Abstract
Background
Ureteral catheters are valuable indispensable devices may readily acquire biofilms on the inner or outer surfaces. This study evaluated the efficacies of ureteral catheters impregnated with ciprofloxacin, N-acetylcysteine each alone and in combination on microbial adherence.
Methods
Antimicrobial durability of ureteral catheters coated, through instant dip method, with ciprofloxacin were determined using modified Kirby-Bauer method. Ciprofloxacin-coated catheters showed zones of inhibition ranged from 15 to 45 mm in diameter (baseline) against nine clinical strains recently isolated from patients undergoing ureteral stent removal. Segments coated with ciprofloxacin, N-acetylcysteine each alone and in combination, through instant dip method, were incubated with the tested microorganisms, washed, sonicated, cultured and the number of viable cells were determined.
Results
Ciprofloxacin-coated catheters soaked in urine and incubated at 37 °C, maintained antimicrobial activities and produce zones of inhibition that measured 2–10 mm for at least 8 weeks. Effect of ciprofloxacin and N-acetylcysteine coated catheters on microbial adherence were found to be dose dependent. Catheters impregnated with ciprofloxacin/N-acetylcysteine showed the highest inhibitory effect on microbial adherence when compared with controls (85.5%–100%).
Conclusion
Catheters impregnated with ciprofloxacin, using instant dip method, were shown to have broad spectrum, prolonged antimicrobial durability and high efficacy. On the other hand, Catheters impregnated with ciprofloxacin/NAC showed the highest inhibitory effect on microbial adherence to stent surfaces.
Introduction
Ureteral catheters are indispensable devices used in the management of ureteral obstruction.
1
Although the stent is valuable, it also has complications, which are stent encrustation, stone formation and biofilm formation. Urinary catheters are tubular latex or silicone devices, which when inserted may readily acquire biofilms on their inner or outer surfaces. It is found that 10% to 50% of patients undergoing short-term urinary catheterization (7 days) and virtually all patients undergoing long-term catheterization (>28 days) become infected.
2
The surfaces of these devices, external or intraluminal, act as substrates for microbial adherence. After initial layers of microorganisms adhere to the surface, they begin to form a biofilm. Biofilm-forming cells adhere to each other and become a viable cluster by embedding themselves in a polysaccharide matrix which protects them from host defense mechanisms and antimicrobial therapy.
3
Biofilm infections result in a complication in the course of treatment, increasing the length of patients stay in hospital and overall cost. Microorganisms commonly contaminate these devices and develop biofilms are
In order to prevent colonization of urinary catheters with microorganisms, we tested the efficacy and the antimicrobial durability of ciprofloxacin-coated catheters against the tested microorganisms and the effect of catheters impregnated with ciprofloxacin, N-acetylcysteine each alone and in combination on microbial adherence.
Materials and Methods
Strains
Nine clinical strains, recently isolated from urine samples and stent segments collected from patients undergoing ureteral stent removal at the department of urology, Assuit university hospital and showed susceptibility to ciprofloxacin, were used in the present work. Strains were
Drugs
Preparation of stock solutions of ciprofloxacin (Bayer, Milan, Italy) was performed according to manufacturer's instructions. Three concentrations (2, 4 and 8 mg/ml) of NAC (Sedico, Egypt) were evaluated.
Antimicrobial Efficacy and Durability Testing
Preparation of pieces
One centimeter segments of sterile double J ureteral stents (polyurethane) were dipped into ciprofloxacin solution (2 mg/ml), so that both the internal and external surfaces were coated. The pieces were left to dry overnight, at room temperature, on a sterile surface. The pieces were then washed using distilled water to remove any possible loosely attached antibiotic off the surface of the coated segments. The pieces were then left to dry for 4 h under a fume hood at room temperature.
Baseline zones of inhibition
Using a modified Kirby-Bauer method, baseline antimicrobial activity was assessed by measuring the zones of inhibition created by duplicates of impregnated segments that were vertically embedded in Muller-Hinton agar plates seeded with the following microorganisms:
Antimicrobial durability
The antimicrobial efficacy of ciprofloxacin-coated urinary catheter segments was assessed over time. The segments were placed in sterile 50 ml polystyrene tubes (Falcon), containing 10 ml urine and were incubated at 37 °C. A 10 ml volume was used to ensure the complete immersion of all of the pieces contained in the tube. Segments were tested in duplicate at weekly intervals, as the soaking fluids were replaced with fresh fluids. Zones of inhibition were determined using the modified Kirby-Bauer method against the same microorganisms as mentioned before. 5
The Effect of Ureteral Catheters Impregnated with Different Concentrations of Ciprofloxacin, N-acetylcysteine Each Alone and in Combination on the Bacterial Adherence
The effect of impregnated catheters were tested against
Statistical Analysis
One-Way ANOVA was employed to evaluate any significant difference between values obtained without the drug (controls) and those observed in the presence of different drug concentrations. Differences were done using SPSS, 11 statistical software (SPSS Inc., Chicago, IL).
Results
Baseline zones of inhibition and durability of coated urinary catheters in urine
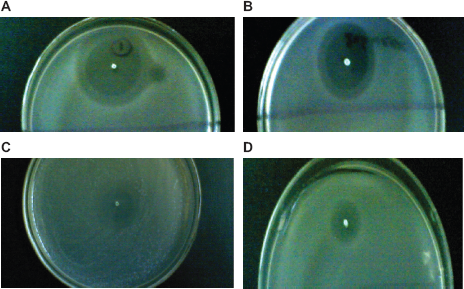
Table 1 and Figures 1, 2 show the results of baseline tests for ciprofloxacin-coated segments and their efficacies against the tested microorganisms after being soaked in urine for 8 weeks. The numbers represent measurement of the diameter of zones of inhibition, in millimeters, not including the diameter of pieces embedded in the agar (2 mm). Zones of inhibition produced by ciprofloxacin-coated segments measured 15–45 mm at baseline. After being immersed in urine (changed at weekly intervals), ciprofloxacin-coated catheters still produced zones of inhibition for 5–8 weeks. Zones of inhibition for
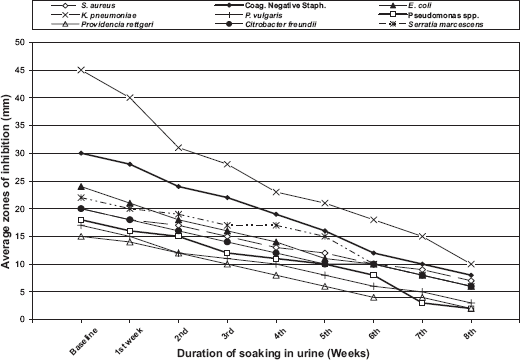
Baseline antimicrobial activity and efficacy of ciprofloxacin coated urinary catheters, soaked in urine that was changed weekly.
Antimicrobial activity and durability of ciprofloxacin-coated stents against
Baseline efficacy of ciprofloxacin coated urinary catheter.
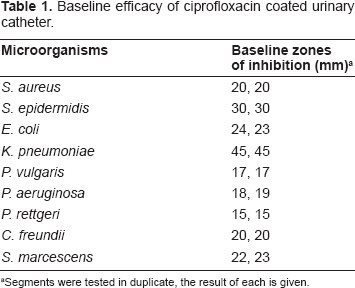
Segments were tested in duplicate, the result of each is given.
Effect of ureteral stents impregnated with different concentrations of ciprofloxacin and N-acetylcysteine each alone and in combination on bacterial adherence to stent surface.
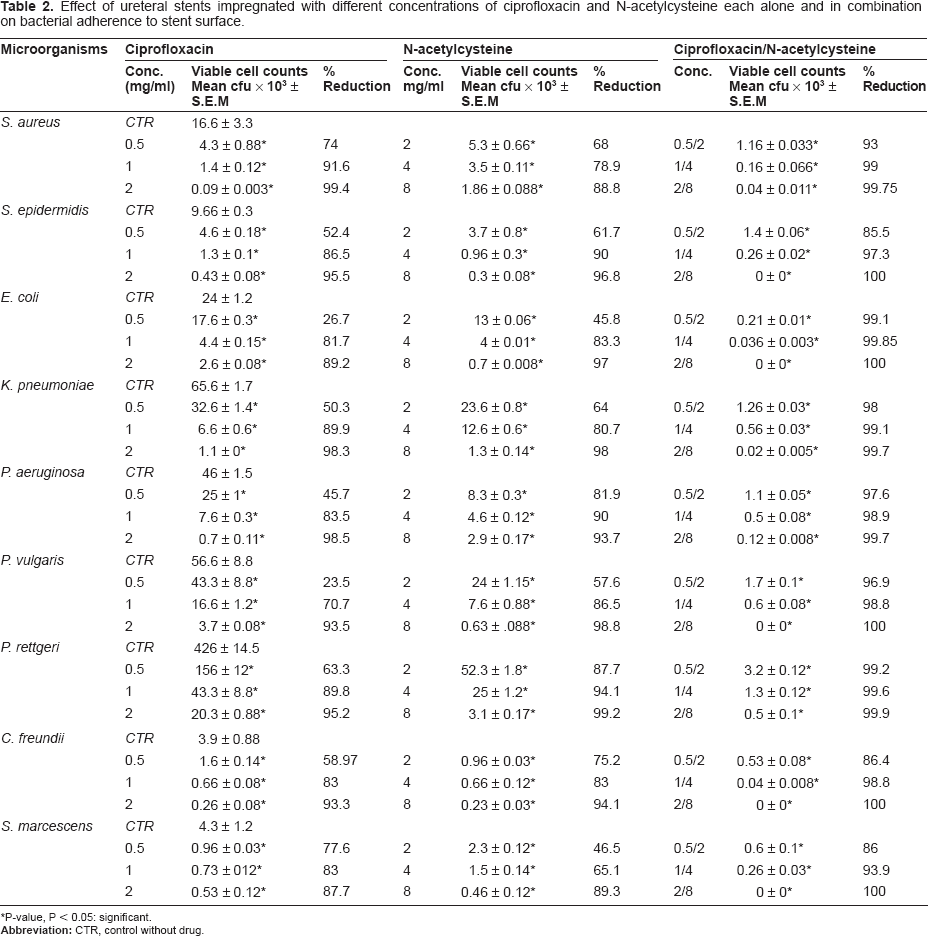
P-value, P < 0.05: significant.
Effect of Ureteral Stents Impregnated with Different Concentrations of Ciprofloxacin, N-acetylcysteine Each Alone and in Combination on Bacterial Adherence
Pretreatment of catheter segments with the tested agents was found to decrease the number of viable adherent cells to stent surfaces. The anti-adherent activity was concentration dependent as the reductive effect of ciprofloxacin at a concentration of 2 mg/ml was in the range of 87.7%–99.4% while the reductive effects of ciprofloxacin at concentrations of 0.5 and 1 mg/ml were in the range of 23.5%–77.6% and 70.7%–91.6% of the controls, respectively. Data show that N-acetylcysteine at a concentration of 8 mg/ml had a significant inhibitory effect on bacterial adherence (88.8%–99.2% of the controls) while the effects of 2 mg/ml and 4 mg/ml were in the range of 45.8%–87.7% and 65.1%–94.1% of the controls, respectively. Ciprofloxacin/N-acetylcysteine combinations were found to be more effective than the effect of each agent alone as CIP/NAC at 2/8 mg/ml showed the highest effect on bacterial adherence (99.7%–100%) while CIP/NAC at concentrations of 0.5/2 and 1/4 mg/ml reduced the number of viable adherent cells by 85.5%–99.2% and 93.9%–99.85% when compared to controls, respectively. These results revealed that N-acetylcysteine increases the therapeutic effect of ciprofloxacin resulting in a significant decrease in the number of adherent cells to stent surfaces.
Discussion
Urinary tract infections are the most common nosocomial infections occurring in critically ill patients. Urinary catheter-associated infections are difficult to be treated with antibiotics and there is a need to change catheters. It is also found that the rates of infections associated with reimplanted devices exceeds that of first time implants by several folds. 7 Catheters are manufactured from silicone or from latex, then coated in either silicone or hydrogel. These materials provide attractive, unprotected sites for bacterial attachment. In addition, irregular surfaces left by the manufacturing process, particularly around eye-holes, can trap cells from an infected urine flows through the catheter. 8
Another problem was found that biofilms produced by urease-positive bacteria such as
A variety of techniques have been designed to prevent biofilm formation, including the controlled release of antimicrobial agents or antiseptics incorporated in the device material, surface coatings with silver and other metals, surface modifications to change hydrophobicity or to create functional groups with intrinsic antimicrobial activity, and anti-adhesive surfaces such as phosphorylcolin.10–13 Several studies showed that Diamond-like carbon coating of ureteral stents is an effective new strategy to improve the surface properties of ureteral stents, decreases friction, encrustation tendencies and biofilm formation. 14 Also, it was found that heparin coated ureteral stents were free from encrustation and biofilm Heparin-coated ureteral stents have limited use as they are more expensive than standard stents and cost four times the price of uncoated stents.15,16
The simplest way to prevent biofilm formation is to impregnate catheters with a broad-spectrum antimicrobial agent that elutes into the surrounding environment and attack planktonic bacteria in the vicinity of the device before they colonize the surface and adopt biofilm-resistant phenotype. 17 Other factors that may have contributed to the superior efficacy of catheters impregnated with antibiotics include the particular method used to incorporate antimicrobial agents into the catheter material, the resulting concentration and availability of those agents on the catheter surface. 18 Difficulties in delivering effective concentrations of antimicrobial agents from catheters for prolonged periods have limited the usefulness of antimicrobial catheters in patients undergoing long-term catheterization.
Ciprofloxacin is active against a wide range of urinary tract pathogens and able to inhibit bacterial colonization of urinary catheters in vitro. 6 It is reported that cells grow in the presence of sub-MIC concentration of ciprofloxacin have lower hydrophobicity and do not adhere to surfaces easily. 19 N-acetylcysteine (NAC) was found to decrease biofilm formation by a variety of bacteria and reduces the production of extracellular polysaccharide matrix while promoting the disruption of mature biofilms. 20 N-acetylcysteine can act as anti-adherent and an antibiofilm agent. In a study carried out by Olofsson et al, 21 it was found that the initial adhesion of bacteria to stainless steel surfaces is dependent on the wettability of the substratum. NAC was shown to bind to stainless steel, increasing surface wettability resulting in decreasing of bacterial adhesion of all tested microorganisms, so that it is expected that an antibiofilm/antimicrobial agent combination would be synergistic. In this study, Ciprofloxacin coated ureteral catheters showed zones of inhibition ranged between 15 and 45 mm in diameter against the tested microorganisms. Also, it is found that ciprofloxacin-coated catheters maintain prolonged antimicrobial durability and activity when soaked in urine against the tested microorganisms and produced zones of inhibition that measured 2–10 mm at 8 weeks. Catheters impregnated with CIP/NAC combinations (2/8 mg/ml) showed the highest efficacy and provided the highest protective effect against microbial adherence. As NAC was found to increase the therapeutic activity of ciprofloxacin. Similar results were obtained by combinations of NAC and fosfomycin 22 and NAC and Tigecycline. 21
Reid et al, 6 reported that pre-incubation of catheters with 50 and 100 μg/ml concentrations (greater than MIC) of ciprofloxacin resulted in up to a 99% reduction in the number of adherent bacteria in comparison to controls that agree with the present study. Reid et al, 23 found that oral fluoroquinolones inhibit biofilm formation and showed no bacteria in patient's urine. They also showed that Ciprofloxacin was more effective as its concentration on the film surrounding stents was significantly higher than that of ofloxacin. On the other hand, Aslam, 24 reported that systemic antibiotics are able to eliminate planktonic organisms released from biofilm but are often ineffective in treating infections resulting from biofilm-embedded organisms.
Johnson et al,
25
reported that nitrofurazone-coated catheter persistently inhibited the growth of the major causative microorganisms of catheter-associated urinary tract infections (CAUTIs) including
Ha and Cho,
27
reported that norfloxacin-releasing catheters, showed continuous delivery of norfloxacin for up to 30 days and have a promising potential for clinical use in patients undergoing long-term catheterization. Cadieux et al,
28
showed that triclosan, is a biocide currently used in medical products that has recently been loaded into a ureteral stent, decreased
In conclusion, catheters impregnated in ciprofloxacin using instant dip method, were shown to have broad spectrum, prolonged antimicrobial durability and high efficacy. In addition, ciprofloxacin/N-acetylcysteine coated catheters showed the highest effect on inhibiting bacterial adherence that result in decreasing the risk of device colonization.
Disclosures
The authors report no conflicts of interest.
