Abstract
A pulmonary artery (PA) catheter was placed in a 60-year-old patient with congestive heart failure, undergoing lumbar spinal surgery. In the prone position, no wedge pressure wave could be obtained, and multiple attempts at repositioning were unsuccessful. Fluoroscopy showed a catheter knot in the right internal jugular vein, which was removed surgically through the original venotomy site. The knot was thought to be caused by excessive manipulation at too great an insertion depth, with low cardiac output. We conclude it is important to follow the guidelines for PA catheter placement, using step-wise gentle manual attempts. If knotted, radiological interventions and surgical extrication must be considered.
Pulmonary artery (PA) catheterization is useful for hemodynamic monitoring in the critically ill, but complications occur in up to 24% of patients (Boyd, 1983). The incidence of major complications, including arrhythmia, hemorrhage, thrombosis, infection, pneumothorax, hemothorax, and cardiac tamponade, is 3%–17% (Abreu, 2004). The formation of an intravascular catheter knot, although rare, is potentially life-threatening (Arnaout, 2001).
We report the successful surgical removal of a knotted PA catheter through the original venotomy site. Although PA catheter knotting is well described, specific guidelines for its proper handling have never been emphasized. A contingency plan is important when this unexpected, perplexing complication is encountered.
Case History
A 60-year-old, 50-kg, 150-cm, female patient with spinal stenosis was scheduled for elective posterior lumbar fusion under general anesthesia. She was receiving oral hypoglycemics for new-onset diabetes mellitus, and had recently undergone percutaneous coronary angioplasty and coronary artery surgery with saphenous vein grafts. She was in congestive heart failure, New York Heart Association class III, and also had chronic renal insufficiency. There was cardiomegaly and an ejection fraction of 30%, with moderate left ventricular hypokinesia and mitral regurgitation. Preoperatively, a cardiologist assessed her cardiac condition as maximally optimized.
After inducing anesthesia, a 7.5 Fr pulmonary artery (PA) catheter, (HANDS OFF®, Arrow International, Reading, PA, U.S.A.) was placed via the right internal jugular vein through an 8.5 Fr introducer (Percutaneous Sheath Introducer®, Arrow International), without difficulty. At 45 cm, the PA pressure was 18/9/12 mmHg; on inflation, the balloon wedged easily, showing a pressure of 10–11 mmHg. The catheter was locked at that time. Without changing the catheter position, the patient was rolled into the prone position via her right side. After re-attaching the monitor, the catheter was still at 45 cm and the PA pressure wave was still present, a wedge tracing could no longer be obtained. Intraoperative repositioning of the catheter by repeatedly withdrawing 10–15 cm and then re-inserting it up to 60–70 cm was unsuccessful. Eventually, it was no longer possible to withdraw the catheter, as firm resistance was encountered with about 40 cm of catheter remaining in the patient. The PA pressure waveform disappeared. No further manipulation was attempted until the end of surgery, when the patient was returned to the supine position. The catheter still could not be withdrawn any further than 30 cm.
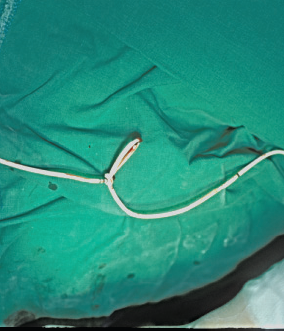
Fluoroscopy showed knotting, with a single loop 5–7 cm in diameter in the right internal jugular vein (Fig. 1). Attempts to remove catheter and introducer together, while tightening the knot using traction at the tip of the introducer, were futile. An interventional radiologist was partially successful at untying the knot using a guidewire. As the patient was still anesthetized and ventilated, consent for surgical removal was obtained from a relative, and a vascular surgeon removed the catheter via a 2-cm venotomy of the right anterior internal jugular vein (Fig. 2).
Portable X-ray showing the knotted pulmonary artery catheter in the internal jugular vein. The picture was taken after the catheter was cut at its proximal end. The reinforced endotracheal tube and median sternotomy wire from the previous open heart surgery are seen. The knotted pulmonary artery catheter after surgical removal. The loop could not be tightened or opened manually.
Discussion
We describe a series of clinical mishaps that led to an entirely avoidable complication. Firstly, it is questionable whether the catheter was needed, as its insertion could have generated no essential information for the clinical management of the patient. Pulmonary hypertension had already been ruled out by echocardiography, which demonstrated no right ventricular/tricuspid valvular dysfunction.
Further, an insertion depth of 60–70 cm was inappropriate, given the initial wedge position with the patient supine of 45 cm. Knotting should have been suspected from the beginning and precautions taken. There was no need to repeatedly inflate the balloon for wedge pressure measurement, as it was already known that PA diastolic and wedge pressure were similar; PA diastolic pressure could have been simply used throughout the course to monitor fluid-volume therapy. Shifting body position from supine to prone might have changed the position of this long, thin-walled, small-diameter flexible catheter, particularly susceptible to bending at body temperature (Bhatti, 2000).
Experience of the physician is the most important guarantee of safe PA catheter insertion. It is imperative to respect the recommended distances and to avoid repeated advance and withdrawal of the catheter. If a knot is suspected, early confirmation using fluoroscopy to detect its initial development (Karanikas, 2002) is strongly recommended to avoid further coiling around a papillary muscle or chordae tendineae (Arnaout, 2001). There is a better chance of non-surgical disentanglement of the knot if it is found early (Mehta, 1998). When a knot is discovered, it is also essential to refrain from extensive manipulation of the catheter. By pulling the catheter against the tip of the introducer, we tightened the knot, making it more difficult to advance the guidewire.
There are several interventional radiological techniques for unraveling knotted catheters. After the guidewire technique failed, our radiologist suggested a femoral approach using loop snares, to be attempted in the cardiac angiography unit. However, it was felt that surgical intervention would eventually be required, given the failed attempts with a guidewire. Further, the patient was still anesthetized, and the catheter laboratory was in another building. The close proximity of the catheter to the subcutaneous venotomy site indicated that a surgical approach would be relatively simple.
To summarize, we suggest the following sequential approach as guidelines for the safe release of a knotted catheter: gentle manual attempts, interventional radiological techniques, and surgical extrication.
Footnotes
Acknowledgement
The original work was conducted at the Department of Anesthesiology and Pain Medicine, Hallym University, College of Medicine, Seoul, Korea.
