Abstract
PURPOSE:
Spina bifida (SB) often results in a complex disability and can also cause cognitive dysfunction. No previous study has investigated the ability to adapt to time in children with SB. This ability is crucial for an individual’s possibility to develop autonomy in life. The purpose of this study was to investigate whether children aged 10–17 with SB have lower time-processing abilities than typically-developing children, and to describe the profile of time-processing in children with SB.
METHOD:
Participants comprised a consecutive sample of 21 children (drawn from a geographical cohort of 45) aged 10–17 years (mean: 14 years, SD: 2 years); 13 were boys. The instruments used were KaTid-Y, Time-S, and Time-P.
RESULTS:
The children with SB had lower time-processing abilities than typically-developing
children (52.4% under
CONCLUSIONS:
The low time-processing ability found in children with SB is likely to be an important contributing factor to low autonomy and independence.
Introduction
Being born with spina bifida (SB) often results in a complex disability [1]. Motor ability and mobility impairments have been well described [2], along with impairments in bladder and bowel functions [3]. Recent studies have also shown that SB often also has cognitive effects [1, 4, 5]. The hydrocephalus (HC) that affects about 84% of those with SB is a worsening factor [4]. The cognitive difficulties predominantly affect executive functions such as initiation, planning, and problem-solving, but also manifest as problems with spatial relations, memory, and attention [1]. Knowledge about the consequences of these cognitive difficulties for the everyday lives of people with SB is still emerging [5]. Executive dysfunction is the factor with the strongest impact on independence for this group, as it creates difficulties in carrying out activities autonomously [6]. One everyday skill of major importance for autonomy is daily time management [8]. Managing daily routines in a timely order and in due time to be ready for school is part of daily time management, and is expected of every child. Coping with this is a way to increase autonomy. It is also a crucial skill for people with SB in particular, as most of them must perform clean intermittent catheterization (CIC) every three or four hours, each day of their lives, in all contexts [3]. Living with a schedule such as this places high demands on time management.
Daily time management is a complex construct which includes both a) adapting to time and b) managing time, and is dependent on the individual’s time-processing ability (TPA). Current research shows that TPA is one cohesive ability that can be seen as hierarchically built up from skills in i) time perception ii) time orientation, and iii) time planning [9, 10]. Consequently, time perception is needed in order to learn time orientation and time planning. TPA develops throughout childhood, with children typically learning it in transactions with significant others [11]. Within daily routines, the young child acquires experience of the duration of activities [9]. The concepts of time and the timely order of days, which form a basis for orientation in time, develop during the preschool and early school years, allowing children to use devices such as clocks and calendars to place themselves in control of time. When time orientation is combined with planning skills, the child develops the cognitive skills of TPA and managing time in daily life, both in daily activities and in less frequently occurring events. Life events during the teenage years give many opportunities to learn adaptation to time; for example, actively using a calendar to manage long-term assignments for school, and re-planning when things turn out differently from the way they were originally planned. TPA also requires other cognitive functions such as spatial thinking, memory, planning, and problem-solving [12].
Despite the knowledge that people with SB have executive and spatial problems, and the clinical/anecdotal experience that adults with SB have a low ability to adapt to time, the published knowledge about the profile of TPA in children with SB is yet scarce. Donlau et al. [8] reported that low TPA impairs independence in the CIC procedure. In a cluster analysis of children aged 5–10 with and without developmental disabilities, children with physical disabilities including both cerebral palsy (CP) and SB had lower mean TPA in comparison to typically-developing children [13]. To the best of our knowledge, no study has investigated TPA exclusively among children with SB, thus such study should be important in order to better provide appropriate help and resources for this group.
The purpose of this study was to investigate whether children with SB aged 10–17 have lower TPA than their typically-developing peers, and to describe the profile of TPA in children with SB.
Methods
The study was a cross-sectional geographical cohort study designed to describe the profile of the cohort.
Participants
All 10–17-year old children with SB who attended their annual urological rehabilitation follow-up according to the Swedish national follow-up program for children and adolescents with myelomeningocele at the Regional Rehabilitation Centre in Gothenburg between 1 November 2013 and 31 October 2014 were invited to participate in the study. All children with SB up to 18 years living in the western region of Sweden (representing 23% of the Swedish population) attend this clinic for urological rehabilitation of their bladder and bowel control.
Inclusion criteria were being requested to attend the follow-up at the clinic during the one-year study period and being able to communicate in Swedish. Of the approximately 45 children in the relevant age span living in the western region of Sweden, 30 met the inclusion criteria. The families received an invitation letter which provided information about the study, and the parents were asked for written consent. The children received their own information letter, and those aged over 15 years were also asked for written consent. Of the 30 children/families invited, 22 agreed to participate; one of these was unable to carry out the assessment because of health issues, giving a total of 21 participants (8 girls, 13 boys; mean age: 14 years, SD: 2 years). Of these, 19 attended mainstream education while the remaining two were educated under the curriculum for learning disabilities (according to Swedish legislation, to be entitled to this type of education the child should have an IQ below 70). Characteristics of the participants and non-participants are summarised in Table 1.
Demographic characteristics of the study group of children with spina bifida
compared to non-participants
Demographic characteristics of the study group of children with spina bifida compared to non-participants
A comparison sample of typically-developing children aged 10–17
(
The children were assessed by a trained and certified KaTid rater (the first author). The training to become a certified KaTid rater includes three days of education and training in using the material among children with and without disabilities. Each assessment took place during the child’s follow-up visit to the centre and took approximately one hour of the child’s time, during which the parents filled in the parental rating form. After the assessment, the children and parents had the option to discuss the result of the assessment with the occupational therapist (most families chose to), and if necessary received a brief consultation about ways to move forward in the development of time-processing skill.
The study was approved by the Regional Ethical Review Board at Gothenburg University and the Regional Ethical Review Board in Uppsala.
Data were collected with three instruments: the youth version of KaTid (KaTid-Youth) to measure TPA, and the Time-Parent scale (Time-P) and Time-Self-rating scale (Time-S) to measure daily time management.
KaTid-Youth [14] was created to
measure the domain of time perception, (i.e. which activities take long and short time;
subscale A), time orientation/concepts (i.e. the timely order of the day, the week and the
seasons; subscale B) and time orientation/objective time estimation (i.e. time quantity
and time perspectives; subscale C), and time management/planning (i.e., the ability to
decide what do I have time to do and the ability to plan ahead to be in time for
something; subscale D), all of which are summed into a total TPA score for children aged
10–17 years. It is a table-top test containing 59 items, in which a professional asks the
questions and the child can answer verbally or by pointing to a picture. An evaluation of
KaTid-Youth found that the mean logit of TPA among typically-developing children
(
Time-S contains 28 items on managing one’s time and adapting to time
demands, which together cover daily time management. The items are divided into three
domains, and are answered using a Likert agreement scale with four response alternatives
from 1 (never) to 4 (always). Analysis of the psychometric properties in children aged
10–17 years with a diagnosis of ADHD, autism, CP, or mild intellectual disability
(
The parents’ ratings of their child’s ability to manage time in daily life
were obtained using Time-P [10], which includes
12 statements and uses the same four-point response scale as Time-S. A version for parents
of children aged 5–10 has been found to be psychometrically sound (internal consistency:
Data analysis
The results from the KaTid-Youth assessment of the study group were
analysed statistically in two different ways. First, the raw scores and scaled scores were
compared to the calculated means and distribution for each age year group (10–17 years) of
the comparison group. The numbers of participants corresponding to the mean range and to
the ranges of
The medians of the children’s and parents’ ratings on each item on the two rating scales were calculated and are presented as a group profile.
A chi
Results
Children with SB had an overall low TPA; 11 of the 21 children with SB had raw
KaTid-Youth scores within
KaTid-Youth: Proportion of children with spina bifida (
21), raw scores and scaled scores, compared to the mean
and SD of the comparison – group of typically-developing children
KaTid-Youth: Proportion of children with spina bifida (
The scaled score results showed no significant difference in the proportion of
how many children with SB did not perform in the same way as their same-age peers in each
year group (
Comparison of medians of raw total-and sub scores and means of scaled score of KaTid-U between spina bifida group and matched control group. KaTid-U Sub scores; A: time-perception, B: time orientation/concepts, C: time quantity and time perspectives, D: time management and time planning
Boxplot, medians, and percentiles of KaTid-Youth raw scores (score range 1-65) in the
spina bifida group and the matched control group.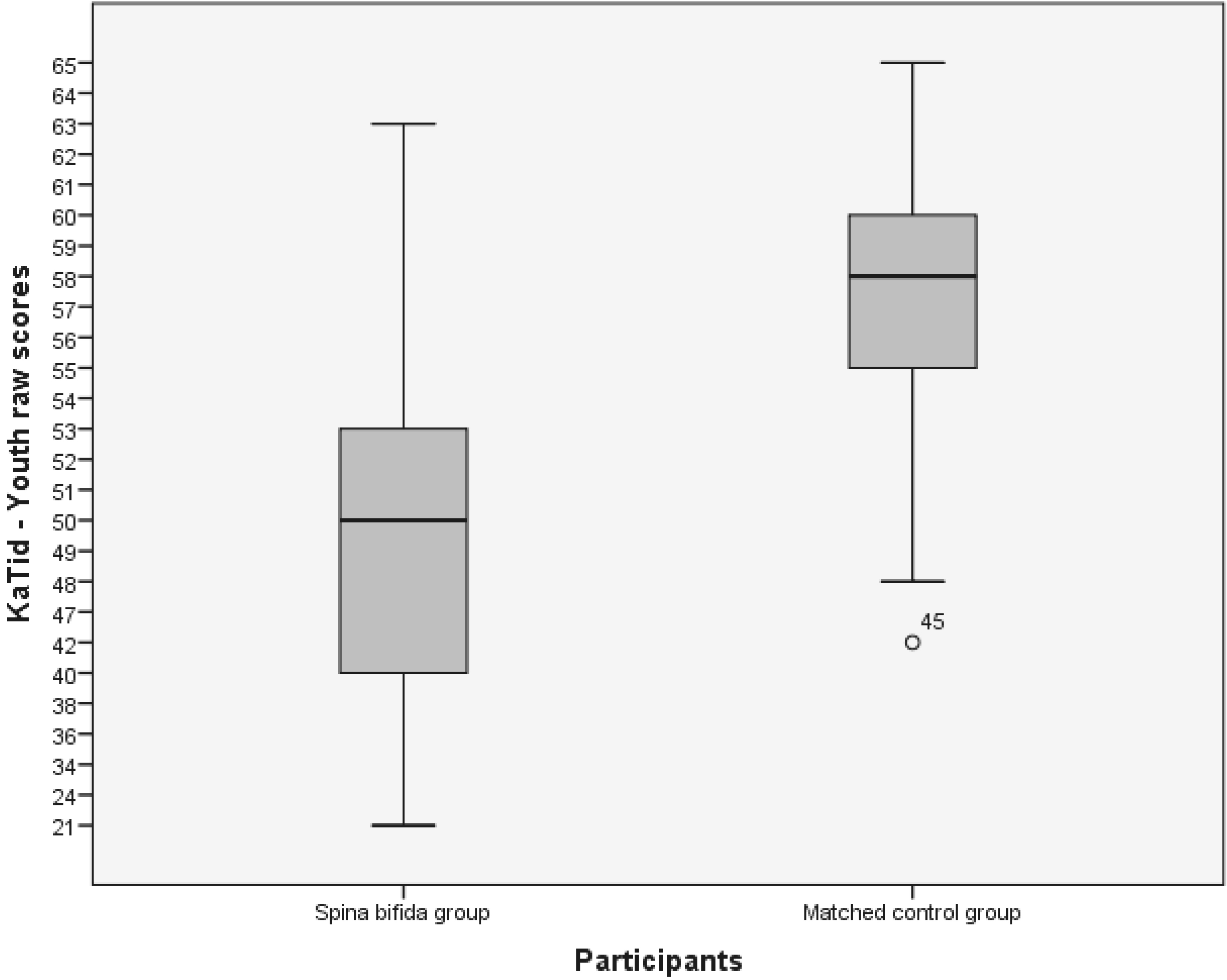
Comparison of the total KaTid-Youth scores of the entire SB group to the scores
from the matched control group showed that the children with SB had significantly lower
scores, both in mean total scaled score (
The subgroups of SB (HC, level of lesion, sex, school type) were small, and no
significant differences were found regarding scaled score. All children who attended school
in special education groups for those with intellectual disabilities (
The profile of the total SB group regarding self-rated daily time management (Time-S) showed that the children scored a relatively high ability (medians of 3 or 4, i.e. “often” and “always”) on 11 of the 13 items in the Routines and habits domain. The children rated themselves as following routines most of the time, except for homework routines. They had low scores on the item “I initiate tasks independently”. In the How I do domain (i.e. how they handled time), they had low scores (median of 1 or 2, i.e. “never” or “seldom”) on 5 of 8 items. They perceived more difficulties with everything that demanded time orientation and prospective memory, problem-solving, or using aids (e.g. keeping track of events occurring in the next week or month, doing things differently when short of time, being prepared in time, or using a calendar). In the Strategies domain, they had low scores on 5 of 7 items; that is, they reported that they used very few strategies, mainly relying on asking someone for help.
The profile of parental ratings (Time-P) revealed difficulties in most items. These ratings had medians of 1 or 2 (“never” or “seldom”) on 10 of 12 items, with the only exceptions being “can wait” and “can deviate from routines in the same way as other children their age”. The parents rated their children as having a low ability on everything that concerned the child’s own responsibility to adapt to time, such as waking up by their own means, being on time, keeping track of coming events, and having strategies for planning trips on public transport.
Two-thirds of the children with SB in this study had lower overall TPA than the typically-developing children in the comparison sample, and more than half of them had considerably lower ability. Their self-ratings showed a low use of strategies in daily time management, and their parents perceived that the children had extended difficulties in daily time management. This result can be explained in light of the cognitive profile of SB, which describes common difficulties with executive functions such as initiating, planning, and problem solving, but also memory and spatial relation [1, 16]. Still, this knowledge of time-processing disability is new, and constitutes an important new piece in the puzzle of why people with SB have such low autonomy in daily life.
The results of this study demonstrate that the children with SB had considerable difficulties with time orientation and time planning. It indicates that despite an average ability to perceive time and to learn time concepts the children were less able to orient to and to estimate objective time, to understand time perspectives and to plan ahead to be in time for an event or use a time frame. These difficulties, manifested in KaTid-Youth subscales C (time orientation/objective time estimation) and D (time planning), are congruent with descriptions of the cognitive phenotype of SB. These subscales involve the ability to consider several factors and merge them into new knowledge which allows decisions to be made (i.e. assembled processing), an ability often described as significantly difficult for people with SB [16]. Time orientation and time planning both also demand good spatial thinking and awareness, which are similarly described as difficult for this group [16].
The finding that the children with SB in this study had better time perception (subscale A) than the children in the matched control group is interesting, but somewhat surprising. It is worth discussing whether children with SB actually have good time perception. These items rely on the child’s experience of time; and according to Dennis Edelstein et al. [17], people with SB have extensive difficulties with timing, which ought to have an impact on time perception. However, the present results give no indication that children with SB have difficulties in time perception, as assessed with KaTid-Youth. In an analysis of TPA in younger children (aged 5–10) with and without disabilities, both the children in the combined group with physical disabilities (including both SB and CP) and those in the group with ADHD had lower mean scores on subscale A than typically-developing children [13]. This is in line with other research in children with ADHD [18]. The results of the present study could thus imply, as an incidental finding, a difference in the pattern of TPA between children with SB and ADHD. Furthermore, in the parental ratings (Time-P), the parents gave their children high scores on two abilities that children with ADHD and autism usually have difficulties with (i.e. waiting for one’s turn and being able to deviate from routines) [19] but low scores on all other items. This strengthens the suggestion that the profile of TPA is different in children with SB compared to children with ADHD and autism. Still, there is a need for further study of time perception among children with SB.
This study has several limitations. The participant group was small, and further research must be conducted on a larger scale. However, the sample was consecutive and represented approximately two-thirds of a geographical cohort. Some studies suggest that children with SB have a slower developmental trajectory [20]. This study only incorporated adolescents up to 17 years, and studies on older adolescents and young adults must also be conducted. Still, given the previously-reported difficulties in autonomy [6]and the present finding that the children did not seem to do better at higher ages compared to peers, it can be presumed that these time-processing difficulties will follow the individuals into adult life. This study was cross-sectional, and aimed to describe the profile of time-processing abilities and daily time management in children with SB. No attempts were made to discover which additional factors, such as insert general cognition, were associated with the profile; nor was the aim to find causal factors of the profile. This can be regarded as a shortcoming of the study, and further studies should be carried out to investigate those questions. It should be recognized, however, that all except two of the children with SB were educated in the ordinary Swedish mainstream school curriculum.
The most important result of this study is that the children with SB had extended problems with TPA and daily time management as a whole, which indicates difficulties in adapting to time. The children also reported restrictive use of strategies, meaning that they did not compensate for their shortcomings; this is probably a consequence of limited problem-solving skills [16]. This knowledge could explain some of the obstacles, described in numerous studies [6, 21, 22], to achieving autonomy in daily life and society. The difficulties in adapting to time described in this study might lead to restrictions in the children’s participation in society, and can also explain the pronounced difficulties in independently sustaining health procedures frequently reported among adolescents and adults with SB [22]. Maintenance of a CIC regime and the procedure of daily skin inspections both require daily time management skills, and the results from the rating scales tell us that that these skills were low in the SB group. According to both the children themselves and their parents, problems particularly occurred when the children needed to use various strategies to adapt to time and when things were not totally scheduled. People with SB have well-known problems in initiating tasks [23], which was also shown in connection to daily time management in the parental ratings. This makes it difficult to get things done in time. Knowledge about this aspect is crucial to consider and appropriate help to manage those difficulties should be allocated from an early age in order to prevent common complications such as early deaths due to renal dysfunction described by Oekshott et al. [24] and unnecessary medical complications from skin wounds or ulcers for people with SB [25].
Conclusions
Children with SB in this study had notably low TPA and daily time management skills, which likely contributes to low autonomy and low independence, and also threatens both their societal participation and their lifelong health. Healthcare professionals, teachers, and parents must consider these difficulties. There is a need to develop and evaluate intervention methods to improve time-processing abilities such as generating one’s own strategies and/or compensating for one’s own shortcomings, to find out if this will enhance participation and autonomy in daily life and in society for people with SB.
Footnotes
Acknowledgments
The authors would like to thank the children and parents who participated in this study. The study was financially supported by the Petter Silfverskiöld Memorial Fund, the Folke Bernadotte foundation, The RBU research foundation and the Swedish Occupational Therapy research foundation.
Conflict of interest
The second author developed the instrument KaTid-Youth, the Time-Parent-scale and the Time-Self rating scale and sell the KaTid material and training courses to professionals. The other two authors have no disclosure or conflicts of interests with respect to authorship and/or publication of this article.
