Abstract
Background:
Early mobilization (EM) has been shown to be important for patients receiving mechanical ventilation in critical care. However, there is a risk of ventilator-associated pneumonia (VAP) if EM is done without proper cuff pressure management. Additionally, the measured cuff pressure during position changes has not been well documented. During EM the sympathetic nerve can be activated more than the parasympathetic nerve, causing the smooth muscle in the trachea to relax, increasing the diameter of the trachea. Given these variables, it is difficult to understand cuff pressure management during EM to prevent VAP. The purpose of this study was to investigate the cuff pressure during position changes between supine and sitting during EM.
Methods:
This study was approved by the IRB at Yokosuka General Hospital UWAMACHI (YGHU). The data was gathered from February — May 2018, in the intensive care unit at YGHU. Fourteen subjects were evaluated while receiving mechanical ventilation via an oral endotracheal tube; there were a total of 21 EM sessions in the 14 individual subjects. During EM, patients were ventilated with a Drager Evita XL, in CPAP with PEEP < 10 cm H2O and pressure support < 10 cm H2O. Baseline vital signs and cuff pressure were gathered with the patient supine, with the head of bed at an angle of 0-30. Cuff pressure was measured by attaching a three-way stopcock and a manometer to the pilot balloon; the stop-cock was only opened during cuff pressure measurement. After establishing baseline pressures, the patient's position was changed and the patient was sat on the side of the bed; cuff pressure and vital signs were recorded immediately, and at three min and five min after the position change.
Results:
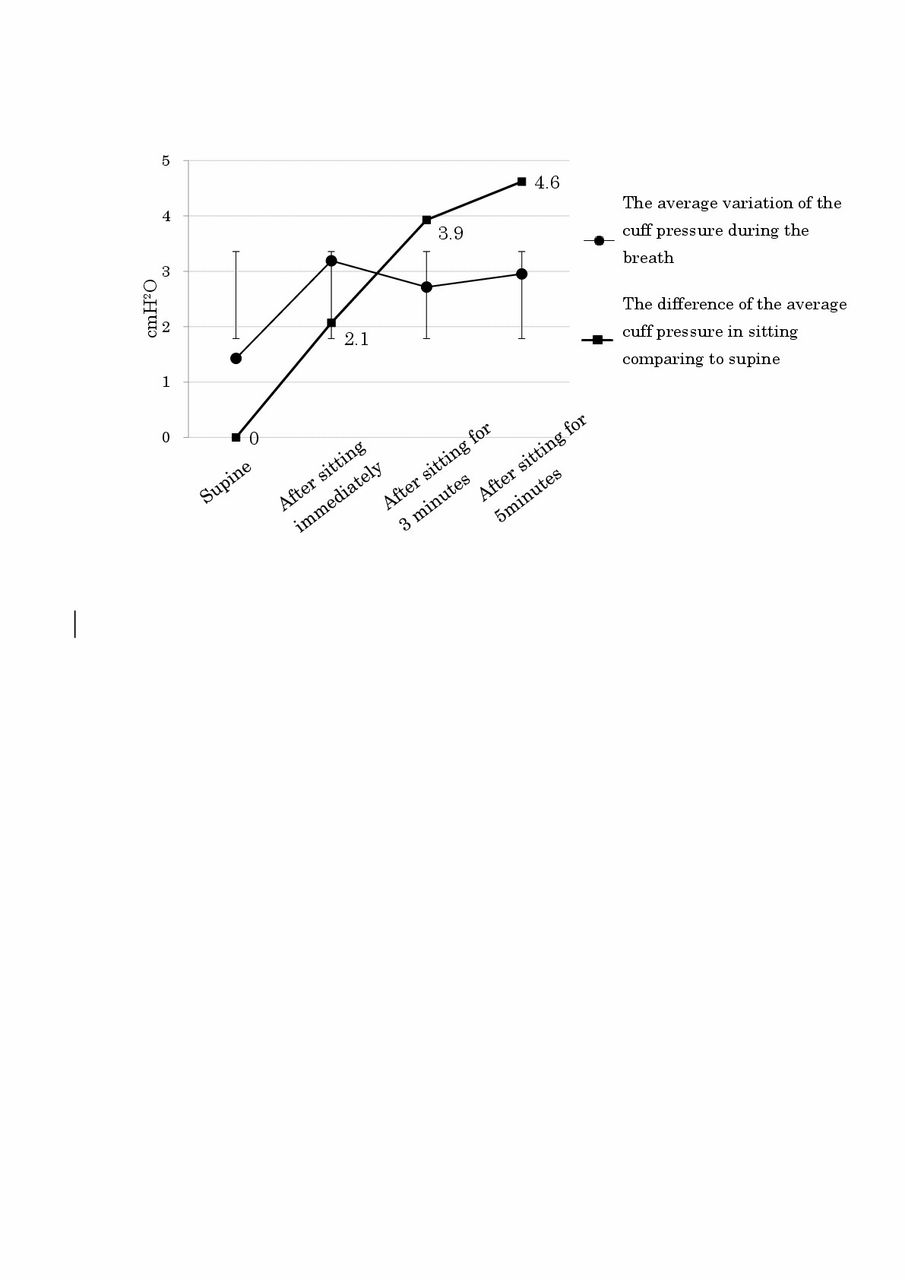
The cuff pressure had an average variation of 1-3 cm H2O between inspiration and expiration during EM. The cuff pressure decreased with sitting, and decreased with the amount of time that elapsed. There was a statistically significant change in the difference in cuff pressure between baseline and sitting at 3 min (P=0.009), and in baseline and sitting at five min (P=0.001).
Conclusions:
The findings suggest that the cuff pressure tends to decrease during mobilization from baseline to sitting, and time elapse during sitting. It is important for respiratory care practitioners to adjust the cuff pressure frequently during mobilization for safe early mobilization.
Disclosures:
None.
Get full access to this article
View all access options for this article.
