Abstract
PURPOSE:
Immediate autologous breast reconstruction (IABR) offers fewer surgeries with better psychosocial, quality of life and aesthetic outcomes. In high-risk patients or those with locally advanced breast cancer (LABC), adjuvant postmastectomy radiotherapy decreases local recurrence and improves survival. However, it has negative effects on the reconstructed flap. Reversing the treatment protocol using neoadjuvant radiotherapy may minimise the negative effects on the reconstructed breast in women requesting IABR. We assessed the safety and efficacy of women who underwent mastectomy and IABR post-neoadjuvant chemoradiotherapy (NACRT) for LABC.
METHODOLOGY:
A cohort study using a retrospective and prospective analysis was performed on women with LABC who underwent mastectomy and IABR post-NACRT between 1998 and 2018. All reconstructions were performed by oncoplastic breast surgeons from a single unit. Outcome measures analysed included surgical complications, flap failure, loco-regional recurrence, overall and disease-free survival. This study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). This study was approved by the institutional review board.
RESULTS:
A total of 28 women with a median age of 50 (33–64) were included. 25% underwent TRAM flap and 75% underwent LD flap reconstruction. The median period of follow-up was 61 months. Post-NACRT, 35.7% achieved complete pathological response (PCR). 3/28 (10.7%) had early complications (2 implant and 1 donor site infection). 7% underwent revision surgery. There was no flap loss. 1/28 (3.5%) had loco-regional recurrence, 3.2% had distant metastasis, and 2.5% had breast cancer related mortality.
CONCLUSION:
In women with LABC, NACRT followed by mastectomy and IABR is safe and may not compromise oncological and cosmetic outcomes. If offers the benefits of immediate breast reconstruction and avoids delaying adjuvant therapy.
Keywords
Introduction
Management of invasive breast cancer has changed dramatically over recent decades [1–7]. Although the rate of breast conserving surgery (BCS) is steadily increasing, mastectomy is still required in a large proportion of cases [2,3,8–11]. It is well acknowledged that immediate breast reconstruction offers better psychosocial and quality of life outcomes [1–7,11–16].
Post mastectomy radiotherapy is essential in women with large tumour size (T3) or have locally advanced breast cancer (LABC) with lymph node metastasis with a high risk of recurrence (Stage IIB), and in Stage III cancer [8–12]. Although radiotherapy is effective in reducing local-regional recurrence and improve overall outcomes, it is associated with several potential negative effects on cases undergoing immediate breast reconstruction. Breast reconstructions have reported to have increased rates of capsular contracture, infection, pain, impaired wound healing, and poor cosmesis post-radiotherapy. Radiotherapy on autologous reconstruction can cause skin changes, vascular compromise, fibrosis, fat necrosis, atrophy, volume loss and flap contracture. Due to the perceived risk of complications, a number of surgeons do not offer or recommend immediate breast reconstruction for women requiring post-mastectomy radiotherapy [12,15–24].
Neoadjuvant radiotherapy is utilised in several other cancer types that are radiosensitive, including rectal and oesophageal cancer [21–23]. Radiotherapy has been shown to enhance cancer-specific immune response. This can activate anti-tumour immunity and can potentially help to eradicate subclinical disease in the breast and rest of the body [7,10,23,24]. The combination of neoadjuvant chemotherapy and radiotherapy has been shown to improve the pathological response rates and the overall outcomes [25]. Recently several studies published in the literature demonstrating the safety of immediate autologous breast reconstruction after neoadjuvant chemo and radiotherapy [1,4,7–10,13–15,24–27].
The aim of this study is to determine the long-term safety and efficacy of IABR using pedicled autologous flaps in the setting of NACRT in an oncoplastic breast unit.
Methods
A cohort study was performed using a retrospective and prospective analysis on women with large tumour size and LABC who underwent mastectomy and IABR post-NACRT between 1998 and 2018. These patients underwent neoadjuvant chemotherapy and radiotherapy followed by mastectomy and immediate autologous breast reconstruction 6–8 weeks later using a flap with or without a silicone implant or tissue expander (Flow diagram).
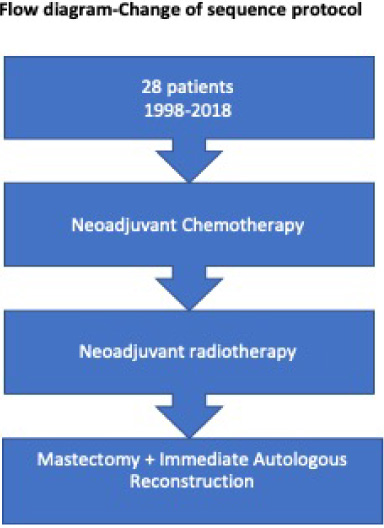
The patients had between six and eight cycles of neoadjuvant chemotherapy, based on the protocol for which there was the most evidence at the time of their treatment. Chemotherapy was administered first, followed by radiotherapy (50–60 Gray) starting two to four weeks later. All patients had their oncological management discussed at a Multidisciplinary Meeting. All reconstructions were performed by oncoplastic breast surgeons from a single unit. Breast reconstruction procedure details and post-operative complications were analysed.
Outcome measures included surgical complications, flap failure, loco-regional recurrence, overall and disease-free survival. All patients were followed up bi-annually for two years and then annually by the oncoplastic breast surgeon involved with their treatment. There was no loss to follow-up.
Results
Twenty-eight women with a median age of 50 (33–64) with locally advanced breast cancer were included in this study. Baseline characteristics of those patients are outlined in Table 1. The average age was 49.8 years with a median follow-up of 61.3 months. Majority of the patients were non-smokers (89.3%). There was no missing data.
Baseline patient characteristics
Baseline patient characteristics
Table 2 outlines the tumour variables. Significant number of patients had multifocal tumours (28%) and 68% with tumour size >50 mm.
Tumour variables
Post-NACRT, 35.7% achieved complete pathological response (PCR). 3/28 (10.7%) had early complications (2 implant and 1 donor site infection). 7% underwent revision surgery. 3.6% patients had abdominal wall hernia. There was no flap loss. 1/28 (3.5%) had loco-regional recurrence, 3.2% had distant metastasis, and 2.5% had breast cancer related mortality (Tables 2 & 3).
Operative details
Table 3 outlines the operative details and complications. 25% underwent TRAM flap and 75% underwent LD flap reconstruction. Table 4 shows the reported cosmetic outcome, with 75.1% reported excellent and 14.3% reported good overall cosmetic outcomes.
Overall reported cosmetic outcome
Patients who did not have complications considered their cosmetic outcome good or excellent.
Postmastectomy radiotherapy (PMRT) has been recommended for node-positive or locally advanced primary breast cancers. In recent years, the indications for post-mastectomy radiotherapy also include intermediate and high-risk breast cancer (i.e., high grade, vascular invasion, 1–3 positive lymph nodes) [28–30].
Although immediate autologous breast reconstruction offers significant advantages, including single surgery, reduced cost to the health sector, excellent cosmetic outcome and superior psychosocial benefits [1–3,5,12,13,18,19,24], it is well recognised that PMRT can have a negative impact on all types of breast reconstruction. For implant-based reconstructions, PMRT can result in higher rates of capsular contracture, infection, pain, impaired wound healing, and poor cosmesis. Autologous breast reconstructions also have increased complications including flap contracture and volume loss, poor cosmesis, and increased fat necrosis with PMRT [3,7,13,17,20,25–30]. Due to the perceived risk of complications, a number of surgeons do not offer or recommend immediate breast reconstruction for women requiring post-mastectomy radiotherapy [12,15–20,29–37]. Other studies have focused on a multidisciplinary team’s ability to predict the need for PMRT in cases of early breast cancer, to not recommend immediate breast reconstruction [29–32,34–37].
In recent years, authors have introduced the concept of reversing the sequence of therapies for high-risk breast cancer, delivering neoadjuvant radiotherapy to the intact breast after neoadjuvant chemotherapy followed by mastectomy [1,4,7–10,13–15,24–27]. The change of sequence has shown to have advantages for the patients and the treating team. As surgery is the last step in the treatment sequence there are no concerns with surgical complications delaying other adjuvant therapies. Immediate autogenous breast reconstruction may also be offered without concerns about irradiating the flap. Delaying the surgery after radiotherapy will also allow patients to recover from the physical and immunological effects of chemotherapy, reducing the physical demands of major surgery on such patients. A recent meta-analysis of reverse-sequence neoadjuvant chemotherapy and radiotherapy for high-risk mastectomy cases concluded that it was both feasible and safe. No intraoperative complications were reported, and for all types of IBR, the postoperative complication rates ranged from 3 to 36%. Furthermore, studies comparing outcomes between control groups of PMRT and no radiotherapy showed that NART did not result in more complications. Cosmetic outcomes were rated favourably by patients and surgeons. Locoregional recurrence rates were low, but many of the more recent, prospective studies had short follow-up times [7]. The results from our study have added to this emerging evidence that reverse sequence neoadjuvant chemotherapy and radiotherapy is safe and effective in high-risk mastectomy cases. Our unit has been offering this reverse-sequence strategy since 1998. The results with long median follow-up of 61 months for our current study are similar to those published by Gornes et al. with a median follow-up duration of 61.9 months, demonstrating a high pathological complete response rate and levels of patient satisfaction [23].
Radiotherapy is crucial and integral part of the treatment protocol in the management of LABC decreasing the rate of local recurrence and improve survival rates. In cases of mastectomy and immediate breast reconstruction, delays to radiotherapy due to surgical complications have adverse effects but the time-frames are less well- established. A meta-analysis including 21 retrospective breast cancer studies suggested an increased risk of loco-regional recurrence if radiotherapy was delayed by more than 8 weeks following surgery [36]. In LABC, the optimal timing of adjuvant radiotherapy after neoadjuvant chemotherapy, mastectomy and immediate breast reconstruction has been subject of ongoing debate [3,5–7,12–15,24,26]. It is well documented that irradiated flaps develop high rates of contracture up to 17% and loss of volume due to fibrosis and fat necrosis [5,9,13,20,26,27]. Reversing the sequence to deliver radiotherapy in a timely manner after neoadjuvant chemotherapy avoids concerns of irradiating the autologous flap reconstruction. Furthermore, Neoadjuvant radiotherapy may impact upon pathological response rates, with high response rates reported in some series (Barrou et al. (53.4%), Gornes et al. (51.3%) [4,23]). The results from our study demonstrated an overall complete pathological response of 35.7% post neoadjuvant chemotherapy (pCR), which is comparable with other published studies. The rate of pCR after neoadjuvant chemotherapy is a well-established marker of good prognosis, depending on the histological tumour subtype [10,14,15,23]. The long-term results from our study parallels those published by Gornes et al. involved the use of pedicled autologous flaps for immediate breast reconstruction [23]. According to the PRADA trial the effects of acute radiation induced vascular injury is known to be within 2–4 weeks post radiotherapy [16]. Therefore, any microsurgical reconstruction needs to be timed to minimise vascular complications. This can be challenging, especially in the already burdened health system. In this study all the autologous reconstructions were pedicle latissimus dorsi flaps were performed within 6–8 weeks post radiotherapy and the overall flap complication rate compares favourably with the wide range of published studies [1–3,5,14,15,24–26]. In our study there was no flap loss, low rate of revision surgery (7%) and hernia (3.6%) supports the feasibility and safety of reversing the sequence in the treatment protocol. The oncologic and cosmetic outcomes were also comparable with other published studies [1–3,5,14,15,24–26]. Patient and surgeon both independently assessed the cosmetic outcome as poor, satisfactory, good and excellent. Overall, 89.4% reported either good or excellent cosmetic outcome (Table 4). IABR with pedicle flap can also minimise complications in patients who smoke and have microvascular disease secondary to chronic systemic illness such as diabetes mellitus.
Although the reversal of sequence is a safe and feasible option, it requires a close working relationship between the members of the multidisciplinary team. As surgery is the last treatment modality in this sequence, patients can prepare emotionally and physically for their surgery. This study demonstrates the experience of an oncoplastic breast surgery unit and raises the awareness of change in sequence as a safe and effective option in LABC. Although having no comparative group is a limitation of this study reversing the treatment sequence is a relatively new concept and further prospective studies with larger sample size will add more vital information to this technique.
Conclusion
Reversing the treatment sequence to include neoadjuvant chemotherapy and radiotherapy allows oncoplastic breast surgeons to offer immediate autologous pedicle flap reconstruction to women with LABC. This study shows that the outcome and complications rates are comparable with reversal of sequence with a most satisfactory oncological and cosmetic outcome.
Footnotes
6.
The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was approved by the hospital ethics committee.
Declaration of interest
None
