Abstract
Unlike pharmacological agents that are taken for proscribed periods of time, food and nutrient intakes have the possibility of affecting bone health over the entire lifespan. While deficiencies or excesses of individual nutrients have been shown to affect bone, it is likely that individual foods or dietary patterns have important effects related to skeletal health. While biochemical mechanisms exist to relate a deficiency of vitamin K to altered bone metabolism, clinical trials related to supplementation of this nutrient have been confusing. It is likely that these disparate results are related to the fact that interactions of nutrients have not been considered or the possibility that suboptimal nutrient status is a marker of poor nutritional status. Vitamin A excess has been postulated to be related to high fracture risk; however, it is likely that retinol is not the best marker for the proposed interaction. Altering whole food patterns, such as the Dietary Approaches to Stop Hypertension diet, have demonstrated beneficial effects on bone metabolism. Individuals who select some vegetarian patterns may need to consider supplementation with nutrients such as calcium and protein. Future studies should center on whole food and dietary patterns and their relationship to bone metabolism and fracture risk.
Osteoporosis is a skeletal disease characterized by low bone mass and microarchitectural deterioration of bone with a subsequent increase in bone fragility and susceptibility to fracture [1]. The National Osteoporosis Foundation estimates that approximately 8 million of the 10 million Americans with osteoporosis are women [101]. A total of 20, 10 and 5% of non-Hispanic Caucasian and Asian, Hispanic and non-Hispanic Black women are estimated to have osteoporosis, respectively. In addition, 52, 49 and 35% of non-Hispanic Caucasian and Asian, Hispanic and non-Hispanic Black women are estimated to have low bone mass (osteopenia), respectively [102]. It has been estimated that from 46 to 62% of bone mineral density (BMD) accrual is related to genetic factors; hence, 38–54% of BMD could be attributed to lifestyle factors [2,3]. The importance of calcium and vitamin D have been extensively reviewed related to bone [4–8]. This paper will review relationships of selected other nutrients (vitamin A and vitamin K), a food (milk) and the effect of dietary patterns on bone health.
Considerations related to the interpretation of data related to nutrients & bone
There are several factors that must be taken into account when evaluating the nutrition literature related to bone health.
Nutrition has been redefined as a whole-organism science with a shifting focus towards an understanding of nutrient intakes that promote the optimal functioning of an organism [9,10]. It has been suggested that foods and dietary patterns and not individual nutrients are the fundamental units of nutrition [10]. Jacobs has suggested a hierarchical pattern that progresses from specific nutrients, food components, foods and food groups to dietary patterns [10]. Table 1 lists examples of levels of evaluation for bone/nutrition-related investigations [9]. The nutrition literature is replete with examples where single nutrients either have an unexpected effect or no effect on health, while whole foods provide a beneficial effect; inter-relationships of nutrients were not taken into account [11–14]. An example is the protective effect of a diet high in fruits and vegetables on the development of lung cancer [15], while β-carotene increased lung cancers [16]. The data from the Women's Health Trial demonstrating that calcium did not protect against fractures [17], did not take into account the fact that the majority of the subjects were vitamin D deficient [18,19], an example of the importance of considering the inter-relationships between nutrients.
Proposed structure for nutritional investigations related to bone.
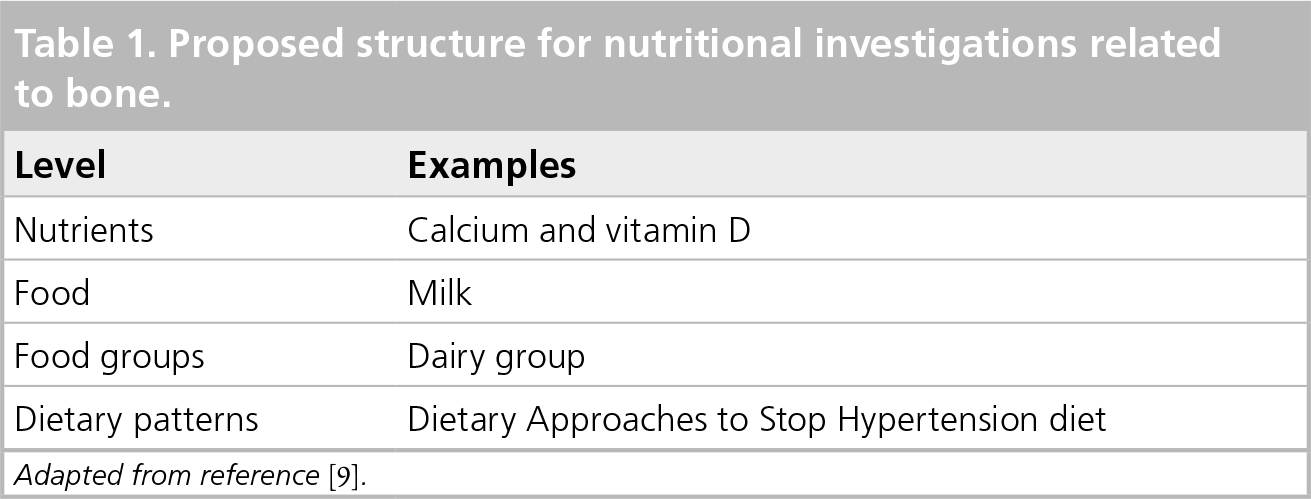
Adapted from reference [9].
As opposed to pharmacological therapies for metabolic bone disease, which most individuals take for defined periods of time, nutrient intakes have the possibility of affecting bone health over the entire lifespan. Heaney has developed the concept of long-latency nutrient deficiency diseases where inadequate nutrient intakes or specific food patterns over the lifespan contribute to the development of chronic diseases [20]. Many short-latency, nutrient-deficiency bone diseases have been documented, such as scurvy and rickets. Osteoporosis can be classified as a long-latency disease caused by inadequate intakes of many nutrients, including calcium and vitamin D. Application of the concept of long-latency disease suggests that short-term nutrient investigations likely do not present a total picture of the effect of the nutrient related to bone health.
The remodeling transient is another important consideration in the evaluation of nutritional interventions on bone [21]. The remodeling transient describes the bone remodeling sequence that includes initial osteoclastic resorption and subsequent osteoblastic formation [21]. A nutritional intervention will affect bone resorption first with new remodeling units being taken out of service faster than the mineralizing units with net bone accrual. Therefore, the first-year response to a nutritional therapy is an expression of the remodeling transient and indicates that the remodeling sequence is functioning normally. The effect of any nutritional intervention should be evaluated after the remodeling transient is fully expressed [21]. This phenomenon has not always been taken into account in osteoporosis investigations related to nutrients.
A variety of design and methodological variables must be taken into account when evaluating the nutrition literature related to bone [22,23]. Prospective, double-blind, randomized, placebo-controlled trials are necessary to establish a causal relationship between interventions and bone health. Many studies are retrospective or cross-sectional. Such cross-sectional or retrospective studies can note relationships between variables, but cannot be used to prove causal relationship [22]. Cross-sectional studies may not account for confounding factors that can hide or cause a relationship between variables and many do not take into account lifetime intakes of nutrients. It has also been acknowledged that groups who adopt specific dietary patterns or take dietary supplements often differ in other lifestyle risk factors, which may bias the results [24].
Studies reporting relationships between nutrient intakes and bone health variables using a food frequency methodology have acknowledged limitations related to assessment of nutrient intakes [25,26].
Interpretation of the effects of nutrients, foods, and dietary patterns on bone health is challenging because there is heterogeneity in outcome variables (BMD, bone markers of formation and resorption, and fracture).
Finally, nutrient levels can be measured in a wide range of tissues and there is often controversy about the optimal assay to evaluate a nutrient (see section on vitamin A and bone) [27].
With these factors in mind, this review will evaluate some of the current evidence related to the effects of several individual nutrients (vitamin K and vitamin A), a food (milk) and dietary patterns on bone health. Where applicable, the data from women will be highlighted.
Individual nutrients & bone health
While there are caveats, as outlined in the introduction, there has been much published literature related to individual nutrients and bone health. This paper will review one nutrient where low intakes are proposed to have a harmful effect and one nutrient where high intakes are proposed to have a deleterious effect on bone health.
Vitamin K
Vitamin K is a fat-soluble vitamin found in green leafy vegetables. The phylloquinones (vitamin K1), are found in green leafy vegetables, soybean and canola oils and are the most important dietary sources of vitamin K. Menaquinones (vitamin K2), are endogenously synthesized and are found in small amounts in chicken, meat and certain cheeses [28]. Fermented soybean products such as natto contain relatively large amounts of menaquinones.
The function of vitamin K is γ-carboxylation of glutamate residues to form γ-carboxygluatmate (Gla) in vitamin K-dependent proteins such as osteocalcin (bone Gla protein), matrix Gla protein and clotting factors II, VII, IX and X. The formation of Gla occurs through a unique vitamin K-dependent post-translational carboxylation of specific peptide-bound glutamate residues in a process that is inhibited by warfarin [29]. Gla residues have a high affinity for calcium; therefore vitamin K deficiency could be detrimental to skeletal health.
There have been several vitamin K2 supplementation trials that have used large doses of menaquinone-4 (45 mg/day) and have documented beneficial effects on bone health [30–32]. A review and meta-analysis of these trials suggested that menaquinine-4 supplementation reduces bone loss and fractures among Japanese patients [28,33]. However, since an unpublished internet trial of menaquinone supplementation in Japanese postmenopausal women, which did not show a favorable effect on fracture, was not included in the meta-analysis, that conclusion has been questioned [34]. This study has recently been published and shows that vitamin K2 plus a calcium supplement was not effective in preventing vertebral fractures in postmenopausal women compared with a calcium supplement alone. However, there was a lower risk of spinal fractures in women with at least five baseline vertebral compression fractures taking the combination of vitamin K2 and calcium [35].
The studies related to vitamin K1 have generally not shown a benefit related to bone markers, or changes in BMD over adequate calcium and vitamin D supplementation [36–39]. Binkley et al. completed a double-blind, placebo-controlled trial of 381 postmenopausal women (>5 years postmenopausal) who received 45 mg of vitamin K2 (menatetrenone [MK-4]), 1 mg of vitamin K1, or placebo for 1 year [40]. All groups received daily calcium and vitamin D supplements. BMD of the lumbar spine and proximal femur were measured at baseline, 6 and 12 months. Serum bone-specific alkaline phosphatase and N-telopeptide of type 1 collagen (NTX) were measured at baseline, 1, 3, 6 and 12 months. Vitamin K1 and MK4 supplementation reduced serum undercarboxylated osteocalcin levels but did not change bone-specific alkaline phosphatase or NTX levels. Vitamin K1 and MK4 supplementation had no effects on lumbar spine, proximal femur or proximal femur geometric parameters. The authors concluded that no role for vitamin K could be demonstrated for osteoporosis prevention in North-American women who were also receiving calcium and vitamin D. They speculated that previous studies demonstrating a relationship between undercarboxylated osteocalcin and bone health may reflect that undercarboxylated osteocalcin levels are a marker for poor diet quality.
In summary, at least in North-American women, vitamin K supplements appear to offer no additional benefit for bone health over calcium and vitamin D supplementation. It is speculated that earlier studies demonstrating a beneficial effect of vitamin K supplementation may be related to vitamin K acting as a marker of poor nutritional status or diet quality. The vitamin K and bone literature underscore the importance of considering the interactions of nutrients and food on bone health.
Vitamin A
Vitamin A includes a family of essential fat-soluble compounds that are structurally related to the lipid alcohol retinol. The vitamin A family also includes the provitamin A compounds, the carotenoids. Good sources of preformed vitamin A are organ meats. Provitamin A is found in yellow and dark green vegetables such as carrots, sweet potatoes, spinach, kale and turnip greens. In the USA, milk and margarine are fortified with vitamin A. Vitamin A functions in vision, growth, reproduction, cell proliferation and immune system integrity [41].
There are animal and human data indicating that hypervitaminosis A can increase bone resorption and inhibit bone formation [42]. There have been several observational studies suggesting that retinol intakes, slightly higher than the recommended daily allowance, are associated with low BMD and increased fracture risk (reviewed in [27]).
However, there are studies that do not support the conclusion that vitamin A is toxic to bone. It has been suggested that fasting serum retinyl esters rather than serum retinol levels are a more sensitive measure of excessive vitamin A intake, since they appear in the circulation if diet or supplemental vitamin A intake exceeds the liver storage capacity or retinol-binding protein production [27]. Ballew et al. evaluated the relationship between serum retinyl esters and BMD measured at the femoral neck, intertrochanter and total hip from the Third National health and Nutrition Examination survey (NHANES III) [43]. The sample included non-Hispanic White, non-Hispanic Black, Mexican–American men and women aged 20 years or older. Using regression analysis, the association between BMD and fasting serum retinyl esters was evaluated. They found no associations between fasting serum retinyl esters and BMD and concluded that retinyl esters were not associated with BMD.
Using 2606 British women over 75 years of age, the relationship between serum retinol, retinyl palmitate and β-carotene was evaluated as predictors of fractures using a case–control design [44]. During a mean follow-up of 3.7 years, there were 312 osteoporotic fractures and 92 hip fractures. Serum retinol, retinyl palmitate and β-carotene levels were not significant predictors of hip fracture or any osteoporotic fracture. They concluded that elevated retinol intake or modest retinol supplementation was not associated with net bone harm. In addition, no associations were found between vitamin A or retinol intake and hip or total fractures in postmenopausal women from the Women's Health Initiative (WHI) Observational study [45].
There has been one short-term supplementation trial of vitamin A in humans [46]. A total of 80 healthy men (aged 18–58 years) received either placebo or 7576 μg (25,000 international unit [IU]) of retinol palmitate daily. Serum bone-specific alkaline phosphatase and the N-telopeptide of type 1 collagen were measured after 2, 4 and 6 weeks of supplementation. Serum osteocalcin was measured at baseline and 6 weeks. None of the bone markers varied between groups at any of the time points. They concluded that short-term vitamin A administration did not affect bone markers. No outcome data is available for long-term vitamin A supplementation or in a cohort of women.
Therefore, there is mixed evidence related to the effect of vitamin A on bone health. The selection of the vitamin A metabolite to be measured is likely responsible for much of this inconsistency [27]. Serum retinol is a poor measure of excessive intake and serum retinyl esters have been suggested as a better measure of vitamin A excess [27]. Stable-isotope dilution techniques are now considered the standard for the measurement of vitamin A status [47]. This is an important issue since vitamin A deficiency is a major international public health issue [48]. In concert with the observation that foods and dietary patterns are the unit of nutritional importance, it has also been speculated that the detrimental relationships between vitamin A and bone may instead be related to foods and dietary patterns. Further studies, using improved methodologies related to vitamin A analysis, should be completed prior to reaching a final conclusion regarding the effect of vitamin A on bone.
Individual food & bone health
Milk
One of the lessons learned related to calcium studies and bone was that it is difficult to isolate the effect of calcium as a single nutrient. Bischoff-Ferrari documented that calcium supplementation alone is not enough to reduce fracture risk, unless vitamin D status is optimized [18,19]. This study illustrates the point that nutrients cannot be considered in isolation related to bone health. Milk will be discussed as an example of the effect of an individual food on bone health.
The inclusion of milk as a part of the dietary pattern is controversial [49–53]. Melnik hypothesizes that the protein in milk induces postprandial hyperinsulinemia and increases IGF-1 serum levels, which have detrimental effects on health, including atherosclerosis, diabetes mellitus, obesity and cancer [50]. However, McCarron and Heaney have reviewed several decades of literature and estimated that if adults in the USA increased their dairy intake to three/four servings per day there would be a first year saving of US$ 26 billion and 5-year savings of US$ 200 billion related to beneficial effects on obesity, hypertension, stroke, coronary artery disease, Type 2 diabetes, osteoporosis, nephrolithiasis, pregnancy outcomes and colorectal cancer [54]. Heaney has reviewed the evidence related to calcium, dairy products and osteoporosis [55] and concluded that inclusion of dairy products in Western diets is both cost efficient and cost effective and that diets lacking dairy products are also devoid of other nutrients such as calcium, phosphorus, magnesium, potassium and zinc, which could have potential beneficial effects on bone health [56]. In addition, the majority of the literature support a beneficial effect of milk consumption related to improved BMD and fracture risk [55].
Woo et al. randomized 441 community-living Chinese women (aged 20–35 years) to receive milk providing 1000 mg of calcium or no supplementation. BMD at the spine and total hip was measured by dual-energy x-ray absorptiometry (DXA) at baseline, 6, 12 and 24 months [57]. Bone markers were also evaluated. There was a higher spine BMD in the milk group at 6 months; however, at other time points there was no difference in BMD or bone markers. The authors speculated that lack of compliance may have explained the findings. Lau et al. assigned 200 Chinese women, at least 5 years past menopause, to receive 50 g of milk powder (800 mg calcium) or no supplementation [58]. BMD was measured by DXA and food diaries were used to measure dietary intakes. The average milk compliance was 94%. The group supplemented with milk lost less height and gained more weight than the nonintervention group. There was significantly less loss of BMD in the milk group compared with the nonsupplemented group. There was also a significant increase in 25-OH vitamin D levels and a decrease in the serum parathyroid hormone level in the milk-supplemented group. The authors commented that it was not possible to conclude whether it was the calcium supplement or supplementation of another nutrient that was responsible for the beneficial effects. They concluded that milk supplementation could be beneficial in Asia in diet patterns that are traditionally low in calcium content.
There have been no randomized, controlled trials evaluating the effect of dairy foods on fracture risk [59]; however, the review completed by the Dietary Guidelines Advisory Committee reported that five of eight observational studies show that dairy consumption has a beneficial effect on fracture risk [103].
In conclusion, while somewhat controversial, the preponderance of the evidence supports the usefulness of milk in individuals who are able or wish to consume dairy products. The data related to dairy products and bone should optimally be evaluated in light of total dietary patterns and other nutrients that also coexist in milk. Future studies could evaluate the effect of dairy products on fracture risk.
Dietary patterns & bone health
There have been numerous cross-sectional, observational and intervention trials that have evaluated the effects of dietary patterns on bone health.
Mediterranean diet pattern
Within Europe, the lowest reported incidence of osteoporosis is in the Mediterranean area [60] and it has been hypothesized that the Mediterranean dietary pattern, which emphasizes high intakes of fruits, vegetables, legumes, nonrefined cereals, fish and olive oil, moderate alcohol intake and is low in meat and dairy intake may be a contributory factor to the low fracture incidence. A total of 220 Greek women (mean age 48 ± 12 years) were enrolled in a cross-sectional trial to evaluate the effect of a Mediterranean diet pattern on bone health. BMD was assessed by DXA and dietary intake was estimated using 3-day dietary intake records [61]. Using multiple linear regression analysis controlling for age, menstruation status, body mass index and physical activity level; higher consumption of fish and olive oils and lower intakes of red meat were positively associated with lumbar spine BMD (p = 0.017). The authors speculated that the Mediterranean dietary pattern may have the potential to preserve bone in adult women [61].
Women's Health Initiative Dietary Modification Trial
Eligible participants from the WHI Dietary Modification Trial (aged 50–79 years at the time of enrollment) were assigned to a low-fat dietary pattern group (goals: total fat <20% of kcal; saturated fat ∼7% of kcal; fruit and vegetables > five servings/day; grain > six servings/day) or a dietary pattern with no changes [62]. A food frequency questionnaire was administered at baseline and after 1 year and then yearly to a third of the participants in a rotating sample. Total fractures and falls were reported. BMD testing was completed at three clinical centers (3951 women). After approximately 8 years of follow-up there were no differences in total osteoporotic fractures or fractures at specific sites between the groups. The dietary modification group had a lower risk of falling two times or more during the follow-up period than the comparison group (HR: 0.92; 95% CI: 0.89-0.96; p < 0.01). The BMD at the hip was 0.4-0.5% lower (p = 0.003) in the dietary intervention group than the comparison group at years 3, 6 and 9. The authors acknowledged that few women met the dietary goals of less than 20% of kcal from fat and that reliance on selfreported food frequency data could have biased the results. The trial was also not designed to test the effect of the diet pattern on osteoporotic fractures. In addition, the observed overall risk of fractures was lower than had been observed in other postmenopausal cohorts and the measured BMDs were, on average, higher than the general postmenopausal population, which could mean that the results were not generalizable to the population [62].
Dietary patterns high in fruit & vegetable intake & the acid-ash hypothesis
There is a large body of literature related to the acid-ash hypothesis, which suggests that food components, such as dietary proteins, produce acid loads that use the buffering capacity of bone, by release of alkaline salts to neutralize the acid load [63]. Lower body pH increases osteoclast activity [64], and drops in body pH within the physiological range can increase bone resorption [65,66]. Foods such as vegetables, fruits and dairy products contain potassium organic acid salts, which are metabolized to potassium bicarbonate and serve as buffers for acid production. Fenton et al. performed a metaanalysis of clinical trials related to the acid-ash hypothesis and found that net acid and calcium excretion are significantly related in both acid and alkaline urine (p < 0.001) but commented that there was no evidence that the calciuria is from bone or that the calciuria contributes to the development of osteoporosis [67,68]. Rafferty and Heaney, using dairy and meat foods as sources of potassium, found that high potassium diets do not exert a large effect on calcium balance since the reduction in calciuria from potassium intake is offset by reduction in intestional calcium absorption [69,70]. However, they noted that their results cannot be generalized to the possible beneficial effects of high fruit and vegetable diets.
There have been a variety of longitudinal cross-sectional, observational evaluations evaluating the effect of potassium-rich and bicarbonate rich diets and net endogenous acid production on bone health [71–74]. These data have generally suggested beneficial effects of such diet patterns on BMD and bone markers. However, as observational studies, this data cannot actually prove the hypothesis that potassium and bicarbonate-rich diets are beneficial to bone health.
A recent study of 103 female Japanese college students, aged 20–21 years, cross-sectionally evaluated green and yellow vegetable intake with bone area ratio of the os calcis as a measure of bone mass [75]. By adjusted logistic regression, women without a daily intake of vegetables had a fivefold risk of having low bone mass.
Intervention trials related to high fruit & vegetable diets
There have been three intervention studies related to the acid-ash hypothesis. The Dietary Approaches to Stop Hypertension (DASH) dietary pattern emphasizes fruits, vegetables, low-fat dairy foods, whole grain, poultry, fish and nuts in moderation and deemphasizes fats, red meats, concentrated sugars and sugar-containing beverages [67]. Since the diet pattern is calcium-rich and has a low acid content, such diets have been hypothesized to be beneficial for bone health [76]. An ancillary trial to the DASH-Sodium trial included 186 subjects who were randomized to a typical US diet or the DASH diet (51% of women in the control diet and 59% of women in the DASH diet group) with three levels of sodium intake (50, 100 and 150 mmol/day) [77]. All food was provided to the participants and the dietary patterns were consumed for 30 days, each in a random cross-over design. Serum osteocalcin was measured as a bone formation marker and serum carbon-terminal peptide of type I collagen (CTX) was evaluated as a bone resorption marker. Table 2 shows the bone marker results from the intervention trial. The serum CTX was 16–18% lower and the serum osteocalcin was 8–11% lower in the subjects on the DASH diet, suggesting lower bone turnover in the subjects on the DASH diet. There was no difference in urinary calcium levels between the treatment groups. The authors speculated that if the reduced bone turnover was sustained, the risk of osteoporosis could be lowered. They suggested that a variety of factors, including higher dietary calcium, potassium and magnesium intakes, low total dietary acidity, and the presence of antioxidants and phytochemicals from fruit and vegetable intake could be beneficial factors for bone health [77]. Nowson et al. evaluated 111 women, aged 45–75 years, on a DASH dietary pattern or a high-carbohydrate, low-fat diet for 14 weeks [78]. Both diets contained more than 800 mg of dietary calcium per day. The DASH diet participants had significantly lower urinary sodium levels compared with the high-carbohydrate, low-fat diet group. There was not a difference between the groups related to C-terminal peptide of type I collagen levels. The high-carbohydrate, low-protein group had a 4% increase in the N-terminal propeptide (p = 0.003), which the authors suggested could be related to increased bone turnover.
Bone and calcium metabolism markers at the end of each 30-day sodium period in adults that consumed DASH or control diets.

Values are means ± standard deviation.
Different from the control diet at the same Na level; p < 0.0001.
Different from the high Na level within the same diet; p < 0.05.
Conversion factors: serum parathyroid hormone, ng/l ÷ 10 = pmol/l; mg/g × 0.00283 = mmol/mol.
Different from the high Na level within the same diet; p < 0.01.
DASH: Dietary Approaches to Stop Hypertension.
Reproduced with permission from [77].
Macdonald et al. performed a randomized, placebo-controlled trial in 276 postmenopausal women to evaluate the effect of high fruit and vegetable intakes on bone health [71]. The women were randomly assigned to four groups: high-dose potassium citrate capsules (55.5 mEq/day); low-dose potassium citrate capsules (18.5 mEq/day); identical placebo capsules; or 300 g of fruits and vegetables/day (equivalent to 18.5 mEq of base/day). A nutritionist assisted the subjects in the dietary group in calculating the amounts of additional fruits and vegetables and that group was given a small stipend to cover the cost of the additional fruits and vegetables. Bone markers and BMD were measured over a 2-year period. Evaluation of food diaries at 1 year showed that fruit and vegetable intake generally did increase; however, there were wide variations among patients, with seven patients who decreased their fruit and vegetable intake. Using repeated ANOVA measurements there was no difference in urinary bone resorption markers between the groups; except that urine deoxypyridinoline/creatinine was significantly lower in the highdose potassium citrate group at 4–6 weeks. By ANOVA, there were no significant differences in loss of BMD at the lumbar spine or total hip between any of the groups. The authors speculated that the reason for the difference of their data from the DASH diet data may have been that the DASH diet provided food and provided a larger number of daily fruit and vegetable servings. They did note that there was a relationship between higher fruit intakes and BMD at baseline in the study subjects, which may represent a beneficial effect of long-term diet patterns on bone health. Therefore, further long-term experiments related to diet patterns and bone need to be completed.
Vegetarian/vegan dietary patterns
Vegetarian dietary patterns have been linked to alterations in bone health. There are various patterns of vegetarianism that range from including dairy (lacto), eggs (ovo), fish (pesco) and combinations of the three food groups as well as the vegan pattern, which includes no animal products.
Bone mineral density in vegetarians
The data related to BMD in vegetarians is somewhat confusing, with several trials before 1990 reporting higher BMD in lacto–ovo–vegetarians than in omnivores [73,79]. However, many of these investigations have been criticized because they were completed in Seventh Day Adventist populations who also tend to have higher levels of physical activity, and refrain from smoking, alcohol and caffeine intake [79].
In a cross-sectional study, 105 Mahayana Buddhist vegan nuns and 150 omnivorous women were recruited from monasteries in Ho Chi Minh City (age range: 50–85 years) [80]. BMD was measured at the lumbar spine and femoral neck and dietary intake was determined from a food frequency questionnaire. There was no difference in lumbar spine or femoral neck BMD between vegans and omnivores; however dietary intake of calcium was significantly lower in the vegans than the omnivores. A recent meta-analysis of vegetarian diets and BMD in 2749 individuals (1880 women and 869 men) concluded that BMD was approximately 4% lower in vegetarians than omnivores at the lumbar spine and femoral neck [81]. Lumbar spine BMD was lower in the vegans than lacto–vegetarians. The authors concluded that these differences in BMD likely did not have an effect on fracture risk.
Fracture rates & vegetarian patterns
One study has evaluated fracture risk in individuals consuming vegetarian diet patterns. The Oxford cohort of the European Prospective Investigation into Cancer and Nutrition (EPIC-Oxford) was followed for 5.2 years and evaluated self-reported fractures [82]. In total, 7947 men and 29,749 women aged 20–89 years were recruited by mail and followed through medical practices. Compared with individuals who ate meat, the fracture incidence rate for men and women adjusted for age, sex and nondietary factors was 1.01 (95% CI: 0.88-1.17) for fish eaters, 1.00 (95% CI: 0.89-1.13) for vegetarians, and 1.30 (95% CI: 1.02-1.66) for vegans. When the data for vegans was adjusted for energy intake and calcium intake, the risk of fracture among vegans was comparable. The authors concluded that the higher fracture rate of vegans was due to their low calcium consumption.
Bone health is affected by many dietary factors and the interaction among nutrients is important. The cross-sectional observations of improved BMD and lower bone markers with high potassium, bicarbonate-rich foods have not been confirmed in a 2-year dietary interventional trial [71]. Individuals on vegetarian diet patterns (lacto–ovo) appear to have similar BMD to omnivores. Individuals who follow a vegan pattern may be at risk for lower BMD and higher fracture risk; however, these patterns may be explained by other dietary changes. If a vegan dietary pattern is followed, it is recommended that attention be paid to adequate calcium and vitamin D intake and possibly protein intake [83]. Future studies need to evaluate food patterns on bone health for longer periods of time, and whether there are particular fruits or vegetables that may be most beneficial.
Conclusion
Nutrients have the possibility of affecting bone over the entire lifespan. While there are numerous studies investigating the effect of single nutrients on bone health, the outcomes are often confusing. In many cases, it has been suggested that deficient nutrients levels are acting as markers of poor nutritional status related to bone health. Future investigations will logically center on the effects of food and dietary patterns on bone.
Future perspective
It is likely that future developments related to bone health and nutrition will be in the area of the effects of whole foods and food patterns on bone metabolism, BMD and fracture risk. Instead of supplementation with individual supplements such as calcium and vitamin D, more emphasis will be placed on counseling related to improving dietary patterns.
Executive summary
Nutrition is a relatively young science. Historically, individual nutrient deficiencies have been emphasized related to health. However, the emerging consensus is that the unit of evaluation should be whole foods or food patterns, which take into account the interaction of nutrients and foods instead of single nutrients.
Cross-sectional and observational studies related to nutrition and bone health do not prove causality between a nutrient deficiency or excess and osteoporosis.
The interpretation of bone/nutrition literature is challenging because there are a variety of outcomes (bone mineral density, bone markers and fracture risk) and sometimes there is confusion about the optimal nutritional marker to measure.
Vitamin K, involved in gammacarboxylation of glutamate, has been postulated to be related to increased bone turnover and loss of bone mineral density. However, a recent double-blind, placebo-controlled trial has shown that in North-American women, vitamin K supplementation does not appear beneficial related to bone health and that vitamin K deficiency is likely a marker of malnutrition or frailty.
Vitamin A has been postulated to have detrimental effects on fracture in amounts not much over the recommended dietary allowance. However, it is likely that measurements of retinyl palmitate and not retinol would be a more sensitive marker related to the effect of vitamin A on bone.
A variety of dietary patterns, such as the Mediterranean diet, and the Dietary Approaches to Stop Hypertension (DASH) diet have been studied. The DASH dietary pattern was shown to have a beneficial effect on bone metabolism.
Individuals who select some vegetarian patterns may need to consider supplementation with nutrients such as calcium and protein.
Recent studies of diets high in fruits and vegetables have not shown consistent effects on bone mineral density or bone markers. Future studies in the area of low acid, high calcium, high fruit and vegetable diets are reasonable.
Footnotes
The author has no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants or patents received or pending, or royalties.
No writing assistance was utilized in the production of this manuscript.
