Abstract
Extranodal lymphoma (ENL) occurs in approximately 30%–40% of all patients with non-Hodgkin lymphoma and has been described in almost all organs and tissues. However, diffuse large B-cell lymphoma is the most common histological subtype of non-Hodgkin lymphoma, primarily arising in the retroperitoneal region. In this article, we report a rare case of an adult male diagnosed with primary diffuse large B-cell lymphoma of the gluteal and adductor muscles with aggressive bone involvement. All appropriate radiological and histopathological studies were done for diagnosis and staging. After discussion with the lymphoma multidisciplinary team, it was agreed to start on R-CHOP protocol (rituximab, cyclophosphamide, doxorubicin (Adriamycin), vincristine (Oncovin®), and prednisone) as the standard of care, which was later changed to R-CODOX-M/R-IVAC protocol (rituximab, cyclophosphamide, vincristine (Oncovin®), doxorubicin, and high-dose methotrexate alternating with rituximab, ifosfamide, etoposide, and high-dose cytarabine) due to inadequate response. Due to the refractory aggressive nature of the disease, subsequent decision of the multidisciplinary team was salvage chemotherapy and autologous stem cell transplant. The aim of this case report was to describe and evaluate the clinical presentation and important radiological features of extranodal lymphoma affecting the musculoskeletal system.
Introduction
Non-Hodgkin lymphoma (NHL) may be extranodal in origin in approximately 30%–40% of patients. Extranodal involvement may also be due to the regional spread of nodal disease or hematogenous dissemination.1,2,8 Primary skeletal muscle NHL of diffuse large B-cell immunophenotype is exceptionally rare (incidence rate of 0.1%–0.5% in all extranodal lymphoma (ENL) of the extremities). 5 7 However, diffuse large B-cell lymphoma (DLBCL), which is the most common histological subtype of NHL, primarily arising in the retroperitoneal region, has rarely been reported. In this indexed case, there was extensive gluteal and retroperitoneal muscular involvement without affecting the genitourinary system. A few cases have been reported in the available literature. 2 Despite advances in imaging devices over the past decade, accurate diagnosis of soft tissue tumors remains a challenge for clinicians, requiring a close team approach between the surgical oncologist, musculoskeletal radiologist, and pathologist. 3
Case Presentation
We present a case of a male patient in his 40s with a history of right proximal thigh and hip swelling associated with unintentional weight loss (10 kg) over a month. There was no history of trauma, intramuscular injection, neurological symptoms, fever, or any signs of infection. On examination, the patient was afebrile; vital signs were within normal range. Right thigh and buttock showed a huge firm swelling with circumferential edema involving the anteromedial aspect of the thigh up to the gluteal region. Distal lower limb pulses were normally felt.
The patient underwent extensive hematological and radiological diagnostic workup. Complete blood count and electrolytes were normal. Creatine kinase was high, 492 Units/L (30–200 Units/L). Radiograph of right femur and pelvis was done (Fig. 1). Doppler ultrasound of the right lower limb veins showed evidence of extensive deep vein thrombosis. Doppler ultrasound of right lower limb arteries was performed, which revealed no abnormalities. Abdominal ultrasound was negative for solid organ involvement; however, retroperitoneal evaluation was grossly limited due to bowel gas.

X-ray Right hip AP view shows lytic area with surrounding sclerosis (arrow)in the femoral head. Soft tissue opacity in the thigh on the medial aspect (star).
Magnetic resonance imaging of the whole spine and pelvis, including thigh, was done (Figs. 2, 3, 4A and B), which showed asymmetrical muscular enlargement with abnormal signal intensity and heterogeneous enhancement involving bilateral pelvic musculature more on the right side and right proximal thigh musculature, confirming the characteristics of a malignant mass. Multiple bone involvement was also noted, including both femoral head and neck, both ilia, and left proximal femur. Remarkably, the partial collapse of vertebrae at various levels was more severe at T12 and L2.

Coronal STIR Sequence shows abnormal bright signal in the femoral head, neck, ilium, Right Gluteus ’ Right adductor muscles. Right extensive subcutaneous edema.

T2 sagittal and T1 sagittal post contrast images showing partial multilevel vertebral collapse more severe at T12 and L2 vertebrae with abnormal marrow signal.

(
Ultrasound-guided biopsy of the right gluteal lesion was done, and histopathology slides were reviewed (Figs. 8, 9A and B). The specimen comprised mainly tumor necrosis and scanty viable tumor cells. The latter were manifested by diffuse large atypical lymphocytes with abundant apoptosis and prominent mitoses. The better preserved tumor cells were arranged around blood vessels. The atypical lymphoid cells were of B-cell lineage (CD20) and were also positive for CD45, BCL2, BCL6, CD10, and BOB-1. They had a high proliferation index with Ki-67 (85%). They were negative for MUM1, CyclinD-1, and CD23. There was a background population of T-cells (CD3 and CD5).
The patient was transferred to our cancer facility for staging workup and further management. Bone marrow was examined that showed no definitive morphologic or immu-nophenotypic evidence of marrow involvement by lymphoma. Meanwhile, the patient was started on tumor lysis prevention measures, prophylactic antimicrobials, and full anticoagulation and was referred to the pain management team.
Final diagnosis and staging: DLBCL; germinal center type with no bone marrow involvement. Stage IVB, bulky disease, high risk of International Prognostic Index.
The lymphoma multidisciplinary team (MDT) discussed the case and decided to start the patient on R-COP as an initial debulking chemotherapy, followed by R-CHOP protocol (6–8 cycles) as a standard of care, with mid-cycle radiological response assessment. In addition, central nervous system prophylaxis (intrathecal chemotherapy ± high-dose methotrexate) was essential. Radiotherapy to be considered at the end of treatment. Intensive multiregimen therapy such as R-CODOX-M/R-IVAC protocol was discussed as well, due to the aggressiveness of the tumor and high proliferation index.
The plan was discussed with the patient, and he accepted to undergo chemotherapy. He received R-COP, followed by R-CHOP by MDT decision. Subsequent persistent thrombocytopenia precludes full anticoagulation and hence was held, and inferior vena cava filter was inserted.
In spite of that, the patient was consistently complaining of severe abdominal pain associated with progressive lower limb swelling and a drop in the hemoglobin level. Emergent abdominal ultrasound was done, which showed a large retroperitoneal collection close to the right psoas muscle, displacing the right kidney anteriorly.
Computed tomography (CT) angiogram of abdomen and pelvis was done for further clarification, which revealed a large right-sided retroperitoneal hematoma along the right psoas muscle (Fig. 5), extending for a length of approximately 16.5 cm, with a maximum transverse dimension of 8.5 cm. Left femur neck fracture was detected with left gluteal hematoma measuring about 8.2 × 6.4 cm. Moreover, pathological fracture lines of the right femur neck were observed.

CT axial image shows right retroperitoneal mass involving psoas muscle.
The patient was not improving clinically and was in persistent pain, despite the maximum measures applied by the pain management team. A positron emission tomography–computed tomography (PET/CT) was ordered for evaluation of the disease after two cycles of chemotherapy, which showed the progression of the disease with redemonstration of right thigh medial ill-defined infiltrative mass with moderate uptake (SUVmax up to 5.0). Multiple bone involvement, with intense uptake (SUVmax up to 9.4), was seen in several vertebrae, bilateral humeri, femora, clavicles, sternum, pelvic, and skull bones, mostly corresponding to lytic bony lesions. Sclerotic foci were also noted with decreased tracer accumulation (Fig. 7).
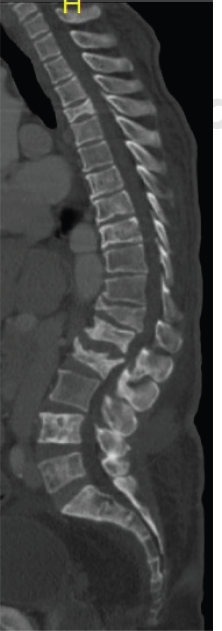
Sagittal CT scan shows multiple collapse of the vertebral bodies, most severe is noted at T12 &L2.

PET MIP show extensive bony metastasis.

The H&E section reveals fibromuscular tissue infiltrated by diffuse, monotonous atypical cells with crushing (streaking) artifact. Tumor necrosis is abundant.

Chemotherapy was continued after stabilization of the patient, with another cycle of R-CHOP. After two weeks, CT chest, abdomen, and pelvis was repeated that revealed differential response in the form of significant progression of the retroperitoneal mass. The left gluteal muscles showed a de novo infiltrative mass lesion with central hypodensities. However, a relative reduction of the previously reported extensive infiltration, forming a large mass extending from the right inguinal region toward the proximal aspect on the medial side of the right thigh, and also a reduction of the infiltrative lesion in the right gluteal muscles were noted. Almost a stationary course of the osseous involvement with collapse of the vertebral bodies DV4, DV9, DV12, LV1, and LV2 was noted (sagittal CT Spine, Fig. 6).
The lymphoma MDT rediscussed the case and decided to proceed with a more aggressive protocol (R-CODOX-M/ R-IVAC) due to the progression of the disease. The plan was discussed with the patient and he agreed. The first cycle of R-CODOX-M was given three weeks after the last cycle.
The PET/CT scan was repeated after three weeks of R-CODOX-M due to nonimprovement in the patient's condition, which showed treatment-resistant disease, in terms of increasing uptake and extent of multiple bone involvement, in addition to increasing size and uptake of the spleen. The case was referred again for MDT discussion due to refractory aggressive disease, with poor performance status. The decision was for salvage chemotherapy and autologous stem cell transplant, if the patient agreed. The plan was discussed with the patient, but he preferred to travel back to his home country. Therefore, arrangements were made through the social worker and the case manager to facilitate the patient's transfer safely.
Discussion
About 30%–40% of all NHL cases arise from sites other than lymph nodes, spleen, or bone marrow.1,2,8 They may also arise from sites typically devoid of lymphocytes. Almost half of all ENL cases reported had DLBCL histology. 8 Often, the primary extranodal presentation requires site-specific strategies for either diagnosis or therapy. 8 Moreover, the particular presenting sites may per se have prognostic implications, and not just the histologic type. 8 , 9
In the literature, the definition of primary ENL is still controversial, and this may contribute to their varying percentages in comparison with the nodal ones. 8 , 10 The designation of stage III and IV lymphomas as primary ENL is indeed questionable, since extranodal involvement in the presence of mainly nodal or disseminated disease may represent secondary extranodal disease spread. 8 Currently, it is accepted to define operationally as extranodal those lymphomas with no or only minor nodal involvement associated with a clinically dominant extranodal component. As for the definition, there is no consensus about the staging of primary ENL: the Ann Arbor staging system is at present widely used for describing the extent of the disease. 8
ENLs can originate in almost every organ. Data from large series reported in the literature have shown gastrointestinal tract, skin, bone, and brain to be the most common sites of ENL; the head and neck localizations are the second most frequent site. 8
Involvement of the skeletal muscles by NHL is unusual.7,20–22 The most commonly affected muscles are those of the extremities, pelvis, and gluteal regions, occurring as a result of metastatic hematogenous, lymphatic spread, or contiguous spread from adjacent involved lymph nodes or bone. 3 Lymphoma spreads by infiltration of malignant cells that lack extracellular stroma and intercellular junctions, resulting in diffuse enlargement of the involved structures and passing fascial boundaries. Thus, the involvement of more than one muscle compartment is typical. 7
Primary skeletal muscle lymphoma is a rare disease, accounting for only 0.5% of all ENL cases, which mainly (>95%) consists of B-cell and NHL type. 7 Primary lymphoma of the muscle has been associated with a poor prognosis and usually has a diffuse large cell histologic feature.7,23
To date, only a few cases of malignant lymphoma with extensive involvement of retroperitoneal, gluteal, and thigh musculature have been reported in the literature (Table 1).
List of published cases of Extranodal lymphomas (listed chronologically).

The most essential radiologic features of ENL affecting the musculoskeletal system are permeative lytic bony destruction and extensive muscular involvement, as seen in our case; however, it will always impose a remarkable diagnostic challenge to reach a conclusive diagnosis. Reasonable differential diagnoses include soft tissue sarcoma, malignant musculoskeletal tumors such as malignant fibrous histiocytoma, malignant neurogenic tumor as Malignant Peripheral Nerve Sheath Tumors (MPNST), or metastasis, rather than malignant lymphoma. 3
The treatment of primary skeletal muscle lymphoma relies predominantly on the type of lymphoma. The prognosis of primary skeletal muscle lymphoma is poor compared with that of lymph node lymphoma, especially at stages III–IV. Therefore, selecting the most effective treatment regimen is essential. 7 The combination of chemotherapy and radiotherapy significantly increases disease-free survival and overall survival rates. 5
The ASCO's recent guidelines strongly recommend PET/ CT for staging of routinely fluorodeoxyglucose avid histologies, especially in clinical practice. 4 A contrast-enhanced CT scan should be included for a more accurate measurement of nodal size if required for trials, to more accurately distinguish bowel from lymphadenopathy, and in the setting of compression/ thrombosis of central/mediastinal vessels. 5
Conclusion
We believe that this case adds an important piece of evidence to the clinically significant problem of systematic diagnostic strategy for an unusual presentation of malignant lymphoma. Moreover, this case emphasizes the crucial role of MDT discussions in Diagnosis and management of such a rare case, where limited clinical guidelines are available.
Author Contributions
Conceived and designed the experiments: SK, MY. Analyzed the data: SK, AN, SA. Wrote the first draft of the manuscript: SK, AN, SA, AA, MY. Contributed to the writing of the manuscript: SK, AN, SA, AA, MY. Agree with manuscript results and conclusions: SK, AN, SA, AA, AE, HO, MY. Jointly developed the structure and arguments for the paper: SK, AN, SA, MY. Made critical##
