Abstract
Background:
Oxygen Saturation Index (OSI) has been shown to correlate with the Oxygen Index (OI) and is associated with increased mortality on the day of ARDS diagnosis1. OSI is calculated by (FIO2 X 100 X MAP) / SpO2. OSI is readily available data with no ABG required as is needed with OI. OSI can be calculated with every ventilator-patient assessment. There is limited information concerning the use of OSI outside of ARDS patients at the time of ARDS diagnosis. We wanted to determine if early changes in OSI on all adult ventilator patients would be associated with differences in patient outcomes.
Methods:
This study is a retrospective review of all mechanically ventilated patients in our adult ICUs since January 2014 who were ventilated in an ICU at least 48 hours. We collected the FIO2, mean airway pressure, SpO2 and location for each documented patient-ventilator assessment on day 1 and day 2 of ventilation. We excluded SpO2 values > 97% and FIO2 values of 100% because large changes in oxygenation only result in small changes of SpO2 in this range, similar to other OSI studies1. We calculated the maximum OSI on day 1 and day 2 of ventilation. We collected the outcomes (death, home discharge or other facility discharge) for all of the included patients. Patients were divided into two groups. Group 1: Maximum OSI decreased from day 1 to day 2. Group 2: Maximum OSI increased from day 1 to day 2. Minitab 18 was used for the data analysis.
Results:
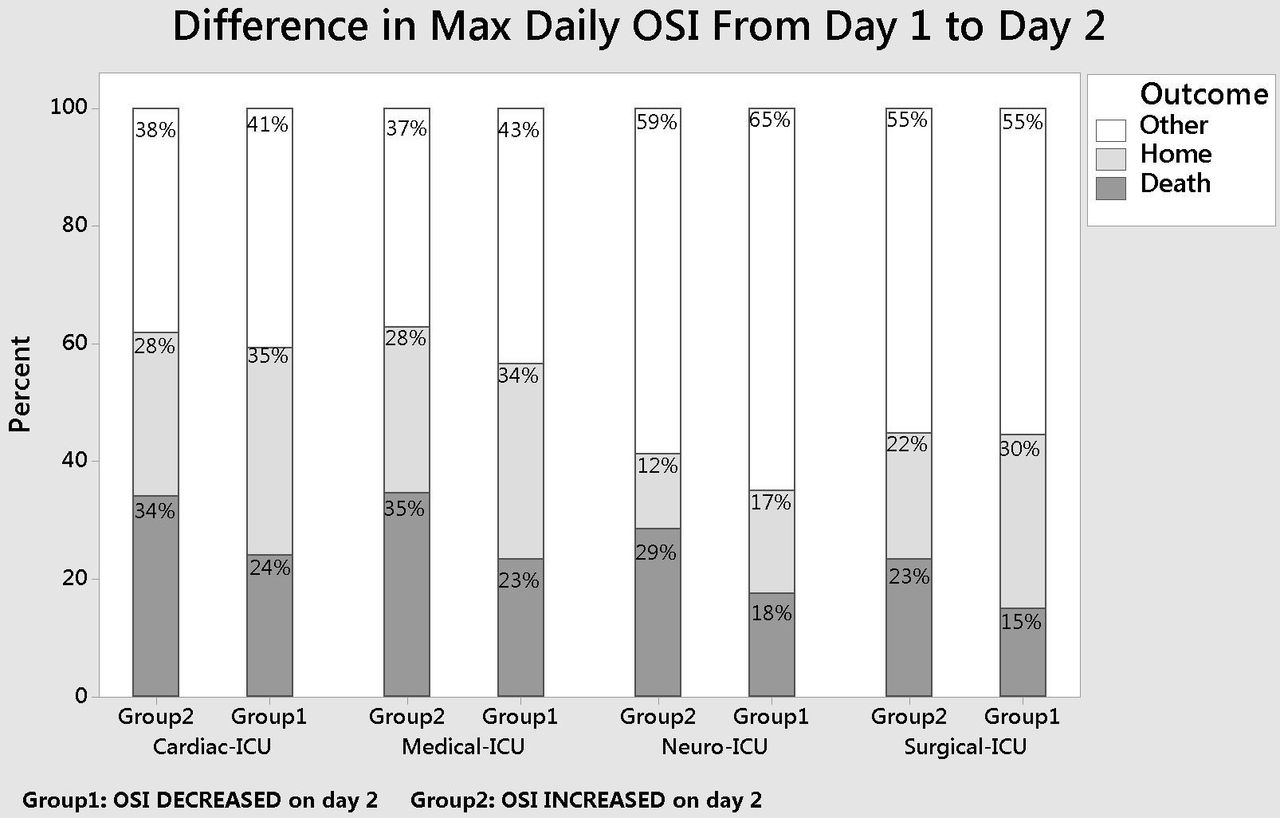
2,870 patients received ventilation > 48 h in an ICU since January 2014. Group 1 data: n=1,829, mortality=21.0%, home discharge=31.1%. Group 2 data: n=1,041, mortality=30.6%, home discharge=24.3%. Outcomes were significantly different between groups (P < .001). All ICU's had lower mortality and higher discharge home for Group 1 patients. See chart for unit specific outcomes.
Conclusions:
OSI can be calculated with readily available information at bedside. This study shows that the direction of change in the OSI between day one and day two of mechanical ventilation correlates to significant changes in mortality and home discharge of mechanically ventilated ICU patients. Awareness of the changes in OSI could help guide care towards more protective therapies if OSI is worsening. Future prospective studies could match patients by disease and severity to better understand the impact on those specific populations.
1. Chest 2017;152(6):1151-1158.
Get full access to this article
View all access options for this article.
