Abstract
Background:
Tracheostomies are routinely performed in children who require long-term mechanical ventilation. Language development and swallowing can be impaired when a tracheostomy tube (TT) is in place, especially in infants. Passy-Muir Valves (PMV) enable phonation and improved swallowing skills by redirecting expiratory flow through the vocal cords. When used during mechanical ventilation, expiratory flow is prohibited from returning to the ventilator and may affect accuracy of set parameters such as PEEP, which Passy-Muir recommends reducing or eliminating. The aim of this study was to compare set PEEP to delivered PEEP while using a PMV in-line with a Trilogy 202 ventilator and a passive circuit in a simulated infant model.
Methods:
To simulate an infant airway with a tracheostomy, a cuffed 3.0 TT Ped Bivona was inserted into an incision made in an 11.5 cm section of elastic tubing with an internal diameter of 6 mm. The distal end was attached to a ASL 5000 lung simulator to simulate a spontaneously breathing infant (∼ 5-6 kg of body weight) with age-appropriate parameters and moderately affected lungs. The proximal end was open to the atmosphere. A pressure line adapter and flow analyzer were placed between the TT hub and PMV. The Trilogy 202 ventilator was attached to the PMV via its proprietary passive circuit and was initially set in S/T mode with settings of: PS 8 cm H2O, PEEP 4 cm H2O, cycle off of 20%, rise time of 1 and flow trigger of 1 L/min. Prior to testing, VT and transtracheal pressures were assessed pre/post PMV placement to confirm adequate flow around the TT. PS was increased to 10 cm H2O and simulations were run and recorded at PEEP settings from 4 to 10 cm H2O in 1 cm H2O increments for 2 min each. The first 30 seconds was discarded and the subsequent minute was used for post-run analysis of delivered PEEP. Descriptive Statistics and Mann-Whitney rank sum tests were used for statistical analysis.
Results:
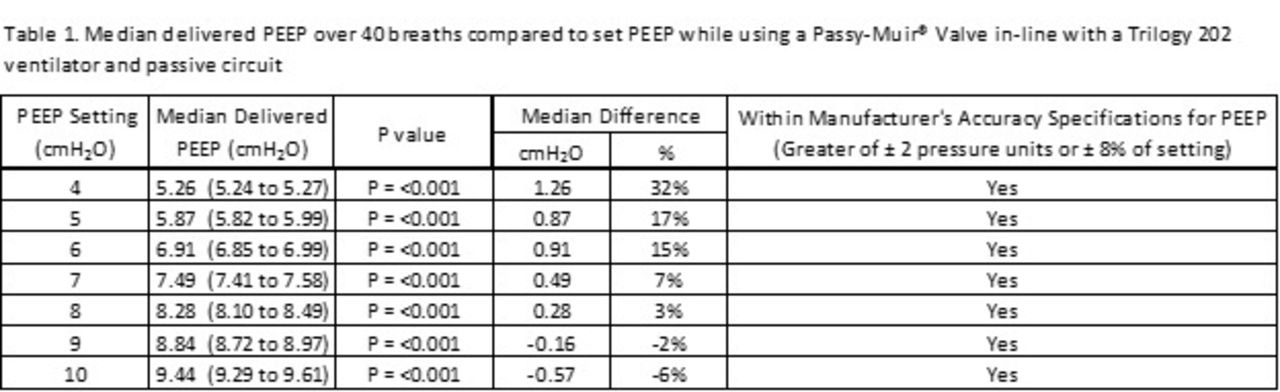
Data are shown below. There was a significant difference (P<0.001) between set PEEP and the median delivered PEEP at all settings. But, delivered PEEP was within manufacturer's specifications (Greater of ± 2 pressure units or ± 8% of setting).
Conclusions:
In this simulated infant model, the Trilogy 202 sub-acute care ventilator with passive circuit was able to deliver set PEEP within manufacturer's specifications while using a Passy-Muir Valve in-line.
Get full access to this article
View all access options for this article.
