Abstract
Background:
In December of 2015, the University of Minnesota — M Health changed our out-of-hospital (OH) refractory VF/VT protocol. Along with specific inclusion criteria, the VF/VT protocol change utilizes local EMS for early transport to M Health's CCL. The protocol inclusion criteria are assessed before implementation of ECLS. Increased patient survival rates utilizing this protocol has significantly increased our number of annual ECLS patients and hours. We report the impact to respiratory therapy due to increased patient survival rates in the VF/VT population; including increased equipment, personal resources, and financial implications.
Methods:
This is a retrospective review of our ECLS patient data from 1/1/2014 — 5/15/2018, with the protocol data from 12/1/2015 — 5/15/2018. Data analyzed includes the total number of ECLS patients compared to the number of protocol patients, the rate of ECLS survival and survival to hospital discharge specific to the protocol; the annual growth due to the protocol; the annual increase in number of ES, RNs and MDs; and the financial impact to the RT department. Patients with an OH VF/VT arrest and arriving at M Health as part of the EMS early mobilization protocol were included in specific survival analysis and comparative analysis to overall ECLS patient and departmental data. Approval from the IRB has been obtained (STUDY00003576).
Results:
M Health has cared for an additional 106 ECLS patients as a result of the protocol change. 45% survived ECMO and 30% survived to hospital discharge. The RT department also adjusted their staffing model, implemented mandatory call, and increased annual ES requirements. The ES may be pulled from a prescheduled RT shift or pick up bedside hours for premium pay. Additional financial implications include increasing the ECLS equipment fleet available for use and the increased amount of disposable supplies used. ECLS operating expenses include salaries, benefits and supplies. The increase in bedside hours forced a staffing model change. Previously, all patients were staffed 1: 1 with an ES and RN. In 1/2016, stable adult patients were paired for the ES (1: 2) and remained 1: 1 nursing.
Conclusions:
A successful OH refractory VF/VT early mobilization protocol has increased annual ECLS volume. It has had a significant impact on the RT department requiring staffing model changes, increased training requirements and increased financial obligations.
ECLS HOURS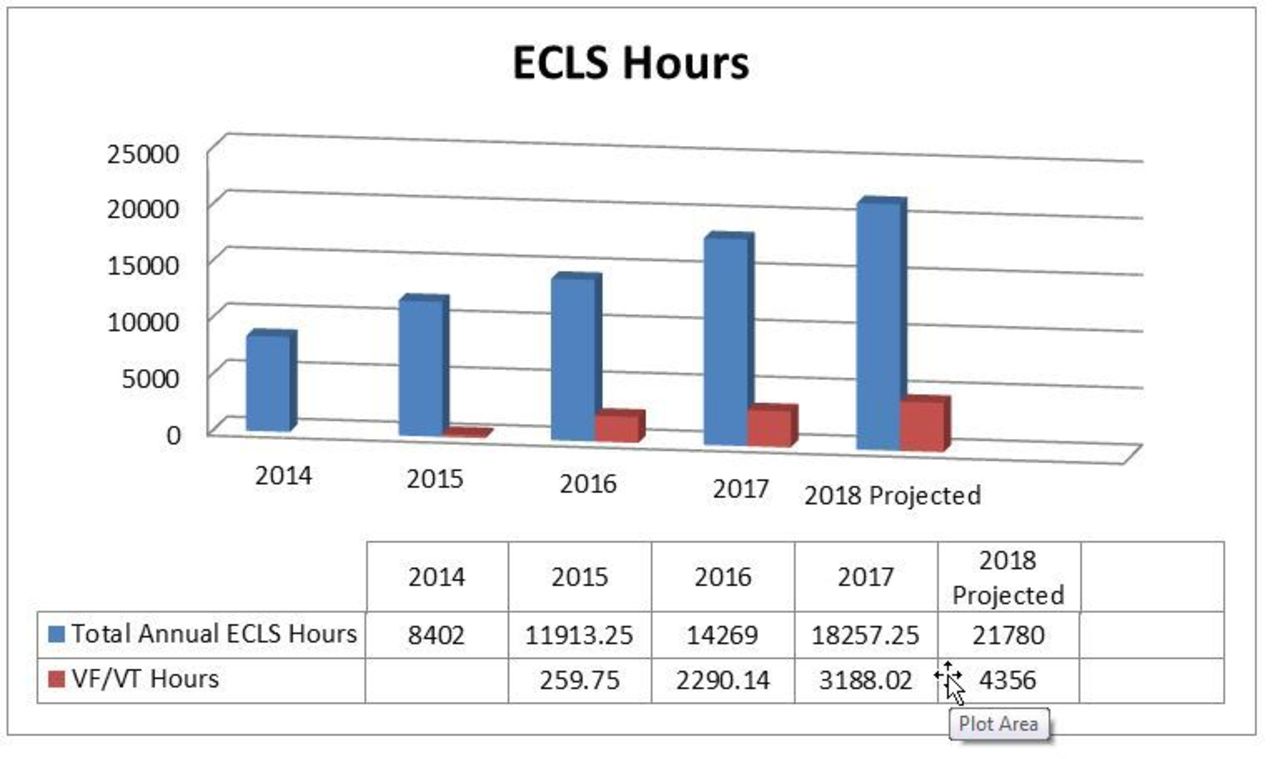
Get full access to this article
View all access options for this article.
