Abstract
Paget's disease of the nipple is an unusual epidermal presentation of underlying breast cancer. It presents as eczematous change or erythematous ulceration, but may also be an incidental histological finding in a mastectomy specimen. Approximately half of the underlying cancers are invasive, the remainder being ductal carcinoma in situ, and only rarely is there no associated malignancy. Routine clinical and mammographic assessment may significantly underestimate the extent of disease, but MRI may increase the sensitivity in detecting occult malignancy. Mastectomy maximizes local control; however, selected cases can be treated by nipple conisation with radiotherapy. Sentinel node biopsy is the standard of care for axillary staging in the clinically and ultrasonically node-negative case. Almost all invasive cases overexpress human EGF receptor-2 and, therefore, are likely to benefit from adjuvant chemotherapy and herceptin.
Keywords
The aim of this review is to consider how the preoperative imaging and histopathology of Paget's disease of the nipple (PDN) determine the available treatment options and probable prognosis.
Paget's disease of the nipple is an uncommon presentation of underlying breast carcinoma and is observed in 0.7–4.9% of all breast cancers. Although Velpeau first described eczematous disease of the nipple in 1856 [1], it was not until 1874 that the relationship between these changes of the nipple and intramammary malignancy was recognized by Sir James Paget [2].
Paget's disease of the nipple is equally likely to be associated with underlying invasive cancer or ductal carcinoma in situ (DCIS). It is rare that there is no malignancy within the breast; this accounts for only 1–6% of those with PDN [3]. When there is PDN and a palpable mass, it is almost always associated with an underlying carcinoma.
The associated carcinoma may be present in any part of the breast and multifocal or multicentric carcinoma associated with PDN has been reported in 32–41% of patients [4,5]. Patients with PDN and no associated breast mass have a peripherally located tumor in almost 30% of cases, which could be missed if a wide excision includes only the nipple–areola complex (NAC) [6].
Histopathology/pathogenesis
The definitive diagnosis of PDN is made from full thickness punch biopsy of the skin of the NAC. An alternative technique is to examine touch smears cytologically. The histopathological appearances are caused by infiltration of the NAC by malignant breast epithelial cells, which are large, round or ovoid with abundant clear, pale cytoplasm and enlarged pleomorphic and hyper chromatic nuclei with prominent nucleoli. Underlying invasive carcinomas are usually grade II/III and, as a consequence, there is a greater risk of metastasis and a poorer prognosis. Associated DCIS is almost always of high grade [4,7].
Considerable controversy surrounds the pathogenesis of PDN. The most widely accepted theory postulates epidermotropic migration of the ductal carcinoma cells from the underlying mammary ducts to the epidermis of the nipple. An alternative view is that in situ neoplastic transformation occurs in pre-existing, benign intraepidermal clear cells of the NAC (Toker cells) that had migrated from non-neoplastic ducts. Most pathologists accept the evidence for migration, but in one study it was demonstrated that, in two cases, Paget's carcinoma cells were genetically different from underlying lesions [8]. Hence, epidermotropism may not be the mechanism in all cases, and sometimes Paget's carcinoma cells might result from in situ transformation of intraepidermal cells, with the underlying malignancy being coincidental (collision tumors).
HER2 overexpression
The majority of studies have demonstrated overexpression of human EGF receptor-2 (HER2) in cases of both DCIS and invasive carcinomas associated with PDN. HER2 positivity has a strong correlation with high-grade invasive carcinomas and is an indicator of poor prognosis. It is likely that this overexpression may be a factor responsible for poorer prognosis of PDN patients with invasive disease in comparison with control cases matched for grade and type. When matched for HER2 positivity, the survival of PDN cases and controls is similar [4,9].
Clinical presentation
Clinical signs can vary from itching and eczematous changes of erythema, to the more classical crusting, bleeding and ulceration of the nipple (
Presenting signs of Paget's disease of the nipple.

Paget's disease of the nipple showing eczematous incrustation.
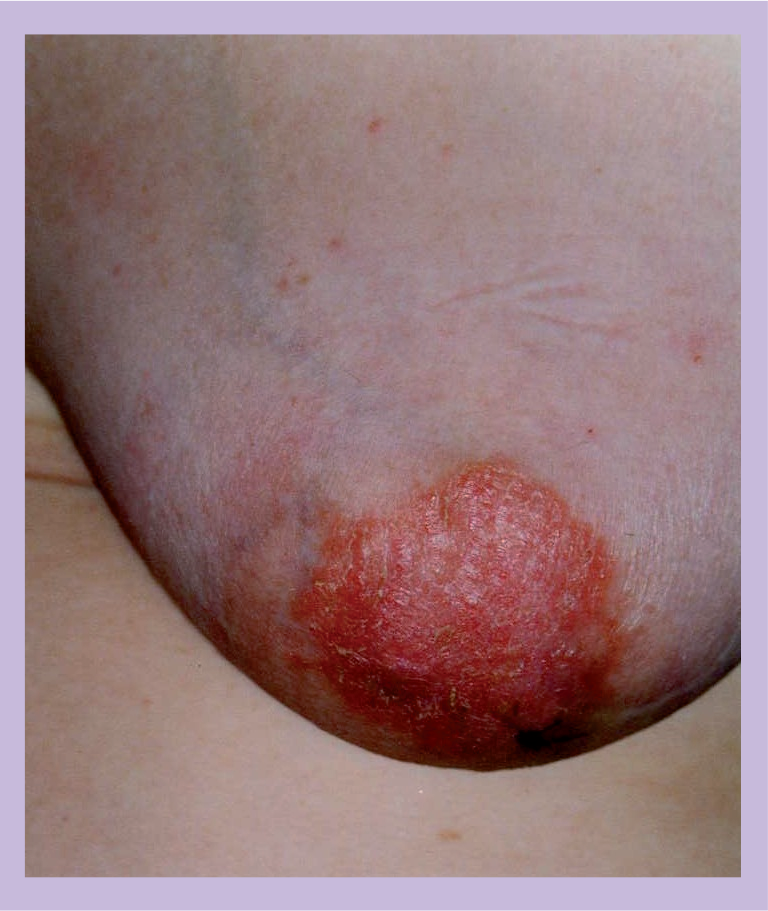
Paget's disease of the nipple showing ulceration and erythema.
Imaging
Mammograms and ultrasound scans are routinely used in the diagnosis and preoperative work-up of patients with PDN. Mammograms can be normal in almost 50% of cases in some studies [11].
Mammography does not discriminate between DCIS and invasive disease, nor can it predict their subtype. As a result, mammograms are of limited use in planning the extent of the surgery.
MRI has been demonstrated to be useful in the detection and diagnosis of clinically and mammographically occult breast malignancies and may also identify tumor foci associated with PDN. Echevarria et al. reported three patients with biopsy-proven PDN who were noted to have an earlier and more intense enhancement pattern in pathological NAC, compared with those with no PDN. The authors suggested that any enhancement on MRI should be regarded with suspicion in a patient at high risk of breast neoplasia, especially since DCIS can very often result in progressive enhancement, which is not typical of malignancy. It is noteworthy that two out of these three patients were confirmed to have neoplasia [12].
Frei et al. reported a series of nine patients with biopsy-proven PDN who underwent preoperative mammography and MRI of the breast and subsequent surgery. Histologically, eight out of nine patients (88%) had DCIS in the retroareolar lactiferous ducts and MRI in these eight patients showed abnormal nipple enhancement with an ill-defined thickened NAC. Mammography was normal in six patients. DCIS elsewhere in the breast, at least 20 mm away from the NAC, was diagnosed in four of nine patients (45%) and MRI demonstrated nonfocal enhancement in all four patients. Mammography identified a suspicious cluster of micro calcifications in three of the four patients [13]. The authors suggested the use of techniques, such as MRI-guided percutaneous biopsy or wire localization procedures, on suspicious breast foci prior to definitive surgery in order to solve the problem of MRI false-positive results.
Both of these studies had very small sample sizes and, as such, the value of MRI remains unproven; however, any investigation that assists in the evaluation of the extent of underlying disease in proven PDN is welcome since it may impact greatly on the choice of surgical treatment offered to patients.
Treatment
Mastectomy with or without axillary clearance was considered the standard surgical management of PDN for many years. As breast conserving therapies became proven to be as safe for selected women with invasive breast cancer, attempts were made to apply this to patients with PDN. Techniques included nipple excision alone, radiotherapy alone and conisation of the NAC or quadrantectomy with or without radiotherapy. Some cases of PDN are confined to the NAC and while breast conserving surgery, which includes the removal of the NAC, would be possible in these patients, increased risk of local recurrence continues to be a problem.
Surgery
The optimal surgical management of PDN remains to be defined. Several studies have recently advocated breast-conserving surgery, particularly for patients with minimal disease. Dixon et al. treated ten patients with cone excision without radiotherapy and reported local recurrence rate in 40%, with two patients developing metastatic disease at 56 months median follow-up [14]. By contrast, Paone and Baker reported a 100% disease-free survival at 5 years for five patients that they had treated with conisation [15]. Results are shown in
Results of local treatment of Paget's disease of the nipple.
BCS: Breast conserving surgery; DCIS: Ductal carcinoma in situ; DFS: Disease-free survival; FU: Median follow-up in months; Inv: Invasive breast cancer; LR: Local relapse; Mx: Mastectomy; n: Number of cases; N/A: Not available; OS: Overall survival; RT: Radiotherapy.
Kawase et al. published a series of 104 patients of whom 97 patients (93.2%) had an underlying invasive or noninvasive cancer associated with PDN. A total of 92 patients (88.5%) underwent mastectomy and 12 patients (11.5%) had a breast-conserving procedure. On univariate analysis, patients aged younger than 60 years at diagnosis who had stage II disease, positive lymph nodes, invasive disease or a palpable mass had significantly lower 10-year disease-specific and recurrence-free survival. There were four locoregional recurrences (three after mastectomy and one after breast conservation). There were no significant differences in overall, disease-specific or recurrence-free survival according to the type of surgery [16].
Kothari et al. reported a series of studies involving 70 women with PDN treated at Guy's Hospital, London, UK, and demonstrated that mammography significantly underestimates the true extent of underlying breast carcinomas in approximately 43% of all cases. In 63% of patients, there was a multifocal or multicentric breast carcinoma with no clinical abnormality other than nipple changes being found. It was concluded that wide local excision consisting of the NAC and a cone of underlying breast tissue (conisation) will leave residual tumor in 75% of all patients with PDN [4].
Radiotherapy with or without surgery
Bijker et al. published a series of studies involving 61 patients from the European Organization for Research and Treatment of Cancer (EORTC) 10873, a nonrandomized study examining the outcome of breast conserving therapy by means of a cone excision and radiotherapy in patients with PDN. A total of 97% of patients had no associated palpable mass and, at histological examination, 93% of patients had an underlying DCIS. After a median follow-up of 6.4 years, four of the 61 patients developed a recurrence in the treated breast (one patient with DCIS and three patients with invasive disease). One patient with an invasive local recurrence died of disseminated breast carcinoma. The 5-year local recurrence rate was 5.2%. The authors concluded that breast-conserving therapy followed by whole breast radiotherapy is a feasible alternative for patients with PDN and a limited extent of underlying DCIS [17].
Stockdale et al. reported a series of 28 patients with PDN, treated by irradiation, of whom nine (32%) had an associated lump. After a median follow-up of 5 years, there was a recurrence in three of the 19 patients (16%) who did not have a palpable lump or mammographic abnormality. Of the nine patients with a lump, recurrence occurred in eight (89%) and death from breast carcinoma was recorded in five (56%) [18].
Marshall et al. reported excellent 10- and 15-year rates of local control, disease-free and overall survival following BCS and RT. A total of 94% of patients underwent complete or partial excision of the NAC and all patients received radiotherapy to whole breast. The authors supported the recommendation of local excision and definitive breast irradiation as an alternative to mastectomy in the treatment of patients with PDN presenting without a palpable mass or mammographic density [19].
Axillary staging
The reported incidence of axillary nodal involvement in PDN patients is 50–60% in the presence of a mass and 21% in the absence of a lump. Sentinel node biopsy (SNB) has become a standard of care for axillary lymph node staging in breast cancer and is suitable for all patients with no evidence of clinical, radiological and cytopathological involvement of axillary lymph nodes.
Sukumvanich et al. reported a series of 39 patients with PDN who had undergone SNB, of whom 19 had PDN without a lump or radiological abnormality and, in this group, invasive cancer was found in 27% of cases and positive sentinel lymph nodes were found in 11%. The authors concluded that SNB should be considered in all patients with PDN, regardless of whether associated clinical or radiographic findings are present [20].
Executive summary
Epidermotropic migration of the ductal carcinoma cells from the underlying mammary ducts to the epidermis of the nipple may not be the mechanism in all cases.
Sometimes Paget's carcinoma cells might result from in situ transformation of intraepidermal cells, with the underlying malignancy being coincidental.
Overexpression of human EGF receptor-2 in both ductal carcinoma in situ and invasive carcinomas associated with Paget's disease of the nipple (PDN) is well known.
Human EGF receptor-2 positivity may be a factor responsible for poorer prognosis of PDN patients with invasive disease in comparison with control cases matched for grade and type.
Clinical examination and mammography can be normal in up to 50% of cases, often leading to a delay in the diagnosis of PDN.
Since PDN is primarily a clinical diagnosis and mammograms may be negative, screening programs without clinical examination may also result in a delay in diagnosis.
MRI helps in the evaluation of the extent of underlying disease in proven PDN, and may impact greatly on the choice of surgical treatment offered to the patient.
Mastectomy was considered the gold standard surgical treatment in the past but now breast conserving surgery with radiotherapy is emerging as a suitable alternative.
All patients should undergo sentinel node biopsy to stage the axilla in the absence of proven preoperative lymph node metastasis.
Laronga et al. reviewed 54 patients with PDN, of whom 36 had SNB, and concluded that PDN should be treated similarly to other breast cancers; SNB should be performed in order to evaluate the axilla when invasive disease is identified or a mastectomy is planned owing to the extent of DCIS [21].
Recently, Caliskan et al. reported a series of studies involving 114 patients with confirmed PDN and concluded that breast conserving surgery was possible when there was complete excision of the NAC with tumor-free margins. The authors also concluded that SNB combined with breast irradiation for both DCIS and invasive carcinoma was the treatment of choice [22].
Conclusion
Treatment of PDN remains controversial. While mastectomy was accepted as the gold standard surgical treatment in the past, breast conserving surgery with radiotherapy is emerging as a suitable alternative for selected cases. Routine preoperative MRI to accurately assess the extent of disease is recommended and will enable accurate planning of appropriate surgical option. All patients should undergo SNB in order to stage the axilla in the absence of proven lymph node metastasis preoperatively.
Future perspective
Neoadjuvant treatment is now widely used for the down-staging of invasive cancer and the availability and proven efficacy of herceptin makes this agent a promising candidate for such a role in the primary treatment of PDN. This approach could render some of these cases suitable for breast conserving treatment with SNB and breast irradiation alone.
Footnotes
The authors have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants or patents received or pending, or royalties.
No writing assistance was utilized in the production of this manuscript.
