Abstract
This article reviews the assessment and management of the pathology of the long head of the biceps tendon, a disease commonly encountered by primary care physicians and orthopedic surgeons. We include a discussion of relevant anatomy, function, pathoanatomy, natural history of the disease, diagnostic methods, and treatment options. Recent literature on the function of the long head of the bicep (LHB) is reviewed. Literature on our evolving understanding of the pathoanatomy behind LHB tendinopathy is discussed. We also discuss the effectiveness of current diagnostic and treatment modalities.
Introduction
The long head of the biceps tendon is an important pain generator in the shoulder. Clinical assessment of the tendon can be difficult and treatment of LHB tendinopathy can be challenging. There are numerous operative and nonoperative treatment options, and debate exists over the utility of these modalities. We discuss the relevant anatomy, function of the LHB tendon, pathoanatomy of LHB tendinopathy, clinical evaluation of the patient, and the array of treatment options, with a particular emphasis on nonoperative treatment.
Methodology
The PubMed and Ovid MEDLINE databases were searched using subject headings and keywords for the concepts of biceps, shoulder joint, long head, tendinopathy, diagnosis, ultrasound (US), arthroscopy, pathology, therapy, and surgery. All studies published 20 years ago were excluded. The references of selected articles were also reviewed.
Anatomy
The LHB tendon originates as an intra-articular structure in the shoulder joint (Fig. 1). Specifically, it originates from the supraglenoid tubercle and superior labrum. Rare anatomic variations of the tendon origin do exist. These include origins off the shoulder capsule, rotator cable, and the supraspinatus.1–3 From its origin, the LHB tendon runs through the rotator interval between the anterior edge of the supraspinatus tendon and the superior edge of the subscapularis tendon, deep to the coracohumeral ligament. The tendon then makes a 30- to 40-degree turn in an inferior direction to exit the shoulder joint. 4 At this turn, the tendon is partially stabilized by the biceps sling (or biceps pulley). This structure is made up of the coracohumeral ligament, superior glenohumeral ligament, and the deep fibers of the supraspinatus and subscapularis tendons. After exiting from the shoulder joint, the LHB tendon travels through the bicipital groove of the humerus. The transverse humeral ligament covers the tendon as it runs through the bicipital groove. The musculotendinous junction of the biceps is encountered soon after the tendon exits from the bicipital groove. The tendon is innervated by sensory sympathetic fibers and its vascular supply is the biceps vinculum (Fig. 2). 5 This tissue lies over the top of the groove. Osteotendinous branches off the thoracoacromial and brachial artery also contribute to the tendon's blood supply. Approximately 1.2–3 cm distal to the origin of the tendon is an area of hypovascularity that relates to the tendon's transition from being intra-articular to just distal to the biceps sling. 6 This area of focal hypovascularity puts this region of tendon at particular risk for attrition and dysfunction.
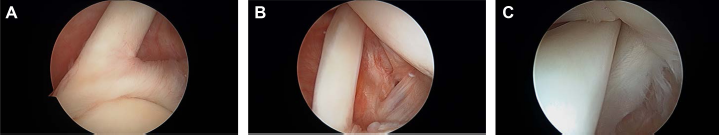
Arthroscopic images of a healthy intra-articular LHB tendon. (

Intra-operative photograph of biceps vinculae. The LHB tendon receives a direct vascular supply via the vinculae. In this photograph, the LHB tendon has undergone arthroscopic tenotomy and has been retrieved through a separate axillary incision. The proximal aspect of the LHB tendon is grasped by a hemostat, and the vinculae is held in the surgeon's left hand.
Function
The main function of the biceps muscle is forearm supination and elbow flexion. It contributes little to the abduction of the shoulder (approximately 10% of the total power), and only when the arm is in external rotation. 7 Studies from the 1990s describe superior translation of the humeral head in shoulders deficient in the LHB while in abduction. 8 Cadaveric studies by Warner showed a decrease in torsional forces across the glenohumeral joint while in abduction and external rotation in shoulders with an intact LHB tendon. 9 However, the role of LHB in depression of the humeral head is controversial. Recent electromyographic analysis refutes this function and calls into question its clinical significance.10,11,57 More research is needed to determine if the LHB tendon has a passive function that does not require active contraction, as this tendon function would not be detected in an electromyographic analysis. In another electromyographic analysis, Kim et al made the assertion that the LHB provides stability to the glenohumeral joint only in the setting of an unstable shoulder joint. 12 This was reinforced in a cadaveric research by Elser et al where they determined that the LHB tendon functional importance increases as shoulder stability decreases. 13 Further research is needed to determine the subtle active and passive functions of the LHB tendon.
Pathoanatomy and Natural History
The natural history of LHB tendon dysfunction, and ultimately tendon failure, begins with tenosynovitis (Fig. 3). The development of tenosynovitis is marked with fluid development, increased vascularity, and adhesions. 14 This does not appear to be mediated with inflammatory cells. Rather, recent histopathologic analysis showed only 2 of 26 tendons had chronic inflammation and none demonstrated acute inflammation. 15 Pathology appears to be mediated by cytokines and growth hormones released because of altered mechanics of the tendon. 16 Tendinosis is the second stage and is best appreciated on magnetic resonance imaging (MRI), US, or arthroscopically. Fibrillations and splits as well as hypertrophy are the hallmarks. From there, delamination can occur in the weakened tendon. Finally, there is a frank rupture of the tendon. Generally, a complete rupture is preceded with the propagation of a chronic partial tear. Ruptures generally occur in the hypovascular zone 1.2–3 cm from the long head tendon origin. 6 After a complete rupture, there may be a total resolution of symptoms.

Arthroscopic images of a pathologic intra-articular LHB tendon. All images are oriented such that the glenoid is on the bottom, and the humeral head is on the top of the image. (
LHB tendinopathy is very commonly associated with rotator cuff tears. Beall et al and Murthi et al found a 90% association between rotator cuff tears and LHB tendinopathy.14,17 Additionally, LHB tendon instability occurs in up to 45% of patients with rotator cuff tears. 18 Any failure of the biceps sling, which is partially composed of portions of the rotator cuff, can lead to tendinopathy of the LHB. There appears to be an especially high rate of instability and entrapment of the LHB when subscapularis tears are present. 19 The subscapularis tendon contributes fibers to the biceps sling, and additionally, the transverse humeral ligament is an extension of the subscapularis tendon across the bicipital groove. Therefore, stability of the LHB tendon relies on an intact subscapularis tendon. In a cadaveric study, Kwon et al found that the subscapularis tendon is the most critical structure for LHB tendon stability, when compared to the coracohumeral ligament, subscapularis tendon, and transverse humeral ligament. 17 Instability of the LHB, resulting in subluxation or frank dislocation of the tendon out of the bicipital groove can occur in the medial or lateral direction. Lafosse et al noted that dislocations often occurred only in the medial direction, and this was more frequently seen in patients with subscapularis tears. 16
Tears of the superior labrum at the biceps anchor (commonly known as superior labral anterior-to-posterior tears, or SLAP tears) can also incite biceps tendinopathy and instability. Type 2 SLAP tears destabilize the biceps anchor, and type 4 SLAP tears extend into the LHB tendon. SLAP tears can be an isolated cause of anterior shoulder pain, or they may occur concurrently with LHB tendinopathy as a cause of anterior shoulder pain.
The study of the natural history of LHB tendon is challenging for several reasons. It is unclear why some people can be pain free after an LHB tendon rupture and some will not have resolution of their symptoms. Another complicating factor is the relative rarity of isolated LHB pathology without rotator cuff involvement. LHB tendinopathy can be isolated in certain populations, including swimmers, gymnasts, and throwing athletes. As discussed earlier, there is a close relationship between the LHB tendon and the rotator cuff. If the cuff is damaged, it will increase the attrition on the LHB tendon. More research is needed to determine the end stages of the natural history of LHB tendinopathy.
History, Presentation, and Diagnosis
LHB tendinopathy can have a variety of clinical presentations. Patients can present with anterior shoulder pain, pain that occurs while the patient is not actively moving his or her upper extremity, that is, rest pain, night pain, and pain with radiation down the arm. Pain can be exacerbated with activities that require repetitive overhead motion, throwing, supination, and elbow flexion, such as chest fly's, pull-ups, or reaching behind oneself. 16 Rarely, one can appreciate instability of the tendon with an audible or palpable clunk or snap. 20 When a rupture occurs, the patient may appreciate a ‘popping’ sensation in his arm and may even note a snapping sound. Ecchymosis around the shoulder can occur. A resultant “Popeye” deformity is classic for a complete rupture. This deformity is named after the 1930s cartoon character Popeye the Sailor Man who had especially protuberant biceps. The deformity can be defined as a bunching of the bicep muscle belly distal from the rupture. This resultant muscle bulge is asymmetric with the contralateral arm. However, the absence of a “Popeye” deformity does not preclude the diagnosis of a complete rupture, as there may be an autotenodesis of the tendon. LHB tendon rupture may be associated with relief of tension or pain in the shoulder. A decrease in forearm supination strength compared to the contralateral side is also noted with a complete rupture. Ruptures account for 96% of all bicep injuries in patients older than 50 years. 21
There are several clinical tests, including the Speed's and Yergason’ tests, that have been described to evaluate for LHB tendon pathology.19,21 Additionally, clinical tests that are more specific for rotator cuff and labral pathology, including the O'Brien's, belly press, bear hug, upper cut, anterior slide, and dynamic labral shear tests, are helpful in the evaluation of the patient. 21 Some of these physical examination maneuvers lack sensitivity or specificity.22–24 For example, several studies show that the sensitivity for detecting LHB tendon pathology using the Speed's test ranged from 49 to 71%.24,26 Hegedus in 2012 (LOE IIa) provided an excellent review on the sensitivity and specificity rates of clinical tests in detecting specific shoulder pathology. 24 They concluded that even with combinations of tests, the sensitivity and specificity still remain suboptimal. 24 However, Kibler's study on the utility of combining multiple clinical tests argued against this conclusion. He showed that the combination of upper cut and Speed's test were significantly better at detecting bicep pathology than other tests (LOE II). 25 Another physical examination finding used to detect bicep pathology is pain with palpation of the bicipital groove. A more recent study noted a low sensitivity for detecting bicep pathology when using palpation of the biceptal groove. 20 This test is most easily performed with the arm in 10 degrees of internal rotation. However, a prospective single-blinded study from 2011 (LOE II) showed an accuracy rate for precise palpation of the LHB tendon within the intertubercular groove of only 5%. 26 Another study showed a sensitivity and specificity of 54% for this test. 27 Therefore, it may be best to utilize US to localize the groove, especially if there will be a diagnostic or therapeutic injection.
The best diagnostic tool for detecting LHB pathology is US. It is cheap, quick, may be used in the office, has no radiation, has the potential for dynamic examination, and most importantly has high sensitivity and specificity. 23 In the literature, the sensitivity of US in detecting LHB pathology ranges from 50 to 96%, and specificity ranges from 98 to 100% when compared to MR arthrography and arthroscopy retrospectively (LOE III).23,28,29 Older literature noted a decreased ability of US to detect partial tears, but this has been refuted in more recent literature.30,31 Drawbacks include the need for operator expertise and interference related to body habitus. If there is suspected rotator cuff pathology or SLAP tear or if the patient is obese, then MRI is the modality of choice.32–34
MRI is a less ideal option for diagnosing tears or inflammation of the LHB tendon. Tendon degeneration is generally diagnosed by noting changes in diameter as well as signal alteration. These findings may be subtle and can be missed or labeled incorrectly as artifact. 35 Mohtadi et al noted in a prospective double-blinded study (LOE Ib) that there is poor correlation between MRI and arthroscopic findings in regard to LHB tendon tears and inflammation. 36 Carr et al in 2016 noted a 27% sensitivity and 86% specificity for detecting partial LHB tears by MRI scan. 16 Complete tears were diagnosed only 54% of the time. Dubrow in 2014 had similar findings. 37 Interobserver agreement using MRI to detect bicep tendon tears was 60% in one study. 38 In contrast, Roy et al published a review in 2015 of diagnostic modalities for rotator cuff tears and determined that MRA, MRI, and US all had similar results. They recommended utilizing US instead of MRI for diagnosing full thickness rotator cuff tears, citing factors including accuracy, access, cost, and efficiency. 39
MR arthrogram has been the study of choice to detect SLAP lesions, and previous literature has shown that MRA can effectively examine the LHB tendon and biceps sling, with sensitivities approaching 89–92% and specificity 56–81%.19,40
Arthroscopic examination is generally considered the gold standard for detecting LHB pathology. 25 27,58 During examination, the LHB must be pulled fully into view in the glenohumeral joint to ensure there is no pathology of the extra-articular portion of the tendon. However, even when pulling the tendon into view, a recent cadaveric study showed only 14 mm, or only 17% of the extra-articular portion of the tendon could be visualized. 41 Other recent literature showed that arthroscopy failed to diagnose lesions in the bicipital tunnel 30–50% of the time.42,43
US-guided local anesthetic injection into the LHB tendon sheath is another diagnostic option that may be performed in the clinic. This is a quick and simple procedure and may be therapeutic if steroids are also injected. In a review of randomized controlled trials (LOE I), Naredo et al noted significantly decreased shoulder pain and improved function at six weeks with US-guided steroid injections compared to blind steroid injections. 40 These improved outcomes are likely secondary to improved accuracy with injections localized using US versus blind injections.41,42 One study showed an accuracy rate of 86% compared to 26% when using US versus no image guidance, respectively, to assist in biceps tendon sheath injections. 44 When performing steroid injections, it is important to avoid injecting into the tendon itself due to the risk of tendon rupture. 45
In summary, we recommend performing a clinical assessment with Speed's test and upper cut test, as well as localization of the shoulder pain. A full evaluation of the rotator cuff and superior labrum should be performed. If suspicion is high for isolated bicep pathology, we would recommend US evaluation. If there is rotator cuff pathology or a SLAP lesion suspected, then an MRI or MRA, respectively, should be obtained.
Nonoperative Treatment
Conservative treatments for long head bicep tendinopathy include rest, NSAIDs, ice, activity modification, and corticosteroid injections. A physical therapy program should be initiated, focusing on stretching the anterior shoulder structures including the pectoralis minor, as well as correcting scapular dyskinesis, if present. Generally, these treatment options constitute first-line therapy. Corticosteroid injections have an improved efficacy when US-guided.46–48 An injection into the glenohumeral joint is also an option but may be less effective than an injection within the biceps tendon sheath.19,49 Mechanical stimulation using dry needling has been shown in animal studies to increase blood flow to the area, thereby introducing growth factors and potentially tendon healing.50,51
Once the acute phase has passed, the patient can begin a physiotherapy program. This would start with range of motion activities and stretching with progression to core and scapular strengthening activities. 52 Stretching of the lower back and hamstring should be included. 53 Next, the patient would graduate to a rotator cuff–strengthening program and eventually a strength regimen of progressive difficulty. If the patient is a thrower, he would start on a progressively more rigorous throwing regimen once the rotator cuff has strengthened sufficiently.
When rupture of the LHB tendon occurs, the patient may be treated conservatively with rest, ice, NSAIDs, and activity medication. Older literature urged practitioners to counsel patients to expect an 8–20% loss of elbow flexion strength and a 10–20% loss of forearm supination strength.54,55 A study by Deutch et al showed that supination strength and endurance loss can be up to 25%. 56 At the time of publication, the writers were unaware of any research directly comparing upper extremity strength in patients with bicep ruptures to those with an LHB tenotomy. However, if one assumes that the two clinical end points are similar, then tentomy functional data can be applied to bicep ruptures. Several recent reviews of level IV studies (LOE IV) showed no significant change in muscle strength and no clinically important change in Constant scores in patients who had an LHB tenotomy versus tenodesis.52,57,58 Patients should be counseled that they may have a “popeye” deformity as the LHB contracts from proximal to distal. The rate of “popeye” deformity development for LHB tenotomy can be as high as 27%.59,60 This can be extrapolated to the population of patients with spontaneous ruptures of the LHB. However, it should be noted that in one study, only 40% of the patients noticed the deformity. 61 In several reviews (LOE IV), it was noted that the majority of the patients who had a “popeye” deformity were not bothered by it.52,57,58 An explanation for the observation that not every patient gets a deformity after rupture or tenotomy was provided by Gothelf et al. He showed there was significant soft tissue restraint inside the bicipital groove, which may lead to an “autotenodesis” of the tendon to the proximal humerus, thereby preventing distal excursion of the long head of the biceps. 62 Kuhn et al showed that if there was a portion of superior labrum attached to the biceps tendon, it required significantly more force to be pulled through the bicipital groove, thereby preventing retraction of the LHB distally. 63 One study showed that up to 87% of patients had an autotenodesis after tenotomy. 64
Operative Treatment
Indications for surgery include tearing of 25–50% of the tendon diameter, disruption of biceps sling, longitudinal tears resulting in poor gliding in groove, catching symptoms, and subluxation of the tendon. Surgical options breakdown into two main categories: tenodesis procedures and tenotomy procedures. Both categories can be open or arthroscopic. LHB tenodesis is becoming significantly more popular in the United States, with the incidence of this procedure increasing from 2008 to 2011 by 1.8 fold. 65
Advantages of tenotomy include decreased cost, no need for implants, decreased surgical time, and no restrictions after surgery. 66 Disadvantages include cramping of the biceps muscle with activity, “popeye” deformity, and loss of forearm supination and elbow flexion strength and endurance. Generally, the cramping resolves within six to eight weeks, but it may occasionally persist. 67 Persistent biceps pain and cramping can occur in 3 to 38% of patients undergoing tenotomy.61,68,69 Kelly et al found that elderly populations may not note any fatigue discomfort, and on examination, the elderly population who had undergone tenotomy showed no strength difference compared to the contralateral side. 68 In two recent studies, the rate of “popeye” deformity was higher after LHB tenotomy (27%) compared to tenodesis (9%).59,60 An alternate and promising avenue for minimally invasive management of LHB tendinopathy is US-guided percutaneous LHB tenotomy. This technique has been shown to be successful in cadavers. 70 In Canada, Aly et al performed US-guided percutaneous tenotomies on six cadavers, resulting in complete transections of the long head of the long head of the bicep tendon in all cadavers. 71 The significance of the retained proximal 1–2 cm of tendon left attached to the superior labrum after this procedure is still unclear.
LHB tenodesis creates an appropriately tensioned muscle, allowing the potential return of full strength and muscular endurance. There is a decreased rate of “popeye deformity.” The potential drawbacks of LHB tenodesis include retained hardware, implant cost, prolonged surgical time, and risk for re-rupture. There is also concern that an incorrectly positioned implant could alter the glenohumeral dynamics. Giphart et al found the risk of altering the glenohumeral kinematics with LHB tenodesis is very small in an otherwise stable shoulder. 72 Tenodesis can be performed open or arthroscopically using suture anchors, interference screws, or the “keyhole” technique. The “keyhole” technique passes a plug of the long head of the bicep tendon between two cortical drill holes one centimeter proximal to pectoralis major tendon and distal to the transverse ligament. 73 Clinical and radiographic failure rates have been noted to be 18%—approximately equivalent to other techniques (LOE IV). 74 Both the arthroscopic interference screw and “keyhole” technique have been noted to have equivalent clinical and radiographic outcomes (LOE II). 75 Another technique is the T-shaped tenotomy. This is a release of the long head of the bicep with a portion of the superior labrum. 63 This “T”-shaped structure then becomes entrapped within the bicipital groove. There is currently a paucity of data comparing this technique to others. Transfer of the LHB to the conjoint tendon is another technique with equivalent biomechanical properties to a subpectoral tenodesis (LOE V). 76
Multiple studies and reviews have looked at the merits of tenotomy and tenodesis.52,53,57,58,64,77 Frost showed equivalent results in the tenotomy and tenodesis groups except for the development of “popeye” deformities, which is significantly higher in the tenotomy group. 78 Hsu compared pain, Constant score, and UCLA score, and found results similar to those found by Frost, with the addition that there was a lower load to tendon failure rate in the tenotomy group. 77 Koh showed an improvement in the Constant and ASES scores, a decrease in the rates of “popeye deformity” in the tenodesis groups but no difference in pain or strength or cramping. 60 The ideal location of the bicep tenodesis is still not definitively known, but Moon et al (LOE IV) noted 80% of bicep tears evaluated had a hidden lesion in the bicipital groove. He proposed a subpectoral tenodesis location to ensure that no hidden lesions were missed out, as might occur with a more proximal tenodesis. 79 Werner et al (LOE III) also looked at suprapectoral versus subpectoral tenodesis and found no clinical difference two years postoperatively. 80 A biomechanical study comparing fixation techniques for proximal biceps tenodesis noted that an open subpectoral interference screw technique had the highest ultimate load to failure. 81 More high-quality research is required to determine the best location for tenodesis. Other procedures for the treatment of LHB tendinopathy include isolated arthroscopic synovectomy, which is generally not effective in resolving symptoms. 82 Coracoplasty and acromioplasty constitute mainly a type of historical treatment. Bicep relocation and reconstruction of pulley were shown in one study to have a 25% re-rupture rate. 83
Conclusion
Tendinopathy of the long head of the biceps encompasses a broad spectrum of disease burden, from mild tendinopathy to rupture. Two distinct patient populations present with this disease—the active overhead athlete who generally presents with tendinopathy and the older patient who generally presents with tendinopathy that may progress to frank rupture. Young patients can present with isolated bicep tendinopathy or can have an associated SLAP tear leading to biceps instability and tendinopathy. In older patients, this condition is commonly associated with rotator cuff pathology. Recent literature has pointed to a change in thinking about the pathology of the LHB tendon. Originally, it was thought this was inflammation and tendinitis. Now it is known that even in young athletes, LHB tendinopathy is more of a degenerative process and less of an inflammatory process. 14 Physical examination findings can help to diagnose this condition, but US appears to be the best method to obtain a definitive diagnosis. MRI or MRA should be used when there is suspected rotator cuff pathology or SLAP tear, respectively. Treatment options depend on the severity of the pathology and the patient's activity level. The mainstay treatment is rest, ice, NSAID use, steroid injections into the sheath, activity modification, and physical therapy. Once conservative therapy fails, older patients with a low activity level may tolerate a tenotomy very well. Tenodesis is generally preferred for patients with high activity levels, patients who are working, and younger patients.
Author Contributions
Analyzed the data: RBL. Wrote the first draft of the manuscript: RBL. Contributed to the writing of the manuscript: RBL, BAR. Agree with manuscript results and conclusions: RBL, BAR, MSK. Jointly developed the structure and arguments for the paper: RBL, BAR, MSK. Made critical revisions and approved final version: RBL, MSK. All authors reviewed and approved of the final manuscript.
