Abstract
Background:
As the landscape of healthcare reimbursement has changed, there is an increased emphasis on lowering costs and decreasing length of stay (LOS). As respiratory therapists (RTs), our value is increasingly measured not by daily procedures performed but by our overall impact on LOS and quality metrics. Literature supports the use of respiratory protocols to decrease LOS and improve patient outcomes with appropriate resource utilization by ensuring treatments have established indicators. A quality improvement project to increase respiratory therapy protocol (RTP) usage on patients receiving scheduled respiratory therapy should decrease LOS while better utilizing resources and lowering costs.
Methods:
Utilizing the electronic medical record's embedded RTP order set, subjects were assessed by respiratory staff and placed on an appropriate therapy regimen determined by the scoring tool and therapy algorithms. For the RTP, subjects who scored < 8 did not receive therapy and were placed on PRN therapy with daily assessments for 3 days. Subjects who scored 9 > received scheduled therapy based on therapy algorithm. To ensure RTP orders were placed on appropriate patients, a process was implemented to prompt providers to activate the RTP order set. Pre-intervention time was July 2016- April 2017 and Post-intervention period was July 2017- April 2018.
Results:
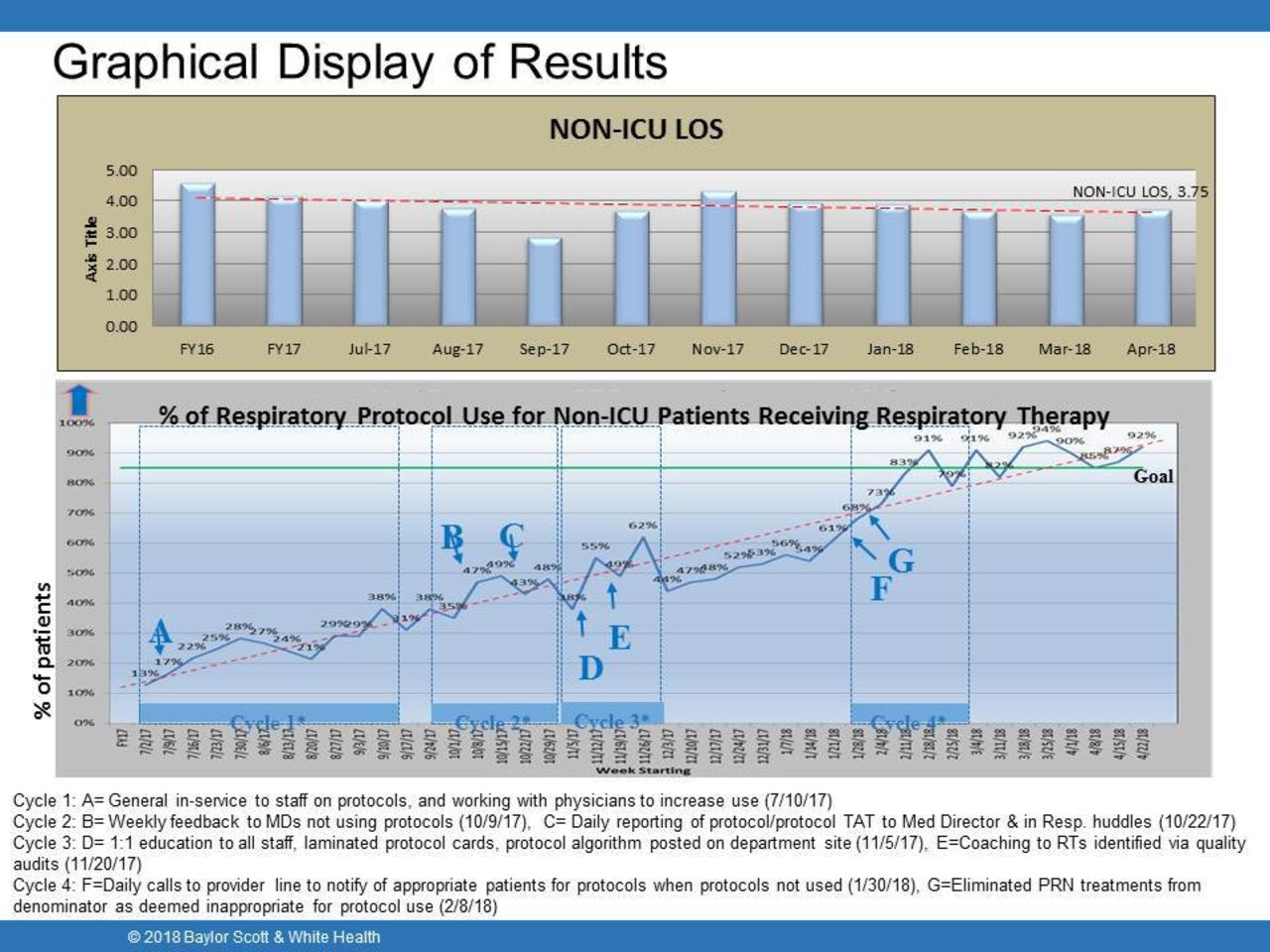
The LOS for our non-ICU COPD patients decreased from 4. 16 in our pre-intervention period (Jul 2016-Apr 2017) to a post-intervention (Jul 2017-Apr 2018) average of 3. 72 days, for a total reduction of 205 patient days and approximately $269, 166 in cost savings. This was based on 350 unique patient admissions for a total of 1305 patient days for COPD LOS. The number of therapies per net equivalent patient day decreased by 11519 for the 10 month post-intervention period and was based on ALL patients with RTP order and therapy modification. The reduction in therapy allowed the RT staff to conduct the increased number of RTP's without adding additional staff. It was also noted the number of missed treatments decreased by 73% from July 2017 to April 2018.
Conclusions:
Utilization of a RTP showed a trend of decreased patient LOS for our patients with a primary COPD admission diagnosis. The implementation of RTP's decreased the number of treatments per net equivalent patient day. By better targeting appropriate therapy, we achieved more efficient staff utilization, while reducing missed therapies.
Disclosures. None.
Get full access to this article
View all access options for this article.
