Abstract
Background:
Research suggests that actuarial neuropsychological criteria improve the accuracy of mild cognitive impairment (MCI) diagnoses relative to conventional diagnostic methods.
Objective:
We sought to examine the utility of actuarial criteria relative to consensus diagnostic methods used in the National Alzheimer’s Coordinating Center (NACC) Uniform Data Set (UDS), and more broadly across the continuum of normal aging, MCI, and dementia.
Methods:
We compared rates of cognitively normal (CN), MCI, and dementia diagnoses at baseline using actuarial versus consensus diagnostic methods in 1524 individuals from the NACC UDS.
Results:
Approximately one-third (33.59%) of individuals diagnosed as CN and more than one-fifth (22.03%) diagnosed with dementia based on consensus methods, met actuarial criteria for MCI. Many participants diagnosed with MCI via consensus methods also appeared to represent possible diagnostic errors. Notably, the CNa/CNc group (i.e., participants diagnosed as CN based on both actuarial [a] and consensus [c] criteria) had a lower proportion of apolipoprotein E
Conclusion:
The present results extend previous findings and suggest that actuarial neuropsychological criteria may enhance diagnostic accuracy relative to consensus methods, and across the wider continuum of normal aging, MCI, and dementia. Findings have implications for both clinical practice and research.
Keywords
INTRODUCTION
Research from our group has demonstrated that the use of actuarial neuropsychological criteria [1–3] and cluster-analytic statistical techniques [4–6] enhances diagnostic sensitivity, specificity, and stability, as well as Alzheimer’s disease (AD) biomarker associations in individuals with mild cognitive impairment (MCI) in the Alzheimer’s Disease Neuroimaging Initiative (ADNI) cohort. These empirically-driven methods have yielded distinct cognitive phenotypes (e.g., amnestic, dysnomic, and dysexecutive/mixed MCI) that have also been consistently observed in other study populations (e.g., Mayo Clinic Study of Aging; Framingham Heart Study) [7, 8] but are not well-captured by the conventional diagnostic methods implemented in ADNI. Empirically-driven methods have also led to the identification of a “cluster-derived normal” subgroup in study cohorts such as ADNI that performs within normal limits on comprehensive neuropsychological testing, despite their ADNI MCI diagnosis. Notably, Edmonds et al. [6] showed that 34.2% of individuals conventionally-diagnosed with MCI in ADNI were better classified as cognitively normal (CN) based on cluster analysis (i.e., they performed within normal limits on more extensive cognitive testing relative to a robust normal control group) and thus represented possible false positive diagnostic errors. Further examination of this cluster-derived normal subgroup showed that they had a tendency to overreport subjective cognitive complaints, and had lower rates of functional decline and progression to dementia, a higher rate of reversion to normal cognition, fewer apolipoprotein E (
According to ADNI criteria, a CN diagnosis requires: the presence or absence of subjective memory complaints, verified by a study partner, beyond what one would expect for age; documented normal memory function by scoring above education-adjusted cutoffs on the Logical Memory II subscale (Delayed Paragraph Recall, Paragraph A only) from the Wechsler Memory Scale-Revised (WMS-R; ≥9 for 16 or more years of education; ≥5 for 8–15 years of education; and ≥ 3 for 0–7 years of education); a Mini-Mental State Exam (MMSE) score between 24–30 (inclusive); a CDR® Dementia Staging Instrument score of 0; and the absence of significant impairment in cognitive functions or activities of daily living. A MCI diagnosis requires: a subjective memory concern reported by the participant, study partner, or clinician; documented abnormal memory function by scoring below education-adjusted cutoffs on the WMS-R Logical Memory II subscale (<11 for 16 or more years of education; <9 for 8–15 years of education; and ≤ 6 for 0–7 years of education); a MMSE score between 24–30 (inclusive); a CDR score of 0.5; and general cognition and functional performance that are sufficiently preserved such that a diagnosis of AD cannot be made. Dementia (due to AD) diagnosis requires: a subjective memory concern reported by the participant, study partner, or clinician; documented abnormal memory function by scoring below education-adjusted cutoffs on the WMS-R Logical Memory II subscale (≤8 for 16 or more years of education; ≤4 for 8–15 years of education; and ≤ 2 for 0–7 years of education); a MMSE score between 20–24 (inclusive); a CDR score of 0.5 or 1.0; and that National Institute of Neurological and Communicative Diseases and Stroke/Alzheimer’s Disease and Related Disorders Association (NINCDS/ADRDA) criteria for probable AD are met. The aforementioned studies highlight a number of limitations of conventional diagnostic methods, such as those employed in ADNI. For example, studies of MCI have provided inconsistent support for a relationship between subjective cognitive complaints and objective neuropsychological performance and some have suggested that incorporating self-reported cognitive complaints into diagnostic criteria may confound impressions and result in diagnostic errors [5, 15]. Additionally, while cognitive screening measures may be helpful for identifying individuals who may benefit from more comprehensive evaluation, they are limited in their diagnostic utility [16–18]. Moreover, relying on a single neuropsychological test score to render diagnostic decisions is likely to result in inaccurate diagnoses both due to the heterogeneity of MCI and dementia profiles [1, 19–21] as well as base rates for low test scores and test variability in older adults [22].
A different set of criteria, termed “consensus” criteria, are implemented by the National Alzheimer’s Coordinating Center (NACC). According to NACC criteria, a CN diagnosis requires that the participant does not meet criteria for MCI or dementia (see below). To render an MCI diagnosis, the diagnosing clinician or team must determine if memory impairment is present (i.e., cognitive complaint is supported by evidence of impairment or decline that is not normal for age, yet functional activities are essentially normal, and the extent of impairment/decline is not sufficient to warrant a dementia diagnosis), based on clinical judgment and/or neuropsychological memory test(s). The same clinical and/or psychometric approach is applied to determine whether other cognitive domains are also impaired. Standard criteria for dementia due to AD or for other non-AD dementia disorders are used to guide dementia diagnoses. The NACC consensus criteria are more consistent with current standards of MCI classification (which include complaints of cognitive impairment or decline, objective evidence of cognitive impairment in any domain, and preserved activities of daily living [11, 24]), but are distinct from the specific diagnostic methods used in ADNI in that they do not require memory impairment for a diagnosis and are therefore more amenable to the heterogeneity of MCI. However, both the consensus approach and the conventional approach leave room for subjectivity in diagnostic decision-making given their use of cognitive and functional screening measures and heavy reliance on clinician judgment. Moreover, it is worth noting that NACC diagnoses are made by either a consensus team or a single physician, with the actual process varying according to each center’s specific protocol. Therefore, examination of whether this inherent variability in the consensus methods implemented in NACC reduces diagnostic accuracy is needed. In contrast, actuarial neuropsychological criteria provide a more objective and standardized approach to clinical diagnosis and are likely to enhance diagnostic sensitivity, specificity, and stability relative to both conventional and other consensus diagnostic approaches, particularly in large, multisite studies. Furthermore, the aforementioned studies that examined the utility of actuarial diagnostic methods focused on individuals who were CN or had MCI [1, 15], precluding individuals with more severe cognitive and functional impairment (i.e., dementia). Thus, what also remains unclear is the utility of actuarial neuropsychological criteria across the wider continuum of normal aging, MCI, and dementia.
Here we extend previous investigations of the utility of actuarial neuropsychological criteria by including a novel and more comprehensive analysis of their utility relative to the consensus diagnostic methods implemented in NACC, across the broader continuum of normal aging, MCI, and dementia. Differences in rates of CN, MCI, and dementia diagnoses at baseline, as well as patterns of neuropsychological performance and
MATERIALS AND METHODS
The NACC Uniform Data Set (UDS) was implemented in 2005 by the National Institute on Aging (NIA) Alzheimer’s Disease Research Centers (ADRCs) program with the intention of longitudinally assessing cognitive and other clinical changes in MCI and dementia due to AD and related disorders (e.g., frontotemporal lobar degeneration, Lewy body disease). Consent is obtained at the individual ADRCs, as approved by individual Institutional Review Boards (IRBs). As determined by the University of Washington Human Subjects Division, the NACC database itself is exempt from IRB review and approval because it does not involve human subjects, as defined by federal and state regulations. The present study utilized data from Versions 1.2 and 2.0 of the UDS (the neuropsychological batteries associated with these two versions are identical), collected at baseline visits conducted across 31 ADRCs from September 2005 to March 2015 (alz.washington.edu). The study was conducted in accord with the Helsinki Declaration of 1975.
Participants
Participants included 1,524 individuals (mean age = 78.88 years, standard deviation [SD] = 8.53; 47.80% male; 91.90% non-Hispanic White): 640 were diagnosed as CN, 353 were diagnosed with MCI, and 531 were diagnosed with dementia at baseline based on consensus diagnostic methods used in NACC (see below for further details). These 1,524 participants had sufficient baseline neuropsychological data to facilitate reclassification of cognitive status using actuarial neuropsychological criteria (see below for further details regarding actuarial diagnostic methods). Inclusion criteria included at least six years of formal education and fluency in English or Spanish. Exclusion criteria included history of neurologic injury (including stroke, traumatic brain injury, or seizures); history of a movement disorder (e.g., Parkinson’s disease); elevated psychiatric symptoms at the time of evaluation (e.g., Geriatric Depression Scale score of 6 or higher); or current residence in a skilled nursing facility, nursing home, or boarding home.
NACC consensus diagnostic methods
The NACC UDS includes demographic information, medical history and medication use, clinical and neurological examination findings, behavioral and functional measures (e.g., Functional Activities Questionnaire [FAQ]), clinical ratings of dementia severity (CDR), and neuropsychological test scores. Clinical diagnosis (including characterization of cognitive status as normal, impaired-not-MCI, MCI, or dementia) is made by either a consensus team or by the evaluating physician, and this process varies according to each ADRC’s protocol [25–27]. Clinician judgment is based on a review of all available information, including CDR scores as well as overall appraisal of neuropsychological test performance. While normative calculators for UDS neuropsychological test data that account for age, sex, and education are available to researchers [28], whether these calculators are implemented clinically, and the extent to which this is done consistently across ADRCs, is unclear.
Actuarial neuropsychological criteria
Actuarial neuropsychological criteria that were used to reclassify cognitive status were adapted from the criteria put forth by Jak et al. [1, 2] and incorporated objective performance on neuropsychological testing (see below for further details regarding the neuropsychological battery) as well as informant-reported ratings of each participant’s daily functioning (i.e., FAQ responses). A regression-based approach incorporating robust normative data from individuals identified in the NACC UDS as those who maintained a clinical diagnosis of normal cognitive status across all UDS visits (
Actuarial neuropsychological criteria
Regarding race/ethnicity, preliminary analyses demonstrated that there were no significant differences among Hispanic/Latino, Black or African American, American Indian or Alaska Native, Native Hawaiian or Pacific Islander, Asian, or multiracial groups on raw neuropsychological test scores, whereas non-Hispanic White participants had significantly higher scores compared to all other racial/ethnic groups. Thus, race/ethnicity was coded as a two-level categorical variable (non-Hispanic White, racial/ethnic minority) in the present study.
Neuropsychological battery
Raw neuropsychological test scores were derived from measures encompassing domains of 1) verbal memory (Wechsler Memory Scale [WMS]-III or -R Logical Memory Story A [two separate scores for the Immediate and Delayed Recall conditions], MMSE Orientation [sum of correct items for Time and Place]), 2) language (Boston Naming Test, Category Fluency [two separate scores for the Animals and Vegetables conditions]), 3) attention (Trail Making Test [TMT] Part A, WMS-R Digit Span Forward), and 4) executive functioning/processing speed (TMT Part B, WMS-R Digit Span Backward, Wechsler Adult Intelligence Scale [WAIS] Digit Symbol). Raw FAQ scores were examined as a measure of daily functioning.
APOE ɛ 4 carrier status
Data analysis
Statistical analyses were conducted in the Statistical Package for the Social Sciences (SPSS) Version 26.
Actuarial diagnostic classifications across NACC consensus diagnoses
To reiterate, a regression-based approach was used to generate age-, sex-, education-, and race/ethnicity-adjusted
Demographic characteristics
One-way analysis of variance (ANOVA) and chi-square tests (with Bonferroni corrections for multiple comparisons) were conducted to examine actuarial and consensus diagnostic group differences on demographic variables.
Neuropsychological performance
Multivariate analysis of covariance (MANCOVA) tests (with follow-up univariate tests and Bonferroni-corrected pairwise comparisons) were conducted to examine diagnostic group differences on raw neuropsychological test scores across domains of verbal memory, language, attention, and executive functioning/processing speed, and on the FAQ, controlling for age at baseline (years), sex (male, female), education (years), and race/ethnicity (non-Hispanic White, racial/ethnic minority). First, two separate sets of analyses were conducted using actuarial or consensus classifications (CN, MCI, dementia) as 3-level diagnostic group variables. A third analysis was conducted using a 9-level diagnostic agreement/discrepancy group variable to reflect the exhaustive diagnostic classification scheme reflected in Fig. 1 and Table 4. Participants who were 1) actuarially-diagnosed as CN despite receiving consensus diagnoses of dementia or 2) actuarially-diagnosed with dementia despite being diagnosed as CN based on consensus criteria were included in omnibus tests of diagnostic agreement/discrepancy group differences on neuropsychological performance (and
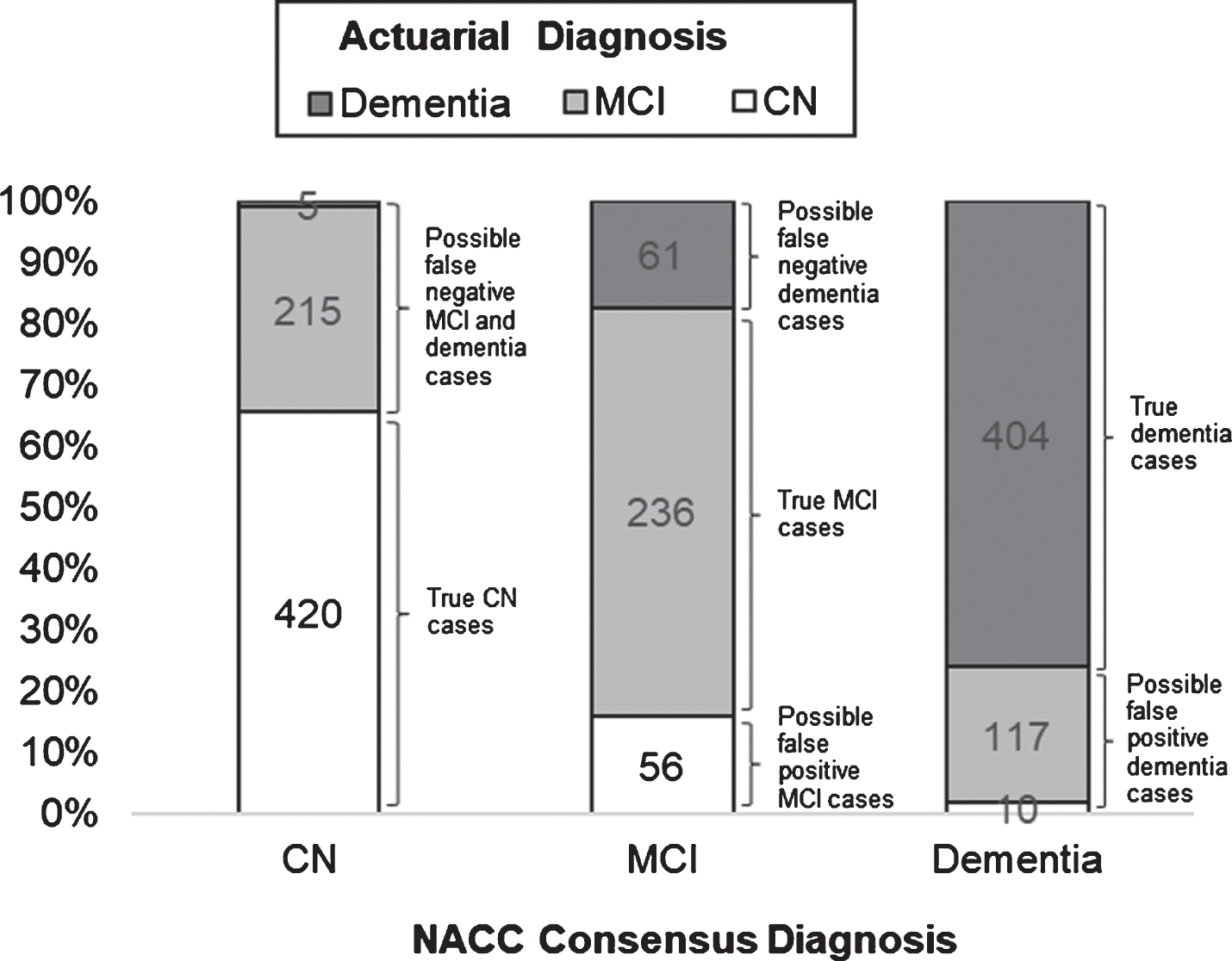
Frequencies and relative proportions of actuarial classifications across NACC consensus diagnoses, with corresponding possible diagnostic errors.
APOE ɛ 4 carrier status
Chi-square tests (with Bonferroni-corrected comparisons) were conducted to examine associations between diagnostic group and
Post-Hoc analyses
RESULTS
Actuarial diagnostic classifications across NACC consensus diagnoses
Frequencies and relative proportions of actuarial diagnostic classifications across NACC consensus diagnoses, with corresponding possible diagnostic errors, are illustrated in Fig. 1. Of the 640 individuals who were diagnosed as CN based on consensus criteria, 420 (65.63%) were actuarially-diagnosed as CN, whereas 215 (33.59%) had MCI and 5 (0.78%) had dementia based on actuarial neuropsychological criteria. Of the 353 individuals who were diagnosed with MCI based on consensus criteria, 236 (66.86%) were actuarially-diagnosed with MCI, whereas 56 (15.86%) were CN and 61 (17.28%) had dementia based on actuarial criteria. Of the 531 individuals who were diagnosed with dementia based on consensus criteria, 404 (76.08%) were actuarially-diagnosed with dementia, whereas 10 (1.88%) were CN and 117 (22.03%) had MCI based on actuarial criteria.
Demographic characteristics
Descriptive and inferential statistics associated with actuarial and consensus diagnostic group differences on demographic variables are provided in Tables 2 and 3, respectively. One-way ANOVA and chi-square tests revealed significant diagnostic group differences on age and sex, with similar patterns observed using actuarial or consensus diagnoses. Regarding age, the CN group was significantly older than both the MCI and dementia groups (
Descriptive and inferential statistics associated with actuarial diagnostic group differences on demographic, genetic, neuropsychological, and functional variables
Descriptive and inferential statistics associated with consensus diagnostic group differences on demographic, genetic, neuropsychological, and functional variables
Neuropsychological performance
Actuarial diagnostic group differences on neuropsychological performance
Tables 2 and 3 displays descriptive and inferential statistics associated with actuarial and consensus diagnostic group differences, respectively, on neuropsychological and functional measures. As expected, MANCOVA and follow-up univariate tests revealed significant actuarial diagnostic group differences on tests of memory (
Consensus diagnostic group differences on neuropsychological performance
MANCOVA and follow-up univariate tests also revealed significant consensus diagnostic group differences on tests of memory (
Diagnostic agreement/discrepancy group differences on neuropsychological performance
Table 4 displays descriptive and inferential statistics associated with diagnostic agreement/discrepancy group differences on neuropsychological and functional measures. Subscripts “a” and “c” are used to indicate actuarial and consensus diagnoses, respectively. Results from MANCOVA and follow-up univariate tests with pairwise comparisons generally demonstrated that 1) the CNa/CNc group performed better than the MCIa/MCIc and MCIa/CNc groups, and 2) the CNa/MCIc group performed better than the MCIa/MCIc group. Similarly, 3) the MCIa/MCIc group performed better than the Dema/Demc and Dema/MCIc groups, and 4) the MCIa/Demc group performed better than the Dema/Demc group. In contrast, performances were comparable between 5) the CNa/CNc and CNa/MCIc groups, 6) the MCIa/CNc and MCIa/MCIc groups, and 7) the MCIa/MCIc and MCIa/Demc groups.
Descriptive and inferential statistics associated with diagnostic agreement/discrepancy group differences on neuropsychological and functional measures and APOE
APOE ɛ 4 carrier status
Chi-square tests revealed significant associations between diagnostic group and
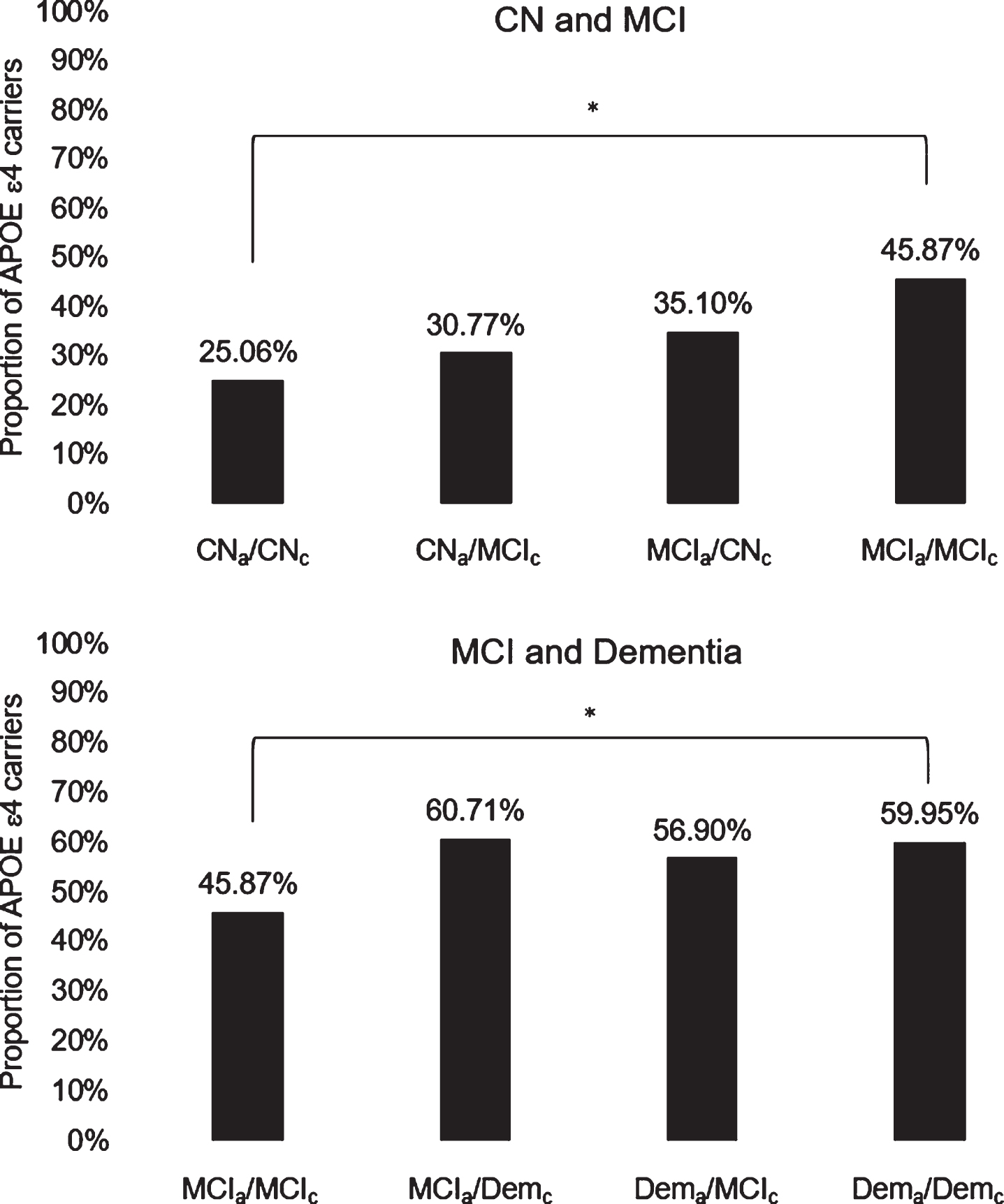
Diagnostic agreement/discrepancy group differences on
Actuarial diagnostic group differences on APOE ɛ 4 carrier status
There was a significant negative trend in the proportions of participants with no
Consensus diagnostic group differences on APOE ɛ 4 carrier status
There was a significant negative trend in the proportions of participants with no
Diagnostic agreement/discrepancy group differences on APOE ɛ 4 carrier status
Table 4 displays descriptive and inferential statistics associated with diagnostic agreement/discrepancy group differences on
An exploratory
Post-hoc analyses of global CDR, total MMSE, and GDS scores
Given the results of our primary analyses,
Global CDR
Analyses revealed significant associations between diagnostic group and global CDR scores using actuarial classifications,
While proportions of participants with a global CDR score of 0 (suggesting normal cognition and functioning, based in part on clinician judgment) significantly decreased across actuarial (CN: 81.89%, MCI: 35.92%, dementia: 0.64%) and consensus (CN: 88.59%, MCI: 8.50%, dementia: 1.51%) diagnostic classifications (
While proportions of participants with a global CDR score of 0.5 (suggesting very mild dementia, based in part on clinician judgment) were highest among individuals diagnosed with MCI and lowest among individuals diagnosed as CN using actuarial (CN: 17.49%; MCI: 57.04%; dementia: 35.74%) and consensus (CN: 11.41%; MCI: 88.67%; dementia: 35.97%) diagnostic classifications (
Total MMSE
Analyses revealed significant associations between diagnostic group and total MMSE scores using actuarial classifications,
GDS
Analyses revealed significant associations between diagnostic group and GDS scores using actuarial classifications,
DISCUSSION
The present study extends previous investigations of the utility of actuarial neuropsychological criteria by including a novel and more comprehensive analysis of their utility relative to the consensus diagnostic methods implemented in NACC, across the broader continuum of normal aging, MCI, and dementia. Analyses revealed that approximately one-third (33.59%) of individuals diagnosed as CN and more than one-fifth (22.03%) diagnosed with dementia based on consensus criteria, met actuarial neuropsychological criteria for MCI (these represent possible false negative MCI cases and possible false positive dementia cases, respectively). Many participants diagnosed with MCI via consensus methods also appeared to represent possible diagnostic errors (15.86% were actuarially-diagnosed as CN and represent possible false positive MCI cases, whereas 17.28% were actuarially-diagnosed with dementia and represent possible false negative dementia cases).
Analyses of diagnostic agreement/discrepancy group differences on neuropsychological and functional measures revealed that the CNa/CNc group (i.e., participants who were diagnosed as CN based on both actuarial and consensus criteria and therefore likely represent true CN cases) performed significantly better than the MCIa/MCIc group (i.e.,participants diagnosed with MCI based on both criteria, likely representing true MCI cases), which in turn performed significantly better than the Dema/Demc group (i.e., participants diagnosed with dementia based on both criteria, likely representing true dementia cases). Moreover, on most neuropsychological measures, performances were comparable between the CNa/CNc (true CN) and CNa/MCIc (possible false positive MCI) groups, and between the MCIa/MCIc (true MCI) and MCIa/CNc (possible false negative MCI) groups. While performances were also largely comparable between the MCIa/MCIc (true MCI) and MCIa/Demc (possible false positive dementia) groups, the Dema/MCIc (possible false negative dementia) group tended to outperform the Dema/Demc (true dementia) group; this is perhaps partly explained by the possibility that our actuarial neuropsychological criteria may have higher sensitivity for dementia and therefore capture more individuals in milder stages of dementia relative to the consensus diagnostic methods implemented in NACC.
Analyses of
A number of attributes associated with the consensus diagnostic methods implemented in NACC may have contributed to the observed discrepancies in classification rates. As was previously noted, determinations of cognitive status in NACC are purportedly based on a review of all available information, including CDR scores (which in part are based on clinician judgment). The present study yielded evidence that global CDR scores are more consistent with consensus diagnoses than with performance on comprehensive neuropsychological testing and corresponding actuarial diagnoses. A
Research also suggests that CDR ratings, as well as subjective cognitive complaints, are susceptible to psychiatric influences [5, 32]. Relatedly, another
The present results extend previous findings showing that the use of actuarial neuropsychological criteria [1, 2] enhances diagnostic sensitivity and specificity as well as AD biomarker associations in individuals with MCI [1, 4–6] by demonstrating the utility of actuarial neuropsychological criteria more broadly across the continuum of normal aging, MCI, and dementia, and that diagnostic errors are not unique to the conventional diagnostic methods used in ADNI. To reiterate, within ADNI, Edmonds et al. [6, 13] found that 34.2% of individuals conventionally-diagnosed with MCI were better classified as CN (based on cluster analysis), and 7.1% of individuals conventionally-diagnosed as CN met actuarial criteria for MCI. In the present study, we found that 15.86% of participants with consensus diagnoses of MCI were actuarially-diagnosed as CN, and 33.59% of participants diagnosed as CN based on consensus criteria met actuarial criteria for MCI. Thus, relative to the conventional diagnostic methods used in ADNI, the consensus diagnostic methods used in NACC may be associated with lower rates of false positive MCI cases and higher rates of false negative MCI cases. However, in addition to differences between the diagnostic methods used in ADNI versus NACC, these discrepancies may also be influenced, at least in part, by inherent differences in demographic and clinical sample characteristics and the number and types of neuropsychological measures available across the two databases.
The results of the present study have significant implications for diagnosis, treatment planning, and other aspects of clinical practice. Consistent with what previous studies have noted, our findings suggest that in order to maximize diagnostic accuracy, clinicians should adopt a comprehensive neuropsychological approach to conceptualization and diagnosis without placing disproportionate weight on subjective complaints, screening measures, or a single impaired neuropsychological test score [6, 32]. Notably, the present study demonstrated that consensus diagnostic methods may result in inaccurate diagnoses of both MCI and dementia. These diagnostic errors, in addition to inaccurate diagnoses that underestimate one’s level of cognitive or functional impairment, can have inadvertent albeit significant consequences. Using actuarial methods in clinical settings to maximize diagnostic sensitivity and specificity is likely to: 1) increase opportunities for valuable intervention (e.g., cognitive rehabilitation, intensive monitoring and/or treatment of relevant medical risk factors, referrals to other appropriate healthcare providers, long-term planning or care) for those who are appropriate candidates and may benefit from such resources; as well as 2) reduce the risk of placing unnecessary or premature restraints on patients’ independence, or increased burden on family members or other caregivers.
Our results also have significant implications for research studies and clinical trials. Enhancing diagnostic sensitivity and specificity through the use of actuarial neuropsychological criteria can improve the rigor of clinical research studies attempting to characterize the preclinical and MCI stages of AD or other neurodegenerative disorders [6, 13]. Reducing diagnostic errors is likely to strengthen observed associations with regard to diagnosis, biomarker abnormalities, rates of progression and reversion, and drug or other intervention effects [33]. Relatedly, Emrani et al. [34] recently discussed the importance of leveraging statistical modeling techniques based on neuropsychological test performance in AD diagnosis and classification schemes, in light of growing evidence for the heterogeneity of underlying neuropathological processes contributing to neuropsychological phenotypes observed along the AD continuum, including in the dementia stage.
Notable strengths of the present study include the use of a large sample and robust norms for generating demographically-adjusted standardized scores on a comprehensive battery of neuropsychological tests. Relatedly, another strength of the present study was the inclusion of race/ethnicity in demographic adjustments of neuropsychological scores. Additionally, we were able to conduct a more comprehensive analysis of diagnostic group differences on
The present study is not free of limitations. Tests of visuospatial functioning or visual memory were not incorporated into actuarial neuropsychological criteria, as more comprehensive measures of these skills were not included in the NACC UDS until Version 3, which was implemented in September 2015, and we opted to use data from Versions 1.2 and 2.0 to maximize our sample size. In addition, while participants in the NACC UDS reflect the demographic characteristics of individuals who participate in Alzheimer’s and dementia research in the U.S., they are not entirely representative of the general population given their substantially higher average level of education and predominantly Caucasian composition. Moreover, given the relative heterogeneity in NACC diagnostic methods (diagnostic decisions are based on a review of all available information and made either by a consensus team or the evaluating physician, and this process varies across ADRCs), it is possible that, in some cases, the neuropsychological tests that were considered in assigning NACC diagnoses were also incorporated into actuarial diagnoses. In contrast, previous studies conducted by our group using ADNI data incorporated memory tests into actuarial criteria that were independent from those that were used to assign ADNI diagnoses. Furthermore, analyses in the present study focused on neuropsychological performance at baseline, and the extent to which actuarial neuropsychological criteria would yield more accurate progression and reversion rates in the NACC UDS is unclear. Given that other studies have provided evidence for enhanced diagnostic stability using actuarial criteria in ADNI [3, 13], future studies should examine and compare the stability of actuarial versus consensus diagnoses in the NACC UDS. Finally, further investigation of associations between actuarial and consensus diagnoses and other biomarkers available in NACC (e.g., neuroimaging, neuropathology) is warranted.
In sum, our findings highlight the utility of actuarial neuropsychological criteria in enhancing diagnostic sensitivity and specificity at baseline across the continuum of normal aging, MCI, and dementia in the NACC UDS. These findings have implications for improving characterizations of the preclinical and manifest stages of AD or other neurodegenerative disorders in research, as well as diagnosis and treatment planning for individuals with MCI or dementia.
Footnotes
ACKNOWLEDGMENTS
This work was supported by the NIH (R01 AG049810 to M.W.B.; L.V.G. is also supported by P30AG059299), the Alzheimer’s Association (AARG-17-500358 to E.C.E.; AARF-17-528918 to K.R.T.), and the U.S. Department of Veterans Affairs Clinical Sciences Research and Development Service (CDA-2 1IK2 CX001415 to E.C.E.; CDA-2 IK2 CX001865to K.R.T.). The NACC database is funded by NIA/NIH Grant U01 AG016976. NACC data are contributed by the NIA-funded ADRCs: P30 AG019610 (PI Eric Reiman, MD), P30 AG013846 (PI Neil Kowall, MD), P30 AG062428-01 (PI James Leverenz, MD) P50 AG008702 (PI Scott Small, MD), P50 AG025688 (PI Allan Levey, MD, PhD), P50 AG047266 (PI Todd Golde, MD, PhD), P30 AG010133 (PI Andrew Saykin, PsyD), P50 AG005146 (PI Marilyn Albert, PhD), P30 AG062421-01 (PI Bradley Hyman, MD, PhD), P30 AG062422-01 (PI Ronald Petersen, MD, PhD), P50 AG005138 (PI Mary Sano, PhD), P30 AG008051 (PI Thomas Wisniewski, MD), P30 AG013854 (PI Robert Vassar, PhD), P30 AG008017 (PI Jeffrey Kaye, MD), P30 AG010161 (PI David Bennett, MD), P50 AG047366 (PI Victor Henderson, MD, MS), P30 AG010129 (PI Charles DeCarli, MD), P50 AG016573 (PI Frank LaFerla, PhD), P30 AG062429-01(PI James Brewer, MD, PhD), P50 AG023501 (PI Bruce Miller, MD), P30 AG035982 (PI Russell Swerdlow, MD), P30 AG028383 (PI Linda Van Eldik, PhD), P30 AG053760 (PI Henry Paulson, MD, PhD), P30 AG010124 (PI John Trojanowski, MD, PhD), P50 AG005133 (PI Oscar Lopez, MD), P50 AG005142 (PI Helena Chui, MD), P30 AG012300 (PI Roger Rosenberg, MD), P30 AG049638 (PI Suzanne Craft, PhD), P50 AG005136 (PI Thomas Grabowski, MD), P30 AG062715-01 (PI Sanjay Asthana, MD, FRCP), P50 AG005681 (PI John Morris, MD), P50 AG047270 (PI Stephen Strittmatter, MD, PhD).
