated within 6 hours from 51.56% in September of 2017 to 81% as of April of 2018.
Disclosures:
None.
Get full access to this article
View all access options for this article.
