Abstract
Obstruction of the lacrimal pathway is manifested by epiphora, infection, and blurred vision as well as ocular and facial pain. Conservative treatments only achieve temporary relief of symptoms, thus surgery is the treatment of choice. Dacryocystorhinostomy (DCR) is recognized as the most suitable treatment for patients with obstructions of the lacrimal system at the level of the sac or in the nasolacrimal duct. The aim of this operation is to create a bypass between the lacrimal sac and the nasal cavity. During the past 2 decades, advances in rigid endoscopic equipment and other instruments have made it possible to obtain more information about the anatomic landmarks of the nasolacrimal system, which led to the development of less-invasive and safer endoscopic techniques. However, many parts of the treatment process related to endoscopic endonasal dacryocystorhinostomy (EN-DCR) still remain controversial. This article reviews the published literature about the technical issues associated with the success of EN-DCR, and clarifies the pros and cons of different pre- and postoperative procedures in adults with lower lacrimal pathway obstructions.
During the past 2 decades, endoscopic DCR (EN-DCR) has become accepted as a suitable treatment for patients with obstructions of the lacrimal system at the level of the sac (saccal obstruction) or below it (postsaccal obstruction).4,5 Although there exists a consensus concerning some technical details in EN-DCR, many aspects of the treatment process still remain controversial. One reason for this uncertainty is the lack of prospective studies related to this operation. There is a definite need for well-conducted studies that evaluate optimal preoperative assessments and for improvements in the surgical protocols, particularly in revision operations and the use of outcome predictors, timing of follow-up, and tools for the subjective assessment after EN-DCR. The purpose of this article was to review the published literature about the technical issues associated with the success of EN-DCR and to clarify the implication of examinations in adults with lower lacrimal pathway obstructions.
Anatomy
The system that secretes and drains tears into the nasal cavity consists of the lacrimal gland in conjunction with the upper and the lower lacrimal pathways (Fig. 1). The upper lacrimal pathway is made up of the puncta and lacrimal canaliculi, whereas the lower lacrimal pathway contains the lacrimal sac and nasolacrimal duct.

Anatomy of the nasolacrimal system: 1, lacrimal gland; 2, punctal openings; 3, inferior canaliculus; 4, superior canaliculus; 5, common canaliculus; 6, lacrimal sac; 7, nasolacrimal duct; 8, uncinate process; 9, middle turbinate; 10, inferior turbinate.
Incidence of Nasolacrimal Pathway Obstructions
The study by Woog, 1 which examined the epidemiology of lacrimal obstruction, demonstrated that the most common form of acquired symptomatic lacrimal obstruction is nasolacrimal duct obstruction (NLDO), which occurs with an annual frequency of 0.02%. The same study also confirmed that acquired lacrimal pathway obstruction was most common in middle-aged individuals, with a median age of 67 years. Moreover, 69% of patients with all forms of obstructions and 73% with NLDO were female.
Obstruction of the Lower Lacrimal System
Primary acquired nasolacrimal duct obstruction (PANDO) accounts for approximately two-thirds of the patients with stenosis. The etiology and the pathogenesis of PANDO are unclear, but it is known that gradual inflammation and subsequent fibrosis of the nasolacrimal duct are factors that predispose to obstruction of the drainage system. 6 PANDO occurs more frequently in postmenopausal women. 1 The narrowness of the bony nasolacrimal canal and the increased angle between the bony canal and the nasal floor in females can cause tear-fluid stasis and infections to spread from the nasal cavity, and can predispose to chronic inflammation of the nasolacrimal drainage system.7–9 Furthermore, individual structural features such as the drain lines from the frontal and ethmoidal sinuses, the anatomically narrow and high infundibulum and septal deviation may play an important role in the inflammatory processes that occur in the nasolacrimal duct. 10
Secondary acquired nasolacrimal duct obstruction (SANDO) in adults may result from a wide variety of specific infections (Actinomyces, Herpes zoster, Adenovirus, Aspergillus); chronic immunologic diseases (sarcoidosis, cicatrical pemphigoid, Stevens-Johnson syndrome); or neoplastic, traumatic, or mechanical causes (e.g., dacryoliths and external compression of the paranasal sinus mucoceles). 11 SANDO may also occur as a result of nasoethmoidal, nasal, or midfacial fractures, or due to repair of other midfacial injuries. 12 Sinus and rhinoplastic surgery carries a potential risk of damaging the nasolacrimal system.13,14
The close anatomic relationship of the lacrimal sac, nasolacrimal duct, and paranasal sinuses may represent a major predisposing factor for the obstruction of the nasolacrimal pathway. Acute infections in the nasal cavity or recurrent and chronic infections of the paranasal sinuses can readily spread through the nasolacrimal duct, followed by mucosa inflammation before scar formation and final stenosis. 10
Evaluation of Obstruction of the Nasolacrimal Pathway
Ophthalmologists and otorhinolaryngologists, particularly those specializing in performing EN-DCR, are the primary consultants for patients with disorders of the lacrimal duct. The goal of the basic examination is to determine the reason of epiphora or lacrimation. Epiphora may be a result of a disorder of tear drainage, e.g., caused by mechanical obstruction, lid malposition, or lacrimal pump failure. Excessive tearing may also be caused by reflex hypersecretion. The reasons for hypersecretion may be dry eye syndrome, allergy, infections, tumors, hormonal changes, foreign bodies, and many neuronal stimuli.
The Schirmer tear test provides information about the tear secretion. 15 Tear break-up time determined by biomicroscopy evaluates the stability of the tear film. Diagnostic probing and syringing of the lacrimal pathway are usually sufficient to evaluate the function of the lacrimal drainage system or to determine the location and extent of the obstruction in patients with epiphora. If the nasolacrimal pathway is open, then the solution flows freely into the nose. In cases of canalicular stenosis, the cannula cannot contact the bony wall of the lacrimal sac, and this results in reflux through the irrigated punctum. If the stenosis is in the common canaliculis or in the lower lacrimal pathway, then reflux will occur via the opposite punctum (Fig. 2).
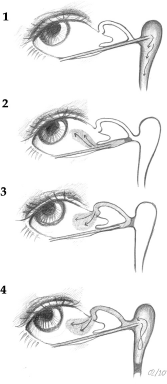
Location of obstruction by irrigating the lower lacrimal system: 1, no obstruction; 2, presaccal obstruction (stenosis of the inferior canaliculus); 3, presaccal obstruction (stenosis of the common canaliculus); 4, saccal or postsaccal obstruction (stenosis in the lower lacrimal pathway)
External and Endoscopic DCR
DCR may be conducted by performing either external-DCR (EXT-DCR) or its endoscopic version, EN-DCR. EXT-DCR has been considered the “gold standard.” However, because recent studies revealed the efficacy and safety of EN-DCR in identifying postsaccal obstruction of the nasolacrimal pathway, this technique has become increasingly popular. Overall, outcomes after EN-DCR and EXT-DCR are comparable, with good results maintained over time. 16
EN-DCR as a Treatment for Saccal and Postsaccal Obstructions
EN-DCR is a minimally invasive procedure with the improved endoscopic instrumentations currently available. The endonasal approaches can be divided into endonasal laser-assisted DCR, powered instrumentation endonasal DCR, and “cold steel” DCR with or without drills. 17
Indications
EN-DCR is indicated in the management of epiphora and infection related to PANDO and SANDO when the obstruction site is located in the lacrimal sac (saccal obstruction) or in the nasolacrimal duct (postsaccal obstruction). In addition, EN-DCR may be beneficial in children with congenital dacryostenosis with nasolacrimal duct cyst formation. 18 Single and short-term infections are common and may be treated conservatively. However, when the condition is recurrent or persists for more than 6–12 months and is not resolved by irrigation of the nasolacrimal duct, then EN-DCR treatment may be considered.
Preoperative Imaging of the Nasolacrimal Pathway
There are many different techniques being used, but there does not seem to be any reliable scientific reports that evaluated the superiority of one technique over the others. The indications for surgery primarily depend on the symptoms experienced by the patient, not on the imaging findings. However, imaging may be considered important because it can exclude infrequent causes of nasolacrimal obstruction, e.g., tumors. The most commonly used imaging techniques are computed tomography, dacryocystography, radionuclide dacryoscintigraphy, and magnetic resonance imaging and dynamic magnetic resonance dacryocystography.19,20
Contraindications of EN-DCR
Obstructions in the upper (presaccal) part of the nasolacrimal system such as punctal and canalicular stenosis are contraindications to the use of EN-DCR. 5
Key Points in the Success of EN-DCR
A review of the literature reveals a success rate of 70–99% for EN-DCR. 16 In the literature, the following points have been recognized as being important in minimizing the possibility of failure.
Anesthesia and Preparation of the Nose
EN-DCR can be performed with the patient under general or local anesthesia with intravenous sedation. Irrespective of the type of anesthesia, vasoconstriction of the nasal mucosa and an anterior ethmoidal and sphenopalatinal nerve block by using cocaine or a solution of lidocaine with adrenaline should always be meticulously carried out. 21
Localization of the Lacrimal Sac
Should the anatomic landmarks of the lateral nasal wall have been altered or do not exist, it may be very difficult to pinpoint the lacrimal sac. 22 Christensen 23 introduced the idea of transillumination to help in visualizing the location of the lacrimal sac in DCR by using an endoilluminator probe introduced through the canaliculis into the lacrimal sac. Today, endoillumination is a widely used method for locating the lacrimal sac with different endoscopic techniques.24,25 Many investigators claim that the axilla of the middle turbinate is a landmark for the roof of the lacrimal sac.22,26 However, Wormald et al., 27 in an anatomic study with 47 patients, showed that the major part of the lacrimal sac (10 mm) is situated above the axilla of the middle turbinate and that it extends 1–2 mm below this landmark (Fig. 3).

Localization of the lacrimal sac: 1, roof of the lacrimal sac; 2, axilla of the middle turbinate; 3, superior turbinate; 4, nasolacrimal duct; 5, uncinate process; 6, middle turbinate; 7, inferior turbinate
Mucosal Incision and Flaps
Tsirbas and Wormald 28 recommend making a cut in the mucosa above the insertion of the middle turbinate in the lateral nasal wall and anterior to the axilla, and vertically down the frontal process of the maxilla. To avoid trauma of the neighboring tissue, the rectangular incisions of the nasal mucosa should be made by using a scalpel blade and the nasal mucosal flap must include the periosteum. 10
The main goal in EN-DCR is to create a large bony ostium to completely expose the medial wall of the lacrimal sac and to achieve a contact between the lacrimal sac and the nasal mucosa. In the earliest studies, this was achieved by suturing. 29 Subsequently, Eloy et al., 5 proposed stapling with titanium clips. More recently, a novel approach was described in which the lacrimal sac is fully exposed and marsupialized into the lateral nasal wall of the nose with nasal and lacrimal mucosa apposition.28,30
Location of the Osteotomy
Welham and Wulc 29 propose the removal of all the bone between the medial wall of the lacrimal sac and axilla to achieve an ideal ostium. Many investigators have recommended developing a larger ostium by removing the frontal process of the maxilla that involves the anterior lacrimal crest and superiorly above the attachment of the middle turbinate to remove bone covering the fundus of the lacrimal sac.4,17,28
Size of Rhinostoma
Some investigators consider the ostium size as being nonsignificant 31 and suggest creating a small ostium that consists of only the inferior portion of the lacrimal bone.32,33 However, a small bony ostium has been proposed as being one of the most important causes of the failure of DCR surgery.27,29,34,35 Metson 36 recommended the enlargement of the rhinostoma to a diameter of 10 mm to allow free passage of a lacrimal probe into the nasal cavity through both canaliculi. To prevent the development of lacrimal sump syndrome, some investigators have proposed performing “terminal” or “inferior” EN-DCR, in which a relatively small ostium is created by marsupialization of only the inferior portion of the lacrimal sac and the adjacent duct into the nose.37,38 However, the available scientific data do not indicate that any one option is clearly superior to the others with respect to ostium size and location. 39
Additional Surgery
When needed, the additional surgery, such as septoplasty, partial resection of anterior middle turbinate, uncinectomy, or functional endoscopic sinus surgery, may favor success, because intranasal abnormalities are common causes of DCR failure.40–43 The need for additional nasal surgery has been reported to be significantly higher in the revision cases than in primary procedures.44,45 It seems that the repair of nasal pathologic findings during the second surgical procedure and thus the prevention of the recurrence of pathology may have accounted for the good success of the revision cases. However, despite the indisputable benefits of the additional surgery in a well-selected patient population, avoiding unnecessary trauma to neighboring tissue is recommended.28,46 Furthermore, the additional nasal surgery at the same time as EN-DCR has also been shown to increase the risk of EN-DCR failure.40,46
Stenting
It is difficult to evaluate the impact of silicon tubes after EN-DCR because there is considerable inconsistency in the published reports. There are studies that detected favorable effects of silicone tubing, e.g., the prevention of the scarring of the rhinostomy site, which led to more successful EN-DCR.47–49 However, some other studies reported that the omission of silicone tubes did not increase the risk of scarring.50,51 Although the use of silicone tubing after EN-DCR has been widely recommended, until recently, no randomized controlled studies had been carried out to evaluate the effects of silicone tubes. Based on the findings of these recent randomized controlled studies, and most meta-analyses, the insertion of silicone tubes cannot be routinely recommended after primary EN-DCR.52–55 In some selected cases, e.g., in patients with narrow canaliculi, silicone stents may be used. In these cases, the stent should be left in place for at least 11–12 weeks. 39
Nasal Packing
To achieve hemostasis and prevent scar formation, various materials, such as dissolvable foam, topical hemostatic sealants, and nonresorbable packs, have been placed in the middle meatus after endoscopic nasal surgery.56–58 However, once again, no controlled studies have been performed that demonstrate the superiority of a particular technique or the effect of these procedures on scar formation. Furthermore, no long-term follow-up data are available.
Postoperative Care
It is indisputable that postoperative care has a major influence on the healing process and plays an important part in the success or failure of EN-DCR.59,60 Postoperative care options include the administration of systemic antibiotics 61 or a combination of antibiotic-steroid eye drops, local irrigation of the rhinostomy site with a saline solution nasal spray, intranasal steroids, and debridement of the intranasal wound.36,59,62
Follow-up and Timing of the Postoperative Visits
The guidelines of the Royal College of Ophthalmologists indicate that the follow-up time should be at least 3 months. The outcome of EN-DCR may decline in long-term follow-up.63–66 In a prospective study, the patients underwent three follow-up visits: at 1 week, and at 2 and 6 months after the operation. The results of this study indicated that scar formation was a slow process, and, thus, a long-term follow-up even beyond 6 months after EN-DCR may be necessary to detect some late complications. 67 However, for most patients, long-term follow-up visits beyond 1 year after EN-DCR may be considered as unnecessary. A practical and cost-effective solution for the patients and the health care system could be the use of a questionnaire.66,68 After completing the symptom questionnaire at home, only symptomatic patients could be invited for an additional visit. 66
Complications
The intraoperative complication rate in DCRs is 1%, and none of the adverse effects resulted in long-term disability, e.g., vision impairment. The overall complication rate after DCRs is reported to be ~6%. 16 Although it appears that EN-DCR is associated with a higher risk for postoperative complications compared with the external technique, this may be attributed to the fact that nasoendoscopy is routinely conducted in the patients who have undergone endonasal surgery. Thus, some minor complications such as granulation tissue formation and synechiae may be detected.
Early complications include intraoperative or postoperative hemorrhage, silicone tubing prolapse, punctal erosion related to silicone tubing, canalicular obstruction, orbital fat herniation, orbital and subcutaneous emphysema, conjunctival fistula formation, retrobulbar hematoma, and temporary ophthalmoplegia. 16 In addition, there are some rare reports of cerebrospinal fluid leaks and meningitis after DCR.69–71
Most of the late complications seem to occur between 1 and 3 months after surgery. 72 The following late complications after EN-DCR have been identified in the literature: scar formation of the rhinostoma40,52,53,73,74; synechiae between the rhinostoma and middle turbinate, between rhinostoma and the nasal septum, and between the septum and the middle turbinate; and granuloma formation within the ostium.50,75
Risk Factors for Failure in EN-DCR
Chronic inflammation76–78 and a history of sinusitis have been shown to increase the risk of failure. 40 However, there is found a higher success rate in patients with a history of dacryocystitis than in those without this kind of history. 1 The presence of a postoperative infection is also known to threaten the normal healing process and surgical outcome of EN-DCR.79,80
Because EN-DCR is a relatively infrequently performed operation with a clear learning curve, the experience of the surgeon plays an important role in the success rate.63,81,82 It was found that, during a mean follow-up time of 4 years, the surgical success was 94% in experienced hands but only 58% in inexperienced hands. 63
The cause of failure can also be linked to the biology of wound healing in the nasal mucosa.83,84 Recently, Smirnov et al., 77 evaluated the factors related to wound healing and demonstrated that the presence of squamous metaplasia in the surface epithelium was associated with unsuccessful EN-DCR. However, the precise mechanisms involved in wound healing in the respiratory mucosa remain unclear.
Outcome Assessment after EN-DCR
The outcome assessments should be based on relief of symptoms, absence of dacryocystitis, and objective signs, and there needs to be an adequate follow-up time. 85 The assessments of objective findings include endoscopic visualization of neo-ostium, 86 lacrimal sac irrigation, and a functional endoscopic dye test.64,72
Patient satisfaction regarding symptom relief and improvement in quality of life is the predominant consideration when determining the success of a surgical intervention. The subjective assessment after EN-DCR includes evaluation of disease-specific symptoms and quality of life questionnaires.87,88 In an attempt to meet that clinical need, recently, two questionnaires, the Lacrimal Symptom Questionnaire and NLDO Symptom Score, were validated.66,68 The most important difference between these two questionnaires is that the NLDO Symptom Score measures only the symptoms related to the lacrimal pathway obstruction, whereas the Lacrimal Symptom Questionnaire includes an additional score for social dimensions.
However, sometimes the objective assessments seem to point to a successful outcome (e.g., fluent lacrimal sac irrigation) related to the procedure, but the symptoms of the patient remain, at least to some degree, most likely due to a functional obstruction in the lower lacrimal pathway.34,89,90 Probably, the functional obstruction is related to insufficiency of lacrimal pump function and often leads to a poorer outcome after surgery. A failure of the lacrimal pump is the most likely cause of continuous postoperative epiphora in the presence of a patent rhinostoma and free (positive functional endoscopic dye test) flow of fluorescein into the nose. 91
Future Studies
Although the success rate of primary EN-DCR is high, 16 not all procedures succeed, in particular, revision procedures tend to have a lower success rate92,93 The most common reason for the failure of this operation is the formation of granulation tissue or scar over the rhinostomy site.40,73,94 It has been hypothesized that the intraoperative topical use of antiproliferative mitomycin C could reduce postoperative scarring and improve the success rate in primary and revision EN-DCR. Recent studies confirm that mitomycin C may improve the outcome of EN-DCR, particularly in revision cases.95–98
Future studies should be directed at projects related to wound healing and regulation of inflammation and fibrosis in the nasal mucosa, which might reveal novel predictors of outcomes for operations in the nasal cavity. 84 These studies are needed to clarify whether these predictors have any implications for operative techniques and for preoperative and postoperative treatments in patients with NLDO. There is also a definite need to create generally accepted and cost-effective clinical treatment protocols for patients with NLDO.
Conclusion
EN-DCR is an effective procedure in adult patients with saccal and postsaccal obstructions of the lacrimal pathway. To achieve the best possible outcome, the surgeon should adhere to standard procedures, not only with respect to surgical technique but, in particular, with pre- and postoperative assessments. As in all surgical procedures, it is inevitable that there will be a learning curve in EN-DCR; however, by adopting a cautious approach, one can increase the likelihood of success and patient satisfaction.
