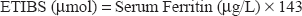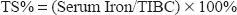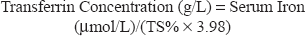Abstract
Much research has shown that iron store parameters are increased in women with polycystic ovary syndrome (PCOS), but an exact explanation for this phenomenon remains unavailable. The objective of this study was to investigate the correlation between iron status parameters and hormonal disturbances in women with PCOS that accounts for their increased iron store levels. Iron status parameters and hormones were measured using colorimetric and enzyme-linked immunosorbent assays, respectively. The results demonstrated a mild iron overload in the patients with PCOS. Good positive correlations between iron status parameters and serum testosterone, prolactin, and insulin were detected in the patient group, whereas iron status parameters and BMI were not significantly correlated. The data also suggest that the increase in serum ferritin and body iron store levels in patients with PCOS are associated with hyperandrogenemia, hyperprolactinemia, and hyperinsulinemia. The findings of this study expand current knowledge on the factors affecting iron stores and suggest a different mechanism of interaction between iron stores and the endocrine system through the harmful deposition of iron in endocrine glands and through hormonal effects on iron absorption and metabolism.
Introduction
Polycystic ovary syndrome (PCOS) is one of the most common disorders in premenopausal women, and it affects 4%–10% of all women.1,2 PCOS is a comprehensive syndrome associated with different metabolic disorders, including obesity, insulin resistance, and dyslipidemia, vascular abnormalities, and carbohydrate metabolism disturbances, including impaired glucose tolerance.3,4 Research has shown that serum and body iron contents are elevated in patients with PCOS5,6 and are probable causes of coronary heart disease (CHD) due to the deposition of iron in the cardiac tissues. Different explanations for the increased iron store levels in women with PCOS have been reported.5–7 Some studies were based on the hypothesis of reduced blood loss due to period irregularity, whereas others assigned hyperinsulinemia as the main cause of iron accumulation in this patient population. Despite these efforts, the correlation between hormone levels and high iron store levels in patients with PCOS remains largely unexplored. Iron overload associated with different disorders has been reported to affect the function of different endocrine glands. 8 On the other hand, the hormonal profiles of patients with PCOS have shown variance and the severity of hormonal disturbances has differed from one research to another. 9
One aim of the present work was to investigate the correlation between hormonal profile and iron status parameters in patients with PCOS that may likely trigger (by precipitation of the iron in certain tissues and subsequent damage to those tissues) the associated features of PCOS, including heart diseases. Another objective of this study was to determine the most effective hormones on iron stores in women with PCOS.
Materials and Methods
Patients
The purpose of the protocol was explained carefully to all the patients and control subjects, and their consent was obtained before the study began. In the initial agreement, the results were given to the participants to allow them to consult their physicians and use the data as reference. One hundred fifty-eight women with PCOS (age, 28.5 ± 6.5 years) were recruited from private gynecological clinics in Najaf, Iraq. PCOS was defined according to the 2003 Rotterdam Revised Consensus Meeting. Oligomenorrhea, clinical or biochemical hyperandrogenemia, and the presence of polycystic ovaries have been previously proposed as the diagnostic criteria for PCOS. 10 Each recruited participant needed to have at least two symptoms of the disease to be considered as having PCOS. Ethical approval was obtained for the use of humans in this research
Sixty age- and weight-matched healthy control subjects with a normal menstrual cycle were also selected for inclusion in this study. Ultrasonography confirmed that these women did not have clinical features of hyperandrogenism or PCOS. Five milliliters of blood samples was drawn from the control subjects in the morning after an overnight fast on the second day of their menses. Spontaneous menstrual bleeding was awaited, and progesterone treatment was not used to induce menstruation. Hemoglobin concentrations and packed cell volumes were directly measured from heparinized capillaries tubes, and the sera were separated, after clotting, and then stored at −20 °C until analysis.
Subjects were excluded from this study if they had a history of diabetes mellitus, hematocrit levels greater than 48%, severe sleep apnea, and congestive heart failure; used androgens; and participated in moderate to intense exercise training. C-reactive protein levels were semiquantitatively estimated in the participants to exclude those with chronic inflammation, which affects serum ferritin levels, and, ultimately, to assess the potential confounding effect of chronic inflammation on ferritin levels; 5 patients with positive C-reactive protein levels (>6 mg/L) were excluded. The human chorionic gonadotropin test was used to rule out pregnancy.
Measurements
Serum levels of iron were estimated using the colorimetric method, whereas total iron binding capacity (TIBC) was estimated colorimetrically according to the following procedure: An excess of iron was added to the serum iron to saturate the transferrin. The unbound iron was precipitated with basic magnesium carbonate. After centrifugation, the iron in the supernatant was determined. Unsaturated iron binding capacity (UIBC), the amount of protein (apo-transferrin) still available to bind iron, was estimated using the formula, UIBC = TIBC – Serum Iron.
The ferritin quantitative test is based on solid-phase enzyme-linked immunosorbent assay (ELISA). The assay system utilizes a rabbit anti-ferritin antibody for solid-phase (microtiter wells) immobilization and a mouse monoclonal anti-ferritin antibody in the antibody–enzyme (horseradish peroxidase) conjugate solution. Estimated total iron body stores (ETIBS) were calculated using the following formula:11,12
Transferrin saturation percentage (TS%) was obtained as follows: 13
Transferrin concentration was calculated using the following formula: 14
The latter formula is based on the maximal binding of 2 mol Fe3+/mol transferrin and a molecular weight of 79,570 g/mol for transferrin.
Luteinizing hormone (LH), follicle-stimulating hormone (FSH), thyroid-stimulating hormone (TSH), prolactin (PRL), total testosterone (TT), estradiol (E2), and progesterone (PRG) were estimated in the luteal phase of the menstrual cycle by ELISA using ready-to-use kits supplied by Monobind® Company (USA). Basal serum cortisol levels were obtained to exclude adrenal disorders, and fasting serum insulin levels were measured using the DRG® Insulin ELISA Kit (Germany), which represents a solid-phase assay based on the sandwich principle.
Biostatistical analysis
Statistical analysis was performed using SPSS 19.0.1 (2010; IBM, USA) and the Regression Analysis and Forecasting model (Business Spreadsheets, USA). The one-sample Kolmogorov-Smirnov test was used to examine the normality of the variable results. The results were expressed as mean ± standard deviation for normally distributed data and as median values for nonparametric variables. A pooled t test was used for comparisons of the measured parameters with normal distribution between the patients and control subjects. Comparisons between pairs of variables without homogenous distribution were determined using the Mann–Whitney U test. Spearman's coefficient (Spearman's ρ, r) was used to identify any correlation between the parameters, and the significance of the correlation was set at ρ ≥ 0.5. Both ρ < 0.05 and P < 0.05 were considered statistically significant. Multivariate regression analysis was used to characterize the influence of the most effective hormones (insulin, PRL, and testosterone) on the level of ferritin, which is the most important serum predictor of iron stores. Correlation coefficients were calculated for the control and patient groups to study the possible relationship between BMI and iron status parameters (results not shown).
Results
The BMI values of the patients with PCOS and control subjects were 33.6 ± 5.8 and 32.4 ± 3.6 kg/m2, respectively. The iron indices are listed in Table 1. Hemoglobin concentrations and PCV percentages did not significantly differ between groups. In contrast, a significant difference (P < 0.05) was observed between the iron indices of the patients with PCOS and those of the control subjects. All parameters, except TIBC, transferrin concentration, and UIBC, which decreased, were increased in the patients with PCOS compared with their healthy counterparts. Table 2 shows the hormonal profiles of the study participants. LH concentration and LH/FSH ratio significantly increased, and the patients with PCOS had hyperinsulinemia, hyperandrogenemia, and hyperprolactinemia. Table 3 highlights the positive correlation detected between iron status parameters and serum testosterone, PRL, and insulin in the patient group.
Iron parameters.

P < 0.05, two-sided pooled t test.
Hormonal profiles.

P < 0.05, Mann-Whitney U test.
Correlation coefficients for iron status parameters and hormones.

P < 0.05;
P < 0.01;
P < 0.001.
Multiple regression analysis produced the following equation:
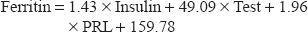
The measured serum ferritin level (actual) plotted against the serum ferritin level obtained from the equation (predicted) in Figure 1 revealed a slight correlation between the actual ferritin level and the ferritin level calculated from the regression equation (Y = 0.144X + 226.9, R 2 = 0.144); ie, 14.4% of the change in ferritin can be explained by the change in the three independent variables with a standard error of ±67.27 pmol/L for the results of the regression equation. Therefore, the multivariate analysis yielded significant results (F = 8.789, P < 0.05). Overall, the data did not reveal any significant correlation between iron status parameters and BMI in either group.

Correlation between the predicted and actual ferritin levels based on the regression equation.
Discussion
Increases in iron indices, especially ferritin and ETIBS, indicate a high availability of iron in different tissues of patients with PCOS (Table 1).5,6 Increases in iron store and ferritin levels in PCOS may be attributed to the absence of regular menstrual blood loss, leading to iron overload, as serum ferritin levels have been observed to be higher in oligo-amenorrheic patients compared with regularly menstruating women. 5 Oxidative stress induces ferritin synthesis to reduce further oxidative damage, given that ferritin neutralizes highly toxic unbound iron; 15 research has also shown that oxidative stress may be increased in women with PCOS. 16 Hyperinsulinemia may also account for this phenomenon. Insulin resistance, which is prevalent in patients with PCOS, may likewise contribute to increased serum ferritin and body iron stores, because insulin may stimulate intestinal iron absorption6,17,18 by up-regulating the activity of hypoxia-inducible factor-1α and down-regulating hepcidin expression. 19
Moreover, hyperandrogenemia, which affects erythropoiesis, is widely known as a critical component of PCOS. Serum ferritin concentrations are increased in patients with PCOS independent of obesity. One study found that androgen excess, insulin resistance, and abnormal glucose tolerance are correlated with ferritin levels in premenopausal women. 20 Treatment with metformin, which ameliorates insulin resistance and hyperinsulinemia, reduces serum ferritin and iron store levels in patients with PCOS. 5 Increased iron stores are believed to contribute to insulin resistance and hyperinsulinemia by iron deposition in β cells and through the reduction of hepatic insulin extraction and metabolism. 21 This indicates that iron precipitating in any tissue does not become extracted and circulated easily. Although iron does accumulate in certain tissues, the levels of circulating iron are low and do not reflect hemochromatosis or hemosiderosis, except the case for ferritin, which is a precursor for ETIBS. 12 The fact that obesity and high dietary intake may facilitate the absorption and deposition of iron in tissues, a mechanism possibly amplified by the reduced menstrual loss of patients with PCOS, may also help explain this finding. 15
Table 2 reveals a disturbance in the hormonal profile of the patients with PCOS compared with that of the control group. This result supports the hypothesis that patients with PCOS often have altered hypothalamo pituitary functions, including increased baseline LH concentrations and elevated LH/FSH ratios, as previously reported. 22 In addition, the increased TT concentration (Table 2) in the patient group is congruent with previous research 23 reporting that obesity plays a crucial role in the pathophysiology of hyperandrogenism and metabolic abnormalities in PCOS, because human adipose tissue is capable of active androgen synthesis and increased expression in obesity may contribute to circulating androgen excess in patients with PCOS. 24
Serum TT, PRL, and insulin showed the most significant correlation with most of the iron status parameters, as shown in Table 3, revealing a positive association between increased iron overload parameters and hyperandrogenemia, hyperprolactinemia, and hyperinsulinemia. The effect of hyperandrogenemia on estimated body iron store levels may be caused not only by the well-known stimulatory effect of androgens on erythropoiesis, thereby increasing intestinal iron absorption, 25 but also by decreased menstrual loss due to the chronic menstrual dysfunction in PCOS. IR in patients with PCOS could increase erythropoiesis, which enhances the body's iron requirement. Escobar-Morreale and Luque-Ramírez (2011) recently showed that the increased serum ferritin levels detected in patients with PCOS are associated with a reduction in insulin sensitivity but that it does not result from an enhancement of erythropoiesis by testosterone excess. 26 Research data strongly suggest that hyperinsulinemia is the underlying origin of increased body iron stores.6,17
Furthermore, elevated iron stores have been reported to be positively associated with the prevalence of metabolic syndrome and insulin resistance. 27 The pathogenic link between metabolic syndrome and PCOS is most likely insulin resistance, which occurs in both obese and nonobese women. 28 The increase in iron status parameters may thus be due to the presence of insulin resistance. Moreover, the increase in iron stores might contribute to the insulin resistance 29 and β-cell dysfunction frequently found in patients with PCOS as a result of the harmful effect of iron deposition in β cells, 30 which is substantiated by the fact that a reduction in ETIBS by blood donation improves insulin sensitivity. 31
Testosterone also plays an erythropoietic role,17,32 and it has been found to decrease ventilation. 33 Estradiol has the opposite actions. 34 Some authors concluded that low testosterone levels may be a predictive marker for men at high risk for cardiovascular disease, 35 whereas another study suggested that increasing testosterone levels might improve the symptoms of coronary artery disease. 36 These findings remain controversial. First, patients with PCOS are at high risk of acquiring CHD due to their increased body iron stores and the subsequent precipitation of iron in their cardiac tissues, in addition to the symptoms of metabolic syndrome that are generally present, such as hyperinsulinemia. Second, high testosterone levels (frequently associated with PCOS) in men are healthy and consequently reduce their risk for CHD. This latter phenomenon needs to be further explored in women with PCOS, particularly to study the possible effects of hyperandrogenemia on their heart health.
The present study did not find any significant correlation between the iron status parameters and BMI in the patient and control groups that would have explained the role of obesity in different iron status parameters. This result was expected because adipose tissues have a mild effect on iron stores, which are located mainly in the liver, bone marrow, and spleen. The regression equation that links the most powerful factors related to ferritin levels showed that only 14.4% of the change in ferritin can be explained by the change in the independent variables (insulin, PRL, and testosterone), with the standard error being ±67.27 pmol/L. This indicates that the limiting effect of these parameters on iron stores in patients with PCOS and even the correlation coefficients between ferritin levels and these parameters are significant. Other possible factors may affect the mild iron overload observed in PCOS, but hormones have certain effects that exacerbate the increased iron store levels in this disease.
Conclusions
The results of this study suggest that increases in serum ferritin and body iron store levels in patients with PCOS are associated with hyperandrogenemia, hyperprolactinemia, and hyperinsulinemia. The data expand current knowledge on the factors affecting iron stores and suggest a different mechanism of interaction between iron stores and the endocrine system through the harmful deposition of iron in endocrine glands and via hormonal effects on iron absorption and metabolism. These findings clearly merit further investigation.
Disclosures
Author(s) have provided signed confirmations to the publisher of their compliance with all applicable legal and ethical obligations in respect to declaration of conflicts of interest, funding, authorship and contributorship, and compliance with ethical requirements in respect to treatment of human and animal test subjects. If this article contains identifiable human subject(s) author(s) were required to supply signed patient consent prior to publication. Author(s) have confirmed that the published article is unique and not under consideration nor published by any other publication and that they have consent to reproduce any copyrighted material. The peer reviewers declared no conflicts of interest.
Footnotes
Acknowledgments
Dr. Sana Muhsin and Miss Mahaa Abd Kadhem are gratefully acknowledged for their kind help in sample collection and diagnosis.