Abstract
BACKGROUND:
The Lichtenstein’s and Kugel’s procedures for inguinal hernia repair have been compared in terms of immediate complications, including hematoma, testicular pain and wound infection, and long-term outcomes such as chronic pain.
OBJECTIVE:
The aim of the present study was to compare trunk muscle strength, quality of life (QoL), and neuropathic pain (NP) components using a prospective controlled study following the above two procedures.
METHODS:
Sixty consecutive patients underwent elective inguinal hernia repair from 2013 until 2014. Thirty patients were operated using standard Lichtenstein, while 30 were treated with a Kugel patch. Six months after initial surgery, trunk muscle strength and patient QoL were evaluated. Additionally, 40 healthy volunteers, matched for age and sex, were recruited for comparison. Trunk muscle strength was measured isokinetically, whereas QoL and pain level were assessed using the Short Form 36 (SF-36) and the PainDETECT questionnaire (PD-Q), respectively.
RESULTS:
Mean peak moment of trunk flexion and trunk flexor-extensor (agonist/antagonist) ratio were significantly lower in patients than in controls, while no differences were observed between the two surgery groups. In addition, trunk extension strength was mearly identical in all there (2 experimental, 1 control) groups. Only two patients in the Lichtenstein group and one patient in the Kugel group showed a PD-Q score over 19 and NP component. There was no difference in the PD-Q scores and SF-36 domains between the different surgery groups.
CONCLUSIONS:
Based on the outcome parameters evaluated in this study, none of the two surgical interventions is superior to the other. Therefore, the particular choice of surgical procedure should rely on other factors.
Introduction
Inguinal hernia repair is a widely known surgical procedure with successful outcomes, minimum postoperative sequela, short-term recovery, and no long-term complications. However, the appropriate surgical method for inguinal hernia repair remains controversial [1]. The choice of the surgical technique to be used is at the discretion of the surgeon, based on the patient profile and prior surgical history [2]. Tension-free hernioplasty, known as Lichtenstein procedure, is currently one of the most popular techniques for repair of inguinal hernias [1, 2]. Furthermore, Kugel described a pre-peritoneal tension-free technique that aimed to combine the utility of the open operation with the advantages of minimal access procedures [1, 2, 3].
Lichtenstein’s and Kugel’s methods have been compared in terms of immediate complications, including hematoma, testicular pain and wound infection, and long-term outcomes such as chronic pain [4, 5, 6, 7]. Recurrence rates and chronic groin pain were the primary endpoints of these two procedures [4, 6, 7]. However, reduced trunk muscle strength and quality of life (QoL) are critical parameters closely related to patient satisfaction [8, 9]. To our knowledge, there are no studies that have compared these two surgical approaches to assess QoL and trunk muscle strength. In addition, neuropathic pain (NP) is caused by a disease of the somatosensory system, which markedly influences QoL [10].
The aim of the present prospective controlled study was to compare trunk muscle strength, QoL, and NP between the Lichtenstein and Kugel procedures. The null hypothesis is that there is no difference between Lichtenstein’s and Kugel’s methods in terms of trunk muscle strength, QoL, and NP component.
Methods
This prospective, controlled study was conducted between December 2013 and February 2014 at Konya Training and Research Hospital. The study and the protocol were approved by the Local Ethics Committee of Selcuk University and received a trial registration number (Number 2013/40). Written informed consent was obtained from all patients. The study was registered with ClinicalTrials.gov, number NCT02871583. The study included 60 consecutive patients who underwent elective inguinal hernia repair from 2013 to 2014; 30 underwent a standard Lichtenstein repair and 30 a Kugel patch. Patients were not randomized to the Lichtenstein or Kugel groups. Type of operation was at patients’ and surgeons’ discretion. Moreover, 40 healthy volunteers who were sex-, age-, and body mass index (BMI)-matched constituted the control group.
Sample size
The number of participants included in this study was determined based on trunk muscle strength. Using Karahan et al.’s findings [11], the sample size was based on a power of 80% (beta: 0.2), a dropout rate of 3%, and statistical significance (alpha: 0.05) of 95% (
Inclusion criteria
Signed written informed consent Male sex (to minimize the effect of sex on muscle strength) Patients between 18–65 years old No prior surgical history Patients within 6–12 months follow-up Ability to speak, read, and write Turkish
Infections or tumors of the spine Systemic bone or joint disorders (e.g., rheumatoid arthritis) Unstable cardiovascular and pulmonary diseases Polyneuropathies and musculoskeletal system diseases Presence of a diagnosed severe psychiatric disorder Presence of severe pain Regular exercise participation (this may affect muscle strength significantly) Recurrent hernia repair Presence of bilateral inguinal hernias or concurrent femoral hernia BMI
Surgical approaches
All surgeries were performed by experienced surgeons and under local, general, or combined anesthesia.
Tension-free repair (Lichtenstein method) was performed in its standard form. A light-weight polypropylene mesh was placed over the posterior wall of the inguinal canal after reduction of the hernia sac and was fortified with polypropylene (Propilene, Dogsan Surgical sutures, İstanbul, Turkey) sutures. The hernia sac was not excised or transfixed.
The Kugel method was applied as described in previous studies [4, 6]. A small
Set-up of the isokinetic dynamometer (Biodex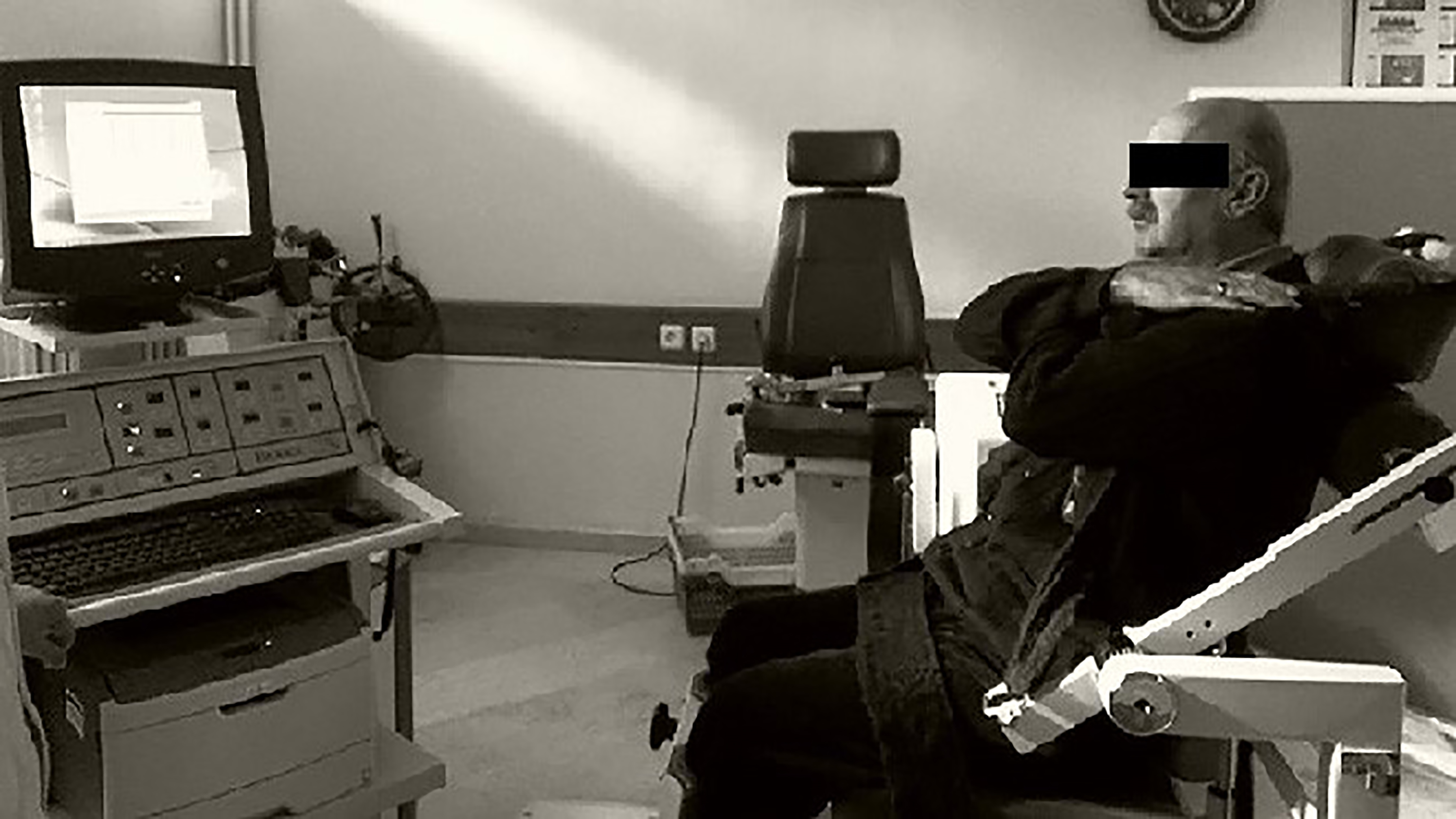
Demographic characteristics, follow-up time, and hernia type by group
*SD: Standard deviation, **BMI: Body mass index.
Isokinetic muscle strength evaluation by group
*
Two physiatrists conducted the evaluations six months after surgery and were blinded to the surgical method. Before assessment, patients were evaluated for recurrence of their hernia. Patients were evaluated with the following parameters:
Trunk muscle strength measurement was performed using the Biodex System 3Pro Multi-Joint System Isokinetic dynamometer (Biodex Medical Inc., Shirley, NY, USA). For the isokinetic strength test, patients were instructed to perform exion and extension of the back with maximum effort three times at 60 Short-Form 36: The Short Form 36 (SF-36) is a 36-item, self-report questionnaire that patients often complete with assistance from the medical team. It is one of the most widely used patient reported outcome parameters to assess health-related QoL and has been shown to distinguish between participants with different severity levels of disease or chronic conditions [13]. It is composed of eight scaled scores, which are the weighted sum of the questions in each section. The eight parts are vitality, physical function, bodily pain, general health perceptions, physical role function, emotional role function, mental health, and social function. The last two scores represent the physical and mental component summaries. Each scale is directly transformed into a numerical score based on a 0–100 scale on the assumption that each question carries equal weight. Lower score reflects greater disability; higher score reflects greater QoL based on lower disability [13]. The PainDETECT questionnaire: The PainDETECT questionnaire (PD-Q) was developed to detect neuropathic signs and symptoms and has been validated for the Turkish Population. PD-Q is a simple, self-administered, questionnaire with high sensitivity and positive predictive accuracy that was designed to screen for NP components without physical examination. PD-Q contains four independent sections [14]. The first part consists of three questions with a 10-point Likert scale format with footnotes in the scale ends (0
SPSS for Windows Version 16.0 software (SPSS Inc. Released 2007; SPSS for Windows, Version 16.0. SPSS Inc., Chicago, IL, USA) was used for statistical analysis. For non-parametric values that comply with normal distribution, the one-sample Kolmogorov-Smirnov test was applied. The Student
Results
Sixty men (mean age: 48.2 years old) and 40 sex-, age-, and BMI-matched healthy participants were included in this study. The average follow-up period after hernia repair surgery was 8.7 months. Table 1 shows demographic characteristics during the follow-up and hernia type within groups (Table 1).
Neuropathic pain component and quality of life parameters by group
Neuropathic pain component and quality of life parameters by group
Mean peak moments for trunk flexion and agonist/antagonist (flxn/extnsn) ratios were significantly lower in the Lichtenstein and Kugel groups than in the control group (
This prospective controlled trial, comparing the Kugel hernioplasty with Lichtenstein repair technique, showed no difference between the two methods in terms of trunk muscle strength, QoL, and NP parameters. Mean peak moment and agonist/antagonist (flxn/extnsn) ratio, as a measure of isokinetic muscle strength, was significantly lower in both surgery groups than in the control group (
The mechanical measurement of trunk muscle strength is an objective approach, frequently used in recent surgical studies [8, 15, 16]. Weakened abdominal muscles are thoroughly associated with inguinal hernias, particularly the direct type of hernias [3]. Inguinal hernias may occur at any age [1, 3]. However, men over 40 years old are more likely to have direct inguinal hernia because of their weakened abdominal wall [1, 3]. Thus, reduced muscular strength of the trunk muscles after inguinal hernia repair may be an anticipated outcome. Moreover, scarred inguinal region muscles, sedentary lifestyle after surgery or weight gain may weaken the abdominal muscles even further. den Hartog et al. [8] measured the abdominal muscle strength to compare two types of operative techniques for incisional hernias. They reported a higher peak moment for a two-layered suture technique without mesh than for a laparoscopic technique, after adjustment for sex [8]. Gunnarsson et al. [16] studied the validity and reliability of measurements of abdominal muscle strength by using the Biodex System in patients with ventral hernia compared to healthy volunteers. They suggested that this method was reliable and valid to assess patient-related endpoints in the evaluation of a ventral hernia and to compare muscle function after different abdominal wall reconstruction techniques [16]. Isokinetic dynamometry was also used to study the effects of breast reconstruction on abdominal strength, focusing on the differences between two abdominal flaps [15]. To the best of our knowledge, this is the first study that compares the impact of Kugel and Lichtenstein operations on trunk muscle strength parameters. Future studies may investigate the recurrence rate in patients with reduced trunk muscle strength. A higher prevalence of chronic back pain is associated with weakened trunk muscles after different surgeries [11]. However, after hernia repair, the clinical relevance of reduced trunk muscle strength and the correlation between chronic groin pain is not yet known.
QoL is often defined as how an ailment affects an individual’s physical health, life satisfaction, family, employment or education, religious beliefs, and wealth [13]. QoL, as an outcome, is an important parameter, similar to other traditional endpoints such as laboratory values [13]. Measuring the health-related QoL after surgery is crucial for decision making by surgeons and patients [17]. The use of QoL measures in surgical trials is increasing. Poobalan et al. [18] questioned patients who underwent inguinal hernia surgery and claimed that social functioning, mental health, and pain dimensions of the SF-36 scores were associated with chronic pain and were significantly lower in patients with chronic pain. Bignell et al. [19] presented the results of a 10-year prospective follow-up study. They studied QoL and chronic pain parameters for bilateral and recurrent inguinal hernia patients and compared laparoscopic versus open mesh repair techniques. According to their results, the incidence of chronic pain was 12% after 10 postoperative years for recurrent or bilateral hernias [19]. While there was no significant difference in QoL parameters between the two surgery groups, QoL was significantly reduced in patients with chronic pain [19]. Singh et al. [20] compared chronic groin pain, QoL, and testicular dysfunction, after laparoscopic and open mesh repair. They found that QoL (in terms of physical functions, SF-36 role-physical, bodily pain, and general health) was significantly better after laparoscopic repair, and the severity and incidence of chronic groin pain were significantly less with activity after laparoscopic repair [20]. The present findings do not show any significant differences between Kugel and Lichtenstein methods in any SF-36 domains.
This study also identified the presence of NP with an instrument to screen for the likelihood that pain is of neuropathic, rather than nociceptive, origin. While some measuring devices include a requirement for clinical examination, PD-Q does not require clinical examination, and is easy to use in surgery clinics because it is a fully patient-reported questionnaire validated for the screening and identification of NP components [14]. The incidence of chronic pain after hernia repair varies from 0 to 37% [21, 22]. Dasari and Grant [5] studied immediate and long-term postoperative outcomes of Kugel and Lichtenstein repair of an inguinal hernia in a retrospective trial. Only 1.6% of patients in the Kugel group and none in the Lichtenstein group complained for severe chronic pain. According to this study, there was no significant difference in the immediate and long-term complications between the two operations [5]. However, there is no report of the NP outcome in their study. Karaman et al. [23] studied 204 patients after hernia repair with the Lichtenstein method and reported that 11.2% of patients had chronic pain six months after surgery. They concluded that almost half (48%) of the patients with chronic pain had an NP component [23]. Hompes et al. [24] reported the incidence and severity of chronic pain after the first year of hernia repair with the Kugel method. They found that 15.1% of 377 patients had chronic pain one year after surgery and suggested that the Kugel method was related to less nerve damage and subsequent NP. In these two studies, the NP component was assessed according to the authors’ definition and reported as NP, without using any specific tool to assess NP. However, according to Lange et al. [25], there is no precise demarcation between neuropathic and nociceptive pain, and the complexity of diagnosis is influenced by several factors including social, genetic, and psychological factors [25].
The main limitation of this trial is that the study population included only men as trunk muscle strength certainly depends on sex; therefore, women were excluded from the study. The present findings could not be extrapolated to the general population. Moreover, exclusions of recurrent herniations and severely (BMI
Conclusion
Our results revealed no significant differences in terms of trunk muscle strength, NP components, and QoL parameters between Lichtenstein and Kugel methods. However, trunk flexion strength and agonist/antagonist ratios were significantly lower in both surgery groups than in healthy controls. After recovery from surgery, it is important to strengthen the abdominal muscles with exercise. Nevertheless, the relationship between reduced trunk flexion strength and recurrence rates after surgery should be investigated in further studies.
Footnotes
Conflict of interest
There are no conflicts of interest regarding the submission and publication of this manuscript and its potential implications. This research received no specific grant from any funding agency.
