Abstract
Background:
The modified early warning score (MEWS) detects early clinical deterioration in patients to prevent catastrophic events. Respiratory therapists usually do not use the MEWS even though it is implemented as a default in the electronic health record (EHR) system. To optimize patient care, clinicians could use special guidelines and protocols that incorporate the MEWS. Objective: To identify the major determinants of respiratory therapists' intention to use the modified early warning score (MEWS).
Methods:
A web-based self-administered survey based on the constructs of the Technology Acceptance Model (TAM) as well as awareness, attitude, and job-relevance was developed and validated using traditional scale development process. The survey was then distributed to 75 respiratory therapists (RTs) from the respiratory care department of Rush University Medical Center who were recruited using consecutive sampling. The RTs were then given a training session on the MEWS after which they were again asked to complete the survey. The study was approved by our institutional review board.
Results:
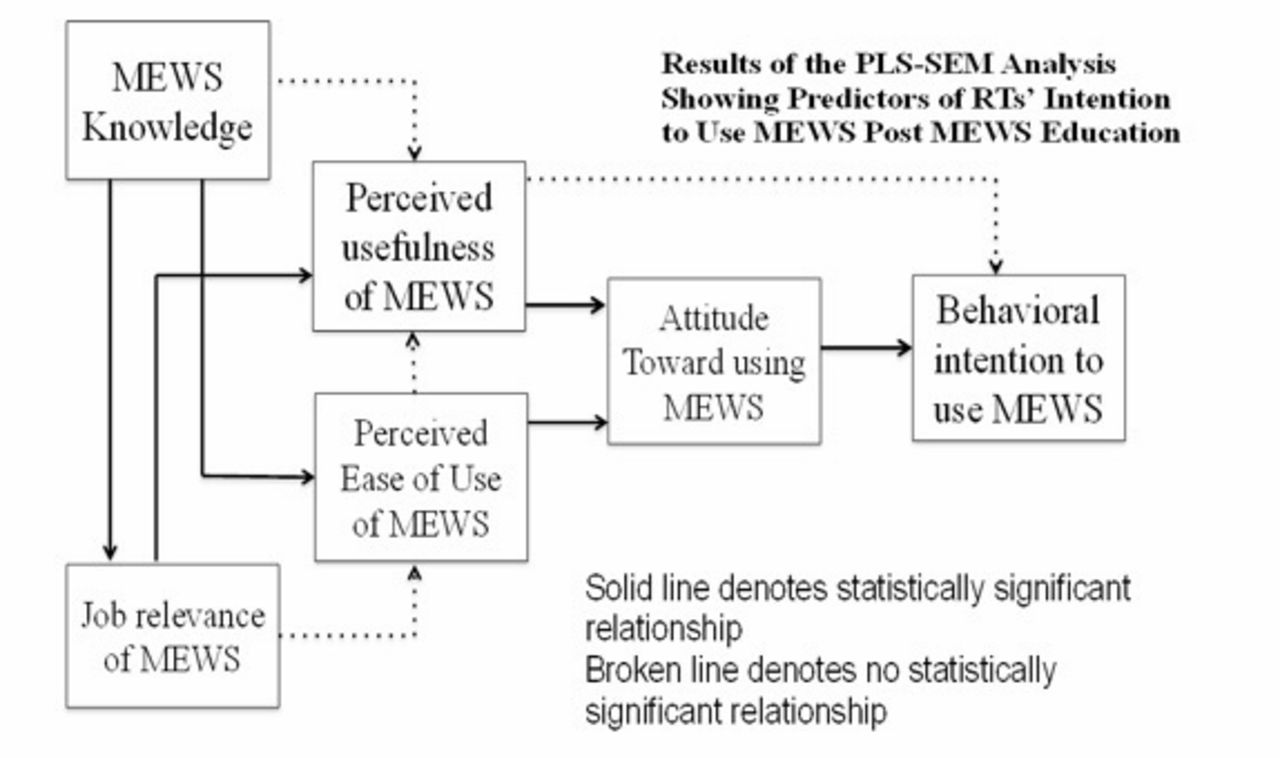
The response rate to both the pre and post survey was 60 percent. Of the 46 participants recruited to the study, the educational intervention elicited an increase in the MEWS knowledge score in 45 participants compared to the knowledge score prior to the educational intervention. Additionally, there was an increase in the behavioral intention score post intervention in 30 participants compared to the behavioral intention score prior to the educational intervention. There was also a statistically significant median increase in MEWS knowledge score (2.0) post educational intervention (4.0) compared to pre educational intervention (2.0), p < .0001. Regarding median behavioral intention scores, there was a statistically significant increase (1.0) post educational intervention (4.0) compared to pre educational intervention (3.0), p < .0001. Partial least squares structural equation modeling (PLS-SEM) revealed that MEWS knowledge influences attitude, which influences behavioral intention.
Conclusions:
Numerous studies have demonstrated that change in behavioral intention is a good predictor of change in behavior. Consequently, the increase in the respiratory therapists' behavioral intention score post MEWS education suggests that they may be more inclined to incorporate the MEWS score in their assessment of patients if they are educated about its clinical relevance.
Get full access to this article
View all access options for this article.
