Abstract
Academic promotion is desired by many faculty practicing at academic medical institutions, but the criteria for promotion often appear opaque to many physician faculty. In nearly all cases, evidence of scholarship is required regardless of academic track. Academic advancement can be stymied by unclear expectations, lack of protected time to engage in scholarly projects, insufficient evidence of dissemination, and limited guidance, mentorship and sponsorship. In addition to being important for promotion, scholarship is an essential aspect of academic medicine because it helps inform and advance the science. Pursuing academic excellence is an important goal for pediatric rehabilitation medicine faculty members because it helps advance the care of children with disabilities and the field itself. Pediatric rehabilitation medicine faculty in the clinician educator or clinician leader tracks are encouraged to understand the criteria for advancement, seek out mentorship, scholarize their career ikigai and identify opportunities to demonstrate academic excellence.
Introduction
Advancing the field of pediatric rehabilitation medicine (PRM) to benefit the health and function of children with disabilities is a laudable goal. One way to help advance the field is to elevate the members of the field through the pursuit of academic excellence and to have that excellence rewarded with academic promotion [1]. Approximately two-thirds of PRM physicians have academic affiliations, meaning they work for or are affiliated with an academic medical center [2]. Notably, over a quarter of pediatric physiatrists who are assistant professors have been at that rank for more than 10 years and over a third of associate professors in practice for more than 20 years have not advanced to professor [2]. Thus, there is an opportunity to focus on improving academic competitiveness to help academic PRM physicians advance in a more timely fashion.
Clinician investigators (also called clinician researchers or clinician scientists) frequently have structured mentorship and clear guidelines for advancement (“publish or perish”) [3], so many do not feel the same ambiguity about the requirements for advancement compared to other academic faculty. Because less than half of academic PRM physicians are engaged in original research, the focus of this manuscript is on PRM clinicians for whom research is not a major part of their careers. Academic advancement tends to be slower for clinician educators who also report less familiarity with the promotion process, less mentorship, fewer opportunities to meet with their leadership, and not having the time or resources to engage in activities that are required for promotion [4].
Focusing on academic advancement also requires addressing gender inequities as there is an under-representation of women at the senior levels of academia worldwide [5]; even after accounting for age, experience, specialty and measures of research productivity, women are less likely to achieve the rank of full professor [6]. Further, there are substantial inequities in advancement for under-represented minorities in medicine [7]. These inequities have long-term consequences to retention, well-being and pay [8]. Structural reform is necessary to address implicit and systemic biases that perpetuate racism, sexism and other forms of oppression and discrimination in academic medicine. Given the current state of academic medicine, members of minoritized groups are frequently disadvantaged compared to their non-minoritized peers in terms of accessing the opportunities that would help them advance and/or not being promoted despite having the qualifications to advance. While acknowledging the need for it, this report does not address strategies for institutional reform; instead, it focuses on approaches for the PRM faculty member seeking a pathway for advancement.
Background information on advancement
Medical schools tend to have at least three academic ranks for physicians: assistant professor, associate professor, and (full) professor. Some routinely use the rank of instructor preceding that of assistant professor. Many institutions further designate professors, such as with an endowment title (endowed professor) or with a distinguished title (distinguished professor) for someone who is a leader in their field of study. Individual faculty progress through the ranks based on requirements as delineated in the faculty handbook or guide for advancement for their academic institution. It is rare for someone to advance to the next rank in less than five years, but it does happen. Some universities have “up or out” policies whereby if the faculty member does not meet their advancement criteria, they lose their faculty status. Many institutions have steps within each of the ranks that faculty members incrementally achieve (climb) before they are promoted or advanced to the next academic rank.
Medical schools tend to have tracks that correspond to how time and effort is spent, such as in clinical care, education/teaching, research/investigation, and/or leadership. Individuals who spend the majority of their time engaged in clinical and education pursuits are usually in the clinician educator track, but this offering is not uniform across institutions [9]. The clinician educator is responsible for a busy clinical practice and provides hands-on education of trainees [10]. They may also disseminate educational innovations through educational scholarship [3]. Some medical schools also have a track for clinician leaders who spend a substantial amount of time in programmatic or administrative leadership in addition to their patient care work. These tracks may exist in the tenure or non-tenure stream, with more rigorous expectations in the former [11].
Academic advancement is tied to excellence which is frequently demonstrated by scholarship. Often, faculty mistakenly assume that scholarship is defined solely by publications. While publications as a form of scholarship are relatively easy to quantify, medical schools tend to recognize scholarly contributions more broadly. There is no uniform definition of scholarship because each medical school determines how they define it, but many institutions use the Glassick criteria for assessing a ‘scholarly approach’: clear goals, adequate preparation, appropriate methods, significant results, effective presentation, and reflective critique [12]. Generally, scholarship is demonstrated when a product applies current knowledge, is judged through a peer-review process and is then disseminated for use by others to enhance their knowledge and expertise [13].
According to the Accreditation Council of Graduate Medical Education (ACGME), scholarship “ \dots begins with curiosity, is grounded in the principles of evidence-based medicine, expands the knowledge base through dissemination, and develops the habits of lifelong learning.” [14] The ACGME considers dissemination of scholarly activity through “grand rounds, posters, workshops, quality improvement presentations, podium presentations, grant leadership, non-peer-reviewed print/electronic resources, articles or publications, book chapters, textbooks, webinars, service on professional committees, or serving as a journal reviewer, journal editorial board member or editor” in addition to peer-reviewed publications [14]. A relatively new way dissemination can occur is through digital media, although only a small percentage of medical schools indicate that social media and digital products would be factored into the promotions process [15]. Altmetrics can be a valuable source of quantifying the impact of scholarly output beyond the traditional methods (impact factor of the journal, number of citations and h-index of the scholar) [15]. Before assuming that their institution considers digital dissemination a legitimate form of dissemination, the faculty member should check their institution’s rules. Often, clinician educators and clinician leaders/administrators get the sense that institutions highly value research and therefore attend only to those associated metrics in their promotions process, putting them at a real or perceived disadvantage [16]. Knowing what ‘counts’ as dissemination of a scholarly product by reviewing one’s institution’s guidelines is a key aspect of preparing oneself for advancement/promotion.
The advancement process is often lengthy. Faculty are encouraged to review expectations and goals annually with their leaders to make sure they are on track for promotion. Usually the decision to ‘put up’ a faculty member for advancement is made by the department chair after reviewing the faculty member’s progress toward meeting the criteria set forth by the university’s (or medical school’s) bylaws for promotion and tenure. In larger departments, there might be a committee that reviews the faculty member’s activities to make a recommendation to the chair. It behooves the chair to only ‘put up’ a faculty member that clearly meets the criteria for advancement; therefore, it benefits the faculty member to assure they can clearly demonstrate how they meet these criteria.
The promotions packet consists of different items (see Table 1) at different institutions, but all require a curriculum vitae (CV) in the institution’s approved format. When preparing an advancement packet for review, the faculty member should make sure to include and cover all the expected activities in adequate detail so that an external reviewer who does not know the faculty member well can come to an informed conclusion as to the appropriateness for advancement. For example, if one of the criteria upon which faculty will be judged is clinical productivity, this information needs to be provided. Similarly, if excellence in teaching is to be judged based on student and trainee scores and evaluative feedback, these data should be provided in the packet.
Items that may be included in a promotions packet
*A portfolio is an organized compilation of evidence of one’s achievements in a particular domain. Some institutions specifically request these but others do not.
Items that may be included in a promotions packet
*A portfolio is an organized compilation of evidence of one’s achievements in a particular domain. Some institutions specifically request these but others do not.
Once the faculty member’s packet is submitted to the promotions and tenure committee, there is a preliminary review, usually in a subcommittee. This review is followed by a request for letters from faculty within and outside the school for a critical assessment of the faculty member’s appropriateness for promotion. If the reviewer assessments are favorable, then a review by the whole promotions and tenure committee is usually conducted. The committee then makes a recommendation to the dean. Institutions may have a more streamlined or more complicated approach than is described here. The process of advancement culminates when a decision has been reached by the dean’s office, although it can take months after a faculty member is approved for advancement for it to be formally reflected institutionally, depending on the institution’s policies.
Clinicians are engaged in the direct care of patients. A PRM clinician educator likely spends most of their time delivering clinical care and in providing didactics and bedside teaching to trainees. This type of clinician educator is often referred to as big C/little e [3]. The faculty member that devotes most of their time to teaching, such as in the classroom for preclinical undergraduate medical students, and has a small role providing clinical care would be a little c/big E clinician educator. These individuals tend to produce educational scholarship and may have or wish to pursue additional training to enhance their teaching skills [3]. The clinician leader similarly either spends most of their time providing clinical care or designing and administering programs. A clinician leader has at least one, and likely more than one, title and associated responsibilities such as division chief, medical staff president, chief medical informatics officer, institute director, associate dean or quality and safety officer. The clinician leader is probably also engaged in bedside teaching, but, because so much of their non-patient care effort is dedicated to programmatic administration, the clinician leader track, if available, could be more aligned with their responsibilities.
Scholarize one’s ikigai
All faculty, but especially early-career faculty, should reflect on what success means to them with the acknowledgement that how institutions define success may differ. As shown in Fig. 1, career ikigai is the intersection of 4 characteristics of work: what the world needs, what someone will be paid to do, what that person is good at and what they love to do [17]. The key to getting promoted is not to start doing things that don’t align with one’s career ikigai, but to scholarize one’s ikigai to the benefit of the individual and the institution. For example, many PRM physicians have created a PRM fellowship curriculum. That curriculum went through a peer review process prior to receiving ACGME approval, but most PRM physicians have not disseminated the final product describing how the fellowship curriculum was created and utilized. Often, scholarizing academic activities means taking some additional steps to build upon the work that you are already doing. A little scholarization can go a long way. It is helpful to know which journals publish abstracts that were presented at meetings (such as when the
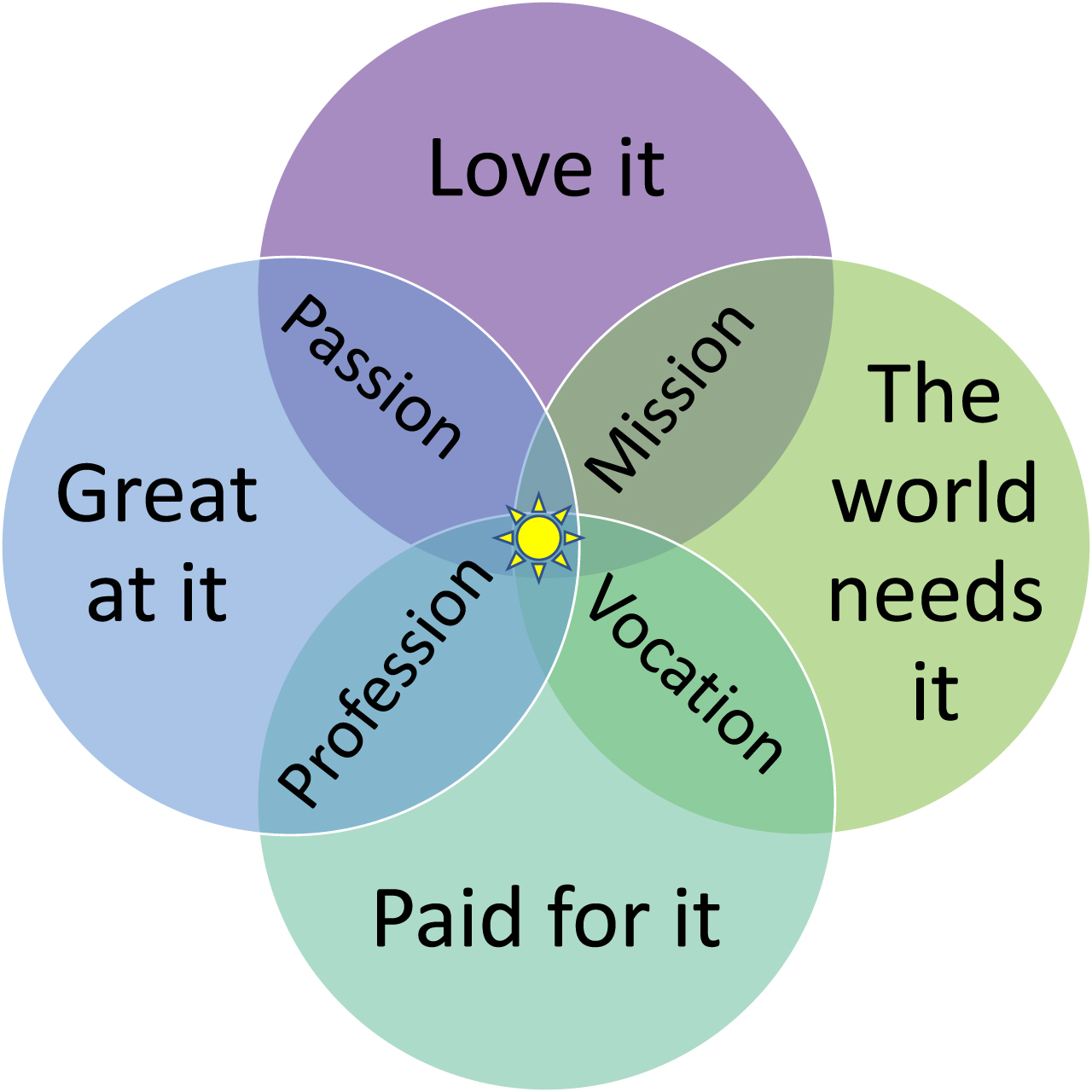
Career Ikagai, the intersection of your passion, mission, vocation and profession.
All physical medicine and rehabilitation (PM&R) residents need to demonstrate scholarship through at least one scientific presentation, abstract or publication [14]. PRM faculty should consider serving as mentors on these projects to boost their mentoring skills and disseminate scholarly findings. PM&R residents must also demonstrate competency in using quality improvement (QI) methods, as do faculty who wish to maintain primary American Board of Physical Medicine & Rehabilitation (ABPMR) certification [14]. Currently, the ABPMR requires a QI project submission every five years for most diplomates for continuing certification [19].
PRM physicians can further scholarize their QI projects with their residents so that it can count towards the scholarly activities necessary for promotion.
As mentioned above, scholarization can occur through social media. For many early-career faculty, engaging in social media is a part of daily life that can be capitalized upon. Social media contributions can serve to propose new ideas (innovate), share resources (disseminate), increase knowledge (educate), and promote change (advocate) [20]. Tracking these contributions on one’s CV, as part of a dossier or in an advancement packet may help demonstrate the faculty member’s impact on the field. Social media promotion also increases attention to published work, which could lead to increased citations and subsequently a higher h-index for those who need to report it as part of their advancement packet [21]. Partnering with the institution’s social media marketing team can create a pathway for dissemination.
In the following subsections, a domain of academic medicine will be reviewed with guidance for the clinician educator or clinician leader. While academic institutions tend to focus on the ‘big three’ (clinical care, education and research), there are other areas that may be recognized as sources of academic excellence, including administration/leadership and service/advocacy. PRM physicians are encouraged to understand how they might meet their institution’s criteria for excellence across these domains. It is also important to note that different institutions value activities differently. What may be sufficient evidence of excellence at one institution might be insufficient at another.
Demonstrating excellence in clinical care
For both the clinician educator and the clinician leader, excellence in clinical practice is expected. Quantitative measures of excellence in clinical care may include clinical productivity, patient satisfaction scores or WeeFIM efficiency (a measure of how quickly patients make functional gains while undergoing rehabilitation). Often these quantitative metrics are necessary but not sufficient to demonstrate excellence in clinical care. Table 2 provides examples of how a faculty member might demonstrate clinical excellence. The early-career clinician is encouraged to build on the clinical skills they gained in training. Finding a clinical niche and building targeted knowledge and skills helps set the early-career faculty member apart. Although QI is not usually its own domain in faculty handbooks, its increasing importance to clinical operations means that PRM physicians are likely engaged in QI and may have the opportunity to scholarize that work. Because QI intends to improve care, processes or outcomes for patients in the clinical setting [22], excellence in QI is often noted under the clinical domain for advancement.
Examples of Clinical Excellence for Promotion
Examples of
The value of QI and Implementation Science, as well as patient safety (PS) efforts, is increasingly recognized by academic institutions. Publishing QI projects takes effort, especially because it is often challenging to find a peer-reviewed journal that will publish them [23]. In 2009, the Society of General Internal Medicine Academic Hospitalist Taskforce and leaders in general internal medicine published a quality portfolio to help outline how excellence in QI can be demonstrated beyond publication in the peer reviewed literature [24]. The components outlined for a portfolio include a narrative, listing of leadership and administrative activities, project description, education and curricular efforts, research and scholarship, recognition and any training or certification obtained in QI or PS [24]. Various institutions have worked to incorporate the portfolio into their advancement policies; even if it is not current process at an individual’s academic institution to use a QI portfolio, using the components can help the faculty member demonstrate excellence [25, 26]. Faculty should be encouraged to document their work in academic journals as a recognized method of academic achievement. Standards for Quality Improvement Reporting Excellence is a framework for publication of QI work that can be used to guide faculty in manuscript submission [27]. Of note, published QI projects may serve as demonstration of excellence in investigation/research (see Table 4). Engaging in QI may also be evidence of excellence in clinical care as described above (see Table 2). Individuals who serve in QI or PS leadership may have that noted as excellence in clinical care or leadership/administration (see Tables 25).
Examples of Investigation/Research Excellence for Promotion
Examples of
In addition to clinical work, the clinician educator engages in the art of teaching the next generation of clinicians. In a mixed methods analysis, competencies endorsed for clinical educators included teaching, scholarship, leadership, educational theory, curricular development, communication, and assessment [28]. The Toolbox for Evaluating Educators, created by the Association of American Medical Colleges (AAMC), identifies five domains of evaluation: teaching, learner assessment, curriculum development, mentoring/advising, and educational leadership and administration [29]. These domains are to be assessed by quantity, quality, scholarly approach and scholarship. Scholarly teaching involves reflection on one’s teaching to assure efficacy and quality, as well as curriculum development, curriculum revision when appropriate and the evaluation of teaching [13]. Scholarly teaching enhances the value of teaching for the institution by assuring its high quality [13]. Dissemination of educational materials through a peer-reviewed process may be achieved through typical research publication pathways, but newer opportunities exist to publish undergraduate and graduate medical education materials geared toward clinical care through MedEdPORTAL, the Journal of Teaching and Learning Resources [30]. Pursuing a degree in medical education may further enhance pedagogical skills for those who are interested in more direct education. Obtaining additional degrees or certifications may also demonstrate academic excellence. Developing and maintaining an educator portfolio such as the one provided by the AAMC is helpful for promotion in this area. In general, excellence is demonstrated by the breadth, depth, longevity and quality of teaching and can be evidenced by summaries of evaluations, receipt of awards, and serving the educational missions of national or international organizations. For more examples of educational excellence, please see Table 3.
Examples of Teaching Excellence for Promotion
Examples of
Examples of
While a minority of PRM physicians are poised to advance based on excellence in research as independent investigators, many will collaborate on research teams and publish. Some might have small projects that they lead, potentially with funding from their institution or a foundation, but these tend not to be substantive enough for the faculty member to be recognized an independent investigator. The primary way excellence in research is demonstrated is through the dissemination of original research in peer-reviewed literature. But, as Table 4 describes, there are a multitude of ways to demonstrate excellence. PRM physicians with an academic interest in research are encouraged to seek out colleagues within and outside their departments for scholarly collaborations. Presenting research in the form of a poster or platform at a national meeting can also serve as evidence of excellence and dissemination. When considering whether to join a project, PRM physicians are encouraged to consider the effort required and the potential benefits to their institution, children with disabilities and themselves. Discussing expectations early and often can help solidify roles and responsibilities and assure that the desired outcomes are achieved. If one of the goals of the collaboration is to publish in a peer-reviewed journal, plans should be made to meet the international criteria for authorship [31]. These criteria assure the author has contributed to work, drafted or critically reviewed/revised the manuscript, approves it for publication and assumes responsibility for the work [31].
Demonstrating excellence in leadership/administration
Some institutions have a specific domain for administrative or programmatic leadership; others highlight leadership in a specific area as evidence of excellence in that domain. For example, a medical directorship may serve as a marker of distinction in the administrative domain or an indicator of superior clinical skills in the clinical care domain. A growing area of emphasis is on diversity, equity and inclusion (DEI). Individuals actively engaged in DEI work should investigate where those efforts should be noted. For example, serving as the chair of a DEI committee might be considered under leadership, but helping recruit faculty may best be listed under service. As Table 5 shows, there are numerous examples of leadership that could be recorded under a different domain depending on the institution’s advancement criteria and the faculty member’s emphasis.
Demonstrating excellence in service and advocacy
Recent awareness of the role of academic medicine highlights that beyond the 3 typical pillars of the academic mission are social accountability and engagement [32]. Participating in advocacy and service can take many forms (see Table 6) including community outreach, knowledge dissemination, conducting advocacy training, and providing organizational advocacy leadership [33]. Community outreach may involve volunteering, such as serving on a board of a non-profit organization or helping an adaptive sports team. Recognition that advocacy is important for the population’s health has helped create a paradigm shift in which physicians’ ethical duty to improve health can be operationalized through advocacy [33]. But there remains incongruence with how institutions designate the value of advocacy and service as compared to research or teaching [33]. For some institutions, service to the community may not be formally considered in the advancement packet; for others, especially if the service is for underserved members of the community, there may be an opportunity to highlight community engagement. For promotion, how to demonstrate a scholarly approach to advocacy with documentation of quality and quantity may differ from institution to institution, so the PRM faculty member engaged in advocacy or service should seek to understand the documentation required. In some institutions, service might not have its own designation of a domain for demonstrating excellence, but instead might fall under each of the three major domains: clinical, teaching, and research.
Examples of Service and/or Advocacy Excellence for Promotion
Examples of
It is beyond the scope of this manuscript to delve into negotiating techniques, but suffice to say, negotiating is an essential component of thriving in academic medicine. When being recruited into the clinician educator track, the faculty candidate should negotiate for the time and resources needed to be academically successful. Recognizing the effort involved in academic pursuits, departments should allow for protected time, but they often do not. Ideally, twenty percent of one’s time can be structured to develop scholarly activities, teaching skills and training programs [10]. Well-utilized protected time benefits both the physician and their institution. Additionally, departments should make resources available for the clinician educator to engage in scholarly pursuits [10]. Faculty at every stage of their career can take stock of their progress and trajectories and dialogue with their leadership regarding academic advancement, new opportunities, shifting responsibilities, and resources needed for academic success. When advocating for resource needs with leadership, being explicit about why the resource is needed and how it will be used can help. Many people ascribe to the SMART goal-making strategy in which goals are Specific, Measurable, Assigned, Realistic and Timed [34].
Every academician needs support to grow professionally. There isn’t a one-size-fits-all model of support. Increasingly, though, protected time for meaningful activities is being identified as important to preventing burnout [35]. The master clinician often benefits from dedicated time and funds to participate in national academic professional societies [3]. The developing master clinician may take on roles for patient-oriented organizations, be engaged in community outreach, write case reports or clinical reviews and give grand rounds on a clinically-relevant topic in their discipline [3]. The clinician leader often benefits from protected time and funds for leadership training, QI and expanded knowledge in health care financing [3]. Potential scholarship might take the form of clinical policy statements or programmatic development and evaluation, in addition to or in lieu of case reports or chapters. For PRM physicians heavily engaged in education, having protected time for scholarship and additional training in curriculum development, learner assessments and educational program evaluation can be leveraged to enhance academic excellence [3]. Leaders in education may produce scholarly products focused on trainees and curricular innovations. In the negotiation for protected time, identifying what outcomes can be expected helps the institution justify the time [3]. Defining outcomes in terms of scholarly products is a concrete demonstration of commitment to the academic mission.
Mentorship
Meaningful mentorship helps build skills, increases productivity, aids in career advancement and helps mitigate burnout [36, 37]. For clinician educators, finding a mentor and establishing a fruitful mentoring relationship can be challenging, especially since many medical schools have inadequate processes set up to foster mentorship [36]. In addition to the standard hierarchical model of mentorship, peer mentoring is a type of mentoring that has gained traction in recent years with formal programs created at many institutions and societies [36]. A faculty member may have several mentors depending on their needs and may simultaneously be mentoring others [38]. Like all relationships, the mentoring relationship takes effort. Both parties need to be engaged and committed [39]. Setting a structure and communicating expectations should be a part of the process.
For individuals on a path to promotion, having a near-peer mentor who has recently gone through the process can be helpful. For faculty searching for opportunities for activities that will raise their national prominence, having sponsorship can be incredibly beneficial [37]. When sponsored, a protégé is put forward by their sponsor for career advancing opportunities. To be an effective sponsor, the individual must have adequate authority or influence over the decision-making process of the opportunity; thus it is essential that the sponsor already have an established career [37]. A mentor can serve as a sponsor, but sponsorship can be much more episodic where meaningful mentorship is usually longitudinal. Many experts see mentorship as insufficient, especially for women and underrepresented minorities in medicine, and highlight the specific need for sponsorship to aid in advancement [37].
A common question that early career faculty ask is “how do I find a mentor?” While this question acknowledges the importance of mentoring, the better question to ask would be “how do I cultivate mentoring relationships?” The faculty member should think about creating a team of mentors that serve different as well as overlapping purposes [38]. Depending on an individual’s needs, a mentor may be more prominent in one career phase than another. Finding a mentor takes action. Sometimes mentors are assigned but often that assignment is short-lived (such as to orient a new faculty member to the institution). The chair or your chief can recommend potential mentors, as can other colleagues. Trusted advisors from residency or fellowship might be able to stay on as mentors or serve as a bridge to new mentors. Faculty are encouraged to be brave and ask! It is not a marriage proposal; the relationship can start small and focused, providing an opportunity to blossom. It is important to realize that being a mentee is not a passive process at any stage. A mentor is not a coach who puts you in the game and tells you what to do. The mentee is the person primarily responsible for ensuring that the mentoring relationship moves forward [39].
Sometimes mentoring relationships don’t work out. Rarely is a mentoring ‘divorce’ necessary, but some relationships should fade away or need to be terminated. Having a team of mentors buffers the faculty member from the loss of one mentoring relationship. Mentees should not expect their mentors to have all the answers or be able to solve all their problems but instead should expect guidance, modeling, encouragement, sage counsel, and help charting a path. One mentor might be great at navigating the politics of academic medicine, while another reliably gives critical feedback on scholarly work, while yet another might serve as a model academician with a career to aspire to.
The question “how do I cultivate mentoring relationships?” should also be reflective. Being a mentor is a part of being in academic medicine. The faculty member taking on mentees should be judicious and be able to commit to the budding relationship. Being clear about one’s capabilities and creating a structure for engagement helps assure that the relationship will be fruitful. Collaborations with mentors and/or mentees should be noted on the CV. Some institutions expect to have each mentee’s trajectory documented as an indicator of mentoring skills. More seasoned PRM physicians should consider how they can sponsor and mentor others.
Conclusion
All academic medical centers have one clear focus: improving health [40]. How faculty members contribute to that mission differs and should be based on the strengths of each of the faculty and the needs of the institution. While some PRM physicians may be heavily engaged in traditional research, most will find their academic strengths in patient care, clinical leadership, QI, educating the next generation of clinicians and service to their communities. To thrive in academic medicine and advance in rank, PRM physicians are encouraged to commit to lifelong learning, ongoing professional development, and scholarizing their ikigai.
Hot tips
Know what success looks like for yourself and at your institution Start planning for promotion/advancement now Know what is necessary for promotion Understand what is sufficient for promotion and in which combinations that capitalize on your strengths Keep an ongoing record of your accomplishments Organize your CV in the institution’s expected format Document how the requirements for promotion are met in your portfolio or advancement packet Scholarize your passions Find opportunities to collaborate with others with strengths that are different than yours Track quantitative measures of dissemination of your scholarly products Seek out senior and peer mentorship Consider additional training in leadership, QI or educational scholarship Engage with professional societies for learning, networking, educating, disseminating and in service
Footnotes
Acknowledgments
The authors have no acknowledgments.
Conflict of interest
The authors have no conflicts of interest to disclose.
