Abstract
Background:
When there's an inability to correctly estimate a pediatric lung transplant patient's caloric needs using predictive equations, there can be an inadequate clinical response due to overfeeding or underfeeding. Measuring oxygen consumption (VO2) and carbon dioxide (VCO2) production to assess resting energy expenditure (REE) can help in determining a customized nutritional plan for this specific patient population; as this population typically has a decline in their nutritional status as evident by body mass index (BMI) z-scores/weight for length pre-transplant. The purpose of our study was to utilize indirect calorimetry to obtain REE measurements with the hope to improve the nutritional status of pediatric post-operative lung transplant (PLT) patients.
Methods:
The Vmax Encore was used to do metabolic testing in patients via a canopy or in-line with the ventilator. Testing protocol includes: pre-transplant period during initial evaluation (if meets inclusion criteria), prior to discharge after transplant, 1-3 month follow-up visit, 6-9 month follow-up visit, and 1 year post-transplant.
Results:
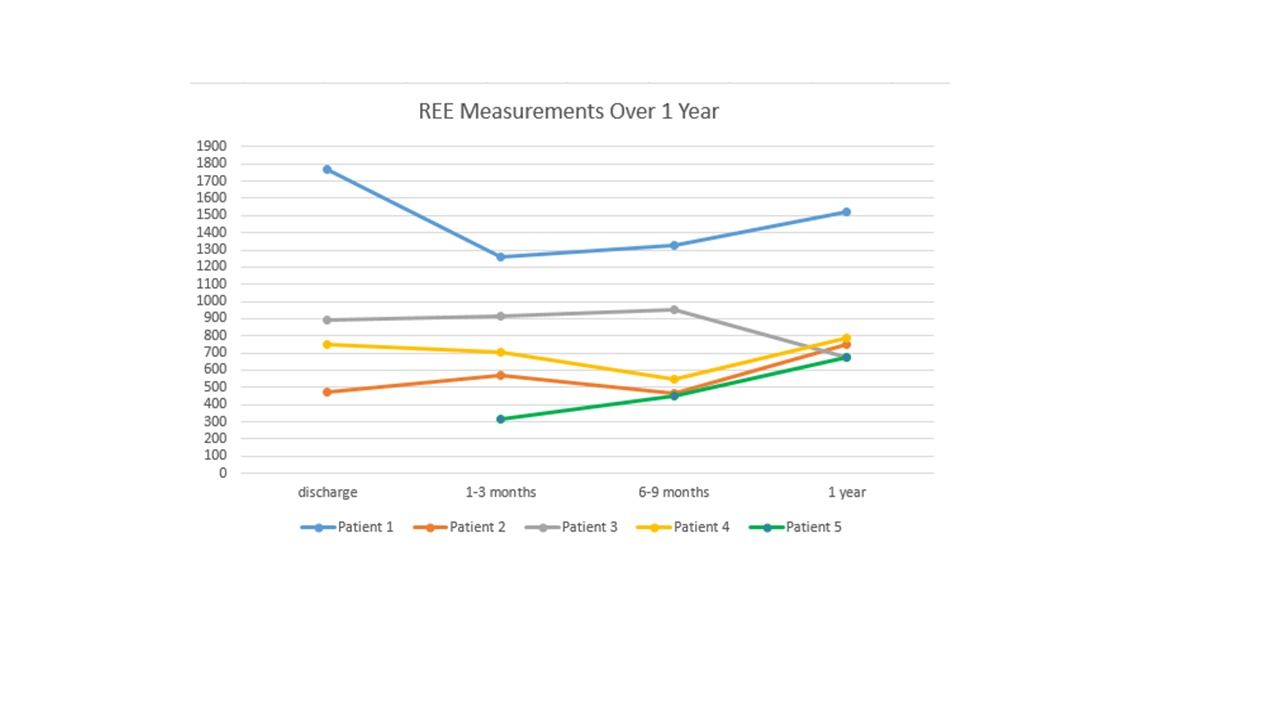
A total of 11 patients were transplanted from 12/2014- 05/2018 that were less than 15 years of age. Six patients were excluded from the results due to not meeting inclusion criteria or completing the testing protocol. Data was collected from 5 patients that showed there was an increase in BMI z-score over 1 year. One of the patients did not receive a discharge PLT study due to a prolonged admission after transplant. A total of 24 studies were administered over a 4 year period which includes: 2 pre-transplant tests, 4 discharge tests, 8 tests at 1-3 month PLT, 5 tests at 6-9 months PLT, and 5 tests were administered at 1 year PLT. The average BMI z-scores were as follows: -2.43 at discharge, -0.33 at 1-3 months, 0.388 at 6-9 months, and -0.65 at 1 year. See table 1 for REE trends over 1 year.
Conclusions:
At discharge, pediatric lung transplant patients were moderately malnourished and with the use of indirect calorimetry, a specific dietary plan was developed for each patient within the protocol that resulted in no indication of malnutrition at each of the protocol time periods.
Disclosures:
None.
Get full access to this article
View all access options for this article.
