Abstract
Three decades with the amyloid hypothesis, nearly two with amyloid-PET imaging, and one with testing of anti-amyloid therapy have not yielded benefits to patients with Alzheimer’s disease (AD). It is time to focus on more promising options, e.g., infection, low dose radiation, and atherosclerosis. The relevance of the latter in managing AD has fluctuated from being significant to insignificant. Current methodologies for detecting cerebral atherosclerosis reflect advanced changes in only major arteries. In contrast, 18F-sodium fluoride PET imaging assessing early-stage cerebral atherosclerosis regionally or in the entire vascular bed may provide new insight in this age-related process in dementia.
After three decades of amyloid hypothesis-based research, nearly two testing the role of amyloid-PET imaging, and a last decade conducting several trials with various anti-amyloid therapies for Alzheimer’s disease (AD), it is clear that none of these initiatives have translated to significant benefit for AD patients. Therefore, the medical community was amazed when the FDA – contrary to its own expert panel – granted “accelerated approval” on 7 June 2021 of aducanumab with reference solely to an alleged dose-dependent decrease in cerebral amyloid deposits assessed by PET imaging. The proponents and the FDA claimed that over time this will slow down disease progress [1]. However, re-interpretation of the amyloid PET results by qualified experts indicate that these changes are more likely due to additional cerebral damage than related to a decrease in cerebral amyloid deposits [2].
To avoid more unjustified mistakes such as wasting resources and risk causing significant harm to patients, it is time to abandon the amyloid hypothesis and its consequences (immunotherapy) and focus instead on more logical and biology-based options [3]. Among potential therapeutic options, in this commentary, we will focus on infection as a possible cause of AD, discuss prospects for low-dose radiation treatment, and then emphasize atherosclerosis as a promising domain of research in this disease.
A prominent proponent of infection is Ruth Itzhaki, emeritus professor in Manchester, UK. She spent decades investigating the role of infection in AD [4] and has led the way by assessing the role of herpes simplex virus (HSV1). She believes that repeated HSV1 infections and presence of the
Recently, another surprising suggestion deals with low-dose radiation (LDR) for treatment of AD as proposed by Ceyzériat et al. [6, 7]. This approach was successfully used during World War II to shorten and alleviate the course of ‘atypical pneumonia’ in US marines [8]. Interestingly, this approach is now being tested for treatment of COVID-19 associated pneumonia [9]. The theory is that LDR, like other environmental stimuli such as diet, exercise, etc., may be an alternative to drug therapy in many inflammatory diseases by inducing dose-dependent macrophage polarization, toward either the pro-inflammatory M1 phenotype with high doses or the anti-inflammatory M2 phenotype with non-toxic low doses of no more than 0.5– 1.0 Gy [10].
In this scientific communication, we propose an intensified effort to understand the significance of atherosclerosis in various dementias, including AD. In particular, we wish to point to the critical role of 18F-sodium fluoride (NaF)-PET imaging for the detection of arterial wall molecular calcification as evidence for ongoing, early-phase atherosclerosis in cerebral arteries [11]. The association between atherosclerosis and AD has been debated with opposing views, ranging from no or little [12–15] to a strong or even a potentially causal role in the development of AD [16–19].
Others have stressed
Methods for
Assessment of atherosclerosis in coronary artery atherosclerosis is based on invasive and non-invasive angiography to detect and characterize plaques in the proximal parts of epicardial arteries. As such, the small transmural arteries and arterioles supplying the most ischemic-sensitive subendocardial layers of the myocardium have been neglected but can now be successfully assessed with NaF-PET imaging [28]. Similarly, NaF-PET allows examining the presence and degree of arterial wall microcalcification globally and for various structures that are affected by atherosclerotic plaques within the carotid arteries (Fig. 1). Conventional CT or MR imaging is unable to characterize changes
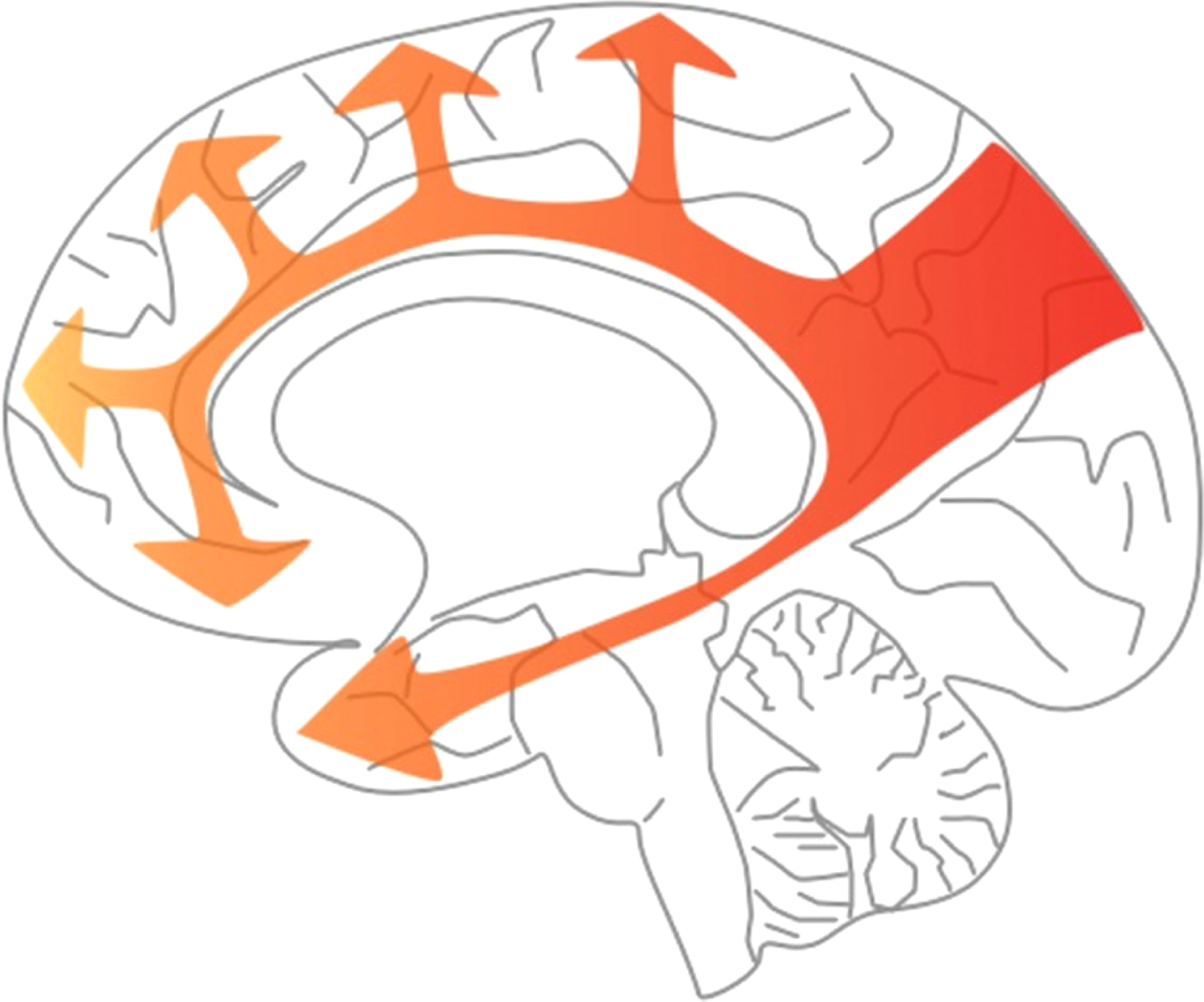
Stereotyped pattern of spread of hypoperfusion in AD. The arrows in this diagram indicate the progression of hypoperfusion, starting from the precuneus, well before the onset of dementia, and spreading to the rest of the parietal cortex and the cingulate gyrus, then the frontal and temporal cortex, largely sparing the occipital cortex until late disease. (This figure was originally published by Love et al. [18] and is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0/"). The figure was not modified.)
Over the past four decades, FDG-PET imaging has been extensively validated for assessing effects of aging and various dementias on brain function. In particular, this approach has been heavily employed for detection of early AD and its course in subjects afflicted with this disease [24]. Furthermore, measurement of atherosclerotic burden in the carotid arteries by FDG-PET and NaF-PET has been proven to be of great value in patients with high risk for this disease [29, 30]. Therefore, combination of NaF-PET and FDG-PET will provide the most powerful imaging modalities for early detection of cerebrovascular disease in patients with various dementias (including AD) and monitoring therapeutic effects of various interventions in this population.
DISCLOSURE STATEMENT
Authors’ disclosures available online (https://www.j-alz.com/manuscript-disclosures/22-0190r1).
