Abstract
BACKGROUND:
Previous studies have shown high rates (47–72%) of self-reported work-related musculoskeletal disorders (WRMDs) in surgeons of the head and neck. Physical requirements in the workplace, individual factors (e.g. poor posture, obesity) and psychosocial factors have been identified as risk factors. Establishing biomechanical risk factors may help prevent further development of WRMDs in this population.
OBJECTIVE:
The purpose of this critical review was to source studies that identified the biomechanical risk factors for WRMDs in this surgical sub-specialty.
METHODS:
Searches were conducted of Medline, CINAHL, and AMED databases from 1980 until September 2018.
RESULTS:
A total of 182 article were identified. Exclusion criteria lead to 163 full-text articles being screened, generating a total of 6 articles for review. The aims of the included studies varied significantly. Surgeons spend the majority of operating time in static, asymmetrical positions. Surgical loupes/headlamps significantly increased cervical spine loading. Articulated surgical arm supports provided optimal ergonomic conditions. Performing surgical operations with the surgeon in standing or sitting had no effect on task performance or demand. Physical fatigue was also measured in both positions.
CONCLUSIONS:
A combination of equipment-based and patient/surgeon position-based factors predispose surgeons to biomechanical risk factors. Studies of greater methodological quality are required.
Introduction
Musculoskeletal disorders are a heterogenous collection of over 150 inflammatory and degenerative conditions that affect the muscles, bones, nerves, tendons, and ligaments [1, 2]. Worked-related musculoskeletal disorders (WRMDs), refer to musculoskeletal injuries or disorders associated with occupational aetiologic factors [3]. WRMDs can be the result of one or cumulative microtrauma and can profoundly impact an individual’s quality of life [1, 4]. The World Health Organisation recognises that WRMDs are exacerbated by work-related conditions and activities and are multifactorial in nature [3, 5].
Although reports of WRMDs have been dated back to the 17th century, more recent epidemiological studies and meta-analyses have established WRMDs as a major public health problem, affecting people of all ages worldwide [1, 7]. In 2015/16, the economic burden of WRMDs in the United Kingdom (UK) was estimated to be $ 14.9 billion [8]. In 2016/17 507,000 workers in the UK were reported to be suffering from WRMDs; this accounted for 39%of all work-related ill-health and resulted in a loss of 8.9 million working days [8, 9]. Key risk factors for developing WRMDs include physical requirements in the workplace (e.g. prolonged static postures, work specific procedures, vibrating tools), individual factors (e.g. poor posture, obesity) and psychosocial factors (e.g. shift work, work-related stress) [2, 7]. While both sedentary and labour-intensive occupations have been identified as high-risk professions for the development of WRMDs, compelling evidence has suggested that surgeons also fall into that category with those operating on the head and neck susceptible to particular risk factors [4, 11].
Literature review
A recent meta-analysis by Epstein and colleagues [11] established high rates of WRMDs amongst ‘at-risk’ physicians, defined as medical interventionalists and surgeons. Twelve-month prevalence estimates of WRMDs of the neck, shoulder, back, and upper extremities reached 65%, 52%, 59%, 39%, respectively. These results are comparable to those in high-risk, labour-intensive occupations [11]. High-rates of burnout, depression and attrition were also reported amongst physicians, necessitating the demand for intervention [11]. A UK-based survey of 325 ear, nose, and throat (ENT) surgeons found that 72%had either back or neck pain, or both [12]. Of those in pain, 53%directly attributed their symptoms to their work. Mal and Costello [13] reported higher rates (24%) of shoulder impingement syndrome in otolaryngologists than endocrinologists in the UK. Vijendren et al. [14] surveyed 323 ENT surgeons, 47.4%of whom reported some form of WRMDs; most commonly affecting the neck and back. With the rise in the reporting of WRMDs in this surgical sub-specialty, the demand for intervention is growing [11].
Factors contributing to the development of WRMDs in ENT surgeons include long work hours, repetitive tasks, static and awkward intra-operative postures, and equipment design challenges [11, 16]. The use of microscopes, endoscopes, surgical loupes and headlamps have also been implicated in the development of WRMDs [14, 17].
Justification for critical review
The earlier review by Vijendren et al. [14] revealed only six articles worldwide reporting prevalence and effects of WRMDs on ENT surgeons. All studies were cross-sectional surveys and collectively reported a prevalence rate of WRMDs in 47 83%of respondents [14]. No literature reviews have been identified that have critically reviewed studies that have objectively measured the biomechanical risk factors of this surgical sub-specialty to elucidate the self-report data.
The aim of this review was to identify existing articles that have assessed work-related biomechanical risk factors in surgeons of the head and neck. Establishing which risk factors are leading to the prevalence of WRMDs in this population may provide insight into the design of future job design, interventions and research.
Methods
Research question
The Population, Intervention, Comparison, and Outcome (PICO) framework was used to formulate the research question: “what biomechanical risk factors are leading to WRMDs in surgeons of the head and neck?”.
Types of studies
The aim of this study was to identify articles that utilised quantitative methods. The Oxford Centre for Evidence-based Medicine classifies randomised controlled trials (RCTs) as one of the highest levels of evidence, however such trials are not always feasible in the context of evaluating surgical procedures [18]. As such, both RCTs and observational studies (cohort, case-control, and cross-sectional studies) were included. Epidemiologic and survey-based studies were excluded.
Types of participants
Any surgical sub-specialty that performs regular surgical operations on the head, neck or face was included. Participants of all ages and professional working years were included.
Types of outcome measures
Studies were included if their primary outcome measure was an instrument that would enable the analysis of posture, muscle activity, fatigue and discomfort. No inclusion/exclusion criteria were applied to secondary outcome measures.
Search method
A literature search was conducted using the ProQuest platform according to Prisma-P guidelines [20], searching the Research Library, Nursing and Allied Health, Physical Education Index and Health and Medical Collection databases. The EBSCO platform was used to search the Medline, CINAHL, and AMED databases. Publication date range limitations were set from 1980 until the date of the search, September 9th, 2018. The large date range accommodated for the scarcity of literature in this field.
An extensive search strategy was created by obtaining a list of surgical subspecialties from The Royal College of Surgeons website [21]. This was then explored for job titles and keywords that could be incorporated into a surgeon specialty-based search term. Keywords that were found through literature searching were also included. Two additional sets of keywords were created; one including musculoskeletal disorder-based keywords, and another including ergonomic measurement/ergonomic analysis-based keywords (Table 1).
Search Strategy
Search Strategy
These three sets of keywords were then applied using the selected databases on both ProQuest and EBSCO, separated by “AND”. When searching on the EBSCO platform, the keywords were only searched in “Anywhere except full text” to maximise the relevancy of the results. Search results were limited to full text and peer-reviewed publications, to ensure access to the complete article and to optimise methodological quality. Due to comprehension issues of the researcher, a language filter was applied to only include articles of the English language. Application of limiters generated a total of 182 records, with 31 and 151 results from ProQuest and EBSCO, respectively. Duplicates were removed manually from the two platforms (19 in total), generating 163 articles for screening. A total of 4 full-text articles were identified. A citation search was performed using the PubMed platform, for each of the 4 included studies. This was to find existing literature that had not been found using the search strategy and limiters. Two additional articles were found and included.
The PRISMA flow diagram of included and excluded articles can be found in Fig. 1. Excluded studies, with rationale, can be found in the Appendix.
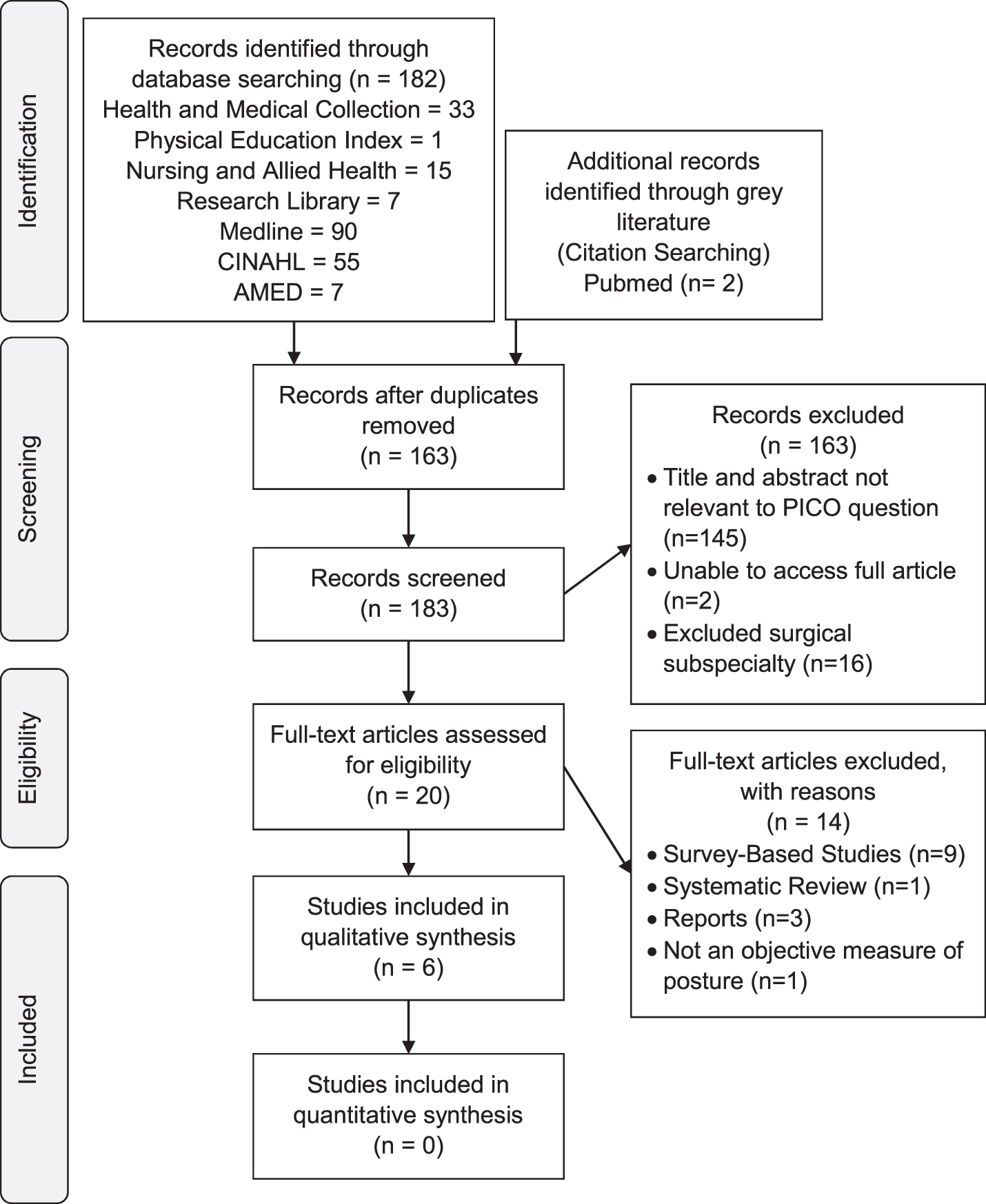
PRISMA Diagram.
Study quality
Six studies were included for appraisal, all of which were observational studies. They were appraised using the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement, which has been validated in the surgical research field [22, 23]. Three studies had a STROBE score of equal to or less than 20/35 [24, 27], and three had a score higher than 20/35 [25, 29] (Table 2), meeting between 49%–66%of the STROBE criteria. This suggests that the included articles are of a low to moderate level of quality.
Appraisal of Studies Using STROBE Checklist
1 Mean = 20.3±1.7 (Range = 17-23)
Appraisal of Studies Using STROBE Checklist
1 Mean = 20.3±1.7 (Range = 17-23)
The aims and results of the studies varied significantly (Table 3).
Summary of Included Studies
Summary of Included Studies
Sample sizes were small across all studies, ranging from 1–13 participants (Table 4).
Sample Size
Sample Size
Reporting of inclusion and exclusion criteria of participants was poor; no studies included eligibility criteria or recruitment strategies. Neither did they provide validation for their sample sizes. Descriptive data of study participants were universally lacking. Shaw et al. [27] were the only ones who provided the mean age of participants. While older age has been identified as a risk factor for WRMDs in surgeons, younger surgeons may also be at risk for WRMDs due to lack of experience [30]. Hence the need to include this information. Surgical experience was not reported in any studies. A positive correlation between surgical experience and time to fatigue in target muscle groups has been reported [31]. This has been attributed to postural maladaptation of the neck and back muscles over years of adopting particular intra-operative postures [31].
Reporting of the anthropometrics of participants was minimal (Table 4). Anthropometry can vary amongst surgeons and can impact their susceptibility to the development of WRMDs. Hand size has been found to increase difficulty of using surgical tools, predisposing surgeons with smaller hands to developing WRMDs [32]. Surgeons of shorter, or taller stature, may experience different WRMDs. Only one study provided ranges for the height of their participants [25]. Two studies measured both male and female surgeons [24, 25] and one only used a male surgeon [26]. Three studies provided no information on the gender of their participants [27–29]. A 2014 survey of female surgeons found that women who were shorter and had smaller glove sizes were more likely to report physical discomfort in the hand while operating [33]. No studies reported the patient’s body habitus or neck mobility, which may influence the positions held by the surgeon [28, 29]. For the purpose of generalising the findings of the studies, as well as implementing the proper intervention, it is crucial to report information on both the physician and the patient’s demographics and anthropometrics.
The types of surgical equipment-based interventions that were analysed varied amongst studies. Surgical equipment included indirect ophthalmoscopes, slit-lamps and microscopes [27], loupes and headlamps [25] and three types of varying arm support [24]. The methodological quality of these three studies was strengthened by their use of comprehensive biomechanical modelling systems. Standardisation and calibration of assessment tools was consistent across all studies. Studying surgical operations on live patients helped strengthen the validity of the findings of Shaw et al. [27] and Nimbarte at al. [25], whereas Statham et al. [24] obtained their data from photographs of surgeons in a simulated environment. Surgeons may alter their position throughout surgical procedures, as muscular fatigue develops from prolonged static posture, a finding which cannot be captured by Statham et al. [24, 34]. During data collection Statham et al. [24] used chairs that were not identical to those used in surgical procedures. Thereby limiting the internal and external validity of their findings.
However, their use of a large number (
Surgeon and patient position-based risk factors
Two studies based their interventions on patient position [28, 29], while one study altered surgeon position [26]. Govil et al. [28] and Govil et al. [29] quantified their results using the Rapid Upper Limb Assessment (RULA) postural assessment tool, while Ramakrishnan and Milam [26] used surface electromyography (EMG) to quantify muscular fatigue. Although the RULA tool is effective at providing a global assessment of musculoskeletal risk, EMG readings are universally accepted to be an effective assessment tool in ergonomic assessments [28, 35].
The greater number of data acquisition sessions (
Patients Used and Data Acquisition Information
Patients Used and Data Acquisition Information
The validity of the findings of Govil et al. [28] were limited by their use of photographs of seven mock patients. Whereas Ramakrishnan and Milam [26] acquired data by performing the operation on a cadaver, strengthening the validity of their findings (Table 5).
The outcome measures that were used in the studies are summarised in Table 6.
Two studies used motion capture systems to generate three-dimensional (3D) models of their participants [24, 25], considered the gold standard of motion analysis [36], and one used accelerometer-based systems to quantify inclination angles [27]. A high level of agreement has been found between accelerometers and the Vicon system (ICC = 0.774), with both demonstrating good reliability for movement measurements (accelerometer = 0.739, VICON = 0.542,
Although the Trigno Wireless EMG system used by Shaw et al. [27] has been reported to have excellent movement classification accuracy, no other literature could be found on the VICON Peak-612 or FAB [37]. No literature could be found that validated the tools with surgeons.
Non-invasive surface EMG
Non-invasive surface EMG has been established as a suitable measurement tool for assessing muscular activity in ergonomic evaluations [38]. A study of 200 participants [39] found EMG readings to have high intra-rater reliability (ICC = 0.86–88); however, Ramakrishnan and Milam [26] dispute this statement claiming EMG readings can be highly variable.
3-D static strength prediction program (3D-SSP) analysis
The 3D-SSP used by Statham et al. [24] is one of the most widely used quantitative ergonomic tools. It has been found to be valid tool for predicting static strength requirements for a variety of occupational tasks [40]. Despite this, the tool has not been validated with surgeons [41]. Statham et al. [24] also state that external forces were applied to a specific joint (i.e. an elbow) rather than proportionately along the length of the segment (i.e. forearm). This may not mimic the dispersion of force along the human body and limits the generalisability of their findings to the human body.
Rapid upper limb assessment (RULA) Tool
The RULA tool was a suitable outcome measure for three of the included studies both due to its validation with static sitting postures, which resemble surgical postures, and for its ability to detect occupational conditions that warrant ergonomic intervention [24]. The RULA tool is designed to provide an overall risk assessment of musculoskeletal injury but has been criticised for the lack of evidence regarding the predictive value of the subcomponents [24]. Thereby, a causal relationship cannot be established between sub-scores on the RULA tool and the development of WRMDs in the respective area. In addition, the RULA tool has been found to have high intra-rater (91.7%), but low inter-rater reliability (ICC < 0.5) [42, 43].
Loading on the upper-body assessment (LUBA) Tool
The LUBA tool was designed to assess a workers’ static postures and their subsequent risk for developing WRMDs in the upper body [42]. This was a suitable tool for Shaw et al. [27] as its classification system is in line with the aims of their study. However, the tool was developed based on a small pool of male subjects (
Analysis
Large periods of time spent in asymmetrical cervical postures during operating time were reported by Statham et al. [24], Nimbarte et al. [25] and Shaw et al. [27]. Surgeons adopted asymmetrical cervical postures for 85%of operating time [25]. An asymmetrical posture was defined as lateral flexion or rotation of the cervical spine greater than 15°, coupled with flexion greater than 15°. Surgeons spent 65%of operating time in a low loading zone, and 35%in medium-high loading zones (Table 7). Moderate cervical flexion (20–45°) was reported during 42%, and rotation (> 20°) during 77%of examinations that involved an indirect ophthalmoscope [31]. The overall spine was found to be moderately flexed (31–62°) during 76.3%of these examinations. Surgical procedures involving the indirect ophthalmoscope were associated with moderate cervical flexion and rotation of during 50%of operating times. The overall spine was recorded to be in moderate flexion during 76%of operating times. Procedures and examinations that did not involve the indirect ophthalmoscope were associated with near neutral (< 15° deviation from neutral in any direction) postures.
Cervical Loading Zones, Adapted from Nimbarte et al. [25]
Cervical Loading Zones, Adapted from Nimbarte et al. [25]
The use of loupes and headlamps was associated with a mean increase of cervical loading of 40%[25]. This effect was amplified in postures involving cervical flexion≥45° and lateral flexion of 15–30°.
Operative chairs with articulated arm supports led to a lower RULA score and decreased levels of neck flexion, in comparison to chairs with a Mayo stand or no arm support at all [24]. A difference in shoulder torque of 30 Nm was reported between arms-supported and Mayo stand position, suggesting that the Mayo stand was less favourable. When compared to a supported position, the unsupported arm position caused a near four-fold increase in compressive forces at the L5-S1 disc space. Unfavourable ergonomic positions were associated with placing the adjustable eye pieces of microscopes upside down, causing cervical extension. A Trendelenburg table positioning, which involved angling the operative table so that the patient’s feet were are above their head, was found to be more ergonomically favourable for the surgeon [24]. A Trendelenburg bed angle of –7 to –12° in the horizontal plane were used and no
Having the patient positioned in the supine position was associated with lower RULA scores (
Ramakrishnan and Milam [26] noted a general decrease in EMG in the upper extremity musculature during sitting dissections, and in the lower extremity during standing dissections. A decrease in mean power frequency was noted in both right and left hamstring muscle groups in standing. The left and right medial deltoids had a lower mean power frequency in standing. This trend was not observed when sitting, suggesting that standing during surgical procedures is more favourable for the deltoid musculature. The authors suggest that these differences are indicative of muscular fatigue, although the results did not achieve statistical significance (
This purpose of this literature review was to find peer reviewed journal articles assessed work-related biomechanical risk factors in surgeons of the HNF. The findings have been summarised in Table 3.
Three of the included studies were of greater methodological quality when using the STROBE checklist (Table 2) [25, 29]. Four of the included studies incorporated robust, highly precise outcome measures, which helped strengthen the findings of this review [24–27]. Although only two of the studies involved real patients [25, 27], their findings were further strengthened by the comprehensive biomechanical modelling systems used to interpret their results. Limitations of this literature review are the small samples of all included studies and the inability to blind participants (Hawthorne Effect). Additionally, reporting of anthropometric data, and inclusion and exclusion criteria, was poor across all studies.
The conclusions of the current review that surgeons spend prolonged periods of time in neck flexion, is consistent with previous studies [45, 46]. Prolonged static neck flexion has been associated with localized muscular fatigue and pain of the neck extension musculature which can lead to subsequent biomechanical load on the cervical intervertebral discs [25, 47]. As little as 10° of static neck flexion can require 5–7%of the maximum voluntary contraction of the cervical neck extensors, which is sufficient to predispose an individual to musculoskeletal neck pain due to the associated muscle fatigue and subsequent biomechanical load on passive structures [24]. This suggests that the neutral to moderate levels (15–45°) (Table 3) of prolonged cervical flexion observed may be sufficient to predispose surgeons to the development of occupational neck pain [24, 27].
Interestingly, a causal relationship between cervical rotation and neck pain has not been established in scientific literature [48]. However, this literature review suggests that surgeons adopt prolonged static postures with moderate amounts of cervical rotation (20–45°) (Table 3) during intraoperative procedures. Despite the lack of supporting literature, this is a posture to which attention should be paid in the design of future interventions, as prolonged cervical rotation is associated with increased activity of the anterior neck musculature, which may contribute to the development of work-related neck pain [49].
Equipment-based risk factors
The ergonomic burden of using the aforementioned surgical equipment has been well documented in scientific literature [18, 50]. The use of slit lamp biomicroscopy and indirect ophthalmoscopy has been associated with increased anterior deltoid and cervical trapezius muscle activity [46]. These increases in muscle activity may be associated with the lack of arm support during microscopic work, and the slumped position that surgeons adopt to approximate themselves to the microscope [50, 51]. This may provide a physiological rational for the musculoskeletal pain reported from surgeons, which is strengthened by the prolonged asymmetrical static postures observed while this equipment is being used [27]. The use of articular arm supports significantly decreased the biomechanical stress on the surgeon [24], which was consistent with a 2012 Cochrane Review [7].
Surgeon and patient position-based risk factors
While the only result from Ramakrishnan and Milam [26] that reached statistical significance was the left hamstring group in the sitting position, the authors suggest that the general decrease in EMG activity is indicative of the sitting being more favourable for the lower limb musculature and standing for the upper limb. With no discernible pattern emerging from survey data, the optimal intra-operative posture may be surgeon-specific and determined by individual factors such as previous musculoskeletal injuries, personal preferences and present workload [26]. A 2005 systematic review of ergonomics during endoscopic surgery highlighted the difficulty of evaluating an optimal posture during surgery, due to the influences of static and dynamic postural stresses [52]. Prolonged static postures were identified as being a principle cause of the development of musculoskeletal complaints in laparoscopists [52]. Therefore, the difficulty in objectively measuring an ideal posture, as well as the lack of a subjectively-reported preferred position, suggest that the ideal posture may be surgeon and operation specific [26]. Recent evidence suggests that the breaking of static postures can decrease the onset of pain and intensity of muscular contractions, suggesting that a key preventative strategy may be avoiding a posture for an extended period of time [17].
Little surgical-based evidence exists to reinforce the findings of Govil et al. [28] and Govil et al. [29], as the patient is most commonly placed in the supine position throughout surgery. However, a supine position is recognised as the most favourable patient position in a dentistry setting, a finding which may be generalisable to surgeons performing procedures in outpatient clinics [53]. An important finding of these two studies is the subsequent decrease in upper arm and neck RULA scores obtained when placing the patient in supine versus in sitting (Table 3), both of which are areas that are susceptible to the development of WRMDs in this population [13, 14].
Implications
The findings of this literature review may be generalisable to other professions that share similar postural requirements and use similar equipment, such as dentists, dental surgeons, and pathologists [51, 55]. However, caution must be taken when generalising these findings as, other professions may differ in static posture position, duration, equipment and workplace ergonomics. Figure 2 proposes an optimal posture for surgeons when performing procedures in the operating room and in an outpatient clinic.
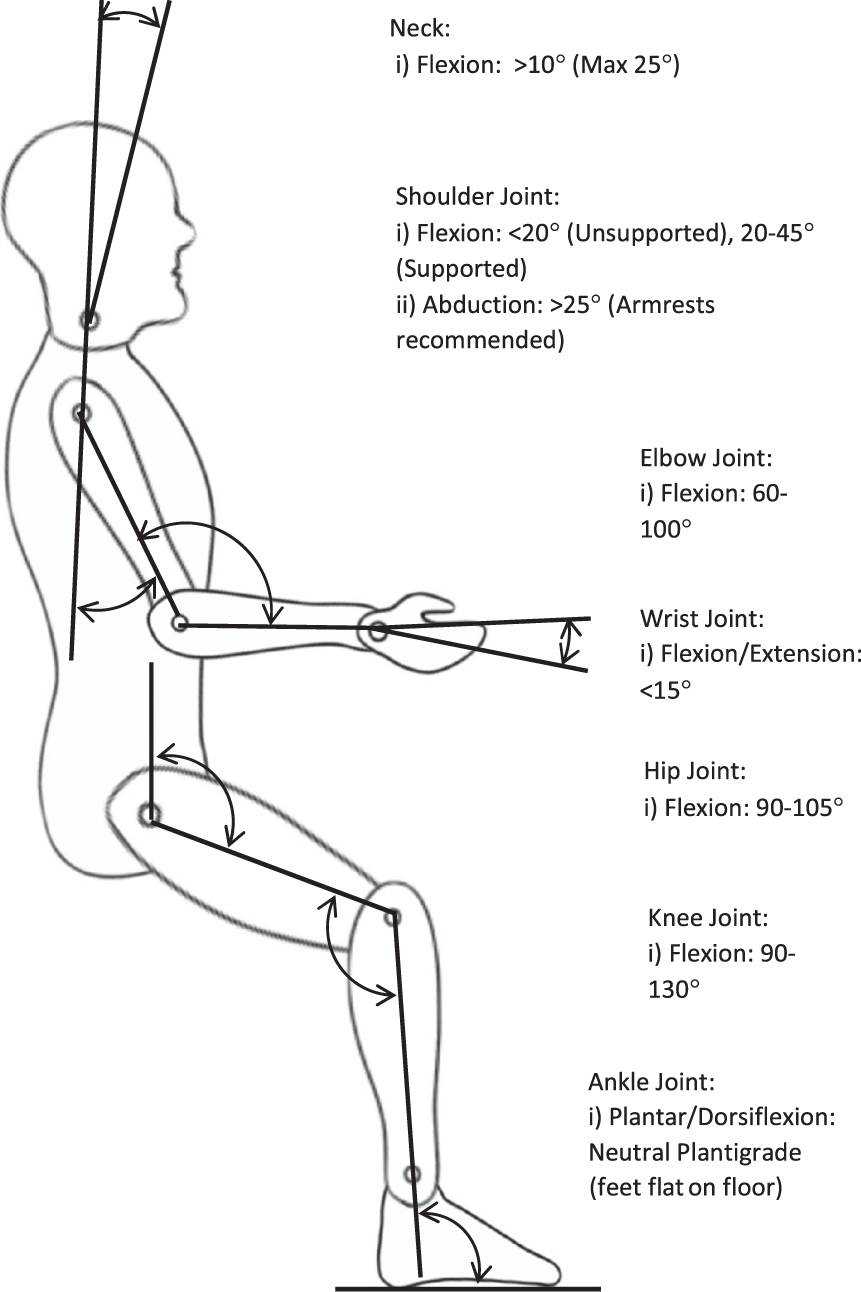
During tasks performed intra-operatively and in an outpatient clinic, surgeons should aim to maintain an anatomically neutral posture and avoid asymmetrical, extreme/end of range postures. Maintenance of a near-neutral posture is especially important when using equipment that may increase the biomechanical loading on the surgeon’s body [27]. When possible, surgeons should utilise a Trendelenburg table tilt to minimise their ergonomic risk [24]. Surgeons can reduce the biomechanical load on the lumbar spine by approximating themselves to the patient [24].
Positioning the patient in a supine position during procedures in the operating room and in outpatient clinics, may improve surgeon positioning [28, 29]. The choice of whether to perform surgical procedures in sitting or standing should be individualised. Surgeons should prioritise one position over the other based on previous musculoskeletal injuries and personal preference. Moreover, they should consider alternating between the two to break up static postures [26, 57]. When operating in a seated position, articulated arm supports are recommended to avoid biomechanical strain [24].
Alrashed [51] suggested the use of a lightweight ophthalmoscope, and to position the slit lamp at the beginning of the workday, adjusting patient position accordingly. Workstation features, such as surgical stool height, operating room table height, monitor placement, and microscope position, should be personalised by the surgeon based on their anthropometrics, and personal preference [51, 58–61]. Optimisation of the surgical theatre environment can improve individual surgeon skill and satisfaction, as well as promote safety [57].
A recent systematic review found the implementation of a saddle seat during surgical procedures to be effective in reducing musculoskeletal discomfort in the neck, back, shoulder and arm in microsurgeons [62]. Favourable subjective and objective results of fatigue and pain in the neck and back in ENT surgeons have been reported with the use of a prototype postural support chair [31].
The use of intraoperative microbreaks during surgical procedures has been highlighted in recent literature, providing evidence that 20 second breaks every 20 minutes can help reduce musculoskeletal pain, improving physical performance and mental focus [63, 64]. The Ipswitch Microbreak Technique, coined by Vijendren et al. [17] found similar improvements with the use of microbreaks on the onset of fatigue and pain in the neck and upper shoulder muscle groups during microscopic procedures.
An individual’s psychological risk factors and perception of work, known as Yellow and Blue Flags, respectively, are associated with the manifestation of WRMD symptoms and are a predictor of disability [65, 66]. Due to the multifactorial nature of WRMDs, it is pivotal that a biopsychosocial approach be taken when implementing interventions targeting at addressing these disorders [2, 66]. A Model of Practice has been proposed in Fig. 3.
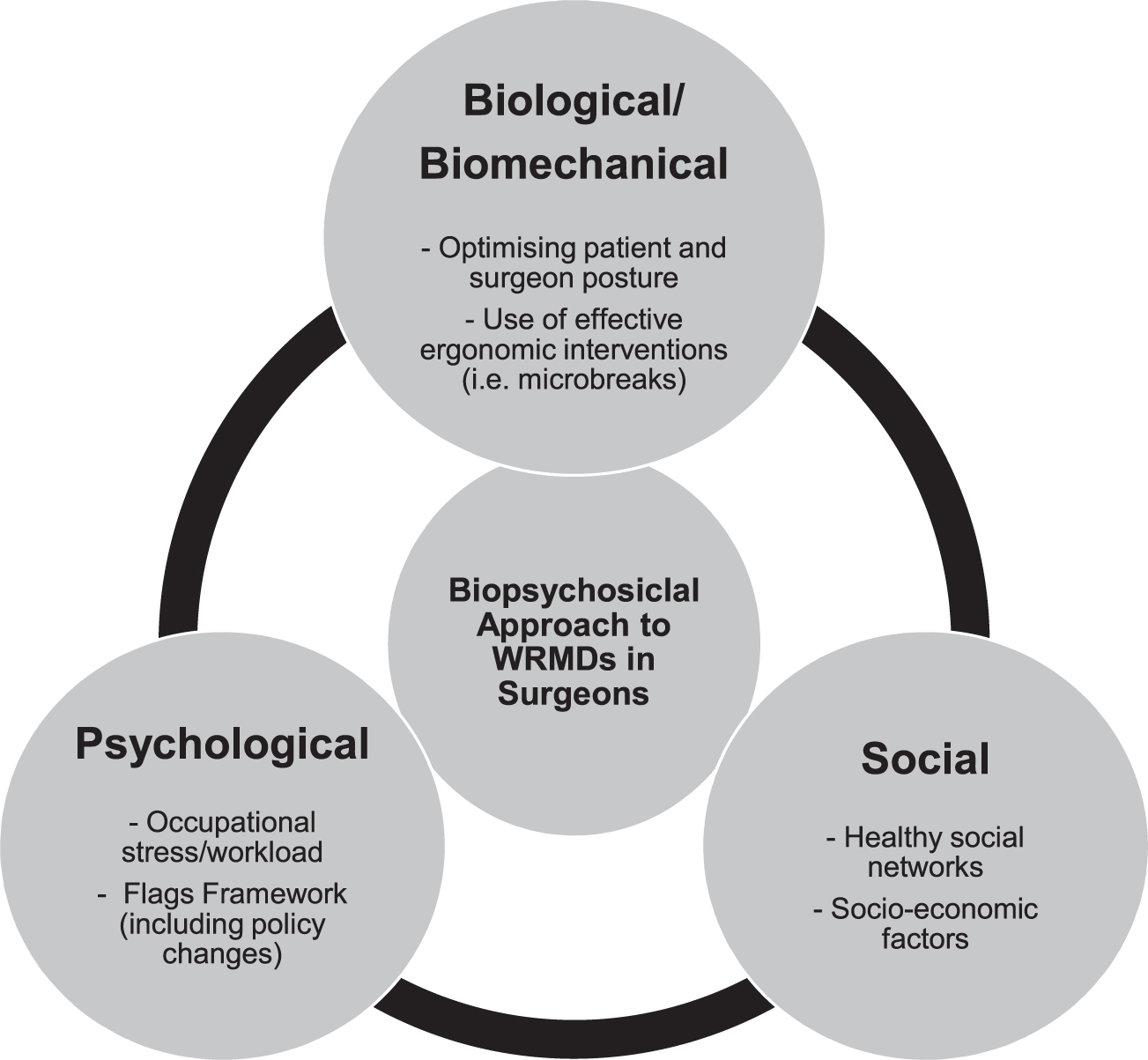
Model of Practice [64].
The implementation of policies that allow surgeons to implement intraoperative ergonomic adjustments to their surgical instruments and surgical environment based on their habitus may be beneficial due to the growing evidence in their efficacy in reducing work-related pain [33, 58].
A 2012 ergonomic survey of ENT surgeons [68] highlighted their lack of awareness of ergonomic principles, despite the high prevalence of WRMDs; a finding that has been reported across multiple surgical specialties by meta-analysis [11]. The authors advocated for the implementation of surgical ergonomic strategies for practitioners, and to implement ergonomic knowledge-based interventions at the education level [68].
Policy changes may look to incorporate intra/inter-operative rest breaks and minimise overtime hours, as these factors may increase the surgeon’s risk of developing WRMDs [51].
Research implications
Future research may look to assess the impact of ergonomic-based (e.g. saddle seats, prototype chairs) and surgeon-based interventions (e.g. microbreaks) to assess their effect on musculoskeletal fatigue and pain, and task performance. Future studies should endeavour to use real life patients in order to strengthen the validity of their findings. Thorough documentation of surgeon and patient anthropometrics and establishing a relationship between their body size and posture during occupational tasks, is paramount to producing results that are generalisable to surgeons of varying body types. The focus of this review was predominantly on the biological/biomechanical domain of the Model of Practice proposed in Fig. 3. Future studies may look to also incorporate outcome measures that assess the psychological and social domains to fully encompass the multifactorial nature of WRMDs.
Limitations
The generalisability of the results to surgeons in the UK may be limited, as the included studies only took place in Canada and the United States. The inclusion of only English-based studies may have caused studies of other languages to be missed in the search strategy. The results may be susceptible to single reviewer bias.
Conclusion
This review elucidates the key biomechanical risk factors and proposed interventions for surgeons of the head and neck adopt postures consisting of moderate amount of cervical flexion and rotation. The use of loupes and headlamps significantly increases the biomechanical load on the cervical spine in postures that deviated from neutral; articulated arm supports were beneficial in reducing shoulder torque and lumbar spine strain; placing the patient in a supine position reduced ergonomic risk; and sitting or standing positions were equally as favourable, biomechanically, for the surgeon.
Conflict of interest
None to report.
Footnotes
Appendix
Excluded Studies and Rationale
EBSCO
1
Vijendren, A., Devereux, G., Kenway, B., Duffield, K., Van Rompaey, V., Van de Heyning, P. and Yung, M., 2017. Effects of prolonged microscopic work on neck and back strain amongst male ENT clinicians and the benefits of a prototype postural support chair.
Not an objective measure of posture
2
Rimmer, J., Amin, M., Fokkens, W.J. and Lund, V.J., 2016. Endoscopic sinus surgery and musculoskeletal symptoms.
Study design (survey)
3
Vijendren, A., Yung, M., Sanchez, J. and Duffield, K., 2016. Occupational musculoskeletal pain amongst ENT surgeons–are we looking at the tip of an iceberg?.
Study design (survey)
4
Williams Jr, K.L., Gupta, A.K. and Schultz, H., 2016. Ergonomics in hair restoration surgeons.
Study design (survey)
5
Lakhiani, C., Fisher, S.M., Janhofer, D.E. and Song, D.H., 2018. Ergonomics in microsurgery.
Study design (report)
6
Alqahtani, S.M., Alzahrani, M.M. and Tanzer, M., 2016. Adult reconstructive surgery: a high-risk profession for work-related injuries.
Study design (report)
7
Bolduc-Bégin, J., Prince, F., Christopoulos, A. and Ayad, T., 2018. Work-related musculoskeletal symptoms amongst Otolaryngologists and Head and Neck surgeons in Canada.
Study design (survey)
8
Lee, J., Kang, S.W., Jung, J.J., Choi, U.J., Yun, J.H., Nam, K.H., Soh, E.Y. and Chung, W.Y., 2011. Multicenter study of robotic thyroidectomy: short-term postoperative outcomes and surgeon ergonomic considerations.
Study design (survey)
9
Khansa, I., Khansa, L., Westvik, T.S., Ahmad, J., Lista, F. and Janis, J.E., 2018. Work-Related Musculoskeletal Injuries in Plastic Surgeons in the United States, Canada, and Norway.
Study design (survey)
10
Wong, K., Grundfast, K.M. and Levi, J.R., 2017. Assessing work-related musculoskeletal symptoms among otolaryngology residents.
Study design (survey)
11
Godwin, Y., Macdonald, C.R., Kaur, S., Zhelin, L. and Baber, C., 2017. The Impact of Cervical Musculoskeletal Disorders on UK Consultant Plastic Surgeons: Can We Reduce Morbidity With Applied Ergonomics?.
Study design (survey)
12
Mendez, B.M., Chiodo, M.V., Vandevender, D. and Patel, P.A., 2016. Heads-up 3D microscopy: an ergonomic and educational approach to microsurgery.
Study design (survey)
13
Ayad, T., Peloquin, L. and Prince, F., 2005. Ergonomics in endoscopic sinus surgery: systematic review of the literature.
Study design (systematic review)
