Abstract
BACKGROUND:
There is currently no widespread implementation of pharmacogenetic testing (PGx) methods in the practice of phthisiology service.
OBJECTIVE:
The aim of this study is to determine how informed and prepared phthisiologists, residents, and postgraduate students of the Russian Medical Academy of Continuing Professional Education (RMACPE, Moscow) use PGx techniques in their work to improve treatment safety, predict the occurrence of adverse reactions (ADRs), and personalize therapy.
METHODS:
A survey was conducted among phthisiologists (n = 314) living in different regions of the Russian Federation and studying at RMACPE, such as residents and post-graduate students (n = 185). The survey was developed on the Testograf.ru web platform and had 25 questions for physicians and 22 for residents and post-graduate students.
RESULTS:
More than 50% of respondents are ready to use PGx in clinical practice and thus are aware of the method’s possibilities. At the same time only a small part of participants were aware of the pharmgkb.org resource. The absence of PGx in clinical guidelines and treatment standards, according to 50.95% of phthisiologists and 55.13% of students of RMACPE, the absence of large-scale randomized clinical trials, according to 37.26% of phthisiologists and 43.33% of students, and the lack of physician knowledge on PGx, according to 41.08% of phthisiologists and 57.83% of students, are all factors that prevent the implementation of PGx in Russia.
CONCLUSION:
According to the survey, the overwhelming majority of participants recognize the importance of PGx and are willing to use the method in practice. However, there is a low level of awareness among all respondents about the possibilities of PGx and the pharmgkb.org resource. The implementation of this service could significantly increase patient compliance, lower ADRs, and enhance anti-tuberculosis (TB) therapy quality.
Keywords
Introduction
According to the World Health Organization (WHO), tuberculosis is the most widespread socially significant disease worldwide. The annual mortality rate from tuberculosis is 1.2 million people [1]. The efficacy of tuberculosis treatment both in Russia and worldwide is rather low and amounts to 69.6% abacillation and 61.4% of destruction closure [2]. Poor drug tolerance from the high incidence of adverse reactions (ADRs) during treatment with TB drugs is a factor affecting such outcomes. However, about 20–60% of patients stop taking one or more TB drugs on their own, which contributes to relapse, continued bacterial excretion, collapse of lung tissue and increased spread of resistant mycobacteria strains.
Emerging ADRs can lead to disability and death if it is not identified and handled immediately [3,4]. The negative effect of ADRs on tuberculosis prognosis is associated with both a direct threat to patients’ health and life as well as an increased risk of treatment failure [5], which has worldwide importance.
One effective approach for dealing with this problem is through the implementation of PGx methods, which allow for both the consideration of individual patient characteristics and reduce the incidence of drug intolerance. Over than 5 million clinical annotations of medicines are already available on the website pharm.gkb.org, as well as 188 clinical recommendations for dosage based on PGx, including TB drugs.
The use of PGx methods in patients with tuberculosis may safely (the study is conducted in vitro) provide personalization of drug treatment and dosage, reduce the risk of ADRs, increase treatment tolerance, improve patient quality of life and the efficacy of TB treatments. Global healthcare could minimize the economic burden of tuberculosis treatment by decreasing the frequency of ADRs and the additional financial costs associated with them, which shows the obvious benefits associated with implementation of this approach.
However, there is currently no widespread implementation of PGx methods in the practice of phthisiology service, which may be due to the low awareness of specialists about the goals and capabilities of PGx methods. The authors’ belief that experienced phthisiologists and novice specialists have different levels of understanding about PGx’s goals and objectives formed the basis of the study’s hypothesis. The objective of the study was to examine the level of awareness and willingness of phthisiologists, both experienced and novice specialists - residents and post-graduate students of the Russian Medical Academy of Continuing Postgraduate Education (RMACPE), to implement PGx - testing methods in their work to improve treatment safety, predict the occurrence of ADRs and personalize patient therapy.
Materials and methods
Study design
The questionnaire (Supplementary Appendix) was created on the popular Russian Federation online service “Testograf.ru” and sent to individual e-mail addresses of specialists working in phthisiology and living in different regions of the Russian Federation. The voluntary and anonymous survey was conducted from December 20, 2021 to January 31, 2022 among physicians who are members of the Russian Society of Phthisiologists. Exclusion criteria were participants who did not express their voluntary participation in the survey. The survey included 314 participants. A survey of young physicians (n = 185) studying in clinical residency and postgraduate education at the Russian Medical Academy of Postgraduate Education in the wider field of “clinical medicine” was done simultaneously by the authors using the same methodology.
Questionnaire
The 25-question questionnaire was conducted in Russian and was divided into several distinct sections. The “general part” section consisted of several blocks. The first block included information about the respondents: gender, age, specialty, work experience, and region of residence (Q1–Q5). The following block was devoted to the general assessment of phthisiatricians’ and novice specialists’ awareness of the relevance of PGx, goals and objectives (Q6–Q10). The second section of the questionnaire included specific questions related to the pharmacogenetics of respiratory tuberculosis (Q11–Q22). The third section of the questionnaire « Patient Interaction » (Q23–Q25), was answered by practicing phthisiologists. Post-graduate students and residents of RMACPE answered only the first 22 questions. The researchers offered only one answer choice. The exception was Q22 of the questionnaire, where it was possible to give several answer options, if necessary. The researchers only allowed one response option for each question, apart from Question 22, where respondents could select multiple answers if necessary.
The survey was tested on a cohort of ten highly competent phthisiologists to authenticate its validity prior to being conducted. After a thorough evaluation, the survey questions proved to be suitable for sociological research and provided us with the data needed to understand the respondents’ understanding of PGX objectives.
Statistical analysis
The results were statistically processed using StatTech v. 1.2.0 (developed by “Stattech” LLC, Russia) and Excel 10 program. To determine a statistically significant difference in the responses of specialists employed in the phthisiology service and young physicians of RMACPE without work experience, the chi-square test (x 2) was conducted, with a significance level of p < 0.05.
Research limitations
Our survey had some limitations. Firstly, it was conducted through an online platform after sending emails to specialists in advance. It is unknown how many people clicked on the survey link, which makes it impossible to calculate the response rate. Secondly, most phthisiologists were represented by older specialists whose undergraduate education did not include information about the goals and objectives of PGx research. Such specialists have selective postgraduate advanced training in pharmacogenetics. The RMACPE residents and post-graduate students who were being compared, however, were given information about PGx by including relevant info in the basic and varied modules of educational programs during undergraduate and graduate education at medical universities, as well as during postgraduate education at RMACPE also during postgraduate and residency training. Thus, the authors made the assumption that the survey findings for those who responded to the invitation to participate in this study may be random.
Results
A total of 499 specialists from 21 cities of the Russian Federation participated in the survey (Table 1). According to the study design and the data presented in Table 1, the participants were divided into specialists working in the phthisiology service who had sufficient work experience - n = 314 (62.92%) - and novice specialists without experience who were enrolled in post-graduate and residency education at RMACPE - n = 185 (37.08%).
General characteristics of respondents
General characteristics of respondents
Among phthisiologists, there were 252 (19.74%) women and 62 (80,25%) men. The respondents were primarily over 45 (221; 70.38%) and had a total work experience of more than 10 years (n = 241; 76.75%).
In terms of gender, there were 56 (30.3%) men and 129 (69.7%) women among novice specialists without prior work experience. 129 (69.7%) of the respondents in this group were specialists under the age of 30.
The authors observe statistically significant differences in the respondents’ opinions for questions Q6, Q7, Q9 after analyzing the responses to questions Q6–Q10 of the questionnaire (Table 2).
Assessment of phthisiologists’ and novice specialists’ awareness on relevance of PGx studying, goals and objectives
Assessment of phthisiologists’ and novice specialists’ awareness on relevance of PGx studying, goals and objectives
In the RMACPE training group, 116 participants (62.7%) responded positively to the question Q6 about whether a patient’s genetic features might affect the treatment of tuberculosis, compared to 252 respondents (80.25%) who had work experience in psychiatry (p = 0.001; p < 0.05).
As compared to the group of experienced phthisiologists, post-graduate students and residents of RMACPE seemed to have the highest percentage of respondents who indicated that a patient’s genetic characteristics might affect their response to drug therapy in terms of efficacy and safety (Q7), at 168 (90.9%) versus 252 (80.25%) (p = 0.011; p < 0.05).
When asked question Q9, novice specialists responded more confidently, giving 84 (45.4%) responses as compared to 87 (25.51%) from phthisiologists with work experience, suggesting that they considered it necessary to include a bioinformatics course in the education systems of medical public universities as a required course (p = 0.001; p < 0.05).
In evaluating the level of awareness and use of a service called PharmGKB (Q11), the majority of respondents, including both experienced and novice phthisiologists — 235 (74.8%) and 140 (75.7%), respectively replied that they were not aware of this site (Table 3).
Special questions concerning the pharmacogenetics of respiratory tuberculosis
Special questions concerning the pharmacogenetics of respiratory tuberculosis
In response to question Q12 of the survey, which asked participants: “Please rate your knowledge of pharmacogenetics on a scale from 1 to 10” (Table 3), the authors found that more than 80% of participants gave their knowledge of PGx a rating of 1 to 5, with no significant differences between the two groups of participants (p = 0.835). This finding suggests that participants generally have a low level of awareness regarding the potential of PGx to personalize TB therapy, improve patient safety and TB treatment prognosis.
Regarding responses to question Q13 concerning the application of PGx by participants in both groups, the authors did not discover any statistically significant differences. Thirty-eight (12.11%) experienced phthisiologists and 30 (16.2%) novice specialists (p = 0.381) confirmed having such experience.
The authors found a significant difference in responses for question Q14 about the potential of the pharmacogenetic approach to help select a drug used in TB patients. In comparison to the group of phthisiologists with experience, the proportion of respondents who answered “yes” to this question was highest in the group of novice specialists, residents, and post-graduate students of RMACPE, at 152 (82.2%) versus 227 (72.29%) - p = 0.014 (p < 0.05).
The majority of participants who responded positively to question Q15 about whether the pharmacogenetic approach could help in selecting the regimen and dosage of medications used in patients also prevailed in the RMACPE novice group - 145 (78.4%) versus 204 phthisiologists with work experience (64.96%) - p = 0.001 (p < 0.05).
Both groups of respondents provided statistically significantly different answers to question Q16 about which class of drugs the use of PGx is most important (p < 0.05 for all answer options). However, the authors found that a majority of specialists with work experience, residents, and postgraduate students RMACPE believe that PGx is required when prescribing third-line drugs, including new and combined TB drugs, 179 (57.01) versus 153 (82.7), respectively (p < 0.001).
When asked Q17 whether PGx could help in choosing the regimen and dosage of medications used in patients, residents and post-graduate students of RMACPE responded more confidently than phthisiologists with work experience, with 145 (78.4%) versus 204 (64.96%), respectively (p < 0.001).
The authors found that 73.88% of phthisiologists and 78.4% students of RMACPE believed that PGx can prevent ADRs during TB drug use (Q18, p = 0.386).
At the same time, the dominant proportion of those interviewed among RMACPE trainees believed that the use of PGx could prevent NCDs when prescribing drugs of the second-line PTP 98 (53%), while half of the interviewed phthisiatricians with experience favored the basic drugs of the first-line - 157 (50.0%), p = 0.584 (Q19).
At the same time, the majority of RMACPE trainees thought that using of PGx could prevent ADRs when prescribing second-line TB drugs, with 98 (53%), while the majority of the experienced phthisiologists preferred the first-line TB medications, with 157 (50.0%), p = 0.584 (Q19).
As reported by the authors, the majority of respondents (62.74% of psychiatrists and 70.3% of RMACPE trainees) understood that PGx can minimize the economic burden by saving money to correct ADRs, (p = 0.218) (Q20).
The majority of participants 207 (65.92%) among experienced phthisiologists and 112 (60.5%) among novice specialists studying at RMACPE declared willingness to use PGx in their clinical practice to predict efficacy and safety of drugs used in treatment (Q21).
On Q22, the authors asked participants to choose among several options. Hence, the researchers discovered that the most common answer to the question of what factors restrict the use of PGx in real clinical practice among experienced phthisiatricians was “lack of PGx in clinical guidelines and treatment standards”, which was submitted by 160 (50.95%) respondents. Another response option, “ignorance of PGx by physicians”, was preferred by post-graduate students and residents of RMACPE, and was selected by 107 (57.83%) of the participants. Among experienced phthisiologists it was the second most frequently selected response - 129 (41.08%). The second most common response among RMACPE post-graduate students and residents was “lack of PGx in clinical guidelines and treatment standards.”, which was the response of 102 (55.13%) participants in this group. “No large-scale randomized clinical trials” was the second most common response among experienced specialists, with 117 (37.26%). Whereas RMACPE post-graduate students and residents identified “no economic reason for the usage of PGx” as the third most important response. Among the responders in this group, 99 (53.51%) showed agreement with this option.
Answers to questions Q23–Q25, were received by the researchers only from phthisiologists with work experience of interaction with patients.
The findings revealed that 110 (35%) physicians with work experience agreed with question Q23 of the questionnaire, “Do you consider the activities of patient organizations/communities to be effective in supporting physician work in implementing genetic research?” 169 (54%) respondents had no such experience, and 35 (11%) disagreed.
At the same time, more than half of the interviewed specialists agree that having patient schools for patients with respiratory TB, teaching how to live with the identified genetic features, is essential (Q24). This was the opinion of 169 (54%) of surveyed specialists.
The authors discovered that 179 (57%) phthisiologists responded affirmatively to the question Q25 “do you consider it relevant to create a digital service (mobile application) to support patients with respiratory TB and identified genetic features?” 97 (31%) had no such experience, and 38 (12%) disagreed with this opinion.
Discussion
A questionnaire developed by the authors was used to survey specialists, both those with work experience in the phthisiology service and post-graduate students and residents of RMACPE, in order to assess the opinion of Russian physicians in the field of PGx tuberculosis.
The authors’ primary hypothesis was that experienced phthisiologists and novice specialists vary in their knowledge of the goals and objectives of PGx. This hypothesis was kind of confirmed during the research process. For example, the researchers found that 252 (80.25%) phthisiologists and more than 168 (90.9%) graduate and post-graduate students and residents of RMACPE, believed that patient genetic features could influence their individual response to drug therapy in terms of efficacy and safety (Q7). In response to question Q9, novice specialists were more confident than experienced phthisiologists that a bioinformatics course should be included as a required subject in the curricula of medical educational institutions.
The majority of respondents who answered positively to question Q15, whether the pharmacogenetic approach can help in choosing the regimen and dosage of medications used in patients, also prevailed in the group of individuals studying at RMACPE.
Residents and post-graduate students seemed to have a statistically significant higher amount of positive responses to the question Q17 about whether PGx can help in choosing the regimen and dose of drugs used in patients.
The authors assumed that the predominance of older age group representatives (70.38%) among phthisiatricians and the absence of PGx subjects during their higher education can account for such statistically significant differences in the answers to these questions. While currently, PGx learning is being more and more integrated into the basic and varied modules of university educational programs.
We could not identify any available publications in the literature on a survey of phthisiology service specialists about the goals and objectives of PGx. A similar survey of physicians in the field of cardiovascular disease (CVD) PGx was conducted in the Russian Federation [6]. The authors discovered that a significant number of Russian physicians support PGx testing for prescribing cardiac drugs. Among the key factors preventing the implementation of PGx tests in clinical practice were physicians’ lack of awareness of PGx, the absence of PGx tests in clinical guidelines and treatment standards, and a lack of economic justification for the use of PGx methods [6].
According to a survey conducted in the United States, more than 97% of nonphthisiology physicians believe that genetic factors may impact individual response to pharmacotherapy [7]. According to studies conducted in the United Arab Emirates, Egypt, Zimbabwe, and Kuwait, survey participants (doctors, pharmacists, and students) showed a lower awareness of PGx researches, ranging from 41.7% to 56% [8–11].
The lack of specialized knowledge and skills, the lack of necessary equipment, limited funding, and the ethical component of research (violation of confidentiality and discrimination based on ethnicity) are among the main reasons that make it difficult to implement PGx in clinical practice in these countries.
According to the results of this research, the key reasons preventing widespread implementation of PGx in clinical guidelines and treatment standards are the lack of pharmacogenetic testing in clinical guidelines and treatment standards, the lack of large-scale randomized clinical trials, physicians’ lack of pharmacogenetic knowledge, and the lack of economic justification for the use of PGx (Fig. 1).
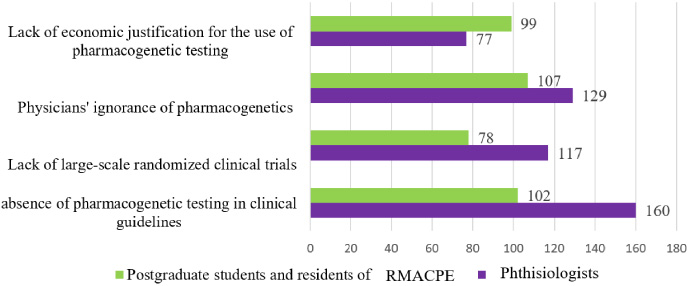
Respondents’ opinions on the problems preventing the implementation of PGx in real clinical practice.
The majority of respondents, including both experienced specialists and novice physicians, said they were unaware of the pharmgkb.org website, according to the researchers’ findings. Moreover, this database offers the results of large-scale randomized clinical trials, with validation of pharmaceutical doses determined by the genetic features of patients. The use of this service might significantly improve TB therapy quality, patient compliance, and reduce the amount of ADRs.
Despite the fact that the majority of respondents rated their knowledge of PGx from 1 to 6 points (on a 10-point scale), 38 (12.11%) phthisiologists and 30 (16.2%) RMACPE residents and post-graduate students have worked with pharmacogenetic testing. The ability to use PGx in the apparent lack of obvious clinical experience among postgraduate students and residents has seemed to be explained by the continuous work of the RMACPE winter and summer schools of young scientists on pharmacogenetics and personalized medicine under the guidance of RAS Academician D.A. Sychev, the presence of a science-intensive base at the RMACPE Institute of molecular and personalized medicine, and the extensive experience in teaching PGx at professional retraining and continuing education cycles.
In the authors’ opinion, the fact that a large majority of respondents believed that PGx testing should go along with the prescription of new, combined drugs rather than first-line medications is important. Furthermore, more than half of the respondents assume that PGx can prevent ADRs during pharmacotherapy and subsequently minimize the economic burden by saving money for their treatment. According to the Federal Clinical Guidelines for the Diagnosis and Treatment of Tuberculosis of the Respiratory System (2022), Order of the Ministry of Health No. 951 of December 29, 2014 “On approval of methodological recommendations for improving the diagnosis and treatment of tuberculosis of the respiratory system,” the main TB drugs of the 1st line are used for chemotherapy in primary drug-sensitive tuberculosis. The prevalence of ADRs is observed in every second patient when first-line TB drugs are used [12].
Since PGx prescribing is strictly regulated at the federal level, phthisiologists may believe that their variability of choice is limited. However, knowledge of individual PGx features of TB drugs could allow phthisiologists to individually adjust the prescription of chemotherapy drugs, increase the safety of such treatment for patients, and reduce the frequency of ADRs without violating federal clinical guidelines. Therefore, it is necessary not only to raise awareness of PGx capabilities and the pharmgkb.org resource, but also to develop guidelines for interpreting these results in the form of a decision-making system.
It seems that the following factors must be present for the successful implementation of PGx tests in the practical healthcare of the Russian Federation and, in particular, in the phthisiology service:
closer integration of clinical experience with modern, knowledge-intensive PGx knowledge, which is only possible with ongoing advancement of expert professional training; evidence-based pharmacoeconomic evaluation of the benefits associated with implementing PGx testing in scenarios significantly impacted by individual, genetic features of patients; the PGx tests’ inclusion in the federal clinical guidelines for the treatment and diagnosis of respiratory TB; development of decision-making systems that take into account PGx results; sufficient time factor, allowing the physician to see in practice the benefits of personalized medicine using PGx tests.
In order to increase the safety of pharmacotherapy, a survey was carried out in the Russian Federation among experienced phthisiologists, post-graduate students, and residents of RMACPE about knowledge and potential of PGx use in patients with TB. According to a survey, experienced phthisiologists and novice specialists are not equally aware of the PGx’s goals and objectives. The authors found that the majority of responders recognize the importance of PGx testing and are motivated to use the tests in clinical practice. All respondents, however, showed a low level of awareness on possibilities of PGx and the pharmgkb.org website, which provides the results of large-scale randomized clinical trials, with validation of drug doses determined by genetic patient features. The implementation of this service could significantly increase patient compliance, lower ADRs, and enhance TB therapy quality.
We hope that after gaining specialized knowledge about the prospects and benefits of PGx, the development of patient-specific decision-making systems, the inclusion of PGx in federal clinical guidelines, and the implementation of PGx methods in psychiatric services in Russia as well as worldwide will become more evident, which will improve the situation with low TB treatment efficacy.
Footnotes
Acknowledgements
All the specialists who participated in the survey are gratefully acknowledged.
Ethics statement
The study was approved at a meeting of the local ethics committee of the Russian Medical Academy of Continuing Professional Education of the Russian Ministry of Health (Minutes No. 12 of the meeting of the local ethics committee dated October 20, 2021). The authors state that they followed the principles outlined in the Declaration of Helsinki for all scientific research involving human subjects. The survey was informed and voluntary.
Conflict of interest
The study was performed within the state assignment of the Russian Medical Academy of Continuing Professional Education of the Ministry of Health of the Russian Federation “New Pharmacogenetic Biomarkers of Safety of Pharmacotherapy of Some Socially Significant Diseases R&D” 121110800062-6 “New Pharmacogenetic Biomarkers of Safety of Pharmacotherapy of Some Socially Significant Diseases” at EGISS. The authors state that the study was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
