Abstract
Background:
Obstructive sleep apnea (OSA) is associated with worse functional outcomes after stroke. Continuous positive airway pressure (CPAP) may improve stroke recovery but has been limited by poor adherence. In a single-arm study, we sought to evaluate an intensive CPAP adherence protocol during and after inpatient rehabilitation on CPAP adherence and stroke recovery.
Methods:
The adherence protocol included OSA education and an iterative process of CPAP adjustments and feedback by respiratory therapists (RTs) and nurses. A 3-night run-in period of auto-titrating CPAP 4-20 cm H2O was utilized as proxy diagnostic testing for OSA and to assess for CPAP tolerance. Qualifying patients were asked to continue CPAP for 3 months. We assessed for factors associated with 3-month CPAP adherence, defined as ≥ 4 h on ≥ 70% of nights, using logistic regression. The University of Washington Human Subjects Review Committee approved the study.
Results:
During the run-in, 74 of 90 (82%) subjects experienced problems with CPAP, most commonly mouth dryness (41%), nasal symptoms (48%) and mask fit or leak problems (49%) [see figure]. The most common adjustments were switching the mask type (28%) and adjusting the humidity (30%). Sixty-two of the ninety (69%) participants qualified after the run-in, and 32 of the 52 (62%) who continued CPAP after discharge from rehabilitation were adherent with average of 4.9 ± 2.6 h per night over 3 months. Predictors of adherence included more severe stroke [NIH Stroke Scale ≥ 5: OR 9. 7 (1.6-60.7), P=0.015] and white race [OR 9. 1 (1.7-48. 3), P=0.009]. Patients with any aphasia were more likely adherent (14/15, 93%) than those without (18/37, 49%), P=0.005. Adherence to CPAP did not differ by baseline sleepiness or body mass index.
Conclusions:
A RT-led intensive CPAP adherence protocol beginning with a short run-in period led to 3-month adherence among nearly two-thirds of stroke patients. Stroke severity, including disability with aphasia, was a significant predictor of adherence, possibly related to a symptomatic benefit in stroke recovery with CPAP or from intensive support. RTs can play a critical role in improving early CPAP acceptance even among severely disabled stroke patients through a process of close supervision with adjustments of mask fitting and machine settings. Further randomized controlled trials with adequate CPAP adherence are needed to further assess the effectiveness of intensive CPAP interventions on stroke recovery.
Common side effects of CPAP therapy during 3-night run-in period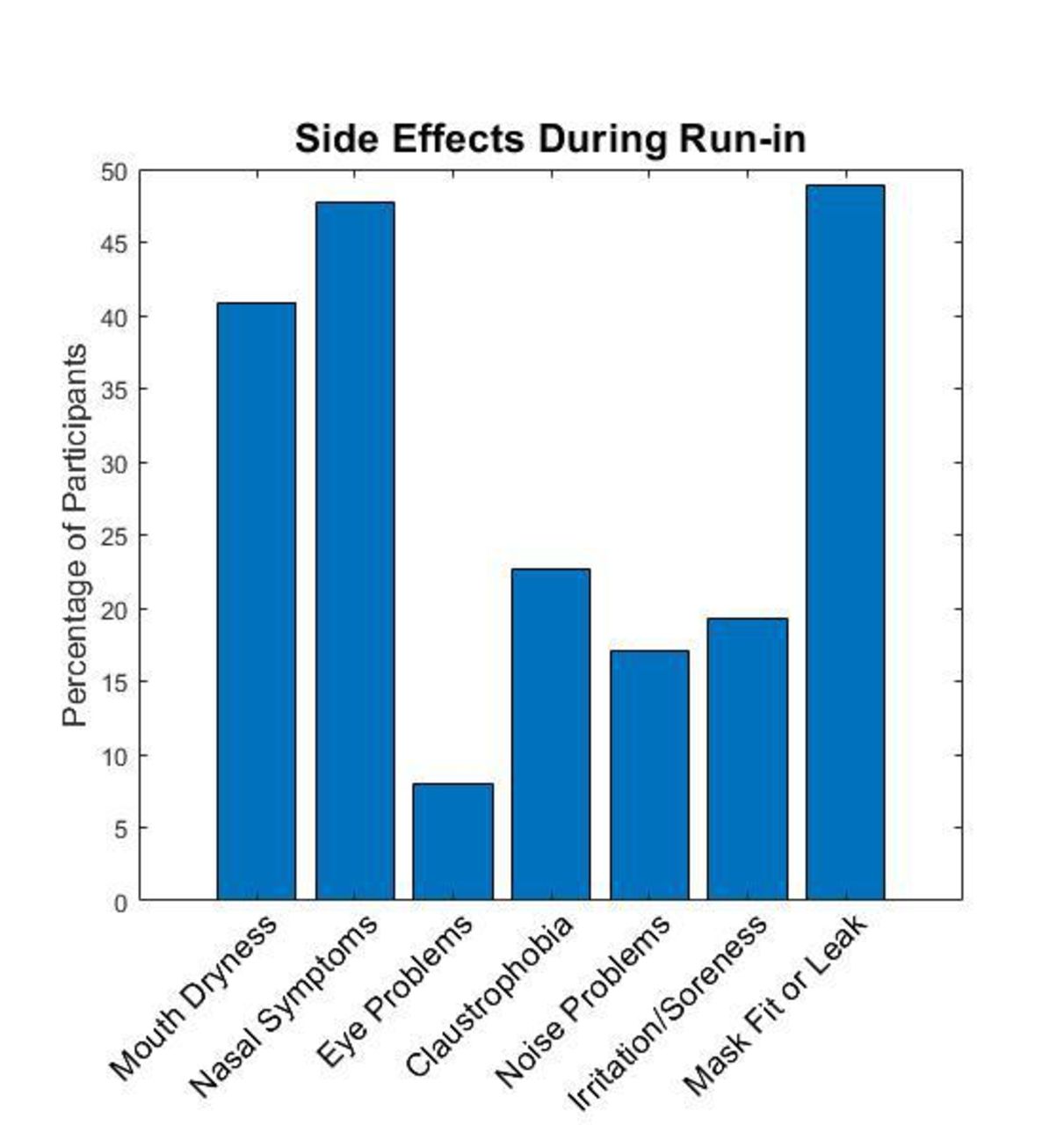
Get full access to this article
View all access options for this article.
