Abstract
PURPOSE:
To describe pulmonary function and determine the impact of neurological level, scoliosis, and obesity on pulmonary function in people with spina bifida (SB).
METHODS:
Participants with SB (
RESULTS:
Distribution of category of impairment in pulmonary function was: 55%
(
CONCLUSIONS:
High prevalence of restrictive pulmonary physiology is present in people with SB, with more rostral neurological levels and greater degree of scoliosis associated with a higher degree of pulmonary function impairment.
Keywords
Background and purpose
Spina bifida results from failure or incomplete closure of the neural tube during embryogenesis; the estimated incidence in the United States is 3.50 per 10,000 live births [1]. Life-long mobility impairments result from myelomeningocele, the most severe form of spina bifida. Assistive devices (e.g., wheelchairs, braces, crutches) are often required to accommodate mobility impairments resulting from the denervation of the sensory and motor nerves at and below the spinal lesion. Spina bifida can also lead to secondary conditions that require collaborative multidisciplinary medical care, including hydrocephalus, Chiari II malformation, renal dysfunction, neurogenic bowel and bladder, neuromuscular scoliosis, lower extremity joint contractures, and pelvic obliquity [2, 3, 4]. The risk of obesity, hypertension, cardiovascular disease, metabolic syndrome, pulmonary complications, and sleep disordered breathing are also high [5, 6, 7, 8, 9, 10, 11].
In people with spina bifida, pulmonary dysfunction is understudied despite the
fact that pulmonary complications are a source of morbidity and mortality in this
population [12]; pneumonia (9%,
Commonly occurring secondary conditions in people with spina bifida that could contribute to pulmonary impairment include scoliosis, obesity, denervation of the internal intercostal musculature (muscles that aid in inspiration), and denervation of the abdominal and external intercostal muscles (muscles that aid in expiration) [14].
Scoliosis may impact pulmonary function and increase the work of breathing in
neuromuscular conditions through reduction of chest wall compliance, uneven lung expansion,
and ineffective length-tension relationship of the respiratory muscles affecting their
actions on the rib cage [15, 16]. Scoliosis (defined as Cobb angle
Obesity could also contribute to pulmonary restriction by reducing chest wall compliance and interfering with diaphragmatic excursion [14, 19]. Obesity is prevalent (35%) in adults with spina bifida [11, 14]. In addition, obesity increases the risk of cardiovascular disease, metabolic syndrome, hypertension, and sleep disordered breathing [6, 7, 8, 10].
Denervation of the inspiratory musculature of the thorax can reduce chest wall
expansion resulting in a decrement in total lung capacity (TLC) and forced vital capacity
(FVC) known as restrictive lung impairment [19].
Denervation of abdominal musculature can decrease cough effectiveness and impact expiratory
reserve volume, contributing to a reduction in forced vital capacity (FVC). Reduction in FVC
in the absence of TLC reduction is commonly termed spirometric restriction [20, 21,
22, 23]. Studies to understand pulmonary function in people with spinal cord injury have
been completed [19, 24, 25, 26] however, there are a limited number of studies
that have explored the pulmonary function of people with spina bifida. Sherman et al. found
that 58% (
The first aim of this study is to describe the pulmonary function of adolescents and adults with spina bifida based on the results of spirometry and plethysmographic lung volume testing. The second aim of this study is to determine the impact of neurological level of spinal injury, scoliosis, and obesity on the severity and pattern of lung function impairment through univariate and multiple regression analysis.
Methods
This observational cross-sectional study was conducted at a large university based laboratory. Following approval by the University of Pittsburgh Institutional Review Board, participants were recruited through flyer mailings, advertisements, and local pediatric and adult spina bifida clinics. All participants signed an informed consent. The inclusion and exclusion criteria for the parent study which also assessed upper extremity exercise capacity were published elsewhere [27].
Eligible participants were: (a) age 13–80 years, (b) diagnosed with spina bifida (not spina bifida occulta without neurological impairments), (c) had scoliosis, and (d) were unable to pedal a standard (two-wheel) bicycle. Potential participants were excluded if they had (a) a history of recent or acute cardiopulmonary conditions that precluded safety of exercise testing (e.g., myocardial infarction, pneumothorax, active pneumonia, or use of a ventilator), (b) a history of conditions that precluded safety of load incremented arm ergometry exercise stress testing (e.g., upper extremity injury, upper extremity or thoracic surgery in the last 6 months, loss of shoulder, elbow, and/or wrist range of motion), and (c) had a medical condition that would contraindicate arm exercise stress testing as indicated by a primary care physician. After the primary care physician’s written medical release was received, participants were scheduled for pulmonary function testing and arm ergometry exercise stress testing. This paper addresses the pulmonary function testing.
Outcome measures
During the visit, sociodemographic information, body composition, and
functional mobility measures were gathered. Sociodemographic variables included race,
gender and diagnosis. Body composition included weight, arm span, and body mass index
(BMI). Weight was measured using a wheelchair accessible scale. Overestimation of BMI can
occur with spina bifida patients who are more likely to have reductions in height due to
scoliosis, pelvic obliquity, and lower extremity joint contractures. Therefore, arm span
was used as a proxy for height in the BMI formula (kg/m
A medical chart review was also conducted dating back to the first entry
for each participant in order to document a history of comorbid conditions associated with
spina bifida that may affect breathing including Chiari II malformation, sleep apnea, and
primary lung conditions such as pneumonia. Neurological level was calculated from physical
exam findings using the American Spinal Injury Association Impairment Scale (AIS):
International Standards for Neurological Classification of Spinal Cord Injury [30, 31].
Cobb angle [32] was calculated from scoliosis
radiographs. When scoliosis was too severe for an angle to be calculated, scoliosis was
categorized as “severe”. When no radiograph was available (31%,
Pulmonary function testing was completed by experienced respiratory technicians using a SensorMedics V6200 Vmax Auto Box Respiratory Analyzer (SensorMedics Corporation, Yorba Linda, CA). Pulmonary function measures were conducted at the University of Pittsburgh Emphysema COPD Research Center. The data collection procedures were defined prior to the start of the study and data were recorded in a protocolized manner. Pulmonary function testing (i.e., spirometry and body plethysmography determination of lung volumes) was completed according to the American Thoracic Society and European Respiratory Society Task Force (ATS/ERS) pulmonary function standards and interpreted using standard prediction equations by an experienced pulmonologist (FS) [33, 34, 35, 36]. Arm span was used as a proxy for height in the calculation of predicted values [5]. As reported in the parent study publication, participants also completed incremental arm ergometry testing [27].
Analysis
Test results were classified as restriction, spirometric restriction,
normal, or mixed (obstructed and restricted). Restrictive lung disease was defined as TLC
Sociodemographic and disease characteristics of individuals with spina bifida
Sociodemographic and disease characteristics of individuals with spina bifida
Key:
Body mass index was classified into four categories: Underweight
(
Statistical analyses were performed using IMB SPSS version 22.0 for
Windows (IBM Corporation, Armonk, NY, USA). Alpha was set at
Univariate analyses using Spearman’s rho were conducted to analyze the
relationship between pulmonary function measures (i.e., FVC, FEV
Results of pulmonary function tests for all participants by type of lung condition
Key: FVC: forced vital capacity; FEV
Distribution of restricted versus non-restricted participants classified by level of lesion, scoliosis and body mass index
Key: PFTs – Pulmonary condition or normal based on pulmonary function tests; deg.
Characteristics of participants
Participants were 29 individuals (15 females; mean
Univariate linear regression analysis (each variable was included separately in the
regression model),
29
Univariate linear regression analysis (each variable was included separately in the
regression model),
Key: %: percent; DVs: dependent variables; SE: standardized error; FVC: forced
vital capacity; FEV
Final model using multiple linear regression analysis,
Key: %: percent predicted; DVs: dependent variables; SE: standardized error; FVC:
forced vital capacity; FEV
The distribution of category of pulmonary impairment for the cohort
(
Spirometry and pulmonary function outcomes for people with spina bifida with
lumbosacral and thoracic neurological level compared to predicted normal total lung
capacity. Key: TLC 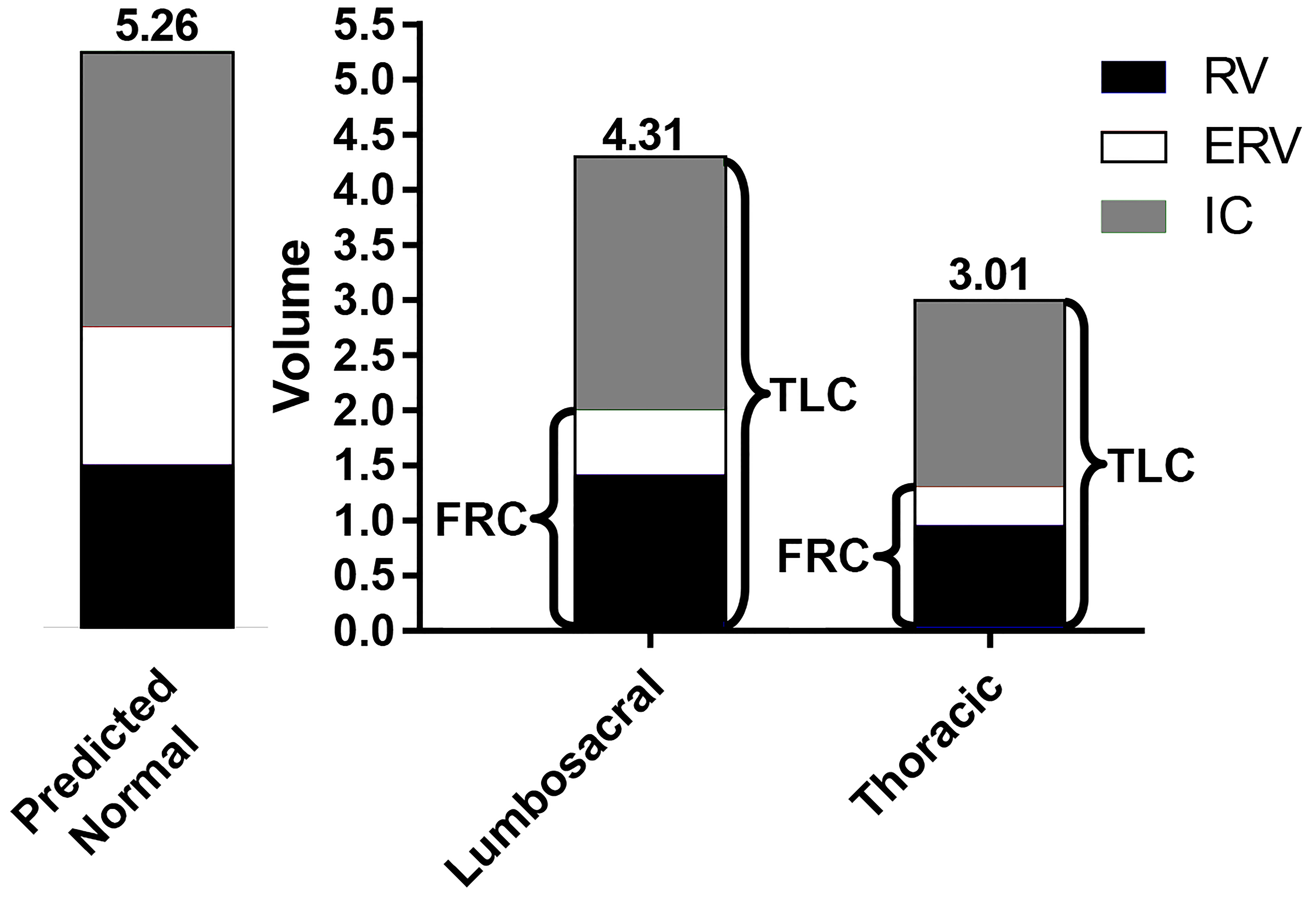
Univariate analysis showed a significant inverse correlation between level
of lesion and scoliosis and all pulmonary metrics, FEV
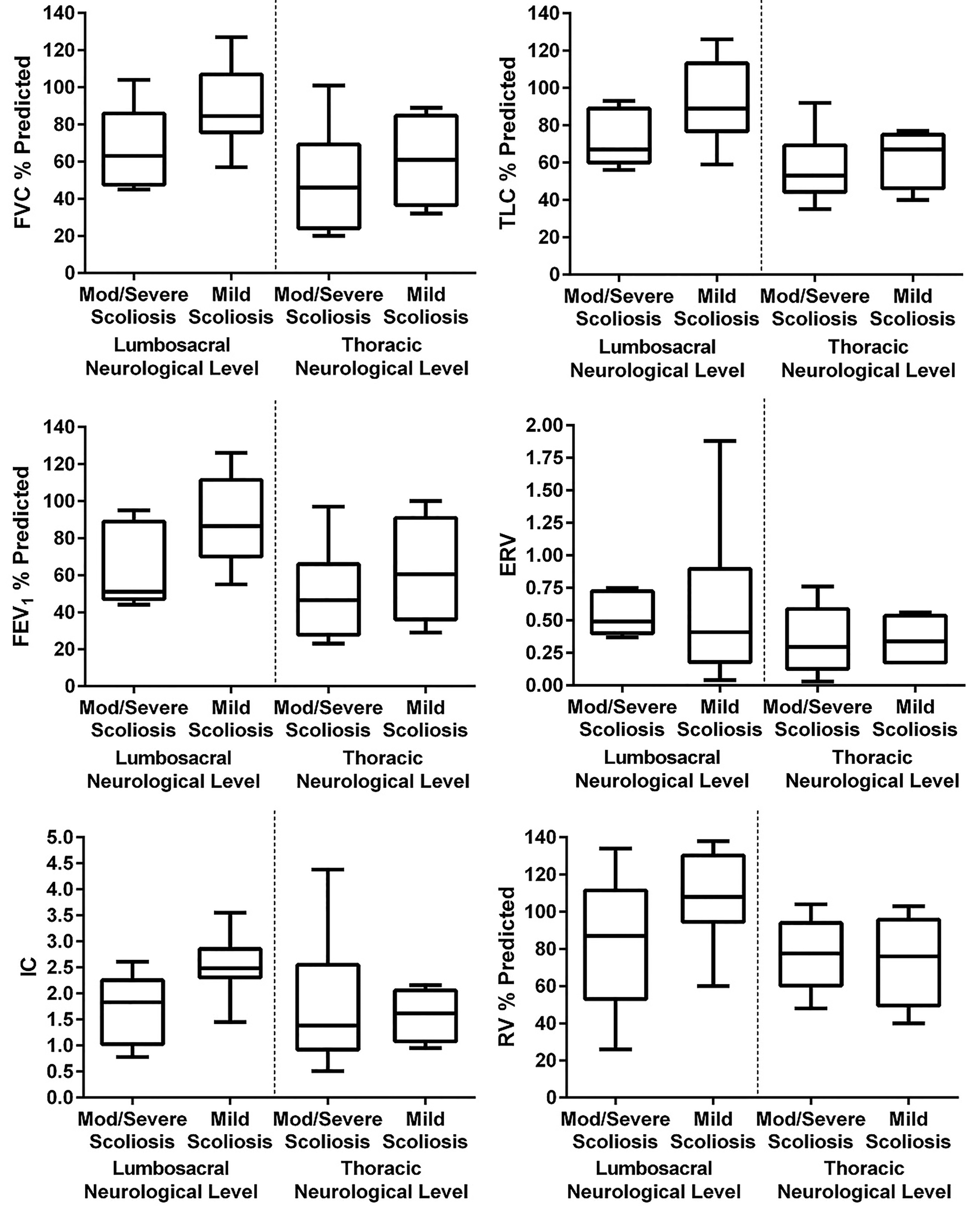
Box plots of group means of PFT’s in people with spina bifida with mild or
moderate/severe scoliosis coupled with lumbosacral or thoracic neurological level.
Box Plots of lung function parameters demonstrate more severe impairment in all
measures in patients with thoracic vs. lumbar neurological level lesions and
indicate that scoliosis severity results in an independent impact on lung function
that compounds the pulmonary impairment for any neurological level. Key: FVC
In multiple linear regression models for FEV
Review of findings
Restrictive lung impairment is common in patients with spina bifida, with
90% of patients who have lesions at the thoracic level experiencing restrictive lung
physiology. Neurological level (more rostral lesions) and scoliosis were significantly
related to FVC, FEV
Comparison of study findings to literature
The findings from this study (55% restricted, 7% spirometrically
restricted,
The findings of level of lesion and scoliosis as predictive factors for
pulmonary function were theorized to be true based on past literature [4]. The high prevalence of restriction in people with thoracic
spinal lesions and the strong significant relation of neurological level with pulmonary
metrics (i.e., FEV
The combined effect of scoliosis with neurological level should also be
considered in the treatment of spina bifida based on the results from this and other
studies [15]. Individuals with neurologic
conditions like spina bifida are at greater risk for hospitalization from respiratory
infections including pneumonia and bronchitis. Those with co-occurring conditions like
scoliosis have the highest rates of hospitalizations from respiratory infections [13]. Therefore, understanding the relationship
between pulmonary function and scoliosis could have lifelong health implications for
people with spina bifida. For children with spina bifida, decisions for the treatment of
neuromuscular scoliosis are often based on preventing decline of respiratory function (FVC
falling below 40%); spinal fusion is an option [4]. For adults, surgical intervention would be less likely as growth has
stopped, fixed spinal deformities may have developed, and spinal fusion surgery may have
been completed as a child (e.g., 31%,
Contrary to this study, Patel et al. found no association of scoliosis with pulmonary restriction [45]. One explanation could be that the retrospective nature of their study did not allow for examination of testing quality, and that their study included only spirometry but not plethysmographic lung volume testing. In addition, all the participants were children compared to our cohort who were primarily adults. Although age could have been a factor, we found that the regression models were not affected by age. Another reason for the difference in results could be that the present study included full-time wheelchair users. For people with spina bifida, a wheelchair seating system that lacks customized postural support could compound oxygen transport impairments by contributing to poor posture, fatigue of respiratory musculature, hindrance of chest wall and diaphragmatic excursion [4, 16, 45, 46]. The participants in this study used customized manual and power wheelchairs provided through a multidisciplinary assistive technology clinic involving a physiatrist, physical or occupational therapist and assistive technology certified wheelchair supplier, which is best practice for providing assistive technology [47]. Because best practice was followed for wheelchair provision in our participants, body position in the wheelchair would be less likely to contribute to pulmonary dysfunction.
We have further identified the impact of neurological level on the components of lung volume that contribute to restriction (Fig. 1). Individuals with thoracic level lesions had the greatest reductions in TLC and FVC related to substantial reduction in IC, most likely impacted by weakness in the muscles of inspiration as well as ERV impacted by the muscles of expiration, including the abdominal muscles. Lumbar level lesions, on the other hand, resulted in less impact on TLC due to more isolated impact on the abdominal muscles of expiration impacting ERV but not impacting IC (Fig. 1). In fact, two patients with lumbar lesions had spirometric restriction represented by isolated reduction in FVC with preserved TLC which is consistent with isolated impact on the muscles of expiration but not inspiration. This is particularly notable since the underlying mechanisms resulting in spirometric restriction are not fully understood [38, 48]. The observation of this spirometry pattern in only low level spinal defects supports an etiology of isolated expiratory muscle impairment as a clinical condition resulting in this pattern of lung function impairment, thus clarifying the gap identified in the Enright editorial [35].
Strengths and implications
This study was the first to measure pulmonary function in a diverse sample that included mostly adult (93%) wheelchair users (86%) from a wide age range (17–71 years) with spina bifida. We further advance the field by defining the independent pathogenic contributions to pulmonary impairment in SB. In addition, we offer a more granular understanding of the mechanisms leading to restrictive lung impairment in spina bifida by describing the plausible associations between neurological level and impairments in the inspiratory and expiratory lung volume partitions.
Limitations
The study results primarily apply to a population of wheelchair users with
spina bifida. This more neurologically involved population may not be representative of
the broader population of people with spina bifida who have comparatively more functional
impairment. In fact, this study included 44% (
Clinical implications
Clinicians who are treating a person with thoracic level spina bifida and scoliosis for a musculoskeletal condition, or for physical deconditioning, should be aware that the risk of pulmonary dysfunction is high. Clinicians can estimate the likelihood of pulmonary restriction in their patients using the regression equations developed in this study. Referral to a pulmonologist may be warranted. A relevant treatment aspect to these observations is that pulmonary restriction could be amenable to treatment with respiratory muscle strength training (RMT) [16, 50, 51, 52, 53]. Studies in persons with spinal cord injury have shown that RMT which included resisted breathing weight lifting or normocapnic hyperpnea, showed trends for improving expiratory muscle strength and vital capacity [54]. In persons with neuromuscular disorders (i.e., Duchenne’s muscular dystrophy) inspiratory RMT improved postoperative FVC; in addition, RMT conducted and controlled through video games improved lung function in this population [55, 56].
Future studies
Future directions should include investigation into the effects of
wheelchair positioning and standers on pulmonary function in people with spina bifida.
Ideally, studies that utilized radiographs should use standardized positioning and
calculation of Cobb angles, with one radiologist completing the measures to reduce
measurement error. Kyphosis measurements should also be included, based on the strong
significant inverse association found between kyphosis and FEV
Conclusion
Pulmonary restriction was common in this cohort of people with spina bifida,
with more rostral neurological levels associated with a higher degree of pulmonary function
impairment than more caudal levels; restrictive pulmonary impairment was observed in the
majority (90%,
Footnotes
Acknowledgments
Funding for this study was provided by the Spina Bifida Association and Ashley Rose Foundation through the Spina Bifida Association Young Investigators Award. This paper is written in honor of Ashley Rose, the beloved daughter of Mr. and Mrs. Raymond and Linda Pitek who had spina bifida. Special thanks to Dr. Ann Spungen, James J. Peters Veterans Affairs Medical Center, Bronx, NY, for initial concept, Dr. Christina Zigler, Department of Physical Medicine and Rehabilitation, University of Pittsburgh School of Medicine, for assistance with statistical analyses and presentation of tables and Chad Karoleski at the University of Pittsburgh, Emphysema COPD Research Center for assistance with statistics and presentation of graphics.
Conflict of interest
The authors have no conflict of interest to report.
