Abstract
People with a mental illness are two and a half times more likely to die from all main causes of death when compared to the general population [1,2]. Despite the high risk of obesity [3,4], cardiovascular disease [5,6], and type 2 diabetes [7,8], the screening of psychiatric patients for physical health disorders is woefully inadequate [2,9]. There is continued disagreement amongst mental health clinicians as to who should take responsibility for the screening and treatment of medical comorbidities, and the situation is further complicated by the relatively high proportion of psychiatric patients who do not have regular contact with a general practitioner. This journal has published a number of important papers highlighting these and related issues [10–14].
The authors' interest in these issues arose from involvement in the Healthright Project in Western Australia, which had been initiated as a result of the ‘Duty to care’ and ‘Who is your GP?’ reports [2,9]. In a survey of Australian psychiatrists we found that even by self-report, comprehensive screening for obesity, hypertension and metabolic abnormalities was not occurring in many services despite a general acknowledgement of its importance [Laugharne JDE, Waterreus AJ, Castle D: unpublished data]. The incidence of obesity and metabolic syndrome in the mentally ill is known to be two to three times higher than in the general population [10,11]. Therefore, to assist clinicians in screening for the metabolic syndrome we developed a clinical algorithm [15]. To build upon the metabolic syndrome algorithm, a comprehensive literature review was carried out with the aim of identifying key dimensions and components associated with the excessive risk of physical illness for mental health patients. The areas of medication, lifestyle, pre-existing or developing physical disorders, alcohol and illicit drug use, and psychosocial factors consistently emerged (Figure 1). From this review, the Clinical guidelines for the physical care of mental health consumers assessment and monitoring package was developed in consultation with mental health clinicians, primary care physicians, and patients. The guidelines incorporate recommended investigations for screening and ongoing monitoring in order to facilitate the improved physical health of all patients with mental health disorders (see http://www.psychiatry.uwa.edu.au/research/community-culture/physical-care-clinical-guidelines) [16].
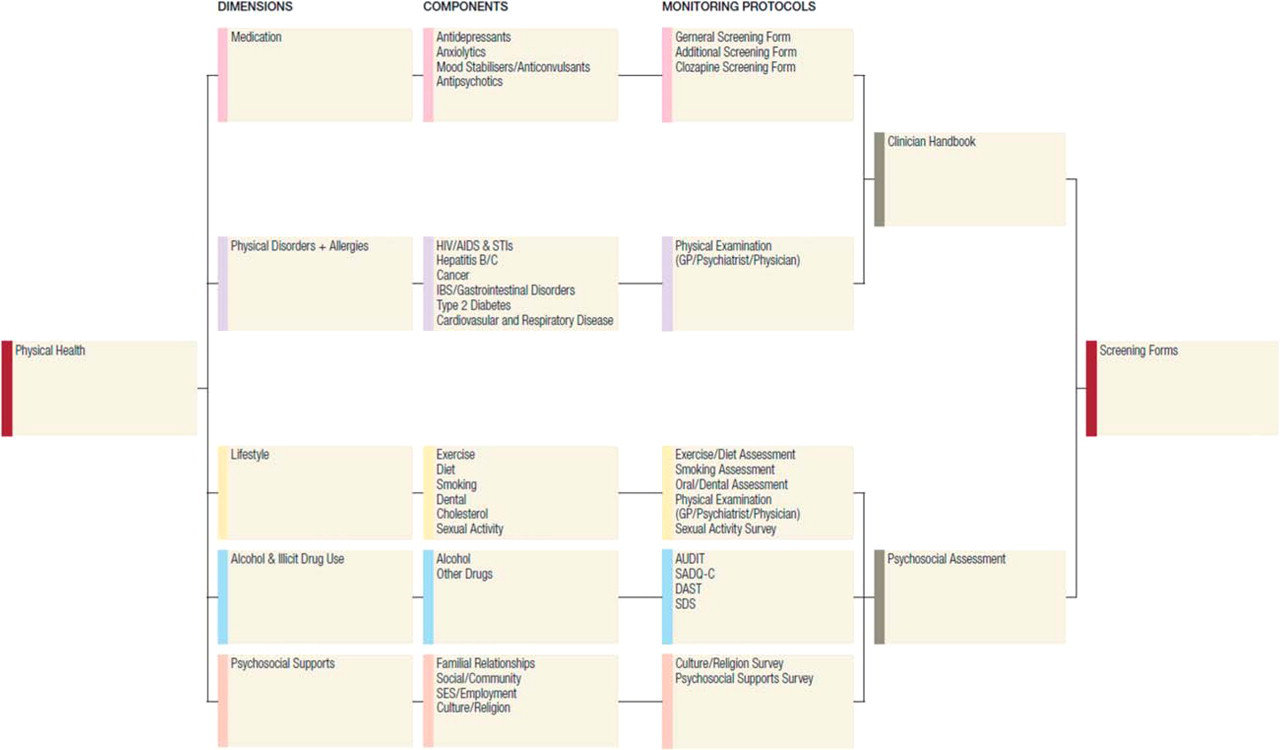
Dimensions of physical health for mental health patients
Adequate screening of the five key areas of physical health requires specific tools of investigation. These tools were either sourced or, when suitable resources could not be found, developed by the authors.
Components of the package
There are six components to the screening package: the clinical algorithm, the Clinician handbook, the Psychosocial assessment booklet, the screening forms, a Consumer diary, and a Carer handbook. Each is colour-coded in a consistent manner to increase ease of use.
Clinical algorithm
A clinical algorithm wall chart for monitoring metabolic syndrome in mental health patients has been included in the package, giving indices and monitoring recommendations for waist circumference, blood pressure, fasting lipids, and fasting blood glucose [15,16]. This represents the essential physical health screening that must be conducted when assessing metabolic syndrome, with the wall chart acting as a reminder to both clinicians and their patients of the required tests to be conducted. The authors recommend regular screening for metabolic syndrome in all individuals on psychotropic drugs as many agents, in addition to antipsychotic drugs, are associated with obesity and metabolic abnormalities.
Clinician handbook
Designed for psychiatrists and general practitioners, the Clinician handbook provides evidence-based information specifically dealing with medications and physical investigation, along with an overview of the other three major health dimensions to be monitored [16]. The first section of the handbook focuses on the adverse effects of psychotropic medications. Each major category of medication is covered (antidepressants, anxiolytics, antipsychotics, and mood stabilizers) along with other key agents (carbamazepine, lithium carbonate, valproic acid, and clozapine) requiring specific tests. Recommended testing for each medication category is outlined, along with common, infrequent, and rare adverse effects [17,18]. In addition, a list of normative ranges for each test is provided for quick reference.
Further into the handbook, information and normative levels for other identified components of physical health such as cholesterol, body mass index (BMI), abdominal girth, and possible drug interactions between psychotropic and dental drugs are provided. This information aids the clinician in gaining an overall perspective of their patient's physical health.
There is a section on common medical comorbidities of which all clinicians treating patients with psychiatric illnesses should be mindful. As the physical health monitoring of people with a mental illness has been shown to often be inadequate [9], it is recommended that a full physical examination at baseline of all people prescribed psychotropic drugs be undertaken, and procedures put in place to ensure the regular screening of associated physical disorders.
Information on alcohol and illicit drug use in Australia, and the possible health complications resulting from drug use and abuse provides the clinician with an up-to-date reference, and suggested screening tests are highlighted. Psychosocial aspects of physical health are also covered, such as culture, values and belief systems, and the importance of language in consultation. Designed for use by psychiatrists and general practitioners, the Clinician handbook represents an easily accessible knowledge source, and is designed to aid collaborative investigation and monitoring of patient physical health.
Psychosocial assessment booklet
The Psychosocial assessment booklet can be used by a psychiatrist, a general practitioner, a mental health nurse or psychiatric case worker, and includes tools for assessing the dimensions of lifestyle factors, alcohol and illicit drug use, and psychosocial factors. The surveys within the booklet can be completed by individuals with or without assistance from health staff.
Lifestyle surveys in the booklet assess physical activity levels, weight and BMI, abdominal girth, and nutrition/diet. These surveys highlight low levels of exercise and increased body weight, particularly central adiposity, associated with type 2 diabetes, hypertension, cardiovascular disease, and dyslipidaemia. Dental treatment is also explored as the oral health of psychiatric patients generally tends to be poor. The high levels of tobacco smoking found in people with a mental illness necessitates the inclusion of the smoking survey [13,14]. This survey assesses levels of nicotine use and dependence, and identifies the individual's interest and confidence in cessation. The sexual activity survey investigates sexual behaviour, sexual difficulties that may be occurring due to medication side-effects, contraception, and HIV and sexually transmitted infections (STIs).
As alcohol and illicit drug use are often comorbid with mental illness, particularly psychotic disorders, screening is necessary to ameliorate possible physical complications and potential drug interactions. The Alcohol Use Disorders Identification Test (AUDIT) [19] identifies possible drinking-related problems, and the Severity of Alcohol Dependence Questionnaire Form-C (SADQ-C) [20] establishes the severity of alcohol dependence. Both have been found to be reliable with psychiatric populations [21]. Illicit drug use is associated with high morbidity and mortality, and can be assessed through the Drug Abuse Screening Test (DAST) [22]. The DAST identifies possible drug abuse, including prescribed or over-the-counter drugs used in excess of the directions and any non-medical use of drugs. Drug dependence is assessed through the Severity of Dependence Scales (SDS) [23], and measures the degree of dependence upon a variety of drugs such as heroin, cocaine, amphetamines and cannabis.
The cultural/religious/spirituality component has been placed at the front of the booklet to aid the assessor to first develop rapport and gain understanding of the patient's point of view. Based upon the theory of cultural safety, this survey attempts to provide a safe environment for people where there is no assault, challenge or denial of identity or needs [24]. Cultural safety encourages the process of collaboration (shared respect, meaning, knowledge, and experience) where people can learn together with dignity, and listen to each other.
Social relationships have been shown to influence both mental and physical health outcomes, with strong social relationships decreasing an individual's risk of mortality [25]. The psychosocial supports assessment has been placed at the end of the booklet evaluating the types and timing of support that may be lacking in the individual's life. In times of crisis, emotional supports are needed where empathy and care allows the expression of emotion and feelings. In times of transition, cognitive supports are needed such as knowledge and information and the development of coping skills to assist with decision-making and personal direction. In times of deficiency, material supports are needed such as rent assistance or hostel accommodation affording a person shelter. Social supports encourage positive change. These surveys can be completed by the patient or with an assessor.
Screening forms
To document informative, individualized assessment, the general screening form allows each patient's results for all assessment components to be noted. The form spans a 24 month time period, starting from an initial baseline measurement, and gives an overall view of the person's physical health to reveal any changes that may be occurring over time. A second screening form has also been provided which outlines additional tests required for specific medications such as lithium carbonate, valproic acid, carbamazepine, antipsychotics and mood stabilizers. A third and separate screening form has been provided for clozapine, due to the additional mandatory investigations associated with this drug [26].
The general screening form can be placed in the front of the patient's medical file, allowing clinicians immediate access to any changes or potential problems that may be developing.
Consumer diary and Carer handbook
Complementing the clinician package, a Consumer diary has been developed to enable mental health patients to work in partnership with their physicians and support staff. The diary is an A5 two-ring file with removable pages containing information and health tips on all five dimensions of physical health, and has tables for patients to record their medical and test results. The diary is designed to be retained over the long term, where pages can be added once a table becomes full. The individual has a choice as to whether they share this information with their carer/s or not. If they choose not to share their medical information, a separate information handbook can be provided for their carer/s.
The Carer handbook will have all of the same information and health tips as the Consumer diary, but will not include the results tables. The language in this handbook will be directed towards carers, with the aim of assisting them in caring for people with a mental illness, and just as importantly, taking care of their own physical health.
Conclusion
The physical health of mental health patients is relatively poor [2,10,11], and both national and international research promote improved screening [1,2,12]. Poor physical health is due to a multitude of factors such as psychotropic medication effects, lifestyle, existing or developing physical disorders, alcohol and illicit drug use, and psychosocial factors. The need, therefore, to improve the general health screening of patients who have a mental illness at both a primary care level and a specialist mental health service level is evident.
The Clinical guidelines for the physical care of mental health consumers assessment and monitoring package provides a unique, practical, evidence-based resource which can be adapted and integrated into a variety of clinical settings. The overarching aim of the package is not to simply identify issues but to aid clinicians in providing workable solutions. The assessment protocols included in the package take a biopsychosocial approach to physical health assessment, and can be used and/or adapted for inpatient, outpatient, or community services. In this regard, coordination of services involving mental health clinicians, general practitioners and physicians at the local level is crucial [12].
The guidelines will need to be regularly updated as new research emerges. Developed for adults, further investigation is required for distinct subdivisions such as older adults, and for children. There is also a need to evaluate the utility of the clinical guidelines in a variety of contexts including inpatient, outpatient community and rural settings. The authors are currently involved in instigating such a multi-service evaluation.
The holistic approach of these clinical guidelines facilitates early identification of those at risk of physical illness, enabling preventive interventions when risk factors are identified, and earlier diagnoses. It is to be hoped that the clinical guidelines reported here will help services address more effectively the disparity in physical health outcomes between the mentally ill and the general population.
Note
Hard copies of the package can be ordered from UniPrint at the University of Western Australia [16]. Electronic copies can be downloaded free of charge.
