Abstract
The vast majority of people experiencing mental illness live and receive treatment in the community, increasing the possibility that they will have some contact with the police [1]. A survey of police officers in Sydney, Australia, found that on average police reported spending approximately 10% of their time dealing with mentally ill people, with three-quarters saying that they had dealt with a mentally ill person in the past month [2]. A more recent study of Victorian police found that they perceived that approximately one-fifth of potential offenders encountered appeared to have a mental illness [Godfredson JW, Thomas SDM, Luebbers S & Ogloff JRP: unpublished data, 2009]. This is broadly consistent with data from overseas [3].
In order for police to resolve an encounter with a person or group of people, they may need to use some kind of force in order to manage the situation. National guidelines for police use of force have emphasized that this should be only the minimum force necessary to perform their duties, and that the use of lethal force should be considered only in situations where it is unavoidable in order to protect life [4–6]. Some research has suggested, however, that perhaps due to the lack of police training on how to deal with mentally ill persons, police may approach dealing with them as though they are encountering a dangerous criminal, thereby leading to use of more severe force, which occasionally results in injury to either party or even death [7,8].
Most studies of lethal use of police force come from the USA. However, there is a scarcity of studies examining mental illness in incidents of police use of fatal force. The potential involvement of mental illness has been most commonly examined in research on ‘suicide-bycop’, also termed ‘law-enforcement-assisted-suicide’, which has been reported to account for between 10% and 46% of police shootings, depending on how specifically the phenomenon is defined [9–12]. Of note, one review estimated that people experiencing mental illness are almost fourfold more likely to be fatally wounded by police than those without mental illness [13]. However, differences in population characteristics, laws and regulations that both govern the society, police conduct, and police culture, however, are important considerations when attempting to relate American findings to other jurisdictions. Moreover, differences in defining and measuring the prevalence of mental disorder in fatal encounters poses additional barriers to valid and reliable interpretations of extant findings.
Between 1990 and 2004 there were 76 police shooting deaths in Australia, more than one-third of which occurred in Victoria [14], despite having only one-quarter of the population [15]. The commonality of police shootings in Victoria has caused considerable debate [16,17], with some commenting on the overrepresentation of mental illness among those shot [14,18,19]. These events were a significant contributor to Project Beacon being established in September 1994 with a ‘safety first philosophy’, which judged the success of police encounters with citizens according to the extent to which force was avoided or minimized [14]. Subsequent changes reflecting this philosophy were introduced to policy and practice of Victoria Police [14,18]. Recent reviews, however, into Victoria Police use of force concluded that police training did not emphasize verbal negotiation skills and tactics aimed at avoiding confrontation [14,20].
Because of the lack of systematic research examining this issue, the aim of the present study was to explore incidents of fatal use of force in Victoria with respect to mental health and offending histories of the individuals involved. Based on recent review reports [14,18,19] it was hypothesized that (i) the majority of the deceased would be known in some capacity to the criminal justice system and/or the mental health system; and (ii) there would be disproportionately high rates of mental illness among those fatally shot as compared to the general population.
Method
Databases
The study of fatalities resulting from fatal police force involved data linkage between three databases: (i) the Use of Force (UoF) Register; (ii) the Law Enforcement Assistance Program (LEAP); and (ii) the Client Interface Management/Operational Data Store (CMI/ODS) database, uniformly known as the Victorian Psychiatric Case Register (VPCR).
The UoF register came into operation in October 1995 as a result of Project Beacon [14]. It contains details of all incidents in which force has been used on or by the police. The LEAP database, in operation since 1993, records all contacts between police and the public as witnesses of crimes, victims of crimes, alleged offenders and offenders. Prior to 1993 contact data were stored on Information Bureau of Records (IBR) cards in more limited form. Therefore to gain a full police contact history, IBR records were linked to contacts recorded in LEAP and to the UoF records.
The CMI/ODS, in operation since 2000, is a compendium of all contacts with the public mental health system. Prior to this, contact data were recorded on the VPCR in more limited form. The CMI/ODS records clients’ contacts with public outpatient, community and inpatient services, but not contacts with private hospitals, private practitioners, or general practitioners for mental health issues [21]. Although information on major mental illness such as psychosis is well recorded on the database, information about more high-prevalence disorders such as mood disorders and personality disorders are not as complete [22], and substance use disorders are primarily addressed in specialist services outside the public system.
Data linkage and ethical considerations
The data on identifying information of fatally wounded individuals between 1 January 1980 and 21 February 2007 were sourced from the UoF database. The timeframe was selected on the basis of the available information, whereby the Victoria Police have recorded this information only starting in January of 1980, with the first fatality recorded in November of 1982, and at the time of data collection the last fatality occurred in February of 2007. The Victoria police have retrospectively recorded fatalities between 1980 and 1994 in a more limited form. Identifiers (full name, gender and date of birth) were extracted and subsequently linked with the LEAP to gather contacts with the criminal justice system, and with the VPCR to collate all contacts with public mental health services. Once linked and verified, all names were permanently removed. The project was approved by ethics committees of Monash University, Victoria Police and Department of Human Services.
For the purposes of this analysis criminal history was defined as being charged or convicted of any crime, with offences classified as violent or non-violent using the Cormier–Lang System [23]. Mental health diagnoses obtained from the VPCR and information from the coronial reports were coded as either present on Axis I or Axis II of the DSM-IV-TR. Disorders were categorized as substance use disorders, mood disorders, anxiety disorders, psychotic spectrum disorders (including schizophrenia), and schizophrenia specifically. Community estimates of Axis I disorders were obtained from a recent study that used the same methodology [24].
To address the natural limitations of using historical data, collected for purposes other than research, coronial reports were sourced from the Victorian Coroner's Office, Monash University Library and the Public Records Office of Victoria. Additional relevant details available in an Office of Police Integrity Report were also considered [14]. For consistency, all coronial reports were reviewed to verify the presence and extent of criminal and mental health histories. This was particularly noteworthy when contact with services had been reported from other jurisdictions because this would not routinely be recorded on the VPCR. Additional mental health diagnostic information, including known contacts in other States and countries, were obtained from coronial reports in 10 cases, and from the Office of Police Integrity Report in two cases. Additional criminal data were obtained from coronial reports in eight cases.
Data analyses
Basic descriptives were used to characterize the sample. Continuous data were compared with independent t-tests while categorical data was cross-tabulated and χ2 tests of association calculated, considering Fisher's exact test statistic when cell values fell below n = 5. All analyses were two-tailed. Odds ratios (ORs) and relative risk (RR) were calculated, and 95% confidence intervals (CIs) were calculated using Miettinen's method [25]. Data were analysed using SPSS version 16.0 (SPSS, Chicago, IL, USA) and Stata version 10.0 (StataCorp, College Station, TX, USA).
Results
General characteristics
Forty-eight people were fatally shot by Victoria Police between November 1982 and February 2007; 45 (93.8%) were male, and three (6.2%) were female. The average number of fatalities per year over the 24 year span was two, although there were a number of years when no-one was shot, and others when there was a spike in fatalities (six fatalities in 1988 and eight in 1994). Exactly two-thirds (32, 66.7%) were shot in the 12 years prior to Project Beacon, and one-third (16, 33.3%) in the 12 years following. The average age of the sample at time of death was 32.3 years (SD = 9.03, range = 19.1–50.5 years); male decedents were significantly younger than female decedents (31.5 years, SD = 8.71 vs 43.6 years, SD = 6.29, p = 0.028).
Contact with the Criminal Justice System
The vast majority of subjects had a recorded offending history (39, 82.2%). On average, their first offence was committed at the age of 24.3 years (SD = 9.4, range = 12–50.4 years). The number of offences committed varied widely, ranging from only one offence, up to some 270 (mean = 25.6, median = 10, SD = 52.98). More than half (26, 54.2%) had a history of both violent and non-violent offences, and 10 (20.8%) were recorded as perpetrators of family violence incidents. Nearly one-quarter (11, 23%) had also been recorded as having been victims of crime. Of these, six had been victims on multiple occasions.
Contact with the Mental Health System
Twenty subjects (41.7%) had contacts recorded on the VPCR. Of note, when additional data sources were consulted, more than half of the sample (26, 54.2%) were recorded as having an Axis I disorder, of whom most (16, 61.5%) had one Axis I diagnosis recorded.
The average age of the subjects at first contact was 29.9 years (SD = 7.66, range = 20.7–40.1 years). In four cases, three involving a diagnosis of schizophrenia comorbid with substance abuse/dependence and one with a delusional disorder, the fatality occurred within 9 days of the subject's last contact with the mental health services. In a further two cases, one involving a diagnosis of hypomania and one of schizophrenia comorbid with substance abuse/dependence, the fatality occurred within 1 month of the subject's last contact with services.
As given in Table 1, more than one-third (19, 39.6%) had substance abuse/dependence disorder, a rate more than 23-fold higher than that estimated in the general community (RR = 23.9, 95%CI = 16.9–33.9). Psychosis was diagnosed in eight cases (16.7%), with most of these (6, 12.5%) being a diagnosis of schizophrenia. The rates of psychosis and schizophrenia were 11.3- and 17.3-fold, respectively, higher than estimated rates in the general population (95%CI = 6.3–20.2 and 9.2–32.4, respectively). Mood and anxiety disorders were also significantly overrepresented (Table 1).
Comparative estimates of Axis I disorders between the fatalities sample and the general population
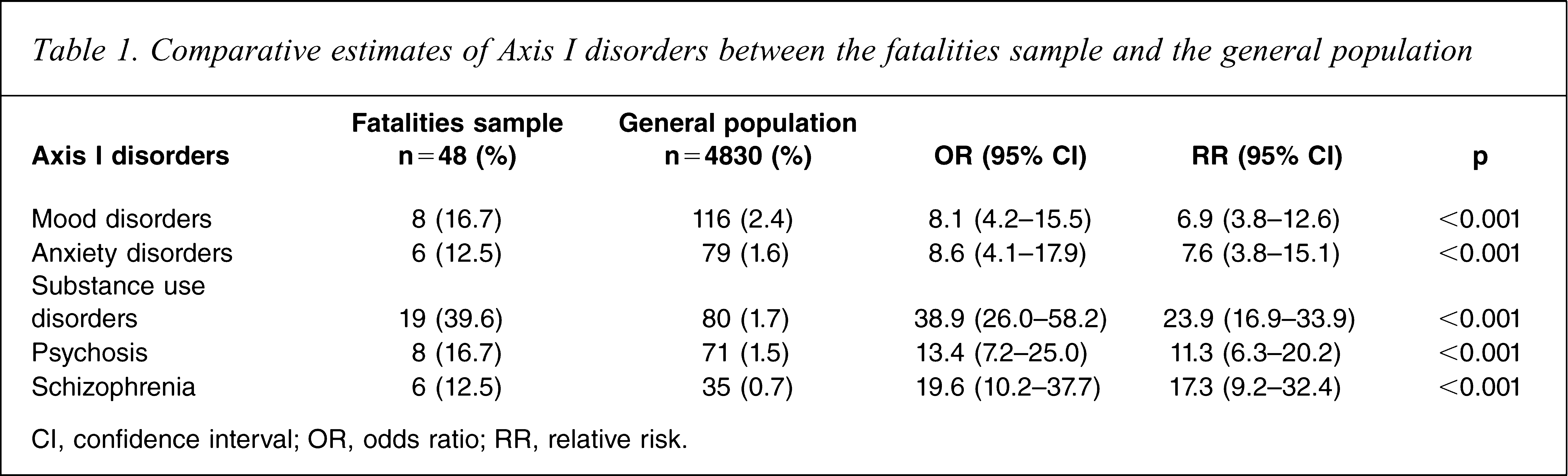
CI, confidence interval; OR, odds ratio; RR, relative risk.
Excluding substance use disorders, one-third of the group (16, 33%) had been diagnosed with a mental illness. Five of the subjects (10.4%) had an Axis II personality disorder diagnosis recorded. These consisted of antisocial (2, 4.2%), dependent (2, 4.2%), paranoid (1, 2.1%) and other (3, 6.3%) personality disorders; with two subjects (2, 4.2%) having more than one personality disorder diagnosis.
The vast majority of subjects (42, 87.5%) were known in some capacity to either mental health services or the police. Additionally, four of the six persons not formally recorded on either system were known to the police and considered suspects in many crimes. The sample came into contact with the criminal justice system at a significantly younger age than their first recorded contact with the public mental health system (t = 2.30, p = 0.025). Furthermore, the majority of those who had an Axis I disorder (21, 80.1%) had also been charged with criminal offences.
Pre- and post-Beacon analysis
In the 12 years prior to Project Beacon, under half of the sample (13, 40.6%) had an Axis I diagnosis; in the 12 years following, this rate rose to 81.3% (13). Although the presence of Axis I disorder was 6.3-fold more likely in the post-Beacon era, and this difference was statistically significant (Fisher's exact test = 0.013), rates of all Axis I disorders were not significantly different between the two time periods. Similarly, there were no significant differences in the presence of criminal histories before and after the Beacon initiative (24, 75% vs 15, 94.8%, Fisher's exact test = 0.24).
Discussion
This study described a full cohort of fatalities resulting from encounters between Victoria Police and civilians between November 1982 and February 2007, exploring the frequency at which the individuals had previously had contact with, and were known to, the mental health and criminal justice systems.
Before discussing the study findings it is important to consider several limitations that may impact on the generalizability of the findings reported here. The main limitation relates to the data linkage method used. Mental health and offending information recorded in the databases was not collected for the purposes of research, hence was naturally limited in scope and depth. More specifically, the VPCR underreports the incidence of high-prevalence disorders [21,26]. Furthermore, the LEAP and the VPCR have differing time-frames of inception and operation, and the extent and the quality of the data needed for the study varied according to these. To try to counter these limitations an examination of relevant coronial reports was conducted. Indeed, the majority of the missing data obtained from the coronial reports was in line with the limitations outlined above (e.g. data not routinely recorded by the databases, data in existence before the databases came into operation, and data from other jurisdictions).
Characteristics of the fatalities
Overall, there have been 48 deaths resulting from police use of force between November 1982 and February 2007, with 32 deaths occurring before 1995, and 16 since 1995. While the majority involved male subjects, the female victims were significantly older at the time the fatality occurred. Gender and age characteristics of this Victorian sample were comparable to a sample of related fatalities over a 4 year period in New York City [27].
Contacts with the Criminal Justice and Mental Health Systems
The vast majority of the decedents had an offending history or were informally known to the police as suspects in crimes, and a substantial proportion had contacts with mental health services. Of note, the sample had been known to the police at a significantly younger age than becoming known to mental health services. It is likely that their presentation to the police may have initiated contact with mental health services, but this hypothesis cannot be tested with these historical data. These findings are in line with the recent research findings of commonality in contacts between police and mentally ill persons [2,4] and that, in their role to protect the safety and welfare of the public and their parens patriae role of protecting citizens with disabilities [28], police are necessarily the first point of contact for many persons experiencing mental illness and emotional distress; hence the reason why police have been regarded as ‘street corner psychiatrists’ [29] and ‘frontline mental health workers’ [30].
Overrepresentation of mental illness
The findings reported here indicate a high prevalence of Axis I disorders among people fatally shot by the police. More importantly, not all of those who had an Axis I disorder had a formal contact with the mental health services. Additionally, half of those suffering from comorbid psychotic and substance use disorders were fatally wounded <2 weeks since their last contact with mental health services. In all but one of these cases the contacts were directly between the patient and the mental health service, and in one case between the police and an emergency psychiatric service regarding the patient's management. Thus, this specific subgroup represent a high-needs group of people whose contact with both the mental health services and the police leads to significant implications for their management in the community.
The rates of severe mental illness, such as psychosis and schizophrenia, were significantly overrepresented in the current sample. The estimated rates reported here are considered reliable because the overwhelming majority of all persons with a psychotic disorder would have at some point accessed the public mental health system [24]. The same premise is not true for the high-prevalence disorders, such as anxiety and mood disorders, so we can assume that the figures officially recorded for the present study, perhaps referred to as a ‘treated prevalence’ in the public mental health system, are a significant underestimate of the true prevalence of these disorders [26]. Broadly speaking, these findings are consistent with the literature indicating that rates of mental illness are overrepresented in offending populations [31,32], and the commonality of severe mental illness presentations among mental health referrals by police [33–35]. They also support previous Victorian investigations suggesting the overrepresentation of mental illness in police fatal shootings [13,14,18].
Success of Project Beacon
The main aim of Project Beacon was to reduce the number of fatal shootings by the Victoria Police by reforming policy and practice of the force. Despite the successful reduction in overall numbers of people fatally wounded, there has been no associated reduction in the number of mentally ill persons shot by the police. Perhaps this indicates that there is a unique aspect to the incidents involving mentally ill persons that the initiatives of Project Beacon and subsequent changes to Victoria Police training and practice have not adequately been able to address [14]. A more in-depth analysis of shootings before and after Project Beacon in the context of changes introduced by the initiative and other legislative changes would be required in order to examine this.
Implications of the current findings and future directions
These findings clearly have very significant practical implications for both the police and the mental health services. These tragedies both victimize the group of people who are already very disadvantaged in terms of their mental illness and criminal lifestyles, as well as the police officers involved [7,36]. The finding that the vast majority had contacts with both mental health and criminal justice services is indicative of a population with complex presentations and needs. The significant overlap in contact between the two services also raises questions about which system, and in what capacity, is best placed to provide interventions that could improve the opportunities and outcomes of this disadvantaged group in our community.
While other contemporary research by some of the authors suggests that police can discern major signs and symptoms of certain mental disorders [Godfredson JW, Ogloff JRP, Thomas SDM & Luebbers S: unpublished data, 2009], the identification of a person with an anxiety or mood disorder may well be more problematic. This then becomes an issue of both knowing more about the person with whom the police are interacting and also knowing how to de-escalate and resolve situations in which persons are emotionally distressed; this reaches beyond simply knowing how to identify the major signs and symptoms of major mental illnesses.
In light of this, interagency cooperation becomes an immensely important practical factor, therefore the forming of a functional partnership between the police and the mental health services becomes critical [14]. Such initiatives have been successfully developed and trialled, based on the well publicized ‘Memphis model’ approach, where police receive specialist training on dealing with mentally ill persons and those in emotional crisis and are further supported via partnerships with mental health services [37–39]. To enable the practicalities associated with information sharing, legislative amendments will undoubtedly be required [39], which necessarily limit the confidentiality inherent in disclosing personal information without an individual's express consent. Although there are undoubtedly significant ethical and legal challenges posed by considering a shared data system with differential levels of access [40], such issues should ideally be addressed in a manner that does not override the core need to better equip police to manage people in emotional distress and to help facilitate better outcomes for people experiencing mental illness. Although there are other initiatives used internationally, these models clearly do not offer a one-size-fits-all solution; partnerships need to be developed according to local systems, services and capabilities in a climate that is conducive to potentially significant legislative and policy change.
Conclusions
The current study provided initial findings regarding the mental health and offending characteristics of the persons who were fatally shot by the Victoria Police between 1982 and 2007. The estimated rates of all major mental illnesses were overrepresented in the sample of fatalities. Although the number of police shootings has halved since the inception of Project Beacon, the proportion of those with mental illness has in fact increased. Further research should include an in-depth investigation of the contextual factors surrounding the incidents to help elicit specific contributing factors and inform training. Learning from situations in which other types of engagement and force have been used may additionally increase our understanding, and ultimately promote more practical developments, such as scenario-based training, information sharing and specialized training for police in dealing with people in emotional distress.
Footnotes
Acknowledgements
This study was supported by a grant from the Australian Research Council; a collaboration between Monash University, Victorian Institute of Forensic Mental Health and Victoria Police. The research team consisted of James Ogloff, Stuart Thomas, Paul Mullen, Trish Martin, Jonathan Clough, Christine Tye, Ashley Dickinson and Ken Lay. We also acknowledge the project managers Stefan Luebbers and Lisa Warren, and the input of Leanne Sargent, David Bradley and David Ballek at Victoria Police.
