Abstract
Mayer–Rokitansky–Küster–Hauser syndrome has a prevalence of one in 4000 females and is the most common cause of vaginal aplasia. Management of Mayer–Rokitansky–Küster–Hauser syndrome patients includes, along with psychological support, the creation of a neovagina. Creatsas vaginoplasty is a fast and simple technique in which a perineal skin flap is used to create a perineal pouch. Initially, the hymen is cut to avoid hemorrhage during the patient's first intercourse, and a U-shaped incision is made at the perineum. Afterwards, the tissues are mobilized and the inner skin margins of the created flap are stitched together using absorbable sutures. The same material is used to approximate the perineal muscles, subcutaneous fat and outer skin margins. In our institution, the Creatsas vaginoplasty has been performed in 200 patients over the last 23 years, with excellent results.
Mayer–Rokitansky–Küster–Hauser (MRKH) syndrome (also referred to as ‘Müllerian aplasia’) is a rare congenital anomaly that represents the most common cause of vaginal aplasia. It is characterized by the absence or hypoplasia of the Müllerian duct derivatives (the uterus and the upper two-thirds of the vagina). The incidence of the syndrome ranges from one per 4000 to one per 10,000 female newborns [1]. The etiology of the syndrome is considered to be genetic, but despite the fact that many candidate genes have been studied, their role and the mechanism of genetic inheritance remains unclear.
Mayer–Rokitansky–Küster–Hauser syndrome is responsible for approximately 10% of all cases of primary amenorrhea [2]. In adolescent girls with normally developed secondary sexual characteristics, normal ovarian function and a normal XX karyotype, who present with primary amenorrhea, Müllerian aplasia is the most probable diagnosis. In some cases, the uterus may be extremely rudimentary and have a functioning endometrium. In such cases, patients with MRKH present with abdominal pain, owing to progressive blood congestion in the uterine cavity. Absence of the Müllerian duct derivatives is, in some cases, accompanied by other malformations. Upper urinary tract anomalies such as pelvic or horseshoe kidney, unilateral renal agenesis, renal pelvis and ureter duplication are among the most common malformations related to the syndrome and are observed in approximately 40% of patients with MRKH [3]. Skeletal anomalies are rarer (observed in 10–12% of the patients) and mostly involve the spine, including wedge and the presence of supernumerary or rudimentary vertebrae [4]. MRKH has also been associated with disorders of the otologic sphere (usually conductive hearing impairment owing to middle ear malformations) [5]. In addition, cardiovascular disorders have been reported in patients with MRKH syndrome, including Fallot's tetralogy and the presence of an aortopulmonary window. Rare complications of the syndrome, reported from our center (University of Athens, Greece), include the development of leiomyomas in the rudimentary uterine horns and the occurrence of symptomatic descending salpingitis [6,7].
Given the vast heterogeneity of the syndrome's clinical expression, the adoption of a standard classification system is mandatory in order to facilitate further studying of the syndrome. Through the years, several methods of classification have been proposed. Nowadays, the classification proposed by Oppelt et al. is considered to be the most useful, especially when studying the genetics of the syndrome [8]. The classes are as follows:
Typical MRKH syndrome: the most common form of the syndrome (64% of the cases) and consisting of isolated aplasia or hypoplasia of the Müllerian duct derivatives;
Atypical MRKH syndrome: the second most common form of the syndrome (24% of the cases), in which ovarian dysfunction or renal malformation is present along with the Müllerian aplasia;
Müllerian hypoplasia/aplasia, renal agenesis and cervicothoracic somite dysplasia (MURCS) association: a rare situation that relates to 12% of MRKH cases and combines Müllerian aplasia or hypoplasia along with renal, cardiac and skeletal malformations.
Diagnostic procedure
Typically, a girl with MRKH syndrome seeks medical advice at approximately 16 years of age when the problem of amenorrhea arises. However, in some cases, the primary cause that leads a girl to an expert is the inability to have normal sexual intercourse.
The cornerstone of the initial evaluation of the patient is the clinical examination, since it can reveal an absence of the vagina and a shallow dimple (2–7 cm) at the introitus area, despite the presence of normal external genitalia. Gynecological examination can be performed even at neonatal age and can clearly reveal vaginal aplasia very early in the patient's life. The patient's secondary sexual characteristics are normally developed. A per rectum bimanual gynecological examination is used to detect the absence of the uterus. Occasionally, it may reveal the presence of hematometra, where a rudimentary uterus with a functioning endometrium is present.
The next step in the diagnostic procedure is the hormonal evaluation of the patient. As mentioned previously, women with MRKH have normal ovarian function. As a result, serum levels of follicle stimulating hormone, luteinizing hormone, estradiol and progesterone are expected to be within the normal range. Androgen serum concentration levels may, rarely, be elevated with or without the presence of clinical hyperandrogenism (acne and hirsutism). Recently, mutations in the WNT4 gene have been associated with hyperandrogenemia in patients with MRKH syndrome [9]. Significantly, elevated androgen levels usually point to androgen insensitivity syndrome (AIS) [1]. Karyotyping can confirm the AIS diagnosis in these cases and is a valuable diagnostic tool for the diagnosis of AIS in prepubertal children who do not have sex steroid production and in males with genetic testosterone synthesis disorders. The presence of an XY karyotype points to a diagnosis of AIS, while a normal XX karyotype in a girl with absence of the uterus and vagina points to a diagnosis of MRKH syndrome.
Further evaluation of the patient includes a pelvic ultrasound scan, MRI and an intravenous pyelogram, as they can reveal anatomic defects of the genital tract and kidneys. MRI provides a better assessment of the pelvic anatomy, but is rarely needed in the initial evaluation of the patient although it is imperative in cases where the findings of the ultrasound imaging are inconclusive. Intravenous pyelogram is only used in cases where the MRI does not provide sufficient information regarding the anatomic integrity of the urinary system since as it involves x-ray radiation, which is better to avoid in a young girl. The last examination that will secure diagnosis is the exploratory laparoscopy, which provides a clear image of the pelvic anatomy. It should be noted that laparoscopy is not necessary to diagnose Müllerian aplasia but is useful in the evaluation of patients with cyclic abdominal pain in order to exclude the presence of a functioning endometrium in the uterine remnants. Should that be identified, excision of the remnants is performed. Finally, otorhinolaryngologic, orthopedic and cardiologic evaluations should also be performed in order to reveal possible associated anatomic defects.
Mayer–Rokitansky–Küster–Hauser syndrome presents two major consequences in a patient's life. First, owing to the absence of the vagina, normal sexual intercourse is not possible. Pregnancy is also impossible, owing to the absence of the uterus, despite the fact that the ovaries are present and have normal function. The definitive diagnosis of the syndrome causes a major psychological shock for both the patient and the patient's parents and makes psychological counseling essential. The patient should be informed that, thanks to modern techniques, a neovagina may be created, and that she will enjoy a normal sexual life. By contrast, the young girl should also be informed that surrogate pregnancy is the only option for reproduction.
Creation of neovagina
Taking into account the consequences that the diagnosis of MRKH syndrome has on a woman's self-image and sexuality, it is easy to understand that creation of a neovagina is necessary in order to provide the young girl the prospect of a normal sexual life. To date, numerous surgical and nonsurgical techniques have been proposed for the correction of vaginal aplasia.
Nonsurgical methods
Among the nonsurgical methods, Frank's technique and its modification by Ingram are the most widely used. Frank's technique involves the placement of dilators into the vaginal dimple. The dilators are held in place by the patient herself for 30 min to 2 h every day. The dimple gradually increases in both length and width in order to form a normally sized neovagina [10]. Ingram described a modification of this technique, where the patient sits on a bicycle seat stool and uses her trunk weight in order to exert the necessary perineal pressure on the dilator [11]. Although these techniques are associated with much less morbidity than the operative ones, they can be very disturbing for the young girl. Therefore, they are only indicated in highly motivated and emotionally mature girls who wish to avoid surgery. Finally, Frank's technique can only be applied when the existing vaginal dimple has a depth of at least 3–4 cm. The vaginal dimple should also be soft and pliable, in order to be easily stretched.
Surgical methods
When the patient does not meet the aforementioned criteria, surgical treatment is generally preferred. Surgery should aim to create a vaginal canal with the appropriate dimensions and correct axis to allow intercourse without the need for continued postoperative dilation. Nowadays, the most popular techniques are the McIndoe operation [12,13] (also known as the McIndoe–Bannister or Abbé–McIndoe operation), the Vecchietti procedure [14], the Williams vaginoplasty [15] and its modification by Creatsas [16–18]. The Davydov technique [19,20] and bowel colpoplasty [21–23] are also used for vaginal reconstruction, but they are not commonly used.
The McIndoe operation is very commonly used by gynecologists in the USA. This technique involves the surgical creation of a space between the patient's rectum and bladder, and the placement of a mould covered by a full-or split-thickness skin graft. Use of amniotic tissue or in vitro-cultured vaginal tissue has also been reported, providing promising results [24,25]. With this technique, the created neovagina is functional 6–10 weeks after surgery, but postoperative dilation is essential until the woman has regular sexual intercourse. Patients who do not like the use of dilators should not be treated with the McIndoe technique since a lack of postoperative dilation leads to a stenosed and nonfunctional neovagina [1]. Moreover, this technique is associated with complications that, although rare, can be serious, such as urethral, bladder and rectum injury, severe hemorrhage, postoperative infections and the creation of fistulas.
The principle of the Vecchietti procedure is to elongate the vaginal dimple by dragging it from the inside of the abdominal cavity. This is achieved with the placement of a small acrylic ball in the vaginal dimple, which is gradually pulled up by sutures that run from the ball to an apparatus attached to the abdominal wall (passing either intra- or extraperitoneally). Only several days of traction are required for the neovagina to be formed [14]. When this technique was introduced back in the mid-1960s, a laparotomy was mandatory in order to pass the sutures and place the traction device on the abdominal wall. In 1992, Gauwerky et al. introduced the laparoscopic modification of the Vecchietti technique and, since then, numerous variations involving the course and the securing of the sutures have been proposed [26,27]. The major disadvantage of this method is that the tension of the sutures needs frequent adjustment, which can be very painful for the patient. Postoperative dilation is also necessary in order to maintain vaginal length.
With the Davydov technique, the patient's peritoneum is used as a lining in order to create the neovagina [19,20]. It is a relatively complex procedure, which may lead to severe complications such as urethra injury and the creation of fistulas.
Bowel colpoplasty is a major operation in which a bowel segment is used to form the neovagina [21]. This technique is considered to be associated with higher failure and morbidity rates and should not be used as a first-line treatment for vaginal agenesis [22,23,28].
Creatsas vaginoplasty
The Creatsas vaginoplasty is based on the Williams vaginoplasty described by Williams and involves the use of a skin flap from the patient's perineum in order to create a perineal pouch [15]. We have modified and applied this technique as follows: in the first step of the procedure, under general anesthesia, a Foley catheter is inserted into the urethra and four Allis clamps are used to put the vulval tissues under stretch (Figure 1). The vulva should at this time be carefully inspected for human papilloma virus lesions. It should be remembered that MRKH patients, who are usually over 17 years of age, tend to change sexual partners (prior to seeking medical advice), trying to achieve successful sexual intercourse. As a result, these patients have a high risk of exposure to the human papilloma virus. In the next step, the hymen is cut with the use of diathermy at the third, sixth and ninth hour positions. It should be noted that the hymen is present in girls with MRKH syndrome as it is not embryologically originated from the Müllerian duct. Rupture of the hymen during first sexual intercourse could terrify the young girl, given her psychological status after the surgery.
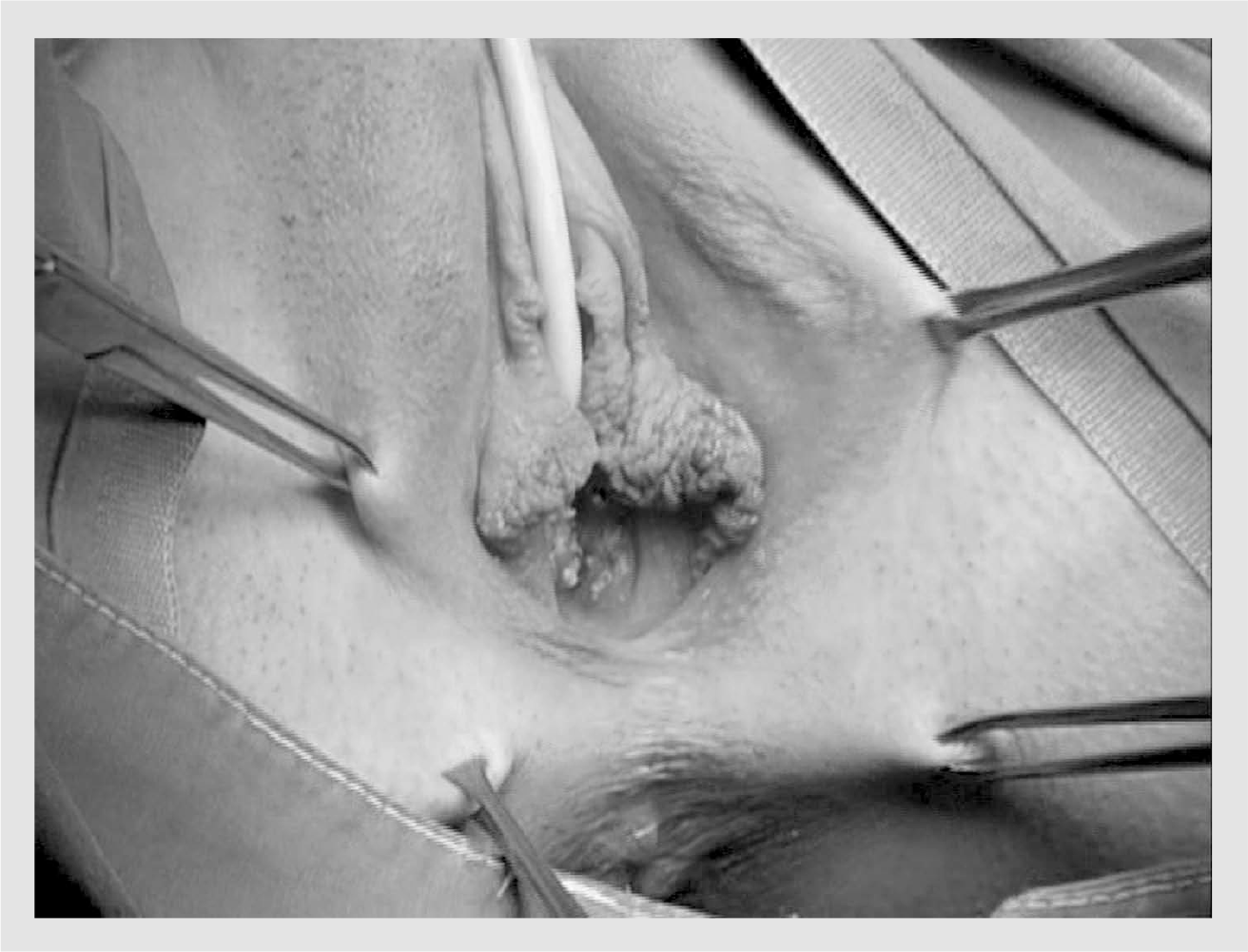
Placement of the Allis clamps.
Subsequently, a symmetrical U-shaped incision is made in the vulva, starting 4 cm lateral to the external urethral meatus at the medial side of the labia majora, extending down to the perineum and up to the other side of the vulva, as shown in FIGURE 2. The perineal subcutaneous tissue is mobilized.

U-shaped incision in the vulva.
A layer of interrupted 2–0 absorbable sutures is put between the inner skin margins with the knots lying on the inside of the neovagina being created in order to create a pouch, as shown in Figure 3. The perineal muscles and subcutaneous fat are then approximated using the same suture material.

The first layer of 2–0 absorbable sutures between the inner skin margins.
Finally, absorbable sutures are also used in order to stitch the external skin (Figure 4). It is important to observe symmetry throughout the whole procedure in order to achieve a proper aesthetic result.

Stitching of the outer skin margins.
Creatsas vaginoplasty is a safe technique with a surgical time of approximately 20 min and a mean hospitalization time of 6 days. Hematoma, wound dehiscence or infection are possible but are rare complications. Careful hemostasis during the operation is essential in order to prevent the occurrence of hematoma. Wound dehiscence can be prevented by avoiding leg abduction during the first postoperative days. Typical wound hygiene and administration of three doses of wide spectrum antibiotics postoperatively significantly reduce the risk of wound infection. Hair growth at the neovagina area is a very rare complication that can easily be managed with laser treatment. The results are summarized in Table 1.

Mean age of patients in years (range): 17.2 (13–26). Mean length of surgery in min (range): 28 (24–43). Mean length of hospital stay in days (range): 6 (3–11).
Williams had noted that because of the high elevation of the perineum, when his patients voided, the urinary stream was distorted and occasionally, postvoiding dribbling of urine was caught in the neovagina. In the Creatsas modification of the Williams vaginoplasty, the above-mentioned phenomenon is not observed because the perineum is not elevated as high as in the Williams technique, reaching just below the level of the urethral meatus.
One of the major advantages of this technique is that there is no need for the postoperative use of dilators to maintain the surgical result, even if the patient does not have regular sexual intercourse. Once the surgical trauma has healed, the patient is free to have her first sexual intercourse. Initiation of sexual relationships, in most of the cases, relieves the patients from the stress caused by their situation, and, in addition, improves the surgical result regarding the size and axis of the neovagina.
Our experience
A total of 200 patients have undergone the Creatsas vaginoplasty over the last 23 years (1987–2009) in our institution (University of Athens, Aretaieion Hopsital, Greece). The mean age of the patients at the time of operation was 17.2 years, while the age ranged from 13 to 26 years. In the vast majority of patients (n = 191), the created neovagina had a length of 12 cm and a width of 5 cm, while the dimensions of the neovagina were insufficient in only nine patients (7–9 cm in length). In these cases, postoperative vaginal dilation was performed in order to achieve a satisfactory result. Wound opening was found in eight patients (4%) and hemorrhage during first intercourse was only reported by one of the patients. Mean hospitalization time, as reported previously, was 6 days [18].
Assessment of the functionality of the neovagina was carried out for all patients through the annual postoperative follow-up (FIGURE 5). Patients were asked to evaluate their sexual life as being satisfactory, adequate or unsatisfactory, and also to report any other possible problems, such as vaginal dryness or dyspareunia. A total of 189 patients (94.5%) declared having a satisfactory quality of sexual life, while ten (0.5%) reported theirs to be adequate (5%). Only one woman (0.5%) reported an unsatisfactory sexual life, after having changed sexual partners more than once. Vaginal dryness or dyspareunia were not reported by any of the patients. Excessive hair growth in the neovagina was observed in three patients and was successfully managed using laser treatment [18].

Postoperative result.
Postoperative ultrasound evaluation reveals that, although the axis of the neovagina appears to be parallel to the perineum, repeated sexual intercourse forces the neovagina to match the anatomical axis of the normal vagina [29]. This happens because of the excellent flexibility of the perineal tissues (FIGURE 6).

Ultrasound imaging of a neovagina, performed with the technique described by Botsis et al. (longitudinal section) in [29].
Recently, two MRKH patients who were treated at our center had children by surrogate pregnancies. In one case, the surrogate woman was the patient's mother, while in the other case there was no familial relationship between the patient and the surrogate woman. Both cases were twin pregnancies and no significant antenatal and perinatal complications occurred.
Managing the patient after the diagnosis
Diagnosis of MRKH syndrome is a strong psychological shock for the young girl and her family, has significant consequences on the patient's sense of sexuality and self-esteem and makes psychological counseling necessary for both the girl and her parents. ‘Buddies’ (older patients with vaginal agenesis) can also offer significant help in supporting the young girl and her parents. The girl needs to be clearly informed that, thanks to modern techniques, she will have the opportunity to have a pleasant and healthy sexual life. On the other hand, it should be clarified that surrogate pregnancy will be the only way for her to have children. It should be noted that, to date, daughters of MRKH patients conceived via assisted reproduction techniques have had normal genital tracts.
The next step in patient management is making the decision as to which is the appropriate technique for the neovagina creation. In order to choose the technique with the best result, the following points must be taken into consideration:
The emotional maturity of the girl should be taken into consideration regarding the best timing for vaginal aplasia correction;
Patients with a vaginal dimple larger than 2.5 cm who are willing to avoid surgery and have no objections regarding dilator use should be treated with nonsurgical techniques since they will have less morbidity. Initial instruction regarding the use of vaginal dilators is important, since an extremely motivated patient may create a very good neovagina, avoiding the need for surgery. In reported series, 43–89% of patients achieve satisfactory results using Frank's technique [30,31];
No matter which technique is chosen, the initial surgery is more likely to succeed than follow-up procedures. Failure of the McIndoe, Davydov or sigmoid colpoplasty techniques in particular (usually because of insufficient postoperative dilation) leads to vaginal scar tissue development and stenosis. Patients who reject dilator use should not be treated with surgical techniques that require postoperative dilation. In these cases, the Creatsas vaginoplasty is more appropriate;
As of yet, there is no consensus regarding the best surgical technique for vaginal aplasia correction. The decision of the surgical method is based on the experience of the surgeon [32];
The decision regarding which surgical technique will be performed can also be affected by the healthcare policy. Operating surgeons may be encouraged to use safer, quicker techniques that require less hospitalization of the patients;
The aim of any surgical technique is to create a vaginal canal of adequate size with the correct axis to allow intercourse without the need for continued postoperative dilation;
The surgical method selected must be the one that is associated with the least morbidity. The McIndoe operation and sigmoid colpoplasty are techniques associated with a possible risk of severe complications.
Conclusion
The Creatsas vaginoplasty is a technique that was developed in our center and has provided excellent results during the last two decades. The undeniable benefit of this technique is that there is no need for postoperative dilation and, consequently, it can be performed in cases where the young girl has objections regarding dilator use. Moreover, cutting of the hymen prevents hemorrhage during the patient's first intercourse, while the use of absorbable sutures throughout the procedure help to prevent wound opening. A short hospitalization time and the opportunity of the patients to start sexual relationships soon after healing of the surgical wound are also important advantages of this technique. Complications associated with the procedure are rare and nonsevere.
The vaginal canal created with this technique has adequate dimensions and the correct axis to offer the patient the prospect of having a pleasant sexual life. The vast majority of our patients were totally satisfied with the quality of their sexual lives, while only one declared a nonsatisfactory sexual life.
The ideal technique for reconstruction of vaginal aplasia should be safe, simple, quick and provide a satisfactory sexual life to the patient. Our results over the past years have demonstrated that Creatsas vaginoplasty has all of these features.
Future perspective
Understanding the genetic background of MRKH syndrome is a major challenge for the coming years. Some candidate genes have already been studied but no single factor has yet been identified as being responsible for the syndrome. Further studies in the near future will help us to identify a possible genetic cause of the syndrome and to understand the molecular mechanisms that block the Müllerian duct's development during the early stages of intrauterine life.
It would also be interesting to conduct a study in order to compare the quality of patients' sexual lives after the application of different techniques. This is extremely difficult since there is no standardized method for assessment, even for normal women, and because the quality of sexual life is strongly related to the partner. Moreover, there are many uncontrollable variants, such as the skills of the different surgeons that would participate in the study and the possible unwillingness of the patients to give a non-favorable review of the techniques (especially in cases where the evaluation of the results is performed by the operating surgeon). On the other hand, this would be the only way of comparing the efficiency of the available techniques.
Finally, we should continue to make efforts to perform first human uterus transplantation. This would be a major breakthrough regarding the management of MRKH patients that will offer the opportunity for MRKH patients to have children without the need of a surrogate mother.
Executive summary
The most common cause of vaginal aplasia is Mayer–Rokitansky–Küster–Hauser (MRKH) syndrome.
MRKH syndrome is characterized by the absence of the uterus and the upper two-thirds of the vagina.
In women with MRKH, the ovaries are present and have normal endocrine function.
Vaginal aplasia is often accompanied by renal, skeletal and auditory defects.
Per rectum gynecologic examination is the first step of the diagnostic procedure.
Hormonal evaluation, pelvic ultrasound imaging and MRI are essential in order to set the diagnosis.
Diagnostic laparoscopy and orthopedic and cardiologic evaluation may also be required.
A variety of surgical and nonsurgical techniques are available for the construction of a neovagina.
Patients with a vaginal dimple deeper than 3 cm, who have no objections against dilator use, should preferably be treated with Frank's technique.
McIndoe's method, Davydov technique and bowel colpoplasty and their variants are major operations that may lead to serious complications and should only be considered in selected cases.
Creatsas vaginoplasty is based on the Williams vaginoplasty and involves the creation of a perineal pouch using a skin flap from patient's perineum.
Initially, the hymen is cut in order to avoid hemorrhage during the patient's first intercourse, and a U-shaped incision is made at the perineum.
Afterwards, the tissues are mobilized and the inner skin margins of the created flap are stitched together using absorbable sutures.
The same material is used to approximate the perineal muscles, subcutaneous fat and outer skin margins.
Postoperative dilation is not necessary for patients who have undergone Creatsas vaginoplasty.
The Creatsas vaginoplasty has been performed in 200 patients over the last 23 years.
A functioning vagina of 10–12 cm in depth and 5 cm in width has been created in 191 cases (95.5%), while a vagina of 7–9 cm in depth and 2–3 cm in width was created for the remaining nine patients (4.5%).
A total of 94.5% (189 out of 200) of the patients claimed to have a satisfactory sexual life, 5% reported an adequate sexual life and only one patient (0.5%) reported an unsatisfactory sexual life after having changed more than one sexual partner.
Creatsas vaginoplasty is a simple and safe procedure that has provided excellent results.
Diagnosis of the syndrome has a strong impact on the patient's psychological status.
Patients should be informed about available treatments, their efficacy and possible complications.
Psychological counseling should be offered to both the patient and her parents.
The emotional maturity of the girl should be taken into consideration regarding the best timing for vaginal aplasia correction.
Creation of a neovagina is a solution regarding the patient's sexual life, while surrogate pregnancy allows patients to have children.
There is no consensus regarding the best surgical technique for vaginal aplasia correction. The decision for the surgical method is based on the needs of the patient, the experience of the surgeon and the healthcare policy.
Footnotes
The authors have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants or patents received or pending, or royalties.
No writing assistance was utilized in the production of this manuscript.
