Abstract
PURPOSE:
Endoscopic Third Ventriculostomy (ETV) and Choroid Plexus Cautery (CPC) are low-cost, safe, and promising interventions for spina bifida-associated hydrocephalus (SBHCP). The purpose of this review was to explore and describe these efforts in Africa in order to upscale surgical training and rehabilitation services.
METHODS:
A PubMed search for articles on ETV and CPC as management of SBHCP in Africa was performed. Two authors appraised the results for key themes in content: indications, technique, outcomes, complications, education, and rehabilitation.
RESULTS:
Twenty of 47 articles identified were included for appraisal. Twelve described indications, ten and seven outlined technique and complications, respectively, and four described predictors of operative success. Fourteen studies describe outcomes, including operative and neurodevelopmental outcomes. Only two outlined educational efforts. Half of the literature stems from a single site in Uganda; in total, only six countries were represented. No articles described significant post-operative rehabilitation services or related training.
CONCLUSION:
The experience of ETV and CPC in Africa is promising, however, efforts to train and empower local staff in surgical technique and methods to upscale post-operative community-based rehabilitation services remain as a key to long-term success.
Studies identified and appraised by main themes addressed
Studies identified and appraised by main themes addressed
Myelomeningocele affects around 1/1,000 newborns worldwide. Although statistics from low-income countries are sparse, given the regional nutritional deficits, the incidence in Africa likely is at least as high as that reported elsewhere [1]. Spina bifida associated hydrocephalus (SBHCP) is often encountered among these individuals. The exact incidence varies by study but is present in the majority of individuals with myelomeningocele [1, 2]. This represents a significant burden in hydrocephalus-related disease in Africa [2]. In middle and high-income countries, following the Management of Myelomeningocele Study (MOMS), prenatal management evolved, decreasing the need for cerebrospinal fluid (CSF) diversion when such was undertaken [3]. In Africa however, postnatal repair remains the norm.
In low resource settings, care for individuals with SBHCP is laden with risk. High ventriculoperitoneal shunting (VPS) failure rates and infectious morbidity [1] make VPS a suboptimal choice in Africa. Increasing international evidence has set forth the endoscopic third ventriculostomy (ETV) with or without choroid plexus cauterization (CPC) as a safe, effective, and affordable alternative to VPS [4, 5, 6, 7]. Concurrently, the World Health Organization (WHO) advocates for the role of community-based rehabilitation for children with disabilities in resource-constrained settings [8]. Along with surgical intervention, community-based rehabilitation has shown to have a significant impact on survival among this population [1]. Thus, alongside surgical interventions, community-based support and follow-up has proven to be life-saving in these settings. Given the known success of surgical interventions coupled with community-based rehabilitation, the purpose of this study was to explore and describe the use of ETV, with and without CPC (ETV/CPC) in Africa in order to encourage the upscaling of surgical training and rehabilitation services.
Methods
A PubMed search from 1959 through January 2017 was conducted. Terms included “Endoscopic Third Ventriculostomy”, “ETV”, “Africa”, and “Hydro- cephalus”. Selected articles included case reports, series, or cohorts where ETV was a key surgical technique in SBHCP. We included articles in English, Spanish, and French. Articles were excluded if they did not reference ETV or were conducted outside of Africa. Included articles were appraised by two of the authors to identify key themes relevant to SBHCP: indications, technique, outcomes (morbidity, mortality, re-intervention, and neurodevelopment), complications (intra- and post-operatively), education (information regarding surgical training initiatives), and use of post-operative rehabilitation services.
Frequency of publications by African country of origin. Piquer et al. [9] (multi-national study) is not included.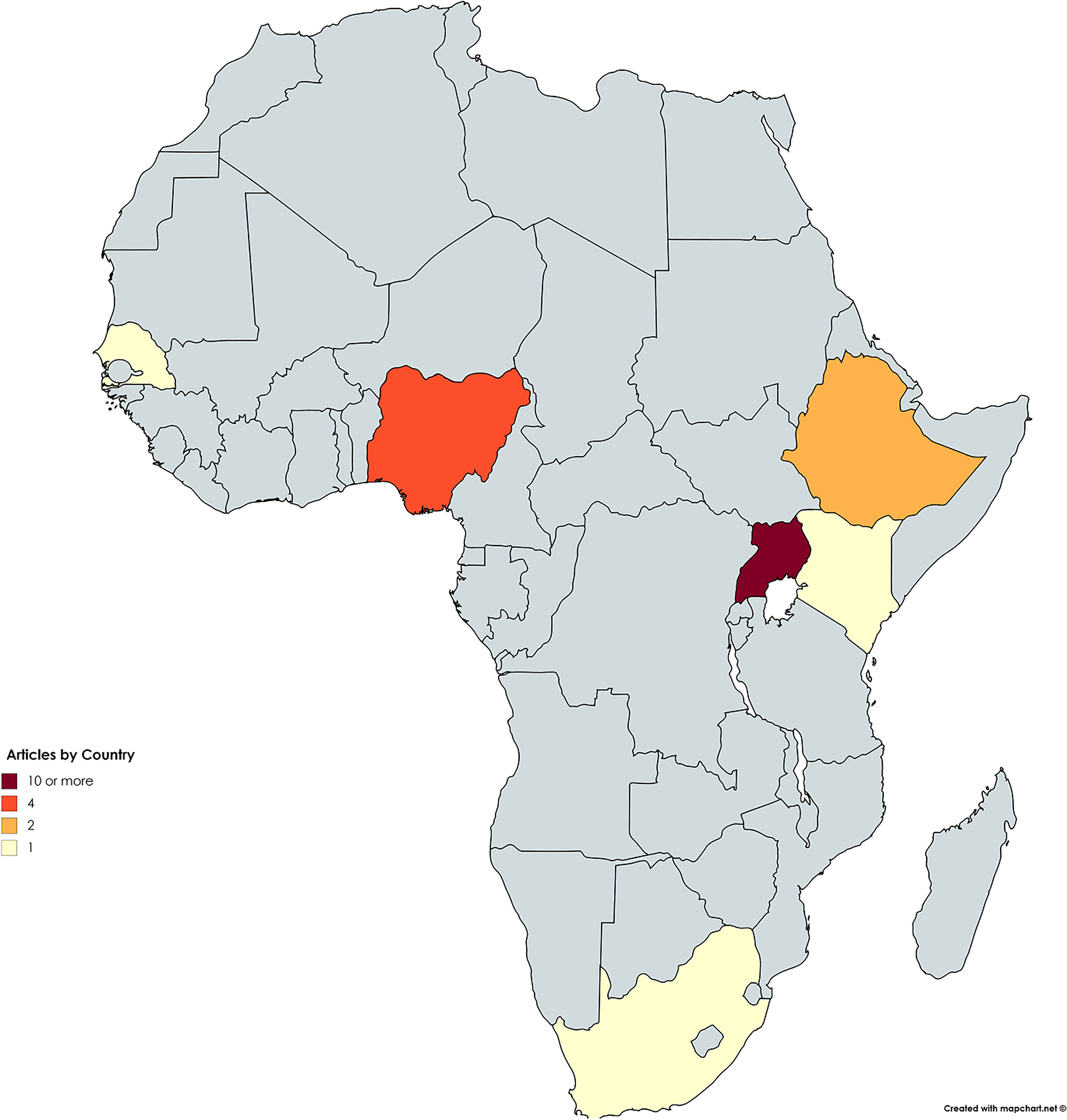
Forty-seven articles were initially identified. Of these, 57% were excluded as
unrelated to SBHCP or because they focused on a different geographical region. Twenty
articles were reviewed; the central themes of these were identified (Table 1). The studies described originated in Uganda
Success rates for ETV and ETV/CPC
Success rates for ETV and ETV/CPC
Twelve articles described surgical indications as a combination of clinical exam findings. Subsequent confirmatory imaging included use of trans-fontanellar ultrasound and computed tomography; several studies noted limited access/use of MRI [13, 14, 15, 16]. One study outlined patient selection and indications for surgical approach, establishing how ETV became the standard for all candidates in Uganda [13]. Surgical technique was outlined in ten articles. Ugandan studies initially predating the introduction of CPC provided information solely on ETV technique [17, 18]; the use of CPC thereafter was detailed in a later study [10]. Similarly, two Nigerian [14, 19] and two Ethiopian studies [20, 21] described their use of ETV and ETV/CPC respectively.
Surgical outcomes
Thirteen articles described outcomes. Success rates, defined most often as the absence of additional need for alternative CSF diversion technique at 6-month follow-up, were described in eight studies (Table 2) [10, 12, 14, 17, 18, 19, 21, 22]. A single study by Laeke et al. in Ethiopia instead reported a 58.3% four-week failure rate in 12 patients with SBHCP following ETV alone [20].
Four studies describe predictors of success and failure in ETV and ETV/CPC. A retrospective analysis of 979 ETV cases (591 failures, including 281 intraoperatively aborted procedures and 12 deaths) led to the development of a prediction model/scoring system utilized in subsequent studies [23]. The ETV success score encompasses nine items among three domains, with a maximum score of nine. One study targeted hazard ratios for intraoperative ETV failure contingent on aqueductal patency and cisternal scarring; among others, SBHCP (HR 0.76), a closed aqueduct (HR 0.66) and an unscarred cistern (HR 0.44) were statistically significant intraoperative predictors of success [24]. Another study in Uganda targeted factors for success of repeat ETV following initial failure in 316 patients. Among 41 cases with SBHCP, factors such as late failure of initial ETV (after 6 months, HR 0.14) and use of ETV/CPC in the initial procedure vs. ETV alone (HR 0.51), were deemed statistically significant [25]. A single South African study of 63 patients with mixed etiology described intracranial pressure monitoring via external ventricular drains for 72-hours post-operatively; the estimated positive and negative predictive values for ETV failure were 76.3% and 100%, respectively [26].
Seven studies, none specific to SBHCP patients, referenced intra- and
post-operative complications including death (up to one month post-operatively). Mortality
for ETV ranged between 1.8 and 1.9% [17, 18]. Complications included infection (wound site
and ventriculitis,
Rehabilitation and long-term outcomes
One study in Uganda looked at neurocognitive outcomes of ETV treatment in
93 patients with SBHCP between 5 and 52 months [11]. Recipients of either ETV/CPC (
Education and training
While three studies [10, 13, 22] referenced surgical training efforts undertaken locally, only two studies provided a robust description. The Neurosurgery Education Program (NED) for treatment of hydrocephalus in Africa described 38 ETV training missions carried out in 21 hospitals over seven countries [9]. Through seminars, conferences, hands-on courses, and supervised surgeries within local hospitals, training for 72 local surgeons (including general surgeons and neurosurgeons) and 122 nurses was provided related to aspects of technique and post-operative care. The content described included neuroendoscopic procedures, sterilization techniques, and equipment maintenance. Only 19 cases of ETV for SBHCP were described as performed, with success ranging from 45 to 50%. Twenty surgeons continued using ETV. After 2009, a neurosurgical training program established in Kenya and Zanzibar was described, which increased the number of surgeons in the region from 21 to 40. One study described differences in performance between resident and neurosurgeon-led interventions in a newly developed neurosurgical care program in Nigeria (which yielded a total of 15 new neurosurgeons), but no description of training structure or case volume was provided [20].
Discussion
There is growing experience in the use of ETV and ETV/CPC in Africa among individuals affected by hydrocephalus including those with SBHCP. Although the majority of studies describe surgical outcomes; the description of post-surgical outcomes, surgical training, or provision of rehabilitation services is wanting. While most studies cite ongoing support from institutions in the United States, it is notable that most of the available literature stems from the CURE Uganda project. Few other sites in Africa have provided additional accounts and there is a paucity of information from the rest of the continent.
Partly due to resource availability, patient selection protocols and diagnostic studies were dissimilar to those available to sites in middle and high-income countries, possibly contributing to differences in success and failure rates. A study by Kulkarni et al. of 1,597 ETV cases included 155 patients with SBHCP: 117 (12%) in Uganda and 38 (6%) in high-income countries; all failures, regardless of etiology, amounted to 62.1% in the former and 42.6% in the latter. Intraoperatively aborted procedures rates were 28.7% in Uganda and 1.9% in high-income countries [13]. As a whole, this suggests that the favorable impact of ETV in Africa is attenuated by limitations in patient selection, surgical skill, and pre-and intra-operative resources.
While several initiatives have been established to further the availability of ETV care in Africa [5, 27], only a few programs have published detailed longitudinal information regarding their educational process and the related outcomes of their local trainees. The existing programs are largely supported through outside resources rather than through national initiatives sustained by local institutions or governments [20, 28]. Though these resulting training sites must be credited for increasing the regional availability of surgeons and generating a net positive impact, there is virtually no information regarding long-term educational outcomes once the programs become autonomous.
Postoperative morbidity/mortality and success/ failures were affected by perioperative patient status, nutritional status, and adverse psychosocial circumstances – including neglect [12, 17]. This finding highlights the need for coordination of care through community based-rehabilitation services to be available beyond surgical care to foment positive long-term neurodevelopmental outcomes. Furthermore, substantial obstacles to consistent patient follow-up after post-operative discharge were also noted. The loss to follow-up by one month post-operatively was reported to be from 2 to 16% [17, 21] and attrition by 6 months was 10 to 30% [17, 23]. Despite the need for comprehensive longitudinal care, no study significantly addressed the use of community-based rehabilitation services. These two realities represent areas where urgent change is needed, where additional training and community engagement is required to support sustainable comprehensive care [28, 29], following models that already are proven to be widely successful in other settings [30, 31].
Our study has several limitations common to literature reviews, such as potential for missing data not identified through the search algorithms, as well as those unique to descriptive works in low-income countries where potentially existent realities are often not completely described in the medical literature. Additionally, given the surgical nature of most articles, the description of comprehensive training efforts and the use of community-based rehabilitation may have been underreported.
Conclusion
The experience in ETV and ETV/CPC in a resource-constrained setting is growing in Africa. It also continues to yield outcomes comparable to VPS, while decreasing complications and costs. Given its clinical advantages, it would appear to be an appropriate option to be up-scaled throughout the region. However, in light of strong recommendations by the WHO to leverage community-based rehabilitation in developing countries it is unexpected that, if present, this review (albeit of the surgical literature) did not find it widely reported. Thus, future efforts and research in regards to education, practice, and up-scaling of community based rehabilitation is certainly warranted.
Footnotes
Conflict of interest
The authors have no conflicts of interest to report.
