Abstract
Desmoid tumors (DTs) are rare tumors classified as deep fibromatoses taking origin from fascial or musculoaponeurotic structures. With pregnancy and surgical scars considered in the etiology, most anterior abdominal wall DTs occur in women in their reproductive years, especially during a pregnancy or post-partum. Herein, we present development of DT in a female patient in the post-partum period following cesarean delivery, which manifested itself with a growing mass in anterior abdominal wall. In our case, possibility of hematoma most probably located beneath the fascia was considered initially as a complication of cesarean section based on ultrasonographic examination and location of the lesion, while upon lack of either spontaneous regression with eventual diminish in size or resolve of symptoms within six weeks, further investigation via MRI and tru-cut biopsy revealed the diagnosis of abdominal DT. Radical tumor extirpation with resection of an adequate margin of surrounding normal tissue was applied, and the post-operative period was uneventful.
Keywords
Introduction
Deep fibromatoses, referred as “desmoid tumor” (DT) most commonly, are rapidly growing tumors often more aggressive than superficial fibromatoses and have a greater tendency to recur.1,2 The clinical behavior and natural history of DTs remain unpredictable and show individual variability ranging from being indolent and stable without any subsequent problem to the rapidly progressive and aggressive forms. 3 Therefore, despite the apparently benign histologic appearance of DTs, the likelihood of their biologic behavior to be rather “malignant” 4 caused them to be considered as malignant tumors with a propensity for local invasion and recurrence and minimal metastatic potential. 5
Occurring from puberty until the age of 40 and more frequently in women,1,2 DTs account for 0.03% of all neoplasms and less than 3% of all soft tissue tumours, 6 with an estimated incidence of two to four million of population per year in the general population. 7 DTs may arise in the abdominal wall (25%) or abdominal cavity (15%) or at extra-abdominal locations (60%), 8 and the tumor location was shown as a prognostic factor 9 with poorer prognosis in case of extra-abdominal locations while abdominal DT has been indicated to frequently cause an inconvenient diagnostic and therapeutic problem because of the difficult and rare localization of an expansive lesion. 2
Although the etiology of DTs has not yet been clarified, pregnancy and surgical scars are considered in the etiology 8 with a strong association reported between DTs and endogenous estrogen level in females.10,11 Most anterior abdominal wall DTs occur in women in their reproductive years, especially during a pregnancy or post-partum, whereas spontaneous regression has been associated with menopause or oophorectomy in women, suggesting a relationship between DTs and estrogens.3,8
In this regard, herein we present development of DT in a female patient following cesarean delivery, which manifested itself with a growing mass in anterior abdominal wall not during pregnancy but under a relatively hormone-free period such as puerperium. Written consent was obtained from the patient to reproduce information or photographs appearing in this work.
Case
A 35-year-old woman (gravida 2, para 2), who gave birth by cesarean section and had uneventful antenatal follow-up period, intraoperative and postnatal period, presented with a feeling of swelling in abdominal wall during the puerperium period, three weeks later following the delivery. On physical examination, a mass of almost 5–6 cm in diameter was palpated on lower anterior abdominal wall between anterior superior iliac spine and umbilicus (Fig. 1). Trans-abdominal ultrasonography revealed an isoechoic mass with well-defined borders. Possibility of hematoma most probably located beneath the fascia was considered as a complication of cesarean section, and the patient was informed about the natural clinical course of hematoma which shows spontaneous regression with eventual diminish in size and resolve of symptoms. However, after six weeks, the patient was admitted to our clinic again upon increase in the size of the mass. Ultrasonography performed by a superficial transducer revealed an isoechoic 10 × 5 cm-sized mass with a well-defined border, while vascular flow inside the mass with low resistance index was observed during Doppler ultrasonography. Magnetic resonance imaging was planned to make differential diagnosis considering an organized hematoma or a soft tissue tumor. Upon detection of a solid 10 × 5 cm-sized tumor located inside the rectus muscle sheath via MRI (Fig. 2A and B), tru-cut biopsy was suggested which revealed the pathological diagnosis of DT. General surgery team excised the tumor widely by involving approximately 3 cm of peripheral normal tissue. The large defect in abdominal wall was repaired with a mesh of 15 × 20 cm in size. The mass weighed 420 g and sized 26 × 12 × 6.5 cm (Fig. 3). The final pathologic examination of the mass revealed the diagnosis of desmoid fibromatosis. Surgical margins were free of tumor, and immunohistochemical analysis revealed that the tumor was CD34 (–), CD117 (–), Ki-67 (+) <1%, Smooth muscle actin (SMA) (–), and Caldesmon (–). Post-operative period was uneventful, and the patient was referred to oncology department following pathological diagnosis of desmoid fibromatosis.

Finding of a palpable mass in abdominal physical examination.

MRI findings of a solid 10 × 5 cm sized tumor
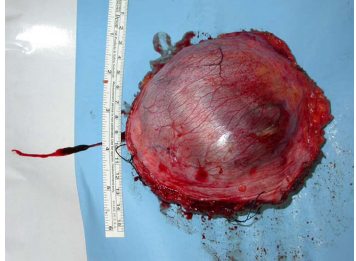
Resected mass.
Discussion
The probable role of hormones in the natural history of DTs is well known with a 33% incidence of estrogen receptor positivity, 12 while hormone-related proliferation of fibroblasts and smooth muscle cells has been shown to be very rapid in early pregnancy and decreases progressively thereafter. 13 Moreover, the dramatic response occasionally obtained with hormonal manipulation of these tumors suggests that many DTs show hormonal dependence and treatment of inoperable or recurrent tumors. 11
The present case report signifies the likelihood of manifestation of a DT as a growing mass in anterior abdominal wall in the post-partum period, following cesarean delivery in a female patient. This can be a unique example in which pregnancy triggers the initial development, while the subsequent growth occurs under relatively hormone-free period such as puerperium.
Clinical management of patients with DTs is challenging, and many issues remain controversial, mainly regarding early detection; the role, type, and timing of surgery; and the value of non-operative therapies. 3
Although considered non-malignant because of their inability to metastasize, DTs are associated with locoregional aggressiveness and high recurrence rate after resection. 9 Hence, in relation to the favorable outcome in DTs with long survival and no metastases 14 along with about 50% of recurrences and the likelihood of accelerating the evolution of the disease, the value of surgery as the mainstay in initial management is under debate 9 with adoption of a wait-and-see policy as initial strategy for some selected patients by several physicians.9,14
Nonetheless, different prognostic subgroups of DTs have been suggested that could benefit from different therapeutic strategies. 9 Ideally, the resection of abdominal wall DTs has been recommended ideally before the tumor becomes large to prevent large soft tissue defects leading the reconstruction of the abdominal wall to be complicated and technically demanding. 3 However, in contrast to abdominal wall desmoids, surgery for intra-abdominal DTs has been considered much more dangerous and is associated with increased morbidity and mortality, mainly because of hemorrhagic complications or extensive enterectomy requiring long-term parenteral nutrition. 3
In this regard, excision of the tumor widely by involving approximately 3 cm of peripheral normal tissue and thence repair of the large defect in abdominal wall with a mesh 15 × 20 cm in size in our patient is consistent with the statement that every effort must be made during the first operation to eradicate all known disease 5 and radical tumor extirpation with resection of an adequate margin of surrounding normal tissue remains the best treatment for DTs. 11
The growth patterns related to DTs clearly evidenced an active phase of tumor development lasting approximately three years, followed by tumor stabilization or regression. 14 While having no metastatic potential, DTs have been considered to behave quite aggressive locally, growing in size and infiltrating surrounding structures which thereby emphasizes the need for a close surveillance of these patients.3,11
Accordingly, consistent with a high local recurrence rate of DT which necessitates regular clinical follow-up in the routine clinical management of these tumors, the histologic features and the widespread and the unfavorable location of the lesion supported the decision to monitor the DT closely with the patient to be examined clinically every month and the tumor to be carefully measured every two months by ultrasonography. Local spread of the tumor was unchanged on the post-operative sixth month.
Differential diagnosis of abdominal DTs has been rather challenging, especially if the tumor is not in the typical anterior pre-peritoneal location with consideration of lymphoma, metastases, neoplastic process originating from the gastrointestinal tract and even a hematoma in the differential diagnosis. 2
In our case, possibility of hematoma most probably located beneath the fascia was considered initially as a complication of cesarean section based on ultrasonographic examination and location of the lesion, and further investigation leading to the diagnosis of DT was performed upon lack of either spontaneous regression with eventual diminish in size or resolve of symptoms. Similar to our findings, in a 43-year-old male who had an abdominal injury because of a bicycle accident, while a hematoma in the right retroperitoneum was considered initially based on acutely performed CT scan, application of MRI upon no change in the findings of an expansive lesion of the retroperitoneum for many days following the injury revealed an expansive lesion of unclear etiology, histological diagnosis of which was a typical intra-abdominal DT. 2
Hence it seems reasonable to assume that, while DTs are unlikely to be misdiagnosed as hematomas given that they do not eventually resolve unlike to hematomas, their diagnosis can be clarified via further imaging with CT or MRI and may become apparent with clinical follow-up of a performed biopsy if necessary; the consideration of hematoma by physician seems more likely in cases with history of recent surgical operation. Nevertheless, given the distinct clinical course of two conditions that lead to the eventual appearance of clinical signs indicative of DT in a patient initially considered as hematoma, misdiagnosis of a DT as a hematoma in patients with recent surgical operation seems to be a clinical entity without substantial impact on the outcome of patients.
Although spontaneous evolution of DTs sometimes shows progressive shrinking of the tumor after the initial growth, 11 in our patient initial growth was followed by an increase in mass within six weeks. Our findings emphasize that for establishment of the accurate diagnosis of DTs, as much clinical data as possible should be available including the use of advanced imaging methods with consideration of abdominal DT particularly in younger individuals with rapidly growing tumorous process located in the abdominal wall or in the abdominal cavity, whereas afterward, biopsy or the histological examination of the operatively dissected material remains as the only method of exact diagnosis. 2
In conclusion, based on the manifestation of a DT as a growing mass in anterior abdominal wall in the post-partum period in the present case which is initially considered as hematoma, our findings emphasize the importance of the availability of as much clinical data as possible for the accurate diagnosis of DTs and support that the radical tumor extirpation with resection of an adequate margin of surrounding normal tissue remains the best treatment for abdominal wall DTs. Given that the main difficulty in managing DTs is that they are histologically benign tumors that however show a high propensity for local recurrence and high ability to recur after initial treatment,3,9 while the available data are mostly based on small case series, 3 future randomized clinical trials are needed to clarify unclear issues regarding the ideal management of DTs with respect to histological characteristics and clinical behavior.
Author Contributions
Conceived and designed the experiments: EG. Analyzed the data: NG. Wrote the first draft of the manuscript: IC. Contributed to the writing of the manuscript: OK. Agree with manuscript results and conclusions: IB. Jointly developed the structure and arguments for the paper: AS. Made critical revisions and approved final version: AG. All authors reviewed and approved of the final manuscript.
Disclosures and Ethics
As a requirement of publication the authors have provided signed confirmation of their compliance with ethical and legal obligations including but not limited to compliance with ICMJE authorship and competing interests guidelines, that the article is neither under consideration for publication nor published elsewhere, of their compliance with legal and ethical guidelines concerning human and animal research participants (if applicable), and that permission has been obtained for reproduction of any copyrighted material. This article was subject to blind, independent, expert peer review. The reviewers reported no competing interests.
