Abstract
It has been reported that majority of cases of gigantomastia, also known as breast hypertrophy and macromastia, occur during either pregnancy or puberty. Gigantomastia is a rare disorder that does not have a clear etiology or well-established risk factors. We present a 26-year-old female patient who appeared to have pregnancy-associated gigantomastia recurrence, large accessory breast and, ectopic breast tissue at external genital three years after bilateral breast reduction surgery. The patient successively underwent bilateral mastectomy and vulvar tumor resection. Breast hypertrophy and progenital ectopic breast were pathologically confirmed. This the first case of gigantomastia reported worldwide.
Keywords
Introduction
Macromastia is clinically characterized by huge breast, distention and heaviness, tight skin, sense of pressure in the chest, usually accompanied by chronic mastitis and pain and even skin erosion under breast. This paper introduces rare case that after treatment, one patient who experienced breast hypertrophy during puberty and pregnancy [1], huge supernumerary breast and ectopic breast tissue, went back to normal [2]. Therefore, patients with macromastia longing for pregnancy in the future can consider to cut bilateral mammary glands and then to reconstruct.
Case report
A 26-year-old G1P0 woman reported that her bilateral breasts developed rapid and irregular enlargements and combined with vulvar tumor breast started at 12 weeks of gestation. From the third mouth of gestation, the patient found that her upper outer quadrant of bilateral breasts near the axillae both had tumors with a size of approximately 3
Juvenile macromastia The patient suffered from gigantomastia when she was 22 years old, the breast reaching below the umbilicus while in the standing position.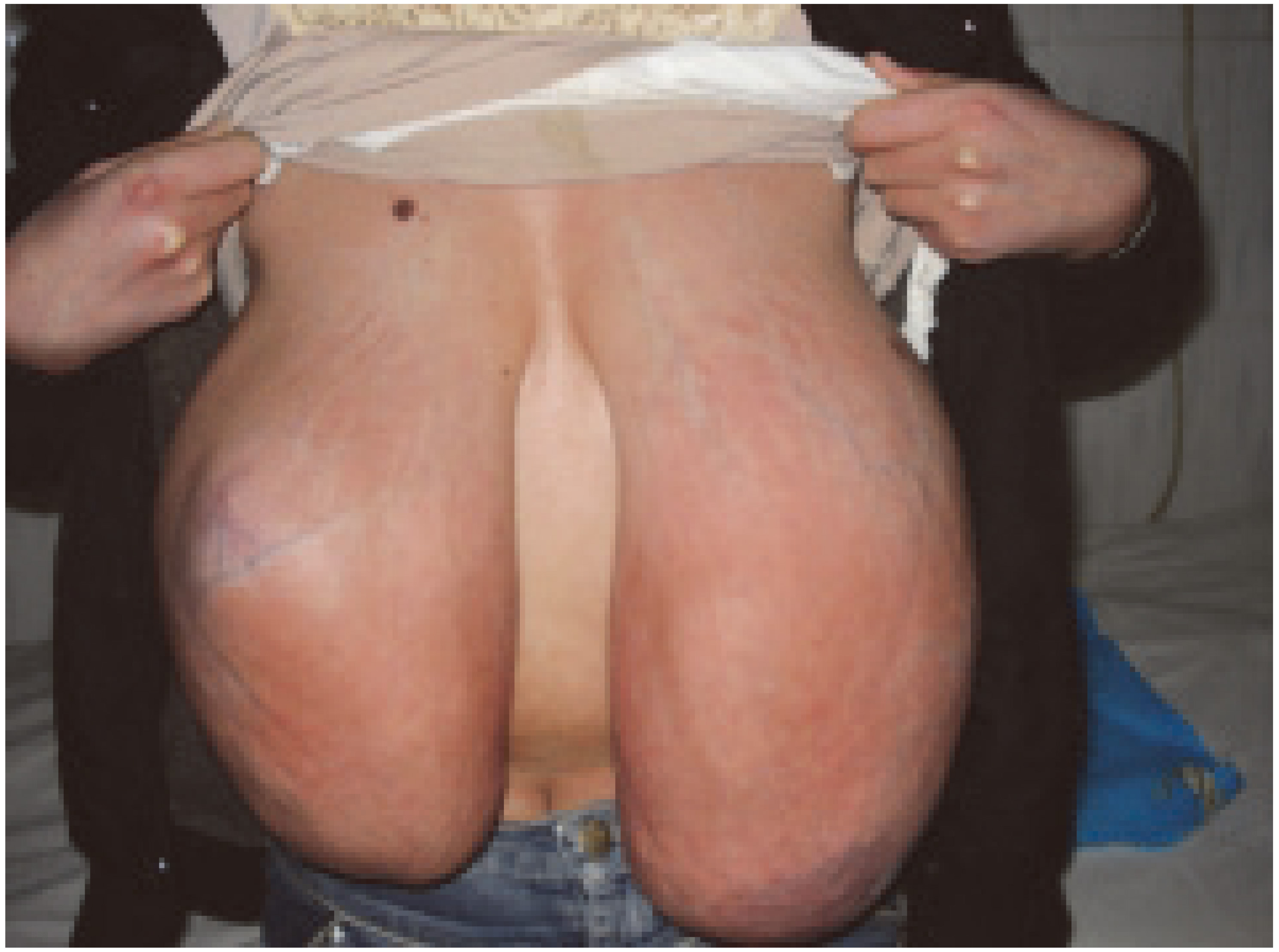
The patient was conducted with bilateralreduction mammaplasty in 2009.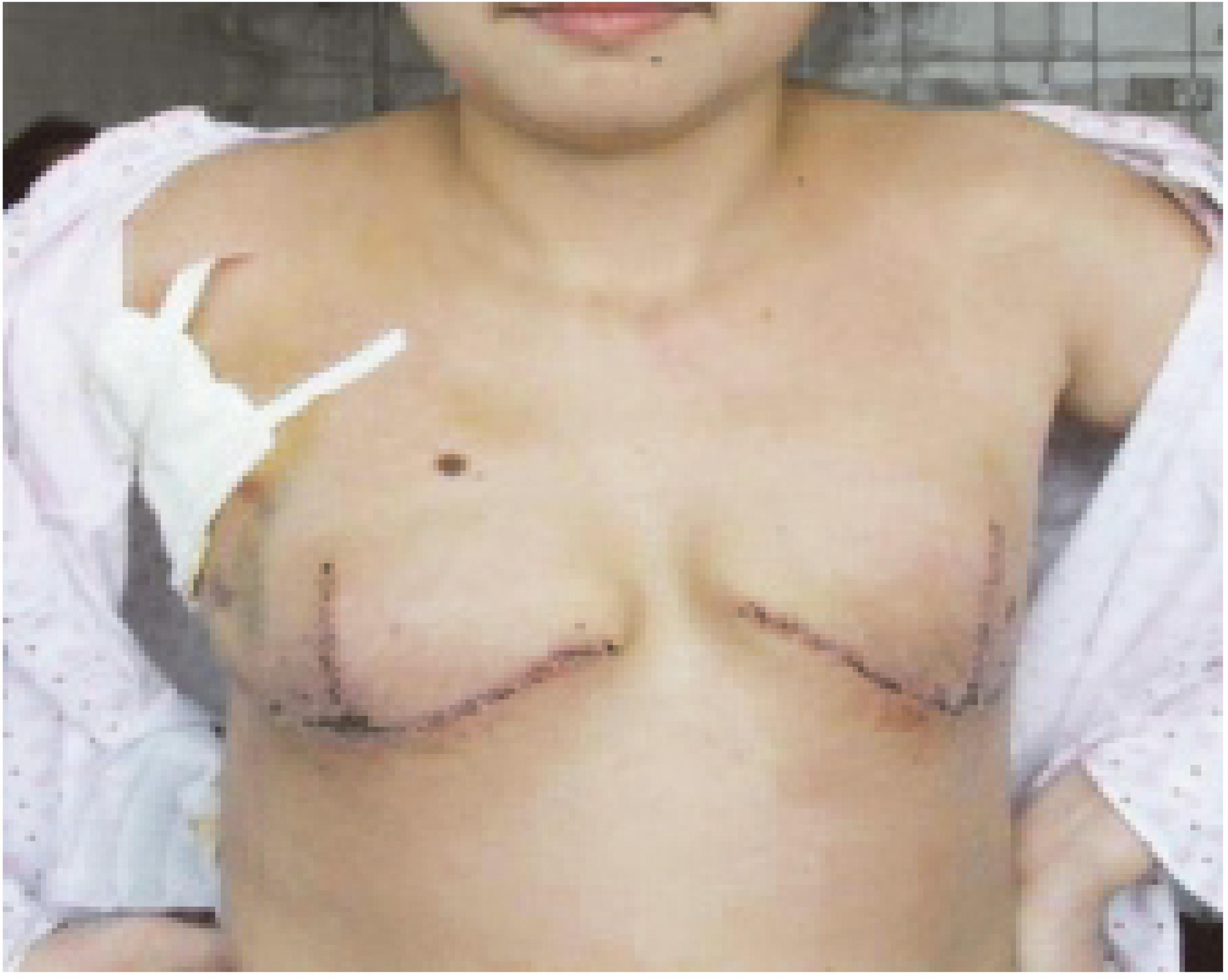
Patient with gestational gigantomastia at 36 weeks Huge bilateral breast and axilla accessory breast with subcutaneous venous filling, right axilla accessory breast formed ulceration with odor.
Progenital ectopic breast tissue Four soft tumors with a petal shaped on the bilateral labium majus pudendi, maximum mass of approximately about 6 
Gigantomastia, also known as breast hypertrophy and macromastia, has been reported to occur during either pregnancy or puberty mostly. This was first introduced by Palmuth in a German literature in 1648 [3]. To date, merely approximately 100 cases have been reported in literature [3, 4]. The incidence of gigantomastia occurring in pregnancy is 1:28,000–1:100,000 [5]. The incidence of ectopic breast tissue is 1–6% [6], and patients who suffer from both at the same time are even rarer. We present a patient who also experienced juvenile macromastia, gestational gigantomastia and great accessory breast, vulvar ectopic breast tissue. This is exceedingly rare.
Gigantomastia can be divided into three categories according to etiology: idiopathic, drug-induced and endocrine etiologies (mainly including puberty and pregnancy) [7]. Idiopathic macromastia is divided into two categories according to BMI: BMI
Juvenile and pregnancy gigantomastia are most common in clinic, often performed for progressive breast enlargement, usually require surgical treatment. In addition, some scholars consider that this disease is associated with autoimmune diseases and malignant tumors [5, 9]. Therefore, lymphoma breast malignant tumors should be identified and differentiated with gigantomastia.
In this report, we present a patient with juvenile macromastia, gestational gigantomastia, large axillary accessory breast and vulvar ectopic breast tissue. However, its pathogenesis remains unknown, but various factors have been proposed. These include over-sensitivity to or over-production of hormones such as estrogen, human chorionic gonadotrophin, human placental lactogen, and prolactin [10]. Furthermore, the patient has a history of hyperthyroidism, intermittently took propylthiouracil for five years without regular monitoring thyroid function, and suffered from gigantomastia after self withdrawal for two years without regular medication and monitoring of thyroid function. The free thyroid hormone was lower than normal before bilateral mastectomy. In addition, it was reported that thyroid hormones may have a confrontation of the value added effect of estrogen on breast tissue, which can increase the binding of sex steroids and reduce the activity of estrogen on breast tissue. On the contrary, reduced thyroid function may lead to the excessive growth of breast tissue through increased sensitivity of mammary epithelial cells to estrogen, prolactin, etc. [11]. Three years after bilateral breast reduction surgery, gigantomastia rapidly recurred during her pregnancy. There is no clear association between the excessive breast growth and the number of pregnancies that the patient has had, although this condition is more common in multiparas [1, 3, 12, 13]. Some theories have suggested that gestational gigantomastia may be related to placental hormones [3, 5]. This rapid enlargement in breast volume occurs most commonly at the end of early pregnancy, coinciding with the period of peak gonadotropin production; thus, strengthening the hypothesis of a hormonal association. However, many cases of gigantomastia have occurred under normal hormone levels or even after medical suppression with bromocriptine [4]. Even with high estrogen and prolactin levels, macromastia continued to develop. Thus, it is unclear whether such levels, which are normally elevated during pregnancy, are pathogenic [14, 15]. In this report, we present a patient who had a recurrence of gigantomastia after bilateral breast reduction surgery. Some authors have suggested that the recurrence rate in patients undergoing breast reduction surgery is higher than in bilateral mastectomy, and the main factor was residual hypertrophic breast tissues [4, 16].
Mamma accessoria begins in the embryonic development stage, when the carcass length is approximately 9 mm (the sixth week of embryonic development). Two lines from both sides of the axillary to the groin have 6–8 pairs of primordial breast. Before birth, except for the pair on chests, the rest have been degraded. Relatively few women retain extra mammary glands, which is called axillary breast. The incidence of female ectopic breast accounted for approximately 2–6% [17], and 95% of which occurred in the anterior axillary fold. Other rare parts include the chest wall, abdomen, groin and thigh; and it can also occur in the perineal [18, 19]. Different symptoms would be revealed before or after the menstrual period, and during pregnancy or lactation, since these are regulated by hormone levels such as estrogen, progesterone and prolactin [20]. Combined with the patient’s history, the investigators of this study concluded that the cause of the disease is related to the following factors [1]. Disorder in hormone levels. In the process of pregnancy, hormone levels greatly changes, and progesterone continuously increases; promoting the growth of the mammary gland [2]. Breast tissue and ectopic breast tissue are target organs of estrogen, progesterone, prolactin, etc. The growth regulation of immature breast tissues becomes uncontrollable under the action of the hormone [3]. Developmental abnormalities. The patient also had gigantomastia and progenital ectopic breast tissue; however, the etiology of the vulvarectopic breast tissue remained controversial. A hypothesis was put forward during 19
As a result of the substantial increase in the size of the breasts, physical complications continued to develop including severe pain, ulcerations, infection, hemorrhage, supine respiratory distress, postural problems and so on. In addition to the effect of the condition on the patient’s psychological status, this directly affected the pregnancy of the patient [22, 23, 24]. If the patient does not receive the appropriate treatment on time, secondary infection may occur such as puerperal mastitis, pyogenic abscess, and sepsis [23, 24, 25]. For patients with gigantomastia, in addition to physical pain, patients often suffer from more psychological trauma due to their pathological appearance such as depression, and even social phobia [4, 10]. Gestational gigantomastia treatment varies on a case-to-case basis, and mainly includes conservative measures and surgical treatment. Conservative measures include proper brassiere support, physical therapy, analgesia, muscle relaxing agent and other symptomatic treatment. Most macromastia occur when hormone levels change dramatically; and therefore, can be treated with hormone antagonists such as bromocriptine, progesterone, tamoxifen and danazol [7, 26]. However, although conservative treatment can control the growth of the breast, it is difficult to restore the breast to its original level [10, 24, 27]. Delayed reconstruction after bilateral mastectomy and breast reduction surgery is the most common surgical intervention, but the latter has the risk of recurrence. Simple mastectomy remains the best therapeutic alternative for gestational gigantomastia, although the exact risks of non-obstetric surgery to the fetus remains debatable [28]. In this case, when the patient suffered from her juvenile macromastia, considering she was young and unmarried, in order to improve her quality of life, breast reduction surgery was the best choice. Three years after bilateral breast reduction surgery, the gigantomastia recurrence rapidly during her pregnancy, for provisional tocolytic treatment, the bilateral breast and axillary mass gradually increased. Then, the right axillary accessory breast formed ulcerations with odor, which continued up to 36 weeks. She complained of mastalgia, back pain and breathing difficulties. Furthermore, she could not walk normally and she was unable to take care of herself. Moreover, the patient was not conducive to pregnancy, because continuing the pregnancy may aggravate the symptoms of the gigantomastia; hence, the patient underwent bilateral mastectomy at 36 weeks of pregnancy. It has been reported that if patients with gestational gigantomastia do not undergo a complete mastectomy, the risk of recurrence during pregnancy is 100% [26]. Bilateral mastectomy with reconstruction is the treatment of choice of women who desire future pregnancies [29, 30, 31].
