Abstract
Inflammation has increasingly become a focus of study in regards to Parkinson’s disease (PD). Moreover, both central and peripheral sources of inflammation have been implicated in the pathogenesis of PD. Central inflammation consisting of activated microglia, astroglia, and T cell responses within the PD central nervous system; and peripheral inflammation referring to activated innate cells and T cell signaling in the enteric nervous system, gastrointestinal tract, and blood. This review will highlight important work that further implicates central and peripheral inflammation in playing a role in PD. We also discuss how these two distant inflammations appear related and how that may be mediated by autoantigenic responses to α-syn.
Keywords
INTRODUCTION
Historically, Parkinson’s disease (PD) has been studied as a disorder that primarily deteriorates the motor circuit of the individuals it affects. In the last 20 years however, several important studies have expanded the scope of PD dysfunction to other systems within the central nervous system (CNS) such as areas controlling cognition (reviewed in Aarsland et al. [1]) and neuropsychiatry (reviewed in Weintraub et al. [2]). Importantly, a growing body of evidence has shown that PD pathobiology clearly has an influence on regions outside of the central nervous system. These regions affected by PD include the peripheral enteric nervous system (ENS) [3], the gastrointestinal (GI) tract [4, 5], and peripheral blood [6]. One obvious link connecting the central and peripheral nervous system dysfunction observed in PD is the presence α-synuclein (α-syn) pathology in neurons of both locations. Another crucial connection is the growing evidence for chronic inflammation in central and peripheral nervous systems and in circulating blood of individuals with PD. Here we specifically aim to highlight the more recent works in the field of PD research detailing inflammation in the central nervous system (brain parenchyma, cerebrospinal fluid, and meninges) and inflammation in the peripheral body (ENS, GI tract, and blood)—as well as discussing how these two distant inflammations may relate to one another in the pathogenesis of PD.
INFLAMMATION IN THE CENTRAL NERVOUS SYSTEM ASSOCIATED WITH PD
CNS inflammation was first associated with PD through pathology studies detailing reactive microglia within the mesencephalon of postmortem brain samples from individuals with PD [7]. This initial observation of inflammation within the primary brain tissue afflicted in PD has only expanded and now includes several additional cell types within the parenchyma as well as the cerebrospinal fluid (CSF).
Microglial inflammation in PD
Microglia, a type of tissue resident macrophage, are the primary immune cell found throughout the CNS. In PD, microglia not only display morphologies indicative of activation, but also have been shown to express markers of inflammation such as HLA-DR [8], CD68 [9], TLR4 [10], and NLRP3 [11]. Further evidence that these molecules are involved in the inflammatory state has been established in animal models of PD, where their genetic knockout has been shown to reduce the neuroinflammation and neurodegeneration observed in those models [11–13]. More recently, triggering receptor expressed on myeloid cells 2 (TREM2), an immune receptor expressed on microglia and previously identified as harboring a genetic risk allele for PD [14], has been shown to be in disproportionate levels in the CSF of PD individuals [15]. Interestingly, overexpression of TREM2 in the CNS of mice undergoing 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) intoxication (a classical model of PD) was both anti-inflammatory and neuroprotective [16]. Generally, it appears that most of the immune molecules associated with microglia in PD are indicative of a cell type responding to environmental stress, cell death, and immune signaling—all things microglia are seemingly equipped to deal with [17]. With that said, it remains puzzling as to what factors initiate, sustain, and prevent the resolution of the pro-inflammatory microglial response in PD. One long-studied source contributing to this microglial dysfunction is the α-syn pathology harbored and propagated by neurons [18, 19]. Recently, a study by Scheiblich et al. [20] detailed an intricate system that microglia employ to cope with degrading excess amounts of α-syn pathology. One component being that “overloaded” microglia will directly transfer their excess α-syn to neighboring naïve microglia. Furthermore, they also showed that lower amounts of α-syn pathology was associated with lower inflammatory profiles within microglia. Taken together, these findings indicate that α-syn pathology is a driver of microglial activation and dysfunction in PD.
Astrocytic inflammation in PD
Although far less studied compared to microglia in the context of PD, astrocytes have increasingly been implicated in playing a role in the PD disease process. One major discovery being the characterization and identification of reactive, neurotoxic astrocytes in postmortem PD brain [21], as well as rodent models of the disease [22]. A key trigger responsible for this pro-inflammatory and neurotoxic [23] switch in astrocytes has already been identified: microglial derived pro-inflammatory factors (IL-1α, TNF, and complement) [21, 23]. This microglia-astrocytic activation axis has also been identified in multiple sclerosis [24], where it was shown that pro-inflammatory T cells interface with these innate cells as well. It seems a similar scenario is occurring in PD, with activated CNS innate cells (microglia/astrocytes) being in close proximity to responding T cells from the periphery.
CNS lymphatics and PD
The presence of T cells in the brain parenchyma of PD, while widely accepted now, was controversial at the time of its observation. Infiltration of CD4 and CD8 T cells in and around the substantia nigra [25] expanded the role of the immune system from the closed CNS and its cells to an interconnected immune response involving the periphery. This concept of neuroimmune interactions in PD has only been bolstered with the re-discovery of the CNS lymphatics [26]. Now CNS-peripheral immune interactions are better realized as the lymphatic trafficking system facilitating them is further characterized in both steady state and disease [27, 28]. In regards to the CNS lymphatics in PD, a recent publication showed that the meningeal lymphatic system itself appears impacted in individuals with PD, resulting in reduced lymphatic drainage/flow compared to age-matched healthy controls [29]. These observations lead to the hypothesis that the route in which T cells traffic through the CNS in PD is impaired, as well as the cells themselves.
CNS T cell inflammation in PD
A central remaining question surrounding the presence of T cells in the PD CNS is the nature of their inflammatory status. Are these cells providing anti-inflammatory responses to the neuronal damage or are they specifically responding with pro-inflammatory responses of their own? Evidence collected recently suggests the latter. In their latest study, Gate et al. [30] reaffirmed that CD3+ T cells can be found in close association with α-syn-laden nigral neurons of postmortem Parkinson’s disease dementia (PDD) and Lewy body dementia (LBD) brains. More importantly, they went on to detail how these parenchymal T cells had increased expression of the pro-inflammatory cytokine IL-17a. Complementary to these findings, the study also showed that T cells within the CSF of PDD/LBD patients had increased expression of a host of immune trafficking and activation markers including CXCR4 and CD69, respectively. The identification of pro-inflammatory T cells in the PD brain and CSF mirrors multiple works that have previously shown activated T cells and inflammation in PD peripheral blood [31–33] as well as in preclinical models of the disease [12, 34]. Overall, this knowledge could further the potential for T cell targeting therapies in PD, with the idea being that there is a common link between central and peripheral responses and targeting one (peripheral) can benefit the other (central).
INFLAMMATION IN THE PD PERIPHERY
Though it took longer to appreciate, the field of PD research now recognizes that the inflammation associated with the disease is not just contained within the CNS. Rather, it appears that the inflammation also extends (or originates) to the ENS/GI tract as well as the blood.
ENS and GI tract inflammation in PD
Braak’s seminal work detailing the initial early staging of α-syn pathology within the olfactory nucleus and vagal nerve was a breakthrough in the study of PD-affected regions outside of the traditional nigrostriatal pathway of PD [35]. Braak then went on to expand on the vagal tract in PD by detailing α-syn inclusions with the myenteric and submucosal plexus of the ENS of postmortem PD patients [36]—providing substantial evidence that the origin of α-syn pathogenesis may occur in the gut, and then propagate into the CNS.
Alongside the α-syn pathology localized to the gut, evidence has begun to accrue which describes a dysfunctional [4] and inflamed [37] GI tract associated with PD. In addition to being impaired and pro-inflammatory, the PD GI tract is also associated with microbiome dysbiosis, with multiple studies detailing alterations in PD microbiota [38, 39] and one recent publication detailing an overabundance of opportunistic pathogens within the PD gut microbiome [40]. This evidence of a diseased GI/ENS in PD is also backed up by several findings in preclinical mouse models of the disease. For instance, several groups have shown that α-syn inoculation in the duodenal wall of mice is sufficient to seed and propagate α-syn pathology/dysfunction from the ENS into several relevant PD CNS sites [41, 42]. Remarkably, this gut-seeded α-syn also induced local GI inflammation (including heightened IL-6) [41] and that this prion propagation of α-syn dysfunction could be halted by vagotomy [42]. Focusing more on potential autoimmune-drivers, a preprint publication [43] reports gut inflammation and a loss of enteric neurons in mice after their immunization with an antigenic α-syn epitope (previously identified in human PD [32]). Notably, when the group depleted CD4 T cells during this α-syn immunization paradigm—enteric neurons were partially rescued. In terms of preclinical PD microbiota work, one study has shown that α-syn overexpressing mice reconstituted with PD microbiota had exacerbated α-syn pathology, microglial activation, and motor deficits compared to normal mouse flora [44]. Lastly, in regards to peripheral gut inflammation and PD, a potential link to inflammatory bowel disease (IBD) has been described. This association gained traction when LRRK2, a common genetic risk factor for PD, was also found to be associated with cases of ulcerative colitis [45]. Perhaps more compelling, it has since been observed that IBD patients are at a higher risk for developing PD [46], and among IBD patients, those taking immunomodulatory anti-TNF treatment had a reduced risk compared to those not on anti-TNF [47]. Taken together, it may be that α-syn begins its PD pathogenesis in ENS of the GI through the potentiation by environmental stress, pathogenic bacteria, and/or misguided immune responses. Now established in the gut, α-syn pathology propagates up the vagus nerve and into the CNS. One potential link between these two processes being the circulating blood immune responses that survey (and remember) both systems.
Blood inflammation in PD
Given the systemic inflammatory immune response observed in multiple PD tissues, it makes sense that this would also be captured in the major pathway for immune cell trafficking in the body, the blood. Indeed, several studies examining the blood of individuals with PD have noted increases in numerous pro-inflammatory cytokines including IL-6, TNF, and IL-2 (reviewed in [48]). In addition to this overabundance of pro-inflammatory cytokines, altered immune cell compositions have been observed in PD as well. For example, PD blood-monocyte populations have been shown to have more proliferative capacity compared to age-matched healthy controls [49]. This immune dysregulation in PD also includes the adaptive immune system. Not only has it been reported that there are increases in IL-17 [31, 33], IL-4 [32, 33], and IFNγ [32, 33] producing T cells, but the target of some of these T cell responses has been identified—α-syn. Indeed, it appears that the pathological hallmark protein of PD, is also the antigenic target of some pro-inflammatory T cells found in the blood [30, 51] and CSF [30, 52] of individuals with PD. Interestingly, the same study that showed increased IL-17a expression in blood T cells stimulated with α-syn peptide also reported increases of IL-17a expressing T cells in the substantia nigra (reviewed earlier) of PDD/LBD patients. While these experiments fall short of directly linking peripheral α-syn specific T cell responses with those T cell response occurring directly in the CNS, the implication is hard to ignore and should be the subject of future studies.
CONNECTING THE CENTRAL AND PERIPHERAL IMMUNE RESPONSES IN PD
The pathobiology of PD has expanded in scope several times since its initial description by James Parkinson in 1817. The disease process of PD is now recognized to affect non-motor regions of the brain as well as areas outside of the CNS—mainly the ENS and the GI tract it innervates. Two key characteristics that appear universally shared by these PD-affected regions are the pathological misfolding of α-syn and increased inflammation. And as we have reviewed here, α-syn can directly potentiate inflammatory responses from both the innate (macrophages/microglia/astrocytes) and adaptive (T cells) arms of the immune system. Another important connection between α-syn pathology and inflammatory immune responses is that both appear to be occurring in PD before the onset of overt motor symptoms. Longstanding work [35, 36] has suggested that α-syn pathology originates in the ENS early and spreads to the CNS later in disease. Newer work suggests that an aspect of the PD immune response may also be occurring long before the establishment of overt neurodegeneration. That is, α-syn specific T cell responses have been observed to be at their highest around the initial diagnosis of PD and wane with progression [50]. Perhaps more compelling, the same study also reported on a longitudinal case of PD and showed that α-syn specific T cell responses were increased and present many years before that individual displayed symptoms and was subsequently diagnosed.
One theory connecting these findings all together (and illustrated in Fig. 1) is that early pathological events taking place in the GI/ENS involve both α-syn dysfunction and inflammatory immune responses. More specifically, dopaminergic enteric neurons acquire initial α-syn pathology through a combination of environmental, genetic, microbiome, and immune factors. This misfolded α-syn species may now be the new target of immune responses from both surrounding macrophages as well as T cells—leading to excess inflammation and neuronal death. Important to note, these excessive PD immune responses also appear to have a genetic basis (similar to α-syn pathology), with several reports detailing PD related genes/mutations promoting inflammation [53]. For instance, the G2019S LRRK2 mutation [54] as well as L444P/N370S GBA mutations [55, 56] being associated with hyper-inflammatory states.
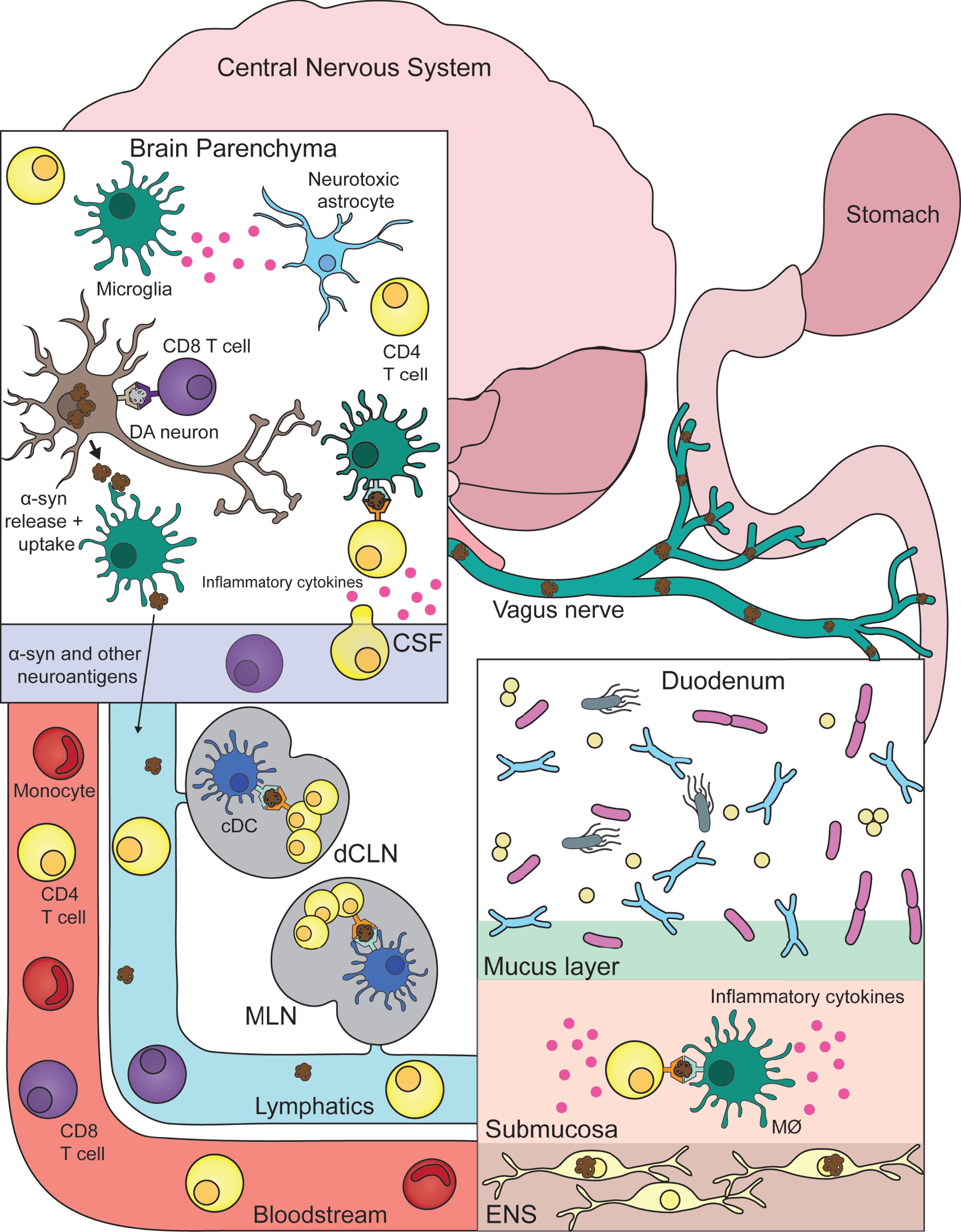
Connecting central and peripheral immune responses in Parkinson’s disease. Inflammatory and damaging events in the gastrointestinal tract (duodenum) caused by a combination of environmental, genetic, microbial, and immune factors leads to α-synuclein (α-syn) pathology in the innervating enteric nervous system (ENS). Misfolded α-syn species within the ENS may become targets for resident macrophages (MØ) with subsequent antigen presentation to T cells that misrecognize self-peptide and possibly expand in the gut-draining mesenteric lymph nodes (MLN). This α-syn provoked inflammatory response promotes further α-syn pathology and eventual propagation to the central nervous system via the vagus nerve. Now α-syn pathology with neurons leads to similar inflammation as described in the gut. With microglia taking up pathogenic α-syn—leading to their activation (and subsequent activation of neurotoxic astrocytes) and presentation of α-syn antigen to cerebrospinal fluid (CSF) patrolling T cells. Another link between the two distant systems is also the bloodstream that connects them. T cells and other immune cells may be able to extravagate through the blood-brain barrier in response to heightened inflammation coming from the brain parenchyma/CSF. Lastly, similar to the MLN, T cells may be encountering and expanding to α-syn and other autoinflammatory neuroantigens within the central nervous system draining deep cervical lymph node (dCLN). DA, dopamine; cDC, classical dendritic cell.
Over time, prion-like propagation of α-syn pathology ascends the vagus nerve into the CNS proper. Similar to ENS neurons, CNS dopaminergic neurons are now negatively affected by α-syn pathology and elicit heightened immune responses from microglia. Now, previously ENS primed circulating α-syn specific T cells produce their same pro-inflammatory response, but now leading to the destruction of CNS neurons. Obviously future work is needed to better realize and substantiate this theory but for now it serves as an aid in marrying peripheral and central inflammation to the pathogenesis of PD. One example of a pressing question that should be addressed in the aforementioned future work being: Are there additional neuroantigens being targeted by autoimmune T cells in PD? With multiple autoantigens indeed being the case for other autoimmune diseases such as multiple sclerosis [57] or lupus erythematosus [58].
In regards to viewing and studying PD as a potential inflammatory disorder, it is important to note and discuss the fact that PD clinical trials targeting immune features of PD have all virtually failed to achieve meaningful benefit for individuals with PD [53]. This could be in part due to their method and rationale for therapy, e.g., many trials are focused on immunization/antibody targeting of α-syn. In Alzheimer’s disease (AD), the targeting/clearance of amyloid-β (Aβ) has been a focus of an intense amount of research that has ultimately cast into doubt whether the reduction of amyloid load in AD patients is actually therapeutic [59]. The same may be true for α-syn in PD, or at the very least, this type of therapy as well as the other anti-inflammatory interventions require prodromal or preclinical PD patients to actually prevent or slow the disease. So even though previous immune-related PD clinical trials have been unsuccessful, it should be a priority in the field to learn and improve upon them to make way for novel immunotherapeutic approaches and patient populations.
CONCLUSION
In conclusion, there are distinct central and peripheral inflammatory responses observed in the brain, blood, and gut of individuals with PD. These inflammatory responses originate from several different cell types including microglia, astrocytes, and T cells. The target of many of these responses are associated with α-syn pathology and/or neurodegeneration. One potential link proposed here is that initial ENS α-syn pathology potentiates a destructive autoinflammatory immune response that then later affects the CNS. Future work is required to better understand these central/peripheral inflammations and how they might be leveraged in the development of immunotherapies for the treatment of PD.
Footnotes
ACKNOWLEDGMENTS
This study was supported by the joint efforts of The Michael J. Fox Foundation for Parkinson’s Research (MJFF) and the Aligning Science Across Parkinson’s (ASAP) initiative as well as the NIH T32AI125179 (GPW). MJFF administers the grant ASAP-000375 on behalf of the ASAP and itself.
CONFLICT OF INTEREST
The authors have no conflicts of interest to report.
