Abstract
Introduction
The frequently used irrigant in dental surgery, sodium hypochlorite, is occasionally the cause of minor, usually circumscribed, adverse effects. Severe, extensive complications, with lasting sequelae, however, also can occur, as in the case we report herein.
Case Report
A 55-year-old woman underwent an endodontic procedure on a maxillary molar, whose roots, unknown to the surgeon, were protruding into the maxillary sinus. After sodium hypochlorite root canal irrigation, the patient immediately developed intense facial pain, facial edema, and periorbital cellulitis. An emergency department evaluation diagnosed an intense inflammatory disease of the maxillary sinus, with significant destruction of its bony walls, accompanied by midface paraesthesia due to infraorbital nerve injury. In the following weeks, the patient slowly developed enophthalmos due to bone erosion of the orbit floor. Treatment, besides prolonged oral steroids, required the endoscopic endonasal opening of the maxillary sinus for profuse irrigation. Two years later, the patient maintained a complete loss of function of the maxillary sinus, anesthesia-paraesthesia of the midface, and inferior dystonia of the eye with an enophthalmos.
Conclusion
Dentists, maxillofacial surgeons, and otorhinolaryngologists should all be aware of the whole spectrum of complications of even the simplest dental work. Sodium hypochlorite irrigations should be used cautiously in root canal surgery, with the full awareness of its potential for causing soft-tissue damage.
However, their use is not without risks. 7 It has been reported that, in case of inadvertent contact of sodium hypochlorite with periapical organic tissues, the symptoms may range from immediate severe pain, with local edema, profuse bleeding, hematoma, ecchymosis, ulceration, tissue necrosis, and risk of secondary infection, to facial nerve weakness and reversible anesthesia-paraesthesia.1–5,8–10 Potentially more severe can be the consequences of the contact with respiratory mucosa, as with the case of an injection of sodium hypochlorite directly into a normally functioning maxillary sinus.
Case Report
A 55-year-old woman, during an endodontic treatment for caries of a maxillary left molar, was injected with an undisclosed dosage and concentration of sodium hypochlorite into her tooth roots. Unknown to the dental surgeon, the molar roots protruded into the maxillary antrum floor, so that, after opening of the apical portion of the root canal or a root canal perforation, the injection of sodium hypochlorite had an effect similar to being administered directly into a closed cavity, the maxillary sinus, lined with delicate respiratory mucosa. Immediately after the injection, the patient experienced a sudden, sharp intense pain in the left maxillary region, associated with a rapidly developing swelling and anesthesia-paraesthesia of the left hemiface, and ipsilateral periorbital cellulitis (Fig. 1). At the emergency department of a large tertiary care hospital, she was diagnosed with acute, “chemically induced,” maxillary inflammatory disease; computed tomography of the sinus showed a thickened mucosa in the left antrum floor, which occurred simultaneously with severe inflammation of the homolateral ethmoid sinus in the areas that correspond to the drainage pathway of the maxillary sinus (Fig. 2). Also evident was a piecemeal destruction of the antral bony walls, mostly in the posterolateral and superior walls. Periorbital cellulitis was also present, with densification of the intraorbital fat and thickening of the inferior rectus muscle and the medial rectus muscle (Fig. 2).

Emergency department computed tomography, showing marked left facial edema with slight proptosis caused by the periorbital cellulitis.
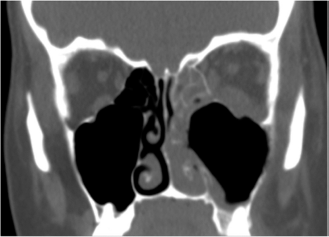
Emergency department computed tomography, showing a thickened inflamed mucosa in the left maxillary sinus floor in the vicinity of the protruding tooth roots, with total opacification of the homolateral anterior ethmoid sinus and of the remaining nasal cavity. Evidence of destruction of the antral bony walls, including of the orbital floor, is seen. Periorbital cellulitis with densification of the intraorbital fat and thickening of the inferior rectus muscle and medial rectus muscle is shown.
After admission, medical treatment included prophylactic broad-spectrum antibiotics (intravenous ceftriaxone, 2 g/day, with oral clindamycin 300 mg every 6 hours, for 10 days), high-dosage steroids (methylprednisolone 1 mg/kg/day), pain control therapy (with nonsteroidal anti-inflammatory drugs), and abundant and frequent saline solution nasal irrigations. Because her clinical status was still not showing any improvement after 48 hours, she underwent endoscopic endonasal sinus surgery while she was under general anesthesia (Supplemental Movie 1) to remove obliterating anterior ethmoid inflammation and create a large middle meatal antrostomy, which allowed effective sinus irrigation with flushing and cleansing of chemical residues and tissue debris. Clear signs were then seen that the antral mucosa was experiencing an intense inflammatory process, “like a massive chemical burn,” with various areas of destruction of its bony walls, including a dehiscence of the infraorbital nerve on the orbit floor (Fig. 3).

Endoscopic evidence, during surgery, of the intense acute inflammation of the antral mucosa. *The dehiscent infraorbital nerve on the orbital floor.
She was discharged 1 week after surgery, and a prolonged convalescence period followed, during which the patient, over months, slowly tapered oral steroids as initial facial pain was painstakingly subsiding, replaced by a constant facial discomfort and numbness. She, simultaneously, slowly developed enophthalmos as a consequence of the destruction of the bony wall of the floor of the orbit. The evaluation after two years of follow-up revealed that, despite no evident external facial edema, a significant hemifacial anesthesia-paraesthesia due to the infraorbital nerve injury still persisted, with inferior dystonia of the left eye and enophthalmos (Hertel exophthalmometer: right eye, 15 mm; left eye, 12 mm) but without diplopia. Nasal endoscopy showed that, despite a free left ethmoid cavity with a patent middle meatal antrostomy, the maxillary antrum was filled with irreversibly damaged nonfunctioning scar tissue. Meanwhile, the patient started a lawsuit process against the dental surgeon on malpractice charges, including the accusation of lack of sufficient preoperative information for the dental procedure undertaken.
Discussion
The rationale for the use of chemical irrigants, such as sodium hypochlorite and hydrogen peroxide, in root canal surgery rests on their disinfecting and tissue dissolving properties, including their alleged potential to interact with calcium in teeth to promote the opening of dentinal tubules.1,4–6 The tissue cytotoxic effects of sodium hypochlorite largely result from its alkalinity (pH 10.8–12.9) and hypertonicity, which lead to local cellular destruction, primarily by oxidation of proteins.1,4
A variety of sodium hypochlorite solutions are available, which range from 0.5 to 5.25%, with no consensual optimal concentration for clinical use.1,3–5 A concentration-dependent efficacy was eventually shown, with higher concentrations displaying higher antiseptic and dissolution activities.4–6 Besides concentration, other factors also seem to be relevant, such as the gauge size of the irrigation needle, how deep into the root canal the tip of the needle is placed, the administered volume and temperature of the solution, and the duration of exposure, which relates to the irrigation time and the frequency and/or repetition of the irrigations.1,3–6
When endodontic irrigants remain confined to the canal space, their use is safe, but when their application is misdirected and they inadvertently reach or are applied to any vital tissue, local necrosis and other complications are expected.1–6,8 There are approximately two dozen cases of sodium hypochlorite accidents reported in the literature, which correspond to the more-severe cases because smaller complications will likely tend to go unreported.1–5,8–10 Most cases deal with the consequences of sodium hypochlorite accidently reaching the periapical area.1,2,4,8
The case we present illustrated the more serious consequences that result from contact of sodium hypochlorite with the respiratory mucosa and bony walls of a normally functioning maxillary sinus as a complication of a dental procedure during which the dental surgeon, probably after a root canal perforation or an open apex, went ahead with a sodium hypochlorite irrigation unaware that the molar roots were deeply protruding into the maxillary sinus. The final effect was equivalent to a direct injection of an undisclosed amount and concentration of sodium hypochlorite into a closed-space sinus cavity, with immediate damage of the respiratory mucosa lining and erosion of large portions of the underlying bony walls, which thus facilitated the further expansion of its tissue toxicity into surrounding structures, such as the midface teguments and the orbit. Along the way, it caused the irreversible lesion of the infraorbital nerve, a not totally unexpected event because sodium hypochlorite shows a high efficacy in destroying nerve remnants when used in root canal surgery. 6 Enophthalmos was a later occurrence, when the erosion of a significant part of the orbit floor caused a slight depression of the orbit contents into the maxillary sinus. Two years later, the full consequences of the event are still striking. When comparing with other cases in the literature, very few seem this dramatic.1,4,5,9,10
To explain why sodium hypochlorite may inadvertently extrude beyond the root canal into vital tissues, investigators have come up with the following most common reasons, any of which may have occurred in our case: (1) iatrogenic tooth apex opening (consequence of incorrect assessment of canal length or accidental widening of the apical foramen), (2) accidental lateral canal perforation, and (3) inappropriate irrigation technique (extreme pressure applied, irrigation needle going too deep into the root canal, and/or blockage of the backflow of the irrigant in the canal space).1,4,5
Conclusion
Dentists, maxillofacial specialists, and otolaryngologists should all be aware of the whole range of maxillofacial complications that may arise from even the simplest dental procedures. The dentists have a critical role in preventing them, but all have the responsibility to rapidly and correctly diagnose the extent of such complications when they happen and treat them adequately. These complications are usually minor, but, on occasion, as this case illustrates, important adverse effects occur and significant lifelong sequelae may persist.
Footnotes
The authors have no conflicts of interest to declare pertaining to this article
