Abstract
BACKGROUND:
The exact immunopathological mechanisms in the progression of breast cancer are not clearly understood, but various factors including CD8 T lymphocytes have lethal properties on tumor cells. On the other hand, interleukin-37 (IL-37), as a new member of the IL-1 family, is an anti-inflammatory cytokine. The exact role of IL-37 in breast cancer has not yet been determined.
OBJECTIVE:
This study aimed to evaluate the CD8 T lymphocytes count and IL-37 gene expression in newly diagnosed breast cancer patients with and without metastasis.
METHODS:
In this study, blood samples from 36 metastatic and 36 non-metastatic breast cancer patients and 36 healthy individuals as control were collected. After RNA extraction and cDNA synthesis, the relative gene expression was performed using real-time PCR. Also, counting the CD8 T lymphocytes was done by flow cytometry technique.
RESULTS:
The results of this study showed that the gene expression of IL-37 in blood samples of metastatic and non-metastatic breast cancer patients was significantly lower than in healthy individuals (P < 0.05). The relative gene expression of the IL-37 in ER+/PR+/HER2+ patients with non-metastatic breast cancer had a significant increase compared to HER2+ patients (P < 0.05). Also, CD8 T lymphocytes count in the samples of patients including non-metastatic and metastatic breast cancer was significantly decreased compared to the healthy individuals (P < 0.05).
CONCLUSIONS:
Our findings provide evidence that IL-37 gene expression and CD8 T lymphocytes count, significantly decreased in non-metastatic and metastatic breast cancer. Considering the possible effects of IL-37 on TCD8 cells in tumor immune responses, more research will be done to benefit from the therapeutic effects of this cytokine in the future.
Introduction
Breast cancer was classified as the most common cancer among women with more than two million cases diagnosed over the world [1]. Breast cancer sub-classification is based on the expression of different molecules including human epidermal growth factor receptor 2 (HER2), estrogen receptor (ER), and progesterone receptor (PR). Accordingly, breast cancer without the above-mentioned receptors is called triple-negative breast cancer (TNBC) that is the most aggressive form and indicates a poor prognosis. The pathological stage of breast cancer is classified as TNM (T: the size of the tumor, N: lymph node metastasis, M: metastasis to distant areas). Metastasis occurs when tumor cells acquire aggressive properties and the ability to escape anti-tumor immunity.
Deficiencies in anti-tumor immunity may facilitate the occurrence of breast cancer. However, the exact immunopathological mechanisms in the progression of breast cancer are not clearly understood. The results of many studies show that the modulation of innate and acquired immune parameters is important for the onset and progression of breast cancer [2,3]. In this respect, there are different types of T lymphocytes including regulatory T cell, helper T cell, and cytotoxic T cell. Among these, cytotoxic T lymphocyte (TCD8) shows more antitumor activity, and an increase in the number of TCD8 in breast cancer patients is associated with greater survival in the patients [4]; however, the role of TCD8 in breast cancer with metastasis is unclear.
On the other hand, cytokines can cause the prevention or development of different cancers [5]. In this way, interleukin-37 (IL-37), as a new member of the IL-1 family, is an anti-inflammatory cytokine and plays a role in many inflammatory and autoimmune diseases and functions as an extracellular and intracellular cytokine [6–8]. The extracellular form of IL-37 binds to IL-18Rα and IL-1R8 molecules and regulates STAT3 and PTEN signaling molecules [9]. On the other hand, the intracellular form of IL-37 can bind to Smad3 and regulate downstream target gene expression after transfer to the nucleus [10]. Recently, the role of IL-37 in tumors has been investigated and it has been found that IL-37 plays anti-tumor roles in tumors such as non-small cell lung cancer, liver cell carcinoma, and kidney cells. The mechanism of action of IL-37 on tumor growth is mainly through the regulation of immune responses, inhibition of cancer cell growth, and tumor angiogenesis [11]. IL-37 shows its antitumor effect by altering the microenvironment of the tumor including TCD8 and natural killer (NK) cells. In this way, IL-37 can stimulate the CD57+ NK cells and can mediate the anti-tumor effects of cytokines including IL-12 and IL-18 that are helpful for the function of NK cells. Also, IL-37 increases the expression of costimulatory molecules such as CD40, CD86, and MHC-II on dendritic cells and secrete cytokines such as IL-2, IL-12, IFN-α, and IFN-γ that increases the function of TCD8 [12]. On the other hand, some studies have shown that IL-37 inhibits the maturation of DCs in atherosclerosis via the IL-1R8-TLR4-NF-κB pathway [13]. The function of IL-37 can depend on its concentration and receptor expression. For example, at high concentrations, it forms a dimer and is inactivated [14]. Considering the effects of IL-37 on increasing the function of TCD8+, measuring this cytokine along with counting the number of TCD8+ lymphocytes can identify their relationship in breast cancer, especially, in association with metastasis, and introduce a new path for future therapeutic approaches.
Materials and methods
Patients
This case-control study was conducted from April 2019 to June 2020 among 72 women with newly diagnosed breast cancer aged 30–55 years who have been referred to the health examination clinics in Khansari Hospital in Arak, Iran. The patients were categorized into two groups including 36 patients without metastasis and 36 cases of invasive ductal carcinoma (metastasis). Patients were diagnosed based on clinical examination, pathological stages, and ER+/PR+/HER2+ receptors. The selected patients including metastatic and non-metastatic breast cancer underwent no immunosuppressive, immunomodulatory, or chemotherapy agents at least three months before the sampling. Patients with infectious and autoimmune diseases were excluded from this study. Also, 36 age-and sex-matched healthy individuals participated in this study (Table 1). Healthy volunteers were selected based on the absence of any disease, especially breast cancer, and taking any medicine. The written informed consent was taken from all participants and the experimental protocol for blood collection was approved by the Ethics Committee of Arak University of Medical Sciences [No: IR.ARAKMU.REC.1398.113].
Clinicopathological characteristic of patients in metastatic and non-metastatic breast cancer
Clinicopathological characteristic of patients in metastatic and non-metastatic breast cancer
ER, estrogen receptor; HER2, human epidermal growth factor 2 receptor; PR, progesterone receptor. SD, standard deviation, *Normal breast cell that is usually slow-growing. **Looks less like normal cells and is growing faster. ***Looks different from normal breast cells and is usually fast-growing.
At first, three ml of the blood sample was collected from all participants in EDTA anti-coagulation tubes. Total cellular RNA was extracted and purified according to the kit instructions (Favorgen Biotech Corp., Taiwan). Extracted RNA was evaluated using Nanodrop (Plat reader epoch 2). Its quality was also confirmed with 2% agarose gel. Finally, cDNA synthesis was performed based on the kit protocol (Yekta Tajhiz Azma, Iran).
IL-37 gene expression assay
Forward and reverse primers of IL-37 (target gene) and GAPDH (housekeeping gene) were designed using AlleleID 6.0 (Premier Biosoft Intl., USA) and their specificity was checked by primer-blast (Table 2). Gene expression assay was performed by SYBR Green qPCR Master Mix (Yekta Tajhiz Azma, Iran) and all reactions were performed in triplicates on a LightCycler system (Roche, Germany). The melting curve assay for excluding the primer-dimer and non-specific bands was performed. The Pfaffle method was used to analyze the reaction data and then the expression pattern was examined by statistical analysis.
Flow cytometry analysis of CD8 T lymphocytes
Flow cytometry assay for CD8 T lymphocytes counting was performed based on manufacture protocol (BD Biosciences, Bedford, MA). Briefly, 50 μl of the blood samples were stained using surface antibodies including peridinin chlorophyll protein (PerCP)-conjugated anti-CD8 and fluorescein isothiocyanate (FITC)-conjugated anti-CD3. After erythrocytes lysing by BD FACS Lysing Solution, the cells were fixed using BD CellFix Solution. Appropriate PerCP- and FITC-conjugated antibodies were included for isotype controls. All antibodies and solutions were obtained from BD Biosciences. The stained cells were analyzed using FACS Calibur Flow Cytometer (BD Biosciences, San Jose, CA) by counting 10,000 cells and analyzed using the Flowjo software (Treestar, Ashland, OR).
Designed primer sequences of IL-37 and housekeeping genes
Designed primer sequences of IL-37 and housekeeping genes
IL, Interleukin; F, Forward; R, Reverse
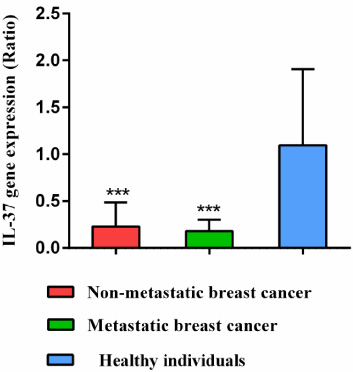
Comparison of the interleukin 37 gene expression in non-metastatic and metastatic breast cancer patients compared to healthy individuals. *; P < 0.05, **; P < 0.01, ***; P < 0.001.
The normal distribution of data was assessed by the Kolmogorov–Smirnov normality test. One way ANOVA test was used to compare means between the different groups. Significant levels were considered less than 0.05. Statistical tests were performed in SPSS version 16.0 (SPSS, Inc., Chicago, IL, USA). Graph Pad Prism software (version 6.0) was used for graph drawing.
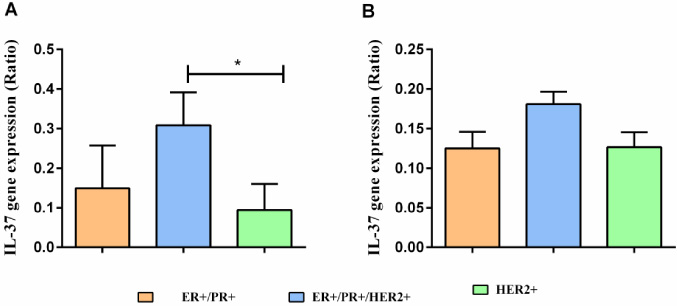
Comparison of IL-37 gene expression in ER+/PR+/HER2+ subgroups of breast cancer. (A) Non-metastatic and (B) metastatic breast cancer. *; P < 0.05, **; P < 0.01, ***; P < 0.001.
IL-37 gene expression
Results have shown that the gene expression of IL-37 reduced significantly in newly diagnosed patients with metastatic and non-metastatic breast cancer compared to healthy individuals (P < 0.001). There was no significant difference between metastatic and non-metastatic breast cancer patients (Fig. 1). Also, the results showed that the relative gene expression of the IL-37 in the ER+/PR+/HER2+ patients with non-metastatic breast cancer had a significant increase compared to HER2+ patients (P < 0.05) (Fig. 2A and B).
CD8 T lymphocytes
The results of flow cytometry (Fig. 3) showed that the number of CD8 T lymphocytes in the blood samples of patients including non-metastatic and metastatic breast cancer was significantly decreased compared to the healthy individuals (P < 0.05) (Fig. 4).
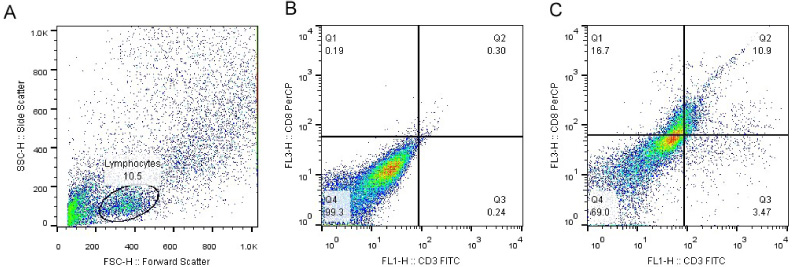
Flow cytometry analysis of CD8 T lymphocytes. (A) Blood leukocytes distribution based on side and forward scatter. (B) CD8 T lymphocytes without anti-CD3 and anti-CD8 staining. (C) CD8 T lymphocytes with anti-CD3 and anti-CD8 staining.
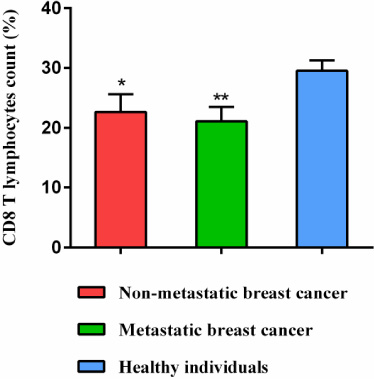
Counting the CD8 T lymphocytes in non-metastatic and metastatic breast cancer compared to healthy individuals. *; P < 0.05, **; P < 0.01, ***; P < 0.001.
The results of the present studies are in agreement with the other clinical studies in which showed that the expression of the IL-37 gene was significantly decreased in patients with a different type of cancer. On the other hand, statistical analysis of the relationship between the expression of IL-37 gene and metastasis showed that the expression of this gene in breast cancer with or without metastasis was not significantly different. Also, the results showed that the number of CD8 T lymphocytes in the samples of patients including non-metastatic and metastatic breast cancer was significantly decreased compared to the healthy individuals [15–17].
In this respect, studies by Cavalli et al. confirmed that IL-37 gene expression was significantly decreased in patients with kidney cancer. This decrease is associated with disease progression because IL-37 acts as an immune suppressor in advanced kidney cancer using the IL-6/STAT3 signaling pathway [18]. In 2003, Gao and colleagues reported that fibrosarcoma growth was suppressed by injecting IL-37 into mice [17]. Zhao et al. reported in 2014 that IL-37 expression levels were negatively correlated with tumor size in hepatocellular carcinoma (HCC) [19]. Wang et al. showed that IL-37 can suppress cell proliferation and metastasis in HCC through the STAT3 pathway [20].
The previous studies showed that IL-37 acts as a tumor suppressor in lung cancer and exerts its antitumor action by inhibiting angiogenesis that can be used as a promising therapeutic target for lung cancer [21]. Previous research has shown that there is a negative correlation between IL-37 expression and angiogenesis in different cancers; however, the exact mechanisms are not depicted [21,22]. Chen and colleagues found that IL-37 stimulates apoptosis and inhibits the migration and proliferation of cancer cells [23]. On the other hand, in vivo experiments showed that IL-37 suppresses tumor growth as well as the expression of the IL-6 and hypoxia-inducible factor 1-alpha (HIF-1α) genes [23].
In addition to studies on IL-37 in humans, numerous studies have shown that the effects of IL-37 in mice are comparable to those on humans. The results confirmed that IL-37 caused significant inhibition of tumor growth in the RCC (renal cell carcinoma) mouse model [23]. Recently, IL-37 has been shown to play an important role in mouse models not only in the innate immune response but in the acquired immunity [24].
In our study, IL-37 gene expression was evaluated in different breast sub-classes of breast cancer. As a result, IL-37 was increased in the ER+/PR+/HER2+ patients with non-metastatic breast cancer compared to HER2+ patients. Baker et al. in 2019 has sown that HER2 expression in breast cancer patients is directly related to inflammatory cytokines such as IL-1 and IL-6 [25]. Previous studies have shown that ER/HER2 and HER2 breast cancer show different metastatic patterns, in which patients with HER2 breast cancer that more likely to metastases to bone and show lower survival and may need more aggressive treatment [26]. So, an increase of IL-37 may prevent metastasis in breast cancer that should be elucidated in the future.
In our study, the results showed that the number of TCD8 in the samples of patients including non-metastatic and metastatic breast cancer was significantly decreased compared to the healthy individuals. As a result, the presentation of antigen to lymphocytes is decreased, and eventually, cytokines such as IL-2, IL-12, IFN-α, and IFN-γ that affect the killing of tumor cells are reduced; however, decreased number of TCD8 in the peripheral blood may show the recruitment of these cells into the tumor site.
In tumor tissues, expression of IL-37 was positively correlated with density of CD57 NK cell. In vitro studies showed that IL-37 was able to attract CD57 NK cells and delays tumor growth [19]. Also, IL-37 cytokine can mediate the effects of IL-12 and IL-18, which perform their antitumor function through the expression of perforin and FAS-L, respectively [12].
According to previous research, IL-37 promotes NK cell activity and anti-tumor cytokines like IL-12 and IL-18. All of the above results suggest that IL-37 cytokine may be a potential activator for cytotoxic T cells in breast cancer; however, identification of the molecular mechanisms of IL-37 on cytotoxic T lymphocytes still need further studies.
In summary, our results suggest that cytokines can promote cell proliferation and invasion through signaling pathways, contribute to cancer metastasis, or prevent cancer progression. The present study showed that IL-37 gene expression and TCD8 count decreased in the new breast cancer patients. Since IL-37 increases the maturation of dendritic cells and induces the secretion of cytokines to increase the antitumor effect, there may be a direct link between IL-37 expression and the count of CD8 T lymphocytes that mediate antitumor responses. Considering the possible effects of IL-37 on TCD8 cells in tumor immune responses, although there are no sufficient studies in this regard, more research will be done to benefit from the therapeutic effects of this cytokine in the future.
Footnotes
Acknowledgments
We appreciate all those who support and assist in carrying out this study, especially people who made it possible to complete the study by giving a sample. This study is related to the results of the first person thesis.
Conflicts of interest
None.
Author contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Najmeh Farahani, Fathollah Mohaghegh, and Ali Ganji. The first draft of the manuscript was written by Najmeh Farahani and Ghasem Mosayebi and Ali Ghazavi commented on previous versions of the manuscript. All authors read and approved the final manuscript.
