Abstract
Recent research aimed at the discovery, integration, and communication of health outcome measures (or “biomarkers”) in Alzheimer’s disease has raised challenging questions related to whether, how and when results from these investigations should be disclosed to research participants. Reflecting the apparent heterogeneity of many neurodegenerative diseases, biomarker or other risk factor results are often probabilistic, interactive, multi-modal, and selective. Such characteristics make it very complex to summarize and communicate to clinicians, researchers, and research participants. Whereas the format and content of academic literature is well-managed by the peer-review process, reporting individualized results to participants involves complex, sensitive, and ethical considerations. This paper describes three key factors to consider in decisions about the return of results to research participants: complexity, precision, and responsibility. The paper also presents six practical recommendations for implementing meaningful and ethical communication with research participants.
NOVEL BIOMARKERS: A GAME-CHANGING CHALLENGE
In the race to develop effective prevention and treatment interventions, the scope and scale of dementia research grows, with international, multi-site trials now looking to enroll thousands of participants. Amidst these efforts, dementia biomarker [1] (and other dementia health outcomes) research presents both game-changing opportunities and disconcerting challenges. The rapid growth in discovery, integration, and deployment of novel and complex biological, neurological, lifestyle, and digital health outcome measures of dementia risk and progression must be balanced by parallel success in the ability of researchers and clinicians to scientifically interpret, publicly translate, and communicate their meaning, strength, limitations, and clinical relevance.
Important progress has been made to further understand the practical and ethical issues involved in communicating dementia biomarker results in research studies [2–8]. From an ethical standpoint that is anchored in the Declaration of Helsinki principles to promote and safeguard the health, well-being, and rights of human research subjects [9], recommendations for biomarker disclosure are evolving. Different criteria have been proposed to guide researchers’ decision-making around return of results. Examples include criteria related to clinical implications, such as disclosing results when the biomarkers are Alzheimer’s disease (AD) risk implicating (increased risk, of the apolipoprotein E (APOE) ɛ4 allele), or diagnostic (as in cerebrospinal fluid (CSF) amyloid-β (Aβ)) and discovered as present in preclinical/asymptomatic persons; related to personal factors, such as when results can promote respect for participant autonomy and inform their engagement in secondary prevention; and related to research goals, such as when disclosure is necessary to facilitate recruitment and participation in longitudinal clinical trials. However, some of these criteria can be challenging to interpret (e.g., determining what constitutes “respect for autonomy”), and none are currently universally accepted.
Despite this guidance, Alzheimer’s disease and related dementias (AD/ADRD) researchers commonly face multiple challenges in communicating biomarker results. Increasingly available are multiple (and multi-modal) indicators of AD/ADRD risk, some of which seem to operate interactively or collectively or in networks. There are multiple or integrated influences on the pathways toward the development of dementia, a fact that reduces the certainty we have about the clinical significance of single risk indicators and their link to a specific diagnostic outcome (AD). There is an important distinction between a cohort-based risk profile and an individual’s risk profile. As most research on risk applies to a group, not to an individual, indicators should be viewed in the context of personalized dementia risk profiles that account for a multiplicity of interdependent factors including age, race, ethnicity, concurrent pathologies, and social and structural determinants of health [8, 10]. Widespread lack of ethnic, racial, and socioeconomic diversity in clinical trials adds to further uncertainty about the precision of dementia risk and is compounded by scant knowledge of the impact of disclosure on underserved individuals, their family members, and communities [6, 8]. Researchers must also contend with the difficult prospect of how to sensitively communicate information about a disease that is inherently feared by lay communities and carries the burden of associated stigma and discrimination [11–14]. Finally, disclosure may have adverse consequences for the participant-researcher relationship by disrupting levels of trust and alliance, the knowledge of which must be balanced among tensions that exist between research ethics and participant preferences [6, 15]. In practice, the lack of consensus as to how to address challenges to biomarker disclosure amounts to communication hesitancy, and the inconsistent handling of results across research sites. A 2021 study of 30 US Alzheimer’s Disease Research Centers (ADRCs) revealed that just over half of sites surveyed returned amyloid positron emission tomography (PET) results, and fewer still returned tau PET results; whereas in contrast, most (83% ) ADRCs returned results for dementia or mild cognitive impairment (MCI) to participants [16]. There is apparent discordance between scientific discovery of modern AD biomarkers, and how to ethically translate them to the individuals and groups concerned.
We continue the conversation on ethical disclosure [6, 17–19], and this increasingly common situation for researchers: how and what to communicate when there are multiple potential and eventual diagnostic outcomes? In light of this uncertainty, we propose eight dimensions of modern biomarker research that should be considered in the communication of results, briefly interpreting available evidence of the impact of disclosure (more fully reviewed here [2–5, 20–22]), and conclude by offering a set of recommendations to support researchers in addressing challenges to biomarker disclosure.
COMPLEXITY ON THE RISE: CAN PRECISION FOLLOW?
In recent years, biomarker and risk-related research in both asymptomatic aging and dementia has accelerated in rate, quality, range, and global coverage [23]. The precision with which diagnostic biomarkers (Amyloid, Tau, and Neurodegeneration, (ATN)), can now be determined has increased dramatically, and at the same time, a challenge remains for determining relative AD risk in asymptomatic aging. The classic National Institutes of Health (NIH) rendering of the term biomarker featured three characteristics: objectivity of measurement, linkage to perturbations in biological processes, and potential as indicators of response to intervention [24]. Such candidate biomarkers are typically extracted and tested independently from neurobiological-related fluids or neuroimaging tools [25]. In AD, the prevailing classification system ATN, offers an unbiased, binarized ordering of diagnostic biomarkers [26]. However, recent research has supplemented this definition by including other modalities of dementia risk sources such as measurement, prediction, and consideration of other pathologies such as vascular changes, inflammation, and Lewy body disease, as proposed in Gauthier et al.’s ATN+ approach [26]. This broader definition encompasses medical, functional, and genetic indicators (e.g., the dynamic interplay of multi-modal ATN+ pathophysiologies), moderator and stratification variables (e.g., age, sex, race), multiple combinations within and across modalities (e.g., indexes, panels, networks, risk scores, burden indicators), and consideration of risk or protective factors (e.g., lifestyle choices, exposures, injuries, frailty), and the influence of social and structural determinants of health (e.g., access to healthcare, social connection, and education) [13, 27]. These advances have been undergirded by rapid improvements in biomarker-related technologies, such as machine learning techniques, omics-related approaches (e.g., metabolomics), digital (e.g., wearables), and neuroinformatic or interactional and dynamic analytics [25], with many of these approaches requiring independent discovery and replication and validation cohorts. The use of integrative approaches to examine multiple modalities of dementia risk (and their interactions) has also become increasingly commonplace [25, 28].
One of the most promising scientific discoveries in recent AD/ADRD research are state-of-the-art blood-based biomarkers (BBBMs). Next to CSF and PET indicators, BBBMs (such as plasma Aβ42/40 ratio, p-tau, glial fibrillary acidic protein, and serum neurofilament light chain) demonstrate high degrees of diagnostic sensitivity and specificity, and in general also offer the distinct advantages of convenient, timely, minimally invasive and affordable sampling [29–35]. While clinical studies continue, the forecast for accessible BBBM testing suggests game-changing potential to target the significant lack of diversity in participant cohorts and fill critical gaps in our knowledge of understanding of under-served groups in AD/ADRD research. Owing to cost-effective and minimally invasive techniques, BBBM sampling offers global scalability and the potential to be used in regions where PET imaging or CSF analysis is unavailable. Direct-to-consumer BBBM sampling reveals additional opportunities to improve health equity and support the right to self-determination and autonomy in health-related decision-making [29, 34]. Optimism for BBBMs, however, must be balanced with an awareness of potential risks, such as the social and ethical implications of using direct-to-consumer sampling in areas where health systems are ill-equipped to offer AD/ADRD care [34].
The promise of biomarker research for detecting early risk and formulating intervention targets for dementia prevention has never been greater. However, knowing when, what, how or whether to disclose results to research participants is a complex challenge: What is it about contemporary biomarker research that exacerbates this communication and ethical challenge?
We identify eight dimensions that represent targets for advancing modern biomarker research, but that also present precarious circumstances for communication. 1) Measurement Quality, or the underlying consideration that specific biomarkers will vary in the extent to which they demonstrate measurement reliability (repeatability), validity (accuracy), and equivalence (correspondence across time and groups). 2) Intensity, or how to evaluate and convey the relative strength of an effect or influence of a biomarker. 3) Complexity, or how to express that biomarker panels or indexes may be comprised of multiple sources or modalities of dementia influence. 4) Generalizability-Precision, or the degree to which biomarker risk is reliably translated and applicable to multiple, diverse populations, as well as the degree of qualified or personalized influence. 5) Risk-Protection Continuum, or the fact that many biomarkers may range in effects not only from 0 (no risk) to 1 (full risk) but also from -1 (protection) to 1 (full risk). 6) Dynamic Characteristics, or the idea that biomarker risk may naturally fluctuate and vary in terms of modifiability, both within and across individuals, inclusive of key demographic categories (sex, race, ethnicity, socioeconomic status). 7) Interactive Aspects, or the fact that some biomarkers may interact (attenuate, moderate, or intensify) their effects (and/or timing) when co-occurring. 8) Evidence Base, or the fact that the evidence base for many biomarker risk effects is limited by methodological, empirical, and geographic (research origin) restrictions.
BIOMARKER COMPLEXITY AND THE ETHICAL IMPERATIVE OF COMMUNICATION
In addition to standard measures of test performance (e.g., specificity, sensitivity, positive and negative predictive value), the impact of biomarkers and risk factors are often expressed as probabilities, risk scores, or burden estimates. These include variations on polygenic risk scores, multi-modal biomarker panels, and interaction or network models [25, 26]. Although products of well-implemented data reduction techniques, such composites are summary indexes of multiple specific markers, each with a unique position along the 8 dimensions noted above. Thus, the apparent simplicity of single scores may mask underlying complexity and hinder interpretative precision. Appropriate interpretation of such biomarker results, and the resulting questions around disclosure are an ethical imperative, dictated by both the research process and the needs and wishes of the participant community. However distinct challenges for effectively relaying this information are exacerbated by mechanistic complexity and the clinical uncertainty of biomarker results, alone or in combination: guidance is needed.
Disclosure of biomarker results may be critical to research design and outcomes. For example, it is well understood that AD is often heterogenous even within a given sample taken from an otherwise homogenous population. In this example, a biomarker scores may be used to determine study group allocations or justify a decision to exclude participants from the study. Also, disclosure may also impact the research itself, especially in the context of time-structured studies such as randomized controlled trials or longitudinal projects. The modality and content of disclosure may change participant behavior which in turn may influence study findings [11, 12]. Specifically, the research team-participant dynamic may be impacted by how the experience of disclosure is conveyed to and interpreted by team members, from the personal perspective of the nominated disclosure researcher. In turn, this may influence the research experience for participants. Directions of these effects are dependent on the quality and method(s) by which complex information is communicated.
Six recommendations for the optimization of the return of biomarker results
The implications of disclosure extend beyond the immediate sphere of research to impact wider clinical, personal, and societal contexts [21]. For participants and their families, disclosure of results has broad influence on lifestyle choices including health and wellbeing behaviors, and decisions around future planning and caregiving [2, 36]. There are also important implications to consider when family members are impacted by the information being returned, such as when genetic risk may apply to parents or offspring. As such, researchers should carefully approach disclosure by balancing participant preferences with research requirements. It is worth noting, however, that empirical evidence about these needs and priorities is mixed. Research examining patient preferences for return of biomarker results indicates that a majority of respondents desire their results [21, 22]. However, these studies suffer from lack of diversity in respondent pools [6] and other lines of evidence indicate that numerical return of results is not always desired or useful [37]. For example, research participants usually understand genetic risk as a binary concept and tend to search for identifiable threshold figures [38]. When recalling risk values, a majority of research participants exhibit a discordant high perception, meaning that they believe their risk is higher than what they are told at disclosure [20, 39]. Adding to this challenge, patient perspectives towards computer-assisted decision-making differ from decisions made by care or research teams. In a study of patient attitudes towards computerized cognitive screening, participants highlighted both benefits (e.g., reliability) and drawbacks (e.g., lack of consideration of human factors) of computer-mediated decision-making [40]. Moreover, Guan et al. [22] highlight that the process of communicating complex information, specifically the sharing of genomic risk with cognitively impaired participants, can significantly disrupt the centrality of person-centered practice and impede researcher-participant rapport. Communicating complex information may impede opportunities to share health and lifestyle information and ask facilitation statements to clarify a participant’s knowledge and understanding. Taken together, these findings highlight the need to capture participant preferences for disclosure of biomarker results as an integral component of the research process. Recent work by Milne et al. [4], Mozersky et al. [7], and the proposed ‘Bill of Rights’ for study participants by Walter et al. [19], demonstrate the concerted efforts being made to shift the paradigm toward co-creation and increased participant engagement in this space. A notable example is the Advisory Group on Risk Evidence for Dementia (AGREEDementia), convened to promote open, multidisciplinary dialogue around ethical and appropriate disclosure of biomarker information [6]. Further, Largent et al. [12] put forward a 5-step approach to biomarker disclosure, that offers researchers a comprehensive approach for designing and implementing disclosure processes. The approach highlights the need for researchers to consider the return of results in the context of ongoing participation in research, alongside pre- and post-disclosure processes such as pre-test education on the strengths, limitations and implications of biomarker testing, and post-disclosure follow-up to promote participant wellbeing.
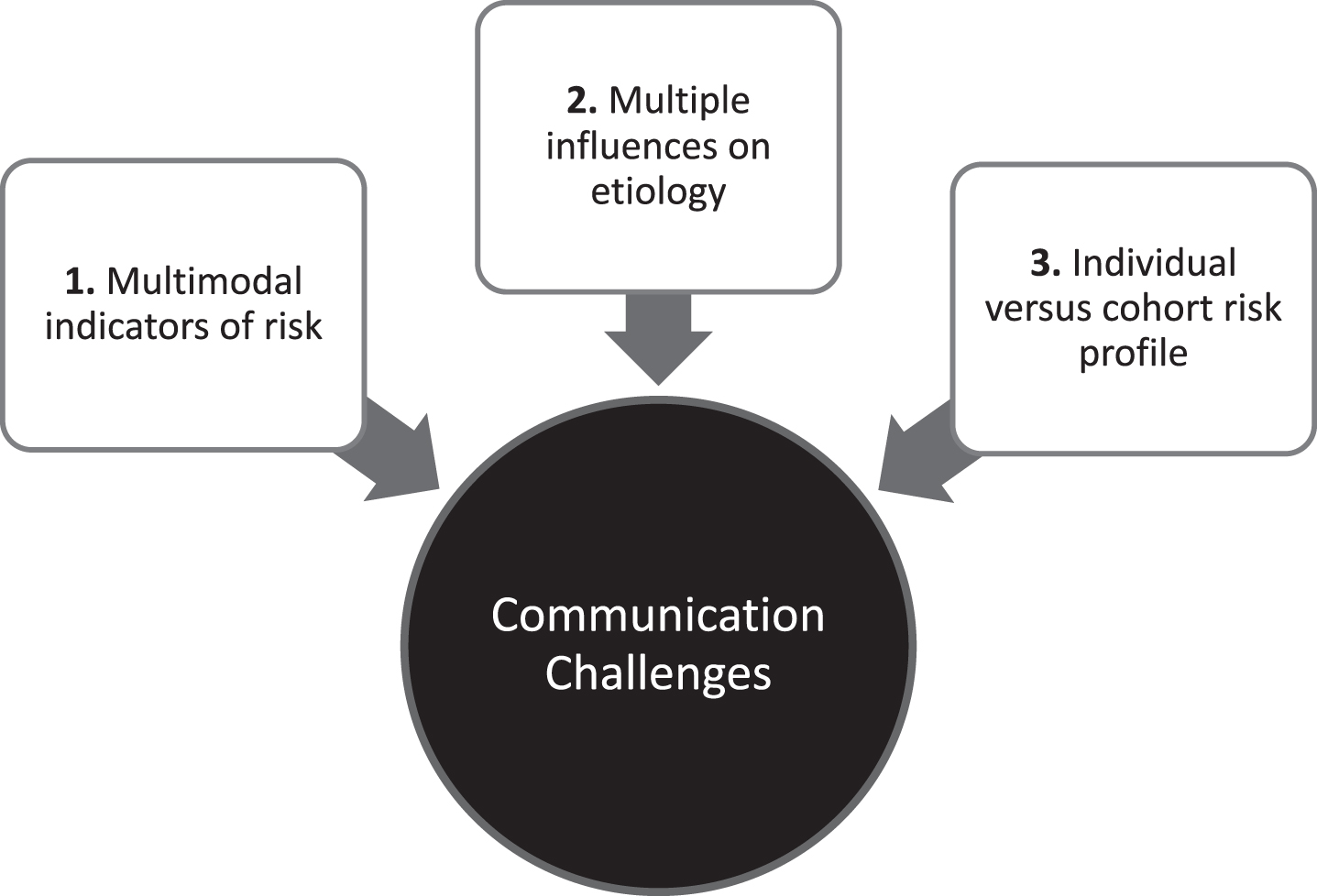
Three key challenges faced by AD/ADRD researchers when communicating biomarker results to participants.
OPTIMIZING THE RETURN OF RESULTS PROCESS: RECOMMENDATIONS FOR FUTURE WORK
Biomarker risk assessments are increasingly reaching further back in the asymptomatic period and broadening the modalities they represent. Correspondingly, the challenge of ethical risk communication becomes greater, and perhaps ever more important. Risk communication must be tailored to participants’ own understandings and must proactively address the notion that simplified understandings of risk play a heuristic role in decision-making in a wide range of contexts, from research participation to personal planning. Researchers should consider the potential benefits and harms of disclosing results that are difficult to interpret: positive lifestyle changes when options exist for decreasing risk [15, 20], health anxiety, poor health decision-making, and financial harm from seeking unproven or inappropriate treatments. While seminal work from the REVEAL study showed that a majority of participants did not experience significant mental health-related harms (e.g., anxiety, depression) following the disclosure of single gene APOE ɛ4 results [41], continued work in this area is required to explore how participants react and adjust to return of results from more complex and multi-modal biomarker panels. Further, researchers should consider study limitations which limit the generalizability and accuracy of said results, such as homogenous sample cohorts or the exclusion of participants with low neurocognitive scores and a history of depression [41, 42]. Return of results processes need to be responsive to the needs of different subgroups of research participants, such as healthy controls, patients at different stages of the disease journey, and belonging to diverse demographic and socioeconomic groups. Although limitations and uncertainties of innovative AD/ADRD research will vary across studies, in communicating with participants, maintaining a foundation of linguistic candor is crucial to limiting misinformation, and the harmful consequences of misused scientific language: truthfulness is an ethical cornerstone that we must respect to safeguard participants and the reputation of our research [43, 44]. In practicing the art of truthfulness and shared decision-making [45], researchers allow for a collaborative exchange of information, that openly acknowledges the uncertainties of innovative research, and limits the propensity for making overstatements, generalizations, or generating false hope, while honoring participants’ individual values, goals, preferences, and risk tolerance [14, 46]. Additionally, when communicating with participants, researchers may consider how to use the term ‘dementia’ with sensitivity and an awareness of the potential negative connotations and social stigma [14].
Therefore, we encourage the research community to plan carefully and to design and disclose the return of results processes within their studies. We acknowledge the pressing need for resources that offer support to researchers in developing the skills necessary for safe and ethical communication [8, 18]. As such, we propose six recommendations for developing and optimizing return of results processes for complex biomarkers as a way to operationalize this call. Embedded in each recommendation is a take-away to elicit clear reporting from researchers around the decision-making and processes for disclosure. The goal of these recommendations is to foster responsible innovation and scientific knowledge exchange and to support the development of best practices in the return of AD/ADRD biomarker results.
CONCLUSION
The return of results of complex biomarkers requires a balance between the specific information and quality of delivery researchers can offer and how participants acquire, extract, interpret, remember, and act on this information. This is a critically important topic for researchers in the life sciences to help establish and continually update frameworks for the responsible and ethical communication of test results. In July 2023, a commercial laboratory company released a blood test for AD for home use “that may help to detect risk of Alzheimer’s disease in an individual.” Although there is a clear need for affordable, accurate, and accessible new assessment measures, healthcare consumers and providers must trust and have confidence in all health technologies assessments. Manufacturers must be forthright in their descriptions and not place short-term profits before an individual’s well-being, particularly in those instances where false-positive results may readily occur.
As precise, novel, and complex biomarkers are continuously emerging, with varying implications for individualized understandings of personal health and subsequent actions participants may pursue, the research community must proceed thoughtfully and truthfully when returning biomarker results to research participant communities.
Footnotes
ACKNOWLEDGMENTS
The authors have no acknowledgements to report.
FUNDING
JMR is grateful for support from the Canadian Consortium on Neurodegeneration in Aging’s (CCNA) Ethical, Legal and Social Implications (ELSI) Cross-cutting Program, the AGE-WELL National Centre of Excellence, and the Alzheimer’s Association. RAD acknowledges support from the CCNA with funding from Alberta Innovates (#G2020000063) and Canadian Institutes of Health Research (#163902).
CONFLICT OF INTEREST
JMR and RAD are Editorial Board members of this journal but were not involved in the peer-review process nor did they have access to any information regarding its peer-review.
All other authors have no conflict of interest to report.
