Abstract
Background:
Exacerbations of bronchiectasis are associated with increased airways and systemic inflammation and progressive lung damage therefor in time proper antibiotics during exacerbation are very important.
Objective:
Find the association of pathogen in bronchiectasis patient between clinically stable and during exacerbation for answering the question whether using the previous clinically stable sputum culture results are able to predict the exacerbation pathogen or not. Study design: Retrospective cohort study.
Methods:
Reviewing good quality and significant sputum culture results in clinically stable and during exacerbation in 98 non-cystic fibrosis bronchiectasis patients who were not exposed to inhaled or oral antibiotic for 3 months before collecting the sputum.
Results:
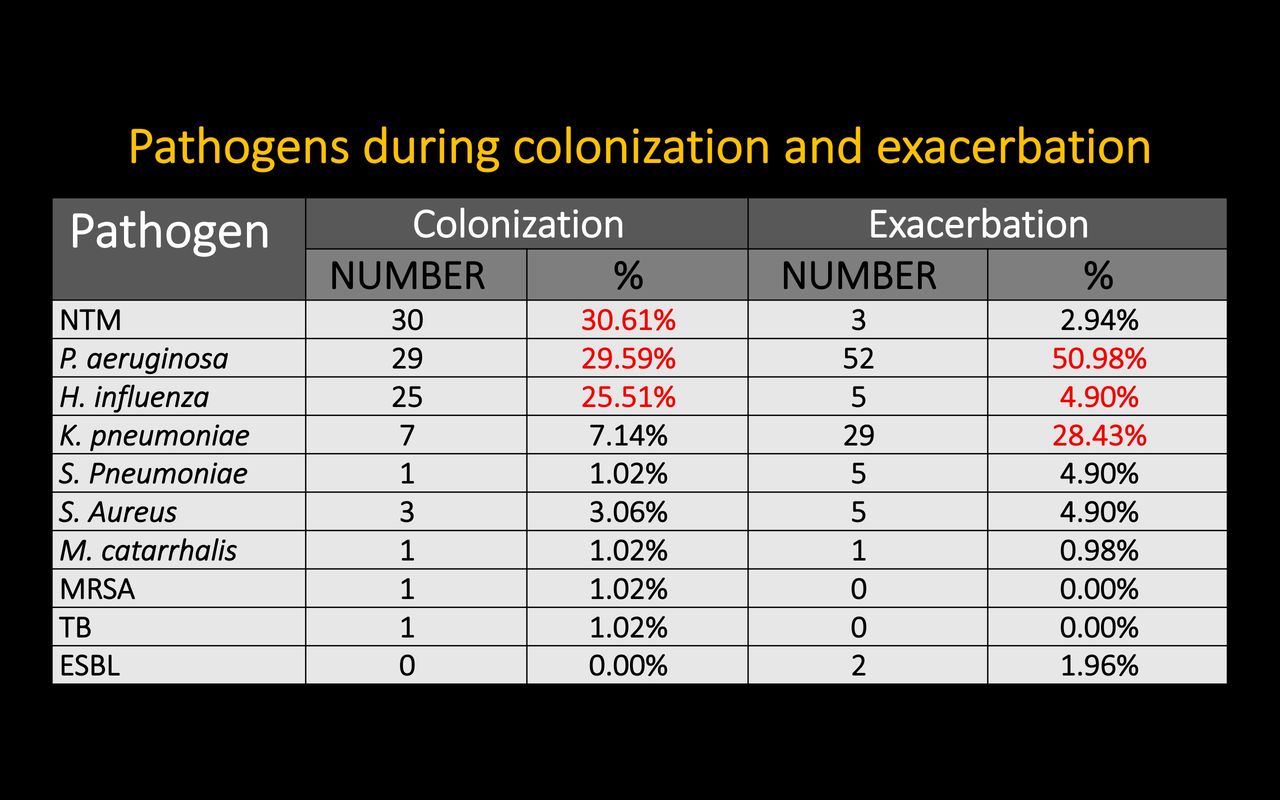
Most of bronchiectasis patient in this study were diffused lesion (68.6%). Previous tuberculosis infection (50.3%), idiopathic (24%) and rheumatoid arthritis (5. 1%) were the three most common causes of bronchiectasis. First three commonly pathogen being found in clinically stable sputum results were non-mycobacterium tuberculosis (30.61%), Pseudomonas aeruginosa (29.59%), Hemophilius influenza (25.51%) and during exacerbation were P. aeruginosa (50.98%), Klebsella pneumonia (28. 43%), H. influenza (4.9%). Agreement for detection of bacteria by culture during clinically stable or exacerbation was good for P. aeruginosa (84.8%) but poorer for other genera. (sensitivity 75% specificity 75.6% PPV 54.5% NPV 88.6%).
Conclusions:
Collecting sputum when clinically stable may helpful for sputum guidance for exacerbation if the colonized sputum pathogens were P. aeruginosa.
Disclosures:
None.
Get full access to this article
View all access options for this article.
