Abstract
Background
Comprehensive treatment and clinical management are central to improving outcomes for people living with HIV (PLHIV). We explored trends in HIV clinical care, treatment outcomes, and chronic kidney disease (CKD) and diabetes monitoring.
Methods
We included patients ≥18 years in care at ten clinical sites in eight Asian countries. Proportions of patients on antiretroviral therapy (ART), with annual viral load, and with viral load suppression (VLS; <1,000 copies/ml) were estimated by year for 2011– 2016, stratified by country income level (lower-middle income [LMIC] and high-income countries [HIC]). Among those on ART in 2016 we evaluated factors associated with annual CKD and diabetes monitoring.
Results
Among 31,346 patients (67% male), the proportions of patients on ART (median ART initiation year 2011, IQR 2007–2013), with annual viral load and VLS had substantially increased by 2016 (to 94%, 42% and 92%, respectively, in LMIC and 95%, 97% and 93%, respectively, in HIC) with the larger increases over time seen in LMIC. Among those on ART in 2016, monitoring proportions in LMIC were 53% for CKD and 26% for diabetes compared with 83% and 59%, respectively, in HIC. Overall, a decreased odds of monitoring was observed for male gender, heterosexual HIV exposure, no viral load and LMIC. Diabetes monitoring was also decreased in those with viral failure.
Conclusions
Our findings highlight suboptimal monitoring of viral load, CKD and diabetes in PLHIV in Asia. There is a need for affordable and scalable monitoring options to improve the joint care for HIV and non-communicable diseases.
Introduction
Goals in the fight against HIV have transformed over time in line with the changing epidemic and improved treatment options. Following the scale up of effective antiretroviral therapy (ART), the current focus is on ending AIDS as a public health threat [1], which entails reducing the global HIV incidence to 200,000 or fewer new cases a year [2]. Landmark studies have shown that ART initiation in earlier stages of HIV infection, before CD4 counts have severely deteriorated, is associated with decreased HIV-related morbidity and mortality [3–5] and that viral load suppression (VLS) through effective ART prevents HIV transmission to others [6,7]. Ongoing virological failure (VF) can contribute to emerging drug resistance, thereby complicating treatment options at both an individual and public health level [8,9]. Following this evidence, key efforts are aimed at improving linkage and retention in care so that people living with HIV (PLHIV) can be started on ART as soon as possible, and achieve sustained VLS [1,2].
The HIV care cascade has gained attention to quantify population level engagement in care and to identify gaps in care that may contribute to unfavourable health outcomes. The care cascade shows a variety of steps typically starting with the total estimated number of PLHIV in a region and with subsequent steps representing proportions of PLHIV diagnosed, linked to care, started on ART, retained in care, tested on viral load and having achieved VLS. Virally suppressed PLHIV may still experience a range of other poor health outcomes, including non-communicable diseases (NCDs), such as chronic kidney disease (CKD) and diabetes [10,11]. In line with this, it has been argued that VLS should not be the ultimate goal of HIV care [12] and the HIV treatment cascade should be extended to include monitoring and management of NCDs [13].
Latest HIV treatment guidelines recommend screening PLHIV for serum creatinine (S-Cr), a marker for kidney function, and blood glucose, a marker of diabetes, before ART initiation and at least annually thereafter [14]. Furthermore, the guidelines suggest assessing viral load every 3 to 4 months, although less frequent monitoring can be considered if patients have sustained VLS for 2 or more years [14]. Adequate laboratory monitoring of PLHIV may be particularly challenging in regions with overburdened and under resourced health systems, such as Asia Pacific [15]. Improved knowledge on HIV-related care, including monitoring practices of viral loads and NCDs, is required to advance overall health outcomes in PLHIV. The current study investigated the extended treatment cascade in The TREAT Asia HIV Observational Database Low Intensity TransfEr (TAHODLITE), a multi-country clinical cohort of PLHIV in Asia which comprises treatment data on all patients in care at participating sites. We assessed proportions on ART, with annual viral load monitoring and VLS in those attending care between 2011–2016 in this cohort. We further investigated S-Cr and fasting plasma glucose (FPG) monitoring among PLHIV in our cohort in 2016 and their prevalence of CKD and diabetes.
Methods
TAHOD-LITE is a sub-study of the TREAT Asia HIV Observational Database (TAHOD), a prospective observational cohort of the International epidemiology Databases to Evaluate AIDS (IeDEA). TAHOD and TAHOD-LITE have been described in more detail elsewhere [16,17]. The 2017 TAHOD-LITE data transfer collected data on demographics, hepatitis serology, ART history, HIV-related laboratory results, S-Cr and FPG from all PLHIV aged ≥18 years under care at clinical sites in Cambodia (1 site), Hong Kong (1 site), India (2 sites), Indonesia (1 site), Singapore (1 site), South Korea (1 site), Taiwan (1 site) and Vietnam (2 sites). Institutional Review Board approvals were obtained at all participating sites, the data management and analysis centre (The Kirby Institute, UNSW Sydney, Australia), and the coordinating centre (TREAT Asia/ amfAR, Bangkok, Thailand).
For the current study, we included adults (aged ≥18 years at enrolment) who received care at one of the participating sites anytime between January 2011 and December 2016. This timeframe was decided on as 2010 World Health Organization (WHO) guidelines suggested phasing in of viral load testing and a scale-up of viral load testing was thus expected from 2011 onwards [18]. Proportions on ART, with annual viral load monitoring and VLS were estimated from 1 January to 31 December for each year. We excluded patients who attended a site only once and were immediately transferred out for their care at a regional clinic. For evaluation of S-Cr and FPG monitoring the study population was restricted to those patients who had attended the clinical site in 2016. To prevent underestimation of annual monitoring, we assessed laboratory testing in the last 13 months of clinical follow-up, accounting for clinical appointments falling just outside the annual time frame or potential missed visits. We thus excluded patients who had last visited the clinic before 2016 and those who had been retained in clinical care for less than 13 months.
Study definitions
Patients were considered to be in care for each calendar year after enrolment if there was a lack of documented death, or loss to follow up (LTFU; defined as not being seen at the clinic >12 months after their last clinic visit or reported as LTFU by clinical site). In case of death or LTFU patients were considered in care for the year in which their last clinic visit took place, but not the year thereafter. Patients were considered on ART if they were started on any regimen of ART, regardless of the number or type of antiretroviral drugs prescribed, and clinic data did not reveal discontinuation of ART. Patients were considered to have been monitored for treatment failure, kidney function and diabetes if they had received at least one viral load test, S-Cr test or FPG test during follow-up. In line with WHO guidelines [19], VLS was defined as a viral load of <1,000 copies/ml. If patients had a viral load ≥1,000 copies/ml, they were considered to have VF. CKD was defined as having an estimated glomerular filtration rate (eGFR) of <60 ml/min/1.73 m2 based on S-Cr assessment and as calculated by the CKD-EPI equation [20]. Diabetes was defined as having an FPG ≥126 mg/dl, in accordance with guidelines of the American Diabetes Association [21].
ART use, viral load monitoring and VLS
Proportions of patients in care, on ART, with evidence of viral load monitoring and with VLS were presented by year for the period 2011 to 2016. Kaplan-Meier (K-M) curves were used to plot time to ART initiation for all newly enrolled patients who were ART-naive at baseline and were compared across calendar year of enrolment using log-rank test. In addition, K-M estimates with 95% confidence intervals (95% CI) were used to evaluate the probability of these patients starting ART by calendar year of enrolment. Proportions, K-M curves and K-M estimates were all stratified by country-income category (lower-middle-income country [LMIC] versus high-income country [HIC]).
Monitoring for kidney function and diabetes
We presented proportions with 95% CI of annual S-Cr and FPG monitoring and the prevalence of CKD and diabetes in those who had attended care in 2016, stratified by country-income category. Furthermore, we fit multivariable logistic regression models to estimate the associations between several covariates and having received annual monitoring for S-Cr and for FPG. Both models incorporated the following a priori chosen variables: sex, age (≤40, 41-50 or >50), HIV exposure category (that is, through heterosexual contact, male-to-male sexual contact, through injecting drug use, or other/unknown), pre-ART CD4+ T-cell count (<200, 200-349, ≥350 cells/μl or missing), by viral load status (VLS, VF or viral load not tested) and by country income category (LMIC or HIC). Associations were considered statistically significant at P<0.05.
Data management and statistical analyses were performed using SAS software version 9.4 (SAS Institute Inc., Cary, NC, USA) and Stata software version 14.1 (StataCorp, College Station, TX, USA).
Results
Between 2011 and 2016, a total of 32,734 patients were in care at the participating sites. We excluded 1,388 patients who were documented as clinic transfers. Characteristics of the remaining 31,346 patients included in this study are outlined in Table 1. The majority of patients attended clinics in India (61%), followed by Singapore (9%), Cambodia (8%), Vietnam (7%), Indonesia (6%), Hong Kong (4%), Taiwan (2%) and South Korea (2%). Median age at clinic enrolment was 36 (IQR 30–43) years and 20,853 (67%) patients were male. Median pre-ART HIV viral load was log10 5.0 (IQR 4.5–5.6) copies/ml and median pre-ART CD4+ T-cell count was 168 (IQR 63–280) cells/μl. Median ART initiation year was 2011 (IQR 2007–2013).
Characteristics of patients in care between 2011 and 2016 (n=31,346)

HBV and HCV coinfection based on ever having had positive hepatitis B surface antigen (HBsAg) and anti-HCV test, respectively. ART, antiretroviral therapy; IDU, injecting drug use; MSM, men who have sex with men.
ART use, viral load monitoring and VLS
Figure 1 shows the number of patients in care and the proportions of those on ART, with evidence of viral load monitoring and with VLS. The total number of patients in care varied: 18,387 in 2011, 19,586 in 2012, 20,263 in 2013, 20,566 in 2014, 20,150 in 2015 and 19,580 in 2016, with the reduction in patient numbers after 2014 mainly caused by a decreasing rate of new enrolment in this period. For each year, the proportions of patients on ART, with evidence of viral load monitoring and with VLS were higher in HIC, however, the increase over time was substantially higher in LMIC. In LMIC, the proportion of patients in care who were on ART increased from 78% in 2011 to 94% in 2016, whereas in HIC, the proportion increased from 82% in 2011 to 96% in 2016. Although viral load monitoring among those on ART increased over time regardless of country income category, in 2016, 42% of patients had received a viral load test in LMIC (increased from 13% in 2011) versus 97% in HIC (increased from 90%). Of those who had received a viral load test in 2016, 92% had achieved VLS in LMIC (increased from 67% in 2011), while 93% had achieved VLS in HIC (increased from 89% in 2011). Among patients who did not receive a viral load test in a specific year, up to 19% became LTFU and around 1% died within that same year.
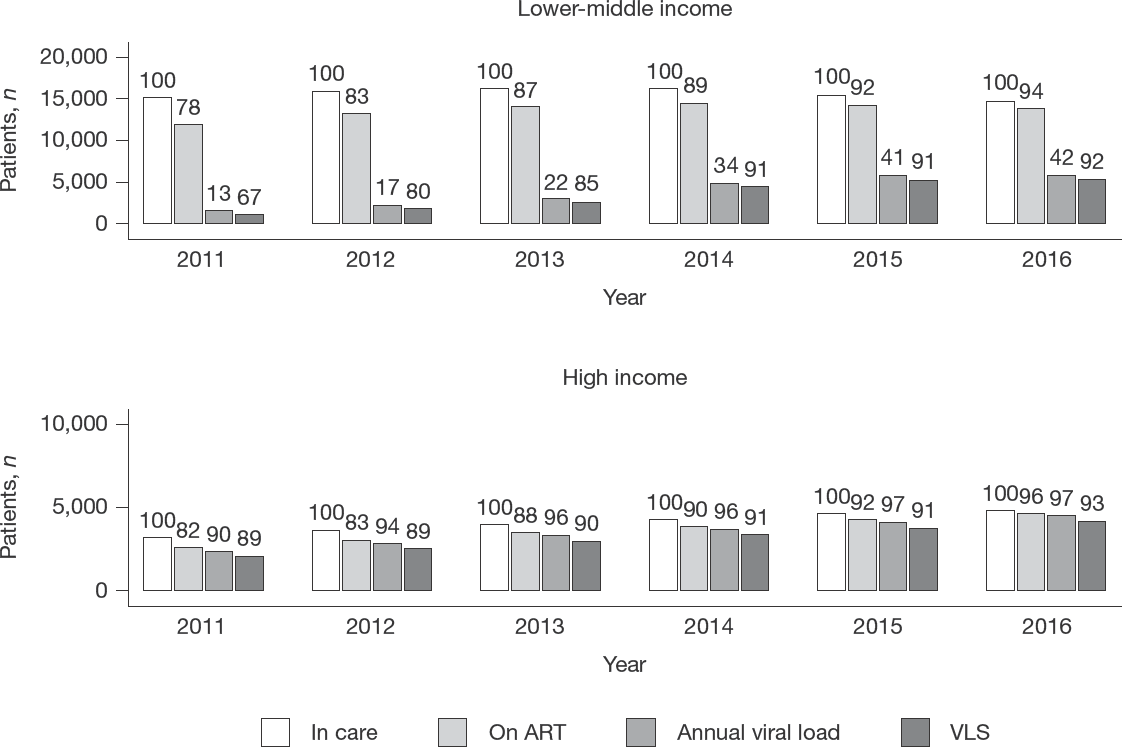
Patients in care, on ART, with annual viral load and viral load suppression from 2011 to 2016, by country income category
Between 2011–2016, 10,382 patients were newly enrolled into care, of whom 8,357 (80%) in LMIC and 2025 (20%) in HIC. The K-M curves show differences in time to ART initiation by year of clinic enrolment (log-rank P<0.001), where the curve was lowest for enrolment in 2015, in LMIC as well as HIC (Figure 2). According to K-M estimates, the probability of ART initiation within 1 month after enrolment increased over time. In LMIC, the probability increased from 45% (95% CI 43, 48%) in 2011 to 63% (95% CI 60, 66%) in 2015, whereas in high income countries, the probability increased 42% (95% CI 38, 47%) in 2011 to 68% (95% CI 63, 72%) in 2015.

Kaplan–Meier curves of time to ART initiation in lower-middle-income and high-income countries, by year of enrolment
Monitoring for kidney function and diabetes
S-Cr and FPG monitoring was assessed in the 16,641 patients who were on ART in 2016 and who were retained in care for at least 13 months. In LMIC, S-Cr and FPG were tested in 53% and 26% of the patients, respectively, while in HIC, the proportion of patients tested was substantially higher at 83% and 59%, respectively. The prevalence of CKD and diabetes in the patients who had been monitored for these conditions was 14% and 36%, respectively, in LMIC, compared with 8% and 17%, respectively, in HIC (Figure 3).
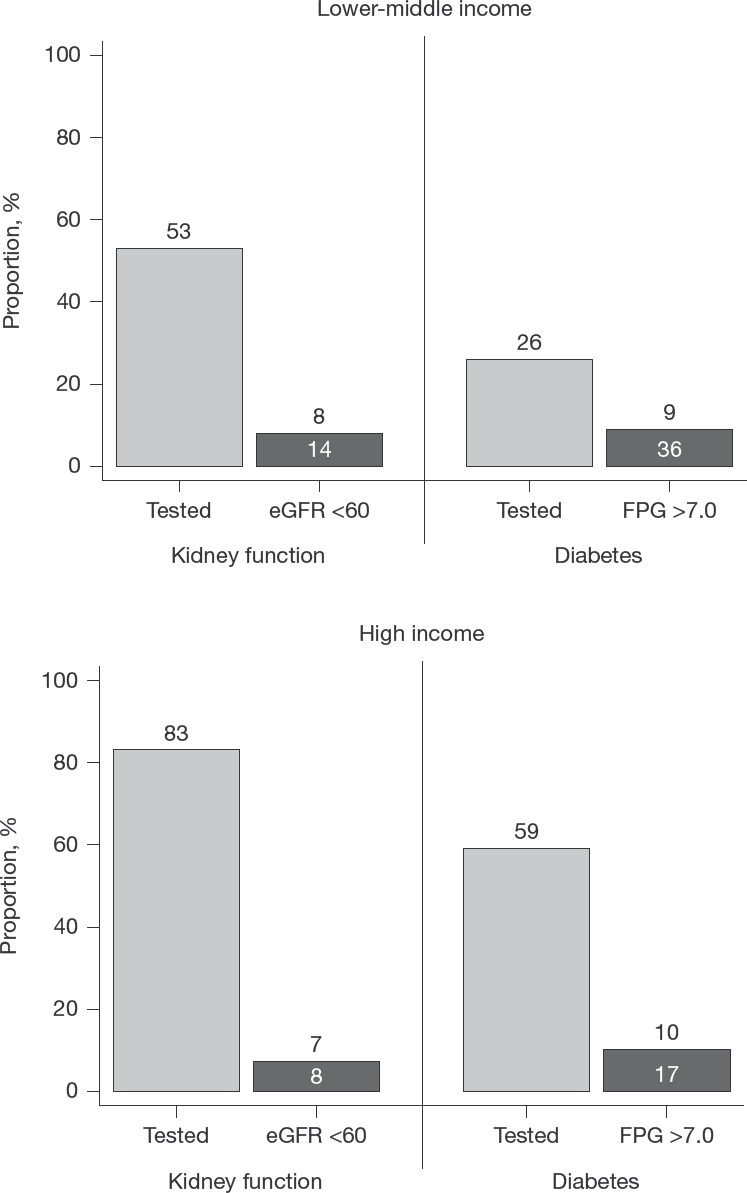
Kidney function and diabetes monitoring in patients in care in 2016, by country income
Table 2 shows the multivariable regression model for factors associated with S-Cr monitoring and with FPG monitoring. An increased odds of S-Cr monitoring was observed in those with HIV exposure through injecting drug use (odds ratio [OR] 6.15, 95% CI 5.01, 7.54, compared with heterosexual HIV exposure) and in HIC (OR 7.13, 95% CI 6.27, 8.09, compared with LMIC), while S-Cr monitoring was decreased in males (OR 0.82, 95% CI 0.76, 0.89), those with a pre-ART CD4+ T-cell count of 200–349 (OR 0.86, 95% CI 0.76, 0.98 compared with ≥350 cells/ml), and those who did not have a viral load assessment (OR 0.88, 95% CI 0.81, 0.95, compared with those with VLS). FPG monitoring was increased in those with HIV exposure through injecting drug use (OR 4.05, 95% CI 3.41, 4.81) and male-to-male sex (OR 1.66, 95% CI 1.47, 1.87, compared with HIV exposure through heterosexual contact) and in HIC (OR 5.06, 95% CI 4.52, 5.67). FPG monitoring was decreased in males (OR 0.82, 95% CI 0.75, 0.89), and those who did not have a viral load assessment (OR 0.55, 95% CI 0.51, 0.60) or those who had VF (OR 0.67, 95% CI 0.58, 0.77 compared with those with VLS). The proportion of patients monitored for S-CR and FPG was higher in older age groups, however, age was not independently associated with either S-Cr or FPG monitoring.
Multivariate analysis of having received serum creatinine and fasting plasma glucose testing among patients on ART and in care in 2016

Age is age in year of serum creatinine or fasting plasma glucose test. P-values in bold represent significant covariates. a P-values for test for heterogeneity excluded other/unknown or missing/not-tested values. IDU, injecting drug use; MSM, men who have sex with men; OR, odds ratio; VF, virological failure (≥1,000 copies/ml); VLS, viral load suppression (<1,000 copies/ml).
Discussion
Our findings demonstrated improvements in treatment uptake, viral load monitoring and viral load suppression in the TAHOD-LITE cohort. Specifically, we observed that ART uptake during the period of 2011 to 2016 had increased from 78% to 94% in LMIC and from 82% to 97% in HIC. Our findings also showed higher probabilities of ART initiation within 1 month after clinic enrolment in later calendar years, regardless of country income. The trends of improved ART uptake are most likely attributable to the global efforts to expand ART access and to the changing HIV treatment guidelines where ART eligibility criteria have been updated with recommendations to initiate ART in PLHIV who present to care with less advanced HIV disease [19]. Furthermore, among the patients in our cohort who were on ART and received annual viral load testing, proportions of VLS increased to over 90% in both LMIC and HIC. VLS in those who have evidence of viral load monitoring may not refect VLS in all of those on ART and, thus, caution is warranted when making inferences about progress on population-level VLS. Still, increasing proportions of VLS are apparent in other data from the region as well [22] and it is possible that this development represents advancements in clinical management of HIV.
After PLHIV have started ART, viral load testing is considered the gold standard to detect treatment failure. Routine viral load monitoring has therefore been recommended by WHO and most national HIV treatment guidelines, however, implementation of routine viral load monitoring has proven challenging for the majority of LMIC [18,19,23]. A lack of routine viral load monitoring was observed in LMIC in our cohort as well, although the proportion of patients with viral load monitoring did triple from 2011 to 2016. Among those without a viral load test in any year, a relatively high proportion of patients were LTFU or died (up to 20% attrition in each observed calendar year), and it may be that some of these patients would have received a viral load test had they remained in care. Regardless, viral load testing was less than annual in at least half of the patients from LMIC in our cohort, suggesting that routine viral load monitoring in this setting remained suboptimal even in the later years of the study period. Findings from Myanmar showed that viral load testing remained suboptimal after the national implementation of routine VL monitoring in 2017, with less than 60% of patients having received a viral load test up to 2 years later [24]. As far as we are aware, no other data has yet been published on routine viral load monitoring after 2016 in Asia.
Monitoring for kidney function and diabetes by means of S-Cr and FPG testing had not occurred on an annual basis for many of the patients in our cohort. Among those on ART in 2016, S-Cr testing was received by 53% in LMIC and 83% in HIC, while FPG testing was received by only 26% in LMIC and 59% in HIC, in their last year of follow-up. The higher proportion of S-Cr testing compared with FPG testing may be a refection of HIV treatment guidelines as these recommend biannual testing of kidney function, but annual testing for diabetes [14]. Moreover, wide-scale testing of kidney function may be more common than diabetes testing because of the potential nephrotoxic effects of tenofovir disoproxil fumarate (TDF) [25]. TDF is widely prescribed in the Asian region as part of the preferred first-line regimen in countries with a high HIV burden [26], while it is also the treatment of choice for chronic hepatitis B [27].
Among the patients on ART who had received monitoring, the observed prevalence of CKD and diabetes was 14% and 36%, respectively, in LMIC compared with 8% and 17%, respectively, in HIC. As the proportion of patients who had received an annual S-Cr or FPG test was relatively low, especially in LMIC, it is possible that our findings are not an accurate estimate of the prevalence of CKD and diabetes in the study population. Still, regardless of country income, the prevalence we observed for these conditions is largely in the range of what has been found in other studies from the Asian region, which have reported CKD in 7% to 20% and diabetes in 5% to 27% of PLHIV [28–34]. Furthermore, the finding that the prevalence of both of these NCDs was higher in LMIC than in HIC refects what has been observed in the general population [35,36].
As our cohort is observational in nature, monitoring for kidney function and diabetes is according to local standards and may be based by clinicians’ decision to perform and patient willingness to receive testing. Our findings showed that monitoring was more common in females than males. Literature from the region suggests that men have poorer health seeking behaviour [37] and women may be more willing to receive monitoring for comorbidities. Furthermore, being monitored was more common in those with HIV exposure through male-to-male sexual contact or injecting drug use. Possibly, clinicians prioritise testing key populations as they may be suspected to exhibit risk behaviours, such as illicit drug use, which put them at greater risk of developing CKD and diabetes [38–40].
Clinicians may be more likely to perform routine monitoring of NCDs in patients who are considered stable in terms of HIV disease. In our cohort, S-Cr and FPG monitoring was increased in those with VLS compared with those with VF, although the association with S-Cr monitoring did not reach statistical significance. We also observed that proportions of S-Cr and FPG monitoring were higher in those with a pre-ART CD4+ T-cell count >350 cells/ml compared with those with lower CD4+ T-cell counts. However, multivariate analysis showed that only those with a pre-ART CD4+ T-cell count of 200–349 cells/ml, but not those with a pre-ART CD4+ T-cell count below 200 cells/ml, were significantly less likely to receive S-Cr monitoring than those who started ART with a higher CD4+ T-cell count. Literature shows that low pre-ART CD4+ T-cell counts and ongoing VF are associated with poor clinical outcomes [41,42]. It is possible that in patients who present to care with more advanced HIV disease and those who have adherence issues or treatment failure, the priority lies in improving primary HIV outcomes, such as immunological recovery and preventing or managing AIDS-related morbidity [43].
Modelling studies have estimated a growing burden of comorbid NCDs in PLHIV [44,45]. The low proportion of patients with S-Cr and FPG monitoring in our cohort can therefore be considered a cause for concern. It is likely that a lack of resources hinders routine testing for CKD and diabetes. Supporting this notion, our findings showed that patients in LMIC in our cohort were over 5 times less likely to have received S-CR and FPG testing. Furthermore, testing for diabetes and kidney function was decreased in those who had not received an annual viral load test, which may imply that S-Cr and FPG monitoring is more likely in patients who have access to viral load monitoring as well. Main barriers to routine laboratory monitoring in resource-limited settings include costs of testing and associated infrastructural needs [46,47]. Such barriers need to be addressed in order to increase access to laboratory monitoring and thereby adequately prevent and manage NCDs in addition to assessing treatment failure in PLHIV on ART.
Over the last few years, an approach of differentiated care delivery has been promoted to increase appropriate routine laboratory monitoring and improve quality of care for PLHIV [48]. The rationale behind this approach is that differentiating care provision according to individual patient needs can reduce attrition and thereby improve health outcomes [48,49]. For example, patients who have achieved sustained VLS are considered stable on ART and care for them may be tailored by minimizing follow-up visits and providing them with ART prescriptions for longer periods of time. By contrast, patients who have been identified as having issues with adherence, treatment or overall health can continue to receive more intensive care with clinic contact as needed. Apart from having the potential to improve health outcomes in those attending care, this tailored approach can also save costs and enable more effective allocation of resources, making it a particularly useful approach for resource-limited settings with strained health systems [50]. Although differentiated care is currently mainly used in the context of viral load monitoring, expanding this approach to integrate care for NCD may improve quality of care and health outcomes of a wider scope.
Our study has several limitations that should be noted. Our findings are from ten sites in eight countries and territories and may not be representative of HIV-related care in the wider Asia–Pacific region. Related to this, over 60% of patients in our cohort were from sites in India. It should be noted that with an estimated 2.1 million PLHIV, India has the largest population of PLHIV in Asia [51] and is considered the focal point of the HIV burden in the region. Furthermore, definitions for CKD and diabetes differ across literature. Various markers have been used to diagnose the conditions and often diagnosis is confirmed by a second assessment taken at a later point in time [21,28–30]. We based the prevalence of CKD and diabetes on single assessments of S-Cr and FPG, respectively, because of the low number of patients with multiple assessments a year. Furthermore, it may be possible that there are different methods of monitoring kidney function and diabetes, for example urine dipstick and Hb1Ac tests. However, other markers of kidney function and diabetes were not included for data collection as S-Cr and FPG were by far the most commonly available laboratory test results in the clinics participating in TAHOD-LITE.
In summary, our study illustrates an increase in the proportion of patients on ART and a decrease in time to treatment initiation across selected clinical sites in Asia between 2011 to 2016. Concerningly, we also found critical gaps in viral load testing and monitoring of S-Cr and FPG, especially in LMIC. Due to plateauing funding for HIV care in more recent years, it may be unrealistic to expect optimal monitoring practices, especially in clinics with limited resource availability. There is a need for affordable and scalable diagnostic testing and monitoring testing options to better evaluate NCDs among people living with HIV in the Asia–Pacific region.
Footnotes
Acknowledgements
The TREAT Asia HIV Observational Database Low-Intensity TransfEr study is an initiative of TREAT Asia, a programme of amfAR, The Foundation for AIDS Research, with support from the US National Institutes of Health's National Institute of Allergy and Infectious Diseases, the Eunice Kennedy Shriver National Institute of Child Health and Human Development, the National Cancer Institute, the National Institute of Mental Health, the National Institute on Drug Abuse, the National Heart, Lung, and Blood Institute, the National Institute on Alcohol Abuse and Alcoholism, the National Institute of Diabetes and Digestive and Kidney Diseases, and the Fogarty International Center, as part of the International Epidemiology Databases to Evaluate AIDS (IeDEA; U01AI069907). The Kirby Institute is funded by the Australian Government Department of Health and Ageing, and is affiliated with the Faculty of Medicine, UNSW Sydney. The PhD of R Bijker has been supported through an Australian Government Research Training Program Scholarship. The content of this publication is solely the responsibility of the authors and does not necessarily represent the official views of any of the governments or institutions mentioned above. Supplementary acknowledgements can be found in Additional file 1.
The authors declare no competing interests.
