Abstract
Background:
Multi-arm, multi-stage (MAMS) platform trials can accelerate the identification of disease-modifying treatments for Parkinson’s disease (PD) but there is no current consensus on the optimal outcome measures (OM) for this approach.
Objective:
To provide an up-to-date inventory of OM for disease-modifying PD trials, and a framework for future selection of OM for such trials.
Methods:
As part of the Edmond J Safra Accelerating Clinical Trials in Parkinson Disease (EJS ACT-PD) initiative, an expert group with Patient and Public Involvement and Engagement (PPIE) representatives’ input reviewed and evaluated available evidence on OM for potential use in trials to delay progression of PD. Each OM was ranked based on aspects such as validity, sensitivity to change, participant burden and practicality for a multi-site trial. Review of evidence and expert opinion led to the present inventory.
Results:
An extensive inventory of OM was created, divided into: general, motor and non-motor scales, diaries and fluctuation questionnaires, cognitive, disability and health-related quality of life, capability, quantitative motor, wearable and digital, combined, resource use, imaging and wet biomarkers, and milestone-based. A framework for evaluation of OM is presented to update the inventory in the future. PPIE input highlighted the need for OM which reflect their experience of disease progression and are applicable to diverse populations and disease stages.
Conclusion:
We present a range of OM, classified according to a transparent framework, to aid selection of OM for disease-modifying PD trials, whilst allowing for inclusion or re-classification of relevant OM as new evidence emerges.
INTRODUCTION
There is currently no proven intervention to delay the progression of Parkinson’s disease (PD). A number of novel and promising treatment approaches are being developed to address this and need to be tested in clinical trials. Multi-arm, multi-stage (MAMS) platform trials may help accelerate the identification of potentially successful treatments by improving efficiency of the clinical trial process. MAMS trials evaluate multiple agents simultaneously against a shared placebo arm and allow the addition of new arms as well as cessation of ineffective treatments at interim stages. However, there is no current consensus on the most appropriate outcome measures (OM) for disease-modifying trials in PD to be included in such an approach.
The Edmond J Safra Accelerating Clinical Trials in Parkinson Disease (EJS ACT-PD) initiative aims to accelerate the identification of disease-modifying treatments for PD through a MAMS platform trial approach. An important component of this novel approach is the identification and selection of appropriate outcome measures, suitable for inclusion across several different study arms as well as meeting the overarching aim. Here, we present an inventory of outcome measures based on current evidence and make initial recommendations for their potential inclusion as core, supplementary (depending on study arm) or exploratory outcome measures in such trials.
This inventory of potential outcome measures for use in disease-modifying trials is based on a consensus effort by an expert group with strong patient and public engagement input. The group used information from literature reviews, other existing and ongoing efforts, and discussion with regulatory bodies and group discussions. Particular consideration for inclusion in the inventory was given to clinically relevant outcome measures that are meaningful to patients, align with regulatory expectations and provide data to support adoption in larger healthcare systems. For future adaptation according to emerging new evidence, a framework was also created for evaluation and inclusion of outcome measures of potential relevance in the future, including clinical outcome measures, biomarkers, and novel measurement technologies.
METHODS
The methodology for this consensus paper is summarized in Fig. 1. A working group (WG) of experts from relevant fields, chaired by AS, was formed to review evidence, and provide expert input in written form and meetings. An initial list of outcome measures for inclusion in the inventory was compiled, based on 1) expert input from the members of the EJS ACT-PD Outcome Measures Working Group (OM WG), 2) the Movement Disorders Society (MDS) critique and recommendation papers, 3) the National Institute of Neurological Disorders and Stroke Common Data Elements (NINDS-CDE) version 2.0, 4) literature searches performed by CGR, 5) patient and public involvement and engagement (PPIE) input, and 6) a systematic review on disease-modifying trials in PD (Dr. Marie-Louise Zeissler, unpublished). Only outcome measures with published data in PD were included.
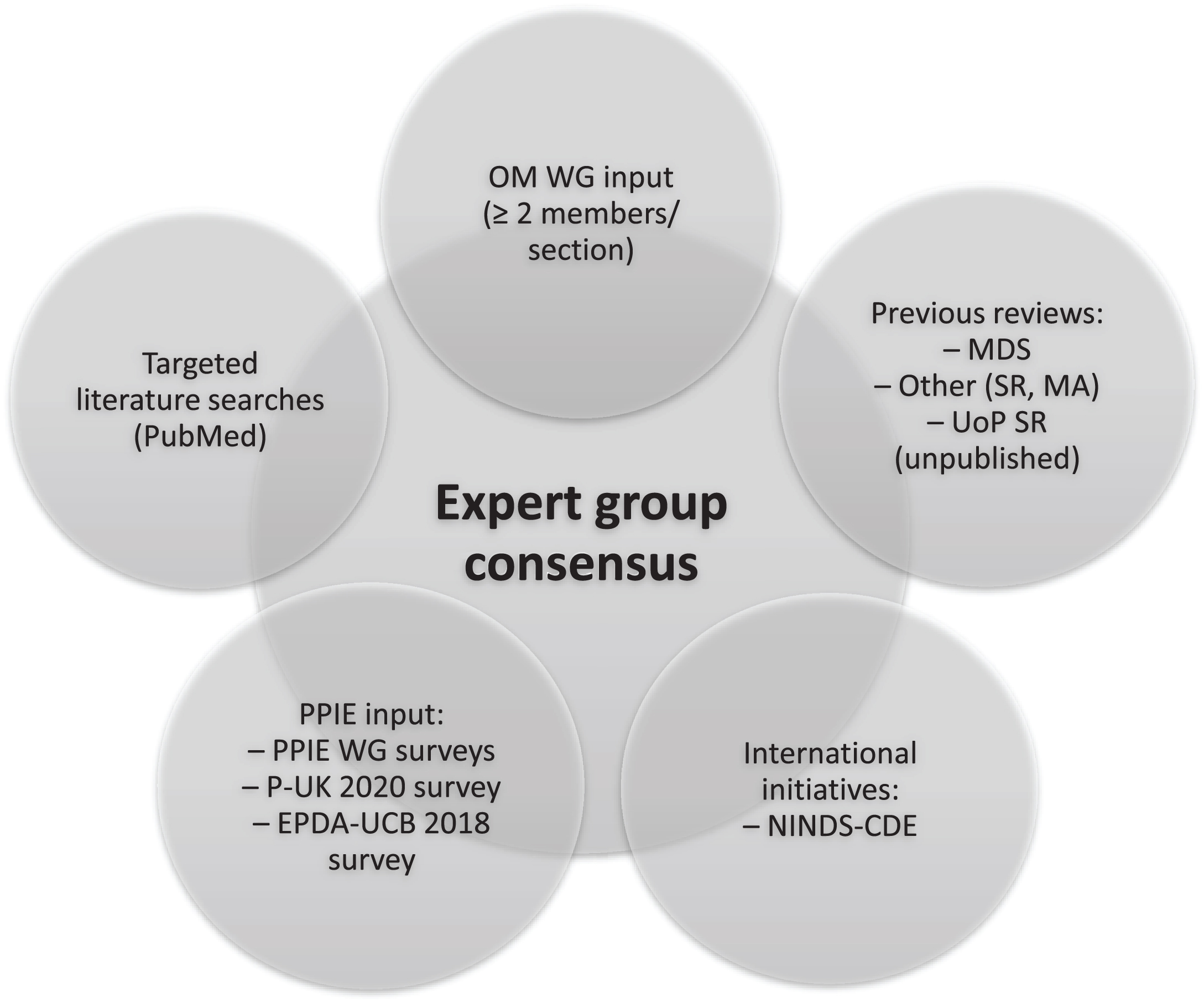
Sources for consensus of outcome measures in disease-modifying trials in Parkinson’s disease. EPDA-UCB, European Parkinson’s Disease Association-UCB Pharma; MA, meta-analysis; MDS, Movement Disorders Society (critique and recommendation papers on different outcome measures); NINDS-CDE, National Institute of Neurological Disorders and Stroke Common Data Elements initiative; OM, Outcome Measures; P-UK, Parkinson’s UK; PPIE, Patient and Public Involvement and Engagement; SR, Systematic review; UoP, University of Plymouth; WG, Working Group.
From this initial list, at least two members of the OM WG with relevant expertise, and supported by CGR, compiled and reviewed the most relevant PD endpoints in each of the following domains: motor, non-motor, disability, health-related quality of life (HR-QoL), resource use, cognitive, digital, quantitative motor, neuroimaging, and wet biomarkers. Where available, MDS critiques and recommendation papers on different measuring instruments for PD in the categories included in this paper were reviewed (https://www.movementdisorders.org/MDS/MDS-Rating-Scales/Rating-Scales-Critiques-and-Recommendations.htm), and the outcome measures classified as “Recommended” were included for consideration. Targeted literature searches in PubMed were then conducted to identify new measures developed since the publication of the MDS recommendations, or new evidence on measures not previously fulfilling the “Recommended” criteria, with a focus on “Suggested” measures. Other recent reviews were considered when writing this consensus paper. For example, for the disability measures, a 2022 systematic review was used to further guide the choice of outcome measures [1]. Similarly, a 2021 systematic review was employed to aid the decision on health-related quality of life outcome measures [2]. Supplementary Table 1 summarizes the “Recommended” instruments according to the corresponding MDS critique and review papers, the Neurological Disorders and Stroke Common Data Elements (http://www.commondataelements.ninds.nih.gov/) [3] in PD version 2.0 recommendations [4], and our selected outcome measures.
Selected outcome measures for consideration and level of recommendation
*Change in LEDD is recommended as Core in trials including PD patients taking symptomatic medication (i.e., not drug-naïve). **Administration of the C-SSRS is recommended if screening question on the PHQ-9 is >0. Core, to be included in all disease-modifying PD trials; Supplemental, recommended but not required for all disease-modification studies in PD depending on the particular trial; Exploratory, may fill current gaps once validation is complete but require further validation; ABC Scale, Activities-Specific Balance Confidence Scale; ACE-III, Addenbrooke’s Cognitive Examination; ADAS-Cog, Alzheimer’s Disease Assessment Scale-Cognitive Subscale; AES, Apathy Evaluation Scale; AS, Apathy Scale; BRAIN, Bradykinesia-Akinesia Incoordination; C-SSRS, Columbia Suicide Severity Rating Scale; CAPSIT-PD, Core assessment program for surgical interventional therapies in Parkinson’s disease; CGI-I, Clinical Global Impression Scale-Improvement; CSF, Cerebrospinal fluid; CSRI, Client Service Receipt Inventory; DRS-2, Mattis Dementia Rating Scale Second Edition; EHR, Electronic health records; EHR, Electronic Health Records; EQ-5D-5L, EuroQoL 5-dimension 5-level questionnaire; eSAPS-PD, Scale for the Assessment of Positive Symptoms in Parkinson’s Disease, enhanced version; ESS, Epworth Sleepiness Scale; FES-I, Falls Efficacy Scale International; FSQ, Functional Status Questionnaire; FSS, Fatigue Severity Scale; GDS-15, 15-item Geriatric Depression Scale; HUI, Health Utility Index; ICECAP, ICEpop CAPability measures; KPPS, King’s Parkinson’s Disease Pain Scale; LARS, Lille Apathy Rating Scale; LEDD, Levodopa-Equivalent Daily Dose; MDRS, Mattis Dementia Rating Scale; MDS-NMS, Movement Disorder Society-sponsored Non-motor Rating Scale; MDS-UPDRS, Movement Disorders Society-sponsored revision of the Unified Parkinson’s Disease Rating Scale; Mini-BESTest, Mini-Balance Evaluation Systems Test; MM4D, Motor fluctuations Monitor for Parkinson’s Disease; MMP, Mini-Mental Parkinson; MMSE, Mini-Mental State Examination; MoCA, Montreal Cognitive Assessment; NfL, neurofilament light chain; NI, not included; NINDS-CDE v2.0, National Institute of Neurological Disorders and Stroke Common Data Elements version 2.0; NMSQ, Non-motor Symptoms Questionnaire; NMSS, Non-motor Symptoms Scale; OPDC, Oxford Parkinson’s Disease Centre; PD-CRS, Parkinson’s Disease-Cognitive Rating Scale; PDQ-8, 8-item version of the Parkinson’s Disease Questionnaire; PDQ-39, 39-tem version of the Parkinson’s Disease Questionnaire; PDQ-Carer, 29-item Parkinson Disease Questionnaire for Carers; PDSS-2, Parkinson’s Disease Sleep Scale-2; PET, positron emission tomography; PHQ-9, 9-item Patient Health Questionnaire; PKG, Parkinson’s Personal KinetiGraph® (formerly Parkinson’s KinetiGraph®); PQoL carers, carers quality-of-life questionnaire for parkinsonism; ProFaNE, Prevention of Falls Network Earth; PROMIS/Neuro-QoL, Patient-Reported Outcomes Measurement Information System/Quality of Life in Neurological Disorders; ROMP, Radboud Oral Motor Inventory for Parkinson’s Disease; S&E ADL SCALE, Schwab and England Activities of Daily Living Scale; SAPS-PD, Scale for the Assessment of Positive Symptoms in Parkinson’s Disease; SCOPA-AUT, Scales for Outcomes in Parkinson’s disease-AUTonomic symptoms; SCOPA-COG, Scales for Outcomes in Parkinson’s disease- COGnitive symptoms; SDQ, Swallowing Disturbance Questionnaire; SF-12, 12-Item Short Form Survey; SF-36, 36-Item Short Form Survey; SPECT, single-photon emission computerized tomography; Supplemental-HR, Supplemental-Highly Recommended; SWAL-QOL, Generic Scale for Dysphagia-Related Outcomes (Quality of Life); TUG, Timed Up and Go; UPDRS, Unified Parkinson’s Disease Rating Scale; UDysRS, Unified Dyskinesia Rating Scale; WOQ-9, 9-item Wearing Off Questionnaire; WOQ-19, 19-item Wearing Off Questionnaire; α-syn, alpha-synuclein; Aβ, amyloid beta
This publication also used the National Institute of Neurological Disorders and Stroke Common Data Elements (http://www.commondataelements.ninds.nih.gov/) [3]. More specifically, the NINDS-CDE in PD version 2.0 [4], a NINDS guide to consistently capture and record data across PD studies and to standardize this process to increase comparability of studies, was reviewed. The levels of recommendation for each endpoint (Core, Supplemental – Highly Recommended, Supplemental, Exploratory, Not Recommended), where available, were considered and a modified version was used for classification of outcome measures for disease-modifying trials on the MAMS platform. In short, in the NINDS-CDE classification, “General Core” data elements are required for all NINDS funded studies, “Disease Core” elements collect essential disease-specific (i.e., PD) information and are required for all PD studies, “Disease Supplemental – Highly Recommended” elements have commonly been used and validated in PD and are essential only for some PD studies; “Disease Supplemental” elements are recommended but not required for PD studies and their use varies according to study type, and “Disease Exploratory” elements require further validation but may fill current gaps once validation is complete and can be used as long as their limited or pending validation is acknowledged within the study. We adopted a simplified version of this classification, namely “Core” indicating outcome measure collecting essential PD-specific information to be included in all disease-modifying PD trials (not necessarily as a measure of disease progression); “Supplemental” those that are recommended but not required for all disease-modification studies in PD (i.e., depending on the particular trial); and “Exploratory” those which may fill current gaps once validation is complete but require further validation.
A four-fold strategy was used to include PPIE input. First, data from a recent survey from Parkinson’s UK [5] was reviewed, in which 790 participants (people with PD (PwP) in different stages, partners, carers or family members) reported the symptoms they would most like to see improved. Furthermore, the 2018 European Parkinson’s Disease Association-UCB (EPDA-UCB) survey results were reviewed to extract the most challenging symptoms according to 984 respondents (PwP and families/carers) [6]. In addition to that, a questionnaire was completed by members of the PPIE Working Group of the EJS ACT-PD Consortium about their judgement on the most bothersome symptoms of PD. Measures for the highest-ranking motor and non-motor symptoms in both surveys were included in this list. Whilst this information is primarily relevant to symptomatic treatments, the aim of any disease-modifying treatment would be to reduce functional disability relevant to patients. The results of these surveys on the highest-ranking symptoms for patients inform about the critical aspects of the condition that disease-modifying therapies should aim to delay or ideally avoid. Further input was sought from two PPIE groups (total n = 22) about the maximal acceptable duration and frequency of study assessments, either remote or in-person. This approach aimed to guide the maximal number of outcome measures/visit to be included in a disease-modifying PD trial.
All outcome measures identified using the information from the above-mentioned strategies were then evaluated for their potential use in disease-modifying PD trials based on: feasibility, clinical meaningfulness for PwP and clinicians, acceptability to regulators, burden on PwP and clinician, reliability, validity, existence of a suggested clinically meaningful cut-off in PD, sensitivity to change, relevance for specific PD subgroups, interpretability, and current NINDS-CDE classification. When several outcome measures for the same feature arose from the search strategies with comparable properties, the frequency of use of each in clinical trials (obtained via a search in clinicaltrials.gov of the considered outcome measure) and its use in disease-modifying trials (identified in the systematic review (Dr. Marie-Louise Zeissler, unpublished)) together with expert opinion and PPIE input was considered for selection to inclusion.
Compilation of information from all sources was combined in a final report by CGR and AS and reviewed by the expert group. The expert group discussed the information in several meetings, and reviewed several drafts of the list. This methodology is intended to guide future evaluation of evidence on outcome measures for inclusion in future trials in the MAMS platform.
RESULTS
Triangulation of the above methods resulted in a range of outcome measures on global impression, motor, non-motor features of PD, overall progression, disability, health-related quality of life, resource use, digital and quantitative outcome measures and neuroimaging and wet biomarkers. The full list and classification based on our criteria is shown in Table 1. Further details on the Core outcome measures are included in Table 2, and information on each individual outcome measures included in the above table can be found in the Supplementary Material.
Brief overview of suggested Core OM in disease-modifying PD trials
*LEDD is recommended as Core in trials included PD patients taking symptomatic medication (i.e., not drug-naïve). **A question enquiring about falls is recommended as Core, and as an example, the ProFaNE falls definition is described under this section. CALYs, Capability-Adjusted Life-Years; CGI-I, Clinician Global Impression scale – Improvement; CSRI, Client Service Receipt Inventory; DSM-IV, Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition; HER, Electronic Health Records; HR-QoL, Health-Related Quality of Life; ICECAP, ICEpop CAPability measures; LEDD, Levodopa-Equivalent Daily Dose; MDS-UPDRS, Movement Disorders Society-sponsored revision of the Unified Parkinson’s Disease Rating Scale; MMSE, Mini-Mental State Examination; MoCA, Montreal Cognitive Assessment; NMS, non-motor symptoms; OM, outcome measure; PD: Parkinson’s disease; PDD, Parkinson’s disease dementia; PD-MCI, Parkinson’s Disease with mild cognitive impairment; PDQ-39, 39-item Parkinson’s Disease Questionnaire; PDQ-8, 8-item Parkinson’s Disease Questionnaire; PHQ-9, 9-item Patient Health Questionnaire; PPIE, Patient and Public Involvement and Engagement; PRIME-MD, PRIMary care Evaluation of Mental Disorders; QALYs, Quality-Adjusted Life-Years; S&E ADL, Schwab and England Activities of Daily Living Scale; VAS, Visual Analogue Scale.
For overall assessment of health, two global status scales were included: the Clinical Global Impression Scale-Improvement (CGI-I) and the Clinical Global Impression Scale-Severity (CGI-S) [7]. We also included the change in Levodopa-Equivalent Daily Dose (LEDD) [8] for trials including PD patients on antiparkinsonian medications.
For assessment of motor features of PD, we included: the Hoehn and Yahr scale [9], the Movement Disorders Society-sponsored revision of the Unified Parkinson’s Disease Rating Scale (MDS-UPDRS) [10], the remote versions of both the Unified Parkinson’s Disease Rating Scale (UPDRS) and the MDS-UPDRS [11–13], the UPDRS Gait-axial score [14], and the Unified Dyskinesia Rating Scale (UDysRS) [15]. We also included scales on motor symptoms flagged as most bothersome by PPIE representatives, namely gait and balance problems (question about falls (e.g., Prevention of Falls Network Earth (ProFaNE) definition of a fall [16]), Mini-Balance Evaluation Systems Test (Mini-BESTest) [17], Berg Balance Scale [18], Falls Efficacy Scale International (FES-I) [19], and Activities-Specific Balance Confidence Scale (ABC Scale) [20]), and speech and swallowing issues (Generic Scale for Dysphagia-Related Outcomes (Quality of Life) (SWAL-QOL) [21–24], Swallowing Disturbance Questionnaire (SDQ) [25], and Radboud Oral Motor Inventory for Parkinson’s Disease (ROMP) [26]). Amongst the “Diaries and other fluctuation questionnaires”, the Hauser Diary [27–29], the Core assessment program for surgical interventional therapies in Parkinson’s disease (CAPSIT-PD) On/Off Diary [30], and the 9- and 19-item Wearing Off Questionnaires (WOQ-9 [31] and WOQ-19 [32]) were included.
The following global non-motor scales and questionnaires were selected: the Non-Motor Symptoms Questionnaire (NMSQ) [33], the Non-motor Symptoms Scale (NMSS) [34], and the Movement Disorder Society-sponsored Non-motor Rating Scale (MDS-NMS) [35]. Similar to the motor features, specific measures were included for the PPIE-reported most bothersome non-motor symptoms: apathy (Apathy Scale (AS) [36], Apathy Evaluation Scale (AES) [37], and Lille Apathy Rating Scale (LARS) [38]), depression (Geriatric Depression Scale-30 (GDS-30) and GDS-15 [39–41]), 9-item Patient Health Questionnaire (PHQ-9) [42], Columbia Suicide Severity Rating Scale (C-SSRS) [43, 44]), fatigue (Fatigue Severity Scale (FSS) [45]), pain (King’s Parkinson’s Disease Pain Scale (KPPS) [46]), psychosis (Scale for the Assessment of Positive Symptoms in Parkinson’s Disease (SAPS-PD) [47] and its enhanced version (eSAPS-PD) [48]), and sleep (Epworth Sleepiness Scale (ESS) [49], Parkinson’s Disease Sleep Scale-2 (PDSS-2) [50]). Given its relevance and relationship with medication, an autonomic OM was also included (SCales for Outcomes in PArkinson’s disease- AUTonomic symptoms (SCOPA-AUT) [51]).
For global cognitive measures we included the Montreal Cognitive Assessment (MoCA) [52–55], the Mattis Dementia Rating Scale Second Edition (DRS-2) [56], the Parkinson’s Disease-Cognitive Rating Scale (PD-CRS) [57–59], the Addenbrooke’s Cognitive Examination (ACE-III) [60–63], the Alzheimer’s Disease Assessment Scale-Cognitive Subscale (ADAS-COG) [64], the Mini-Mental State Examination (MMSE) [65], the Mini-Mental Parkinson (MMP) [66, 67], and the SCales for Outcomes in PArkinson’s disease- COGnitive symptoms (SCOPA-COG) [68].
For overall progression of features of PD, Milestone-based outcome measures [69] were included.
Disability measures selected for this review were the Schwab and England Activities of Daily Living (S&E ADL) Scale [70, 71], the Functional Status Questionnaire (FSQ) [72, 73], and part II of the MDS-UPDRS [74].
The ICEpop CAPability measures (ICECAP) [75, 76] was included as a capability measure. Carer measures taken into consideration were the carers quality-of-life questionnaire for parkinsonism (PQoL Carers) [77], the 29-item Parkinson Disease Questionnaire for Carers (PDQ-Carer) [78], and the Zarit Burden Interview (ZBI) [79, 80].
Health-related quality of life (HR-QoL) measures were divided into generic (EQ-5D-5L [81, 82], 36-Item Short Form Survey (SF-36) [83, 84], 12-Item Short Form Survey (SF-12) [85, 86], Patient-Reported Outcomes Measurement Information System/Quality of Life in Neurological Disorders (PROMIS/NeuroQoL) [87–90], Health Utility Index (HUI) [91, 92]) and PD-specific (39- and 8- item versions of the Parkinson’s Disease Questionnaire (PDQ-39 [93], PDQ-8 [94])).
Resource use data collection methods were also considered, specifically the Client Service Receipt Inventory (CSRI) [95–97] and electronic health records. A brief discussion of requirements for using HR-QoL and resource use information in health economics analysis is also included in the Supplementary Material.
Digital measures were divided into active (Oxford Parkinson’s Disease Centre (OPDC) smartphone app [98], CloudUPDRS [99], APDM [100, 101], and mPower smartphone-derived composite score [102]), passive (Parkinson’s Personal KinetiGraph® (formerly Parkinson’s KinetiGraph®) (PKG)-based proxy measures [103], Motor fluctuations Monitor for Parkinson’s Disease (MM4D)-based proxy measures [104], Axivity gait accelerometer [105–107]), and combined active and passive tools (Roche smartphone app [108, 109]).
Furthermore, the following quantitative motor measures were considered: Timed-Up and Go (TUG) 3 metre [110], Purdue Pegboard test [111, 112], Alternate tap test [113], BRadykinesia-Akinesia INcoordination (BRAIN) tap test [114, 115], and 9-hole peg test (9hpt) [112, 116–118]. The OPDC composite clinical score [119] was considered under the composite quantitative motor measures section.
Molecular neuroimaging techniques include dopaminergic single-photon emission computerized tomography (SPECT) [122–129], dopaminergic positron emission tomography (PET) [130–133], non-dopaminergic SPECT [134–140], non-dopaminergic PET [141–155,], and magnetic resonance spectroscopy (MRS) [156, 157].
Considered structural neuroimaging techniques [120] were magnetic resonance imaging (MRI) T1 structural sequence [158–162], diffusion imaging [163–166], multiple parametric mapping protocol, neuromelanin [167, 168] and iron-sensitive sequences [169–172].
The following wet biomarkers were selected for review [173–178]: plasma/serum neurofilament light chain (NfL) [179–189,], plasma tau [190–195], plasma alpha-synuclein (α-syn) [196–205], cerebrospinal fluid (CSF) neurofilament light chain (NfL) [206–210], CSF tau [211, 212], CSF α-syn [213–215], CSF α-syn aggregation [216–221], CSF beta-amyloid (Aβ) [222–229], and salivary markers, such as salivary α-syn [230, 231].
PPIE input revealed that the mean maximum time per study visit varied depending on the frequency of assessments: for 6-monthly visits, it varied between roughly 2 and 3 hours (longer visits more acceptable when remote), and for yearly visits, between 3 and 3.5 hours. Tables 3 and 4 detail the maximum acceptable length of visits for the PPIE WG and for the PPIE broader engagement group.
PPIE WG input on maximal acceptable duration of visits (n = 10)
PPIE broader engagement group input on maximal acceptable duration of visits (n = 12)
240/Not acceptable frequency: the 2 most common answers were either 240 minutes or “this assessment frequency is not acceptable”.
The set of Core outcome measures proposed in Table 2 would take 70 to 90 minutes (i.e., 1 to 1.5 hours) to complete, making it acceptable to patients according to the above.
DISCUSSION
We here present an up-to-date inventory of outcome measures for disease-modifying trials in PD based on expert and PPIE consensus. This inventory and framework will be used to guide the decision to select the outcome measures of the EJS ACT-PD MAMS platform trial, based on their fulfilment of desired criteria for an endpoint (e.g., validated, reliable, sensitive to change, acceptable) and their relevance to the intervention based on its mechanism of action and previously known effects (e.g., wet biomarkers as surrogate or direct markers of target engagement). When selecting and classifying the above measures as Core, Supplemental and Exploratory, a compromise had to be made between measures with the best clinimetric properties, acceptability to patients, feasibility, previous experience of use in PD trials, and regulatory considerations, which potentially might have led to prioritizing measures which appear less “promising” from a purely theoretical point of view (i.e., original validation study results) over others, to achieve an adequate balance and provide a realistic and practical tool. This work could also inform other trial initiatives aiming to identify disease-modifying treatments for PD and the framework used will allow updates with new emerging evidence in the future. However, this inventory of outcome measures was created as part of the development of a MAMS trial for progression of PD and as such, presents some particularities which might have influenced the final list of included outcomes. This type of trial requires large participant numbers across a variety of centers, and has a much longer duration than usual randomized controlled trials (RCTs) (i.e., several years) [232, 233]. Therefore, MAMS trials require endpoints which can be measured in different research settings (ideally remotely), and which are sensitive to changes and capture relevant events in disease progression in the longer term. Alternative trial designs, studies focused on particular PD subpopulations, or those looking into changes in a particular aspect of the disease (e.g., cognition, gait) might require an adaptation of this inventory, although it could provide a basis for such adaptations. All of these caveats emphasize the need for a common core set of outcome measures applicable across trial designs and PD populations, to ensure translatability of results regardless of differences between individual trials. Furthermore, it is important to note that this classification does not intend to dictate the choice of primary endpoint, which should be based on the individual trial characteristics (aim, intervention, population, design), and prioritize, among others, sensitivity to change (i.e., detection of disease-modifying effects), relevance, patient acceptability, and feasibility. We refer the readers to regulatory guidance on this subject [234, 235].
Despite being included as exploratory due to the lack of formal validation in this setting, novel outcome measures, and especially digital endpoints, are a promising alternative to complement the currently available instruments. Their potentially increased sensitivity and the possibility of continuous monitoring in real-life conditions (i.e., at home) is likely to be a valuable addition to the administration of scales in the clinical setting. In line with this, a number of initiatives are looking into the clinical validity of these endpoints and their implementation in clinical research [236, 237]. This group selected some of the digital outcomes with more information on PD populations to be included in the inventory. Nevertheless, this is a fast-moving field and recommendations here could require more frequent revision than for other types of endpoints.
The main strength of our approach was strong expert and PPIE consensus, embedding the patient’s voice into the development and recommendation of outcome measures, as well as evidence from literature reviews, information from other initiatives, and input from regulatory bodies.
Conclusions
With the above methodology, we have identified a broad range of outcome measures which can be potentially included in disease-modifying PD trials, and make recommendations for their inclusion as core, supplementary (for specific arms) and exploratory measures in the EJS ACT-PD MAMS initiative. For other MAMS initiatives, this review aims to serve as a resource from which to select the desired outcome measures according to the requirements of the study (e.g., population, mechanism of action of the intervention, etc.). We also provide a framework for future update of the evidence on outcome measures in disease-modifying PD trials.
EJS ACT-PD CONSORTIUM MEMBERS
Additional EJS ACT-PD consortium members (further details are provided in the Supplementary material): Roger Barker, James Carpenter, Yoav Ben Shlomo, Mark Edwards, Alan Whone, Carl Counsell, Dorothy Salathiel, Sue Whipps, Anna Jewell, Priti Gros, Tom Barber, Shlomi Haar Millo, K Ray Chaudhuri, Anthony HV Schapira, Oliver Bandmann, Simon Stott, George Tofaris, Esther Sammler, Heather Mortiboys, Li Wei, Alan Wong, Susan Duty, David Dexter, Paula Scurfield, Keith Martin, Edwin Jabbari, Stephen Mullin, Huw Morris, David Breen, Christian Lambert, Prasad Korlipara, Monty Silverdale, Kailash Bhatia, Alison Yarnall, Raj Khengar, Helen Collins, Fleur Hudson, Gareth Baxendale, Rebecca Croucher, Sandra Bartolomeu-Pires, Jennifer Allison, Jodie Forbes, Alex Edwards, Sheila Wonnacott, Dilan Athauda, Joy Duffen, Sonia Gandhi, Emily Henderson, Maryanne Graham, Shona Clegg, Karen Matthews, Vince Greaves, Eric Deeson, Laurel Miller, Joel Handley, David Dexter, Helen Matthews, Kevin McFarthing, Amit Batla, Nikul Bashi, Emma Lane, Miriam Parry, Natasha Ratcliffe, Romy Ellis-Doyle, Sally L Collins, Rebecca Chapman, Jesse Cedarbaum, Anthony Lang, Brian Fiske, Richard Wyse, Mahesh Parmar, Adam Boxer, Denise Wilson, Jean Christophe Corvol, Jennifer Harris.
Footnotes
ACKNOWLEDGMENTS
This work was done as part of the Edmond J Safra Accelerating Clinical Trials in Parkinson’s Disease (EJS ACT-PD) Initiative, which is funded by the Edmond J Safra Foundation.
CONFLICT OF INTEREST
RSW has received speaking honoraria from GE Healthcare and a writing honorarium from Britannia.
DVW reports consultancy and speaker fees from Bial and Britannia.
MTH received payment for Advisory Board attendance/consultancy for Lundbeck, ESCAPE Bio, Evidera, Manus Neurodynamica, Biogen MA, CuraSen Therapeutics, Roche Products Ltd. MTH is an advisory founder of NeuHealth Digital Ltd (company number: 14492037), a digital biomarker platform to remotely manage condition progression for Parkinson’s.
AJ has been involved in the development and clinical assessment of a smartphone-based tool for Parkinson’s disease (cloudUPDRS).
ML received fees for advising on a secondary analysis of a Parkinson’s RCT (GDNF) sponsored by North Bristol NHS trust.
AN has been involved in the development of the Bradykinesia-Akinesia Incoordination (BRAIN) test. AN is an Editorial Board Member of this journal, but was not involved in the peer-review process nor had access to any information regarding its peer-review.
HZ has served at scientific advisory boards and/or as a consultant for Abbvie, Acumen, Alector, Alzinova, ALZPath, Annexon, Apellis, Artery Therapeutics, AZTherapies, CogRx, Denali, Eisai, Nervgen, Novo Nordisk, Optoceutics, Passage Bio, Pinteon Therapeutics, Prothena, Red Abbey Labs, reMYND, Roche, Samumed, Siemens Healthineers, Triplet Therapeutics, and Wave, has given lectures in symposia sponsored by Cellectricon, Fujirebio, Alzecure, Biogen, and Roche, and is a co-founder of Brain Biomarker Solutions in Gothenburg AB (BBS), which is a part of the GU Ventures Incubator Program (outside submitted work).
CBC has received personal fees from AbbVie, Bial, Scient, Orkyn, Abidetex, UCB, Pfizer, EverPharma, Lundbeck, Global Kinetics, Kyowa Kirin, Britannia, and MedScape; and appointments as a Cure Parkinson’s Linked Clinical Trials (LCT) committee member, a Cure Parkinson’s Research Committee member, and a Parkinson’s UK College of Experts Panel member. CBC is an Editorial Board Member of this journal, but was not involved in the peer-review process nor had access to any information regarding its peer-review.
TF has served on Advisory Boards for Peptron, Voyager Therapeutics, Handl therapeutics, Gain therapeutics, Living Cell Technologies, Abbvie, Bluerock, Bayer & Bial. TF has received honoraria for talks sponsored by Bial, Profile Pharma, Boston Scientific & Novo Nordisk. TF is an Editorial Board Member of this journal, but was not involved in the peer-review process nor had access to any information regarding its peer-review. AS is a member of the MDS-UPDRS Development Group, the MDS-NMS Development Group, the NINDS CDE QoL Group, the MDS Rating Scales Review Committee, and the MDS COA Early and Prodromal PD Working Group. AS has been involved in the development of the MDS-UPDRS, the MDS-NMS, and the PQoL.
AS reports consultancy fees from Biogen, Abbvie, Roche, Bial, and GE Healthcare; license fees from University College London; and royalties from Oxford University Press. CGR, MB, MBu, CSC, BH, CL, GM, PP, KP, LR, CS, CWG and MLZ have no conflict of interest to report.
DATA AVAILABILITY
Data sharing is not applicable to this article as no datasets were generated or analyzed during this study.
ADDITIONAL STATEMENT
For the purpose of open access, the author has applied a Creative Commons Attribution (CC BY) license to any Author Accepted Manuscript version arising from this submission.
